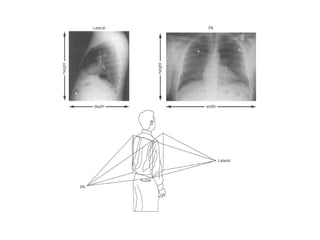
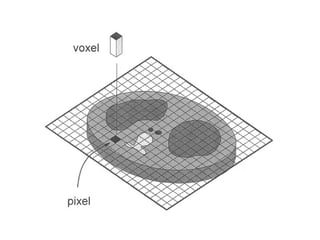
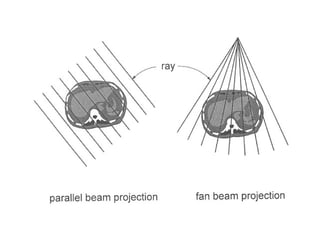
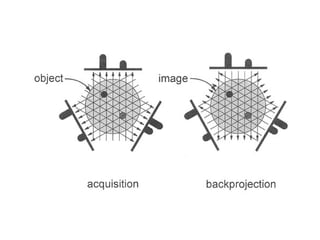
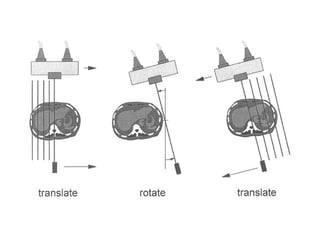
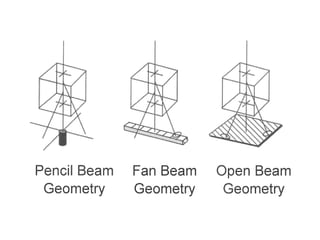
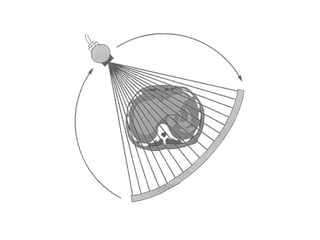
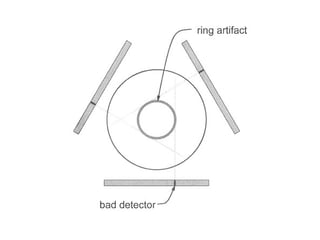
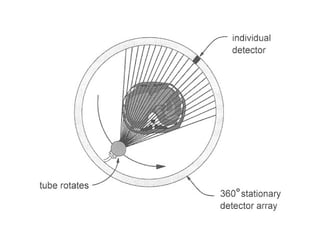
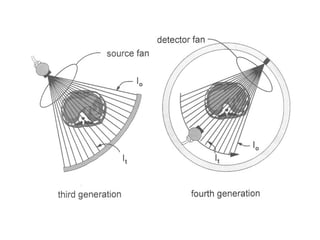
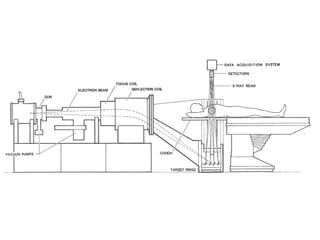
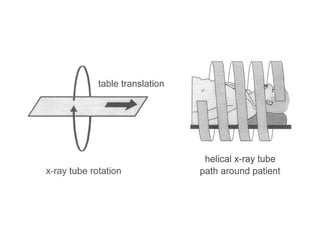
This document describes the basic principles and historical development of computed tomography (CT) imaging. It discusses how CT uses mathematical principles and X-ray projections to create 3D images of internal anatomy. The document then summarizes the key innovations and technologies of each generation of CT scanners, from early pencil beam systems to current multi-detector array systems, which provide faster and higher resolution volumetric imaging.