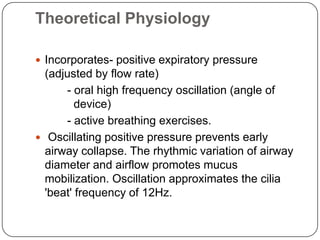
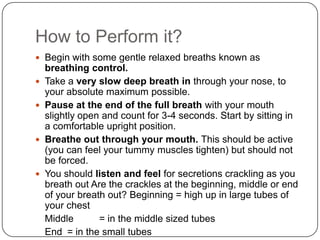
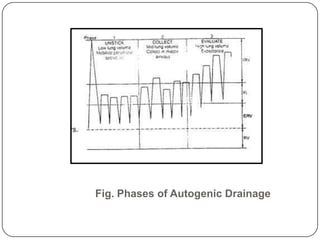
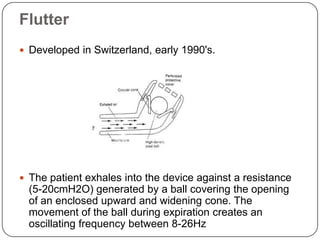
Autogenic drainage (AD) is a controlled breathing technique, developed in Belgium during the late 1960s, aimed at clearing chest secretions without excessive coughing. The process involves three phases: 'unsticking' secretions through low breathing, 'collecting' them in mid-sized airways, and 'evacuating' them with high-volume breaths. The technique is designed for patients with retained secretions, particularly beneficial for children, while precautions must be taken for certain medical conditions.