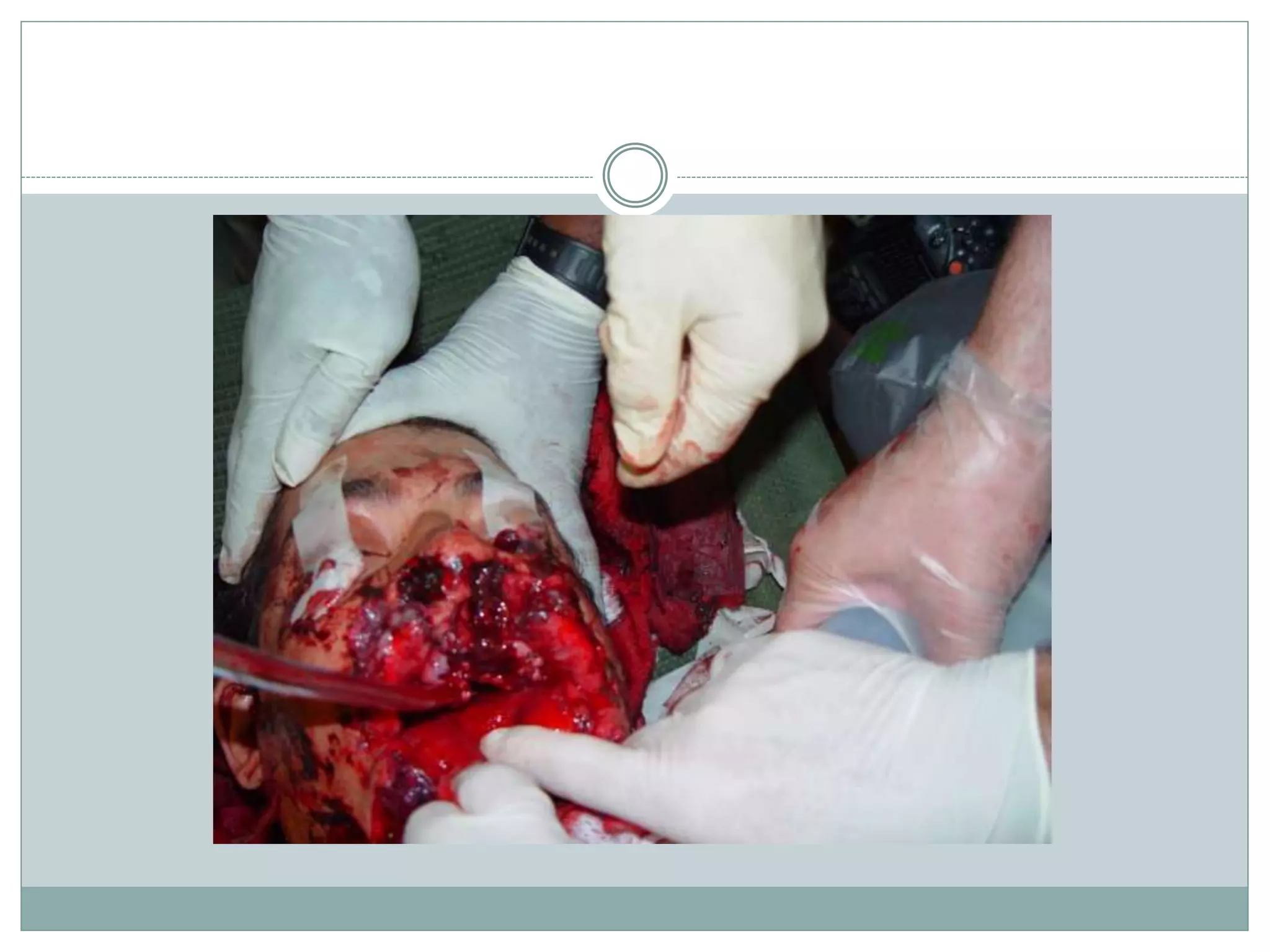
1) Blast injuries can cause a wide range of damage depending on factors like the type of explosive, distance from the blast, and presence of barriers. Primary injuries result directly from blast wave overpressure and include blast lung and traumatic brain injury.
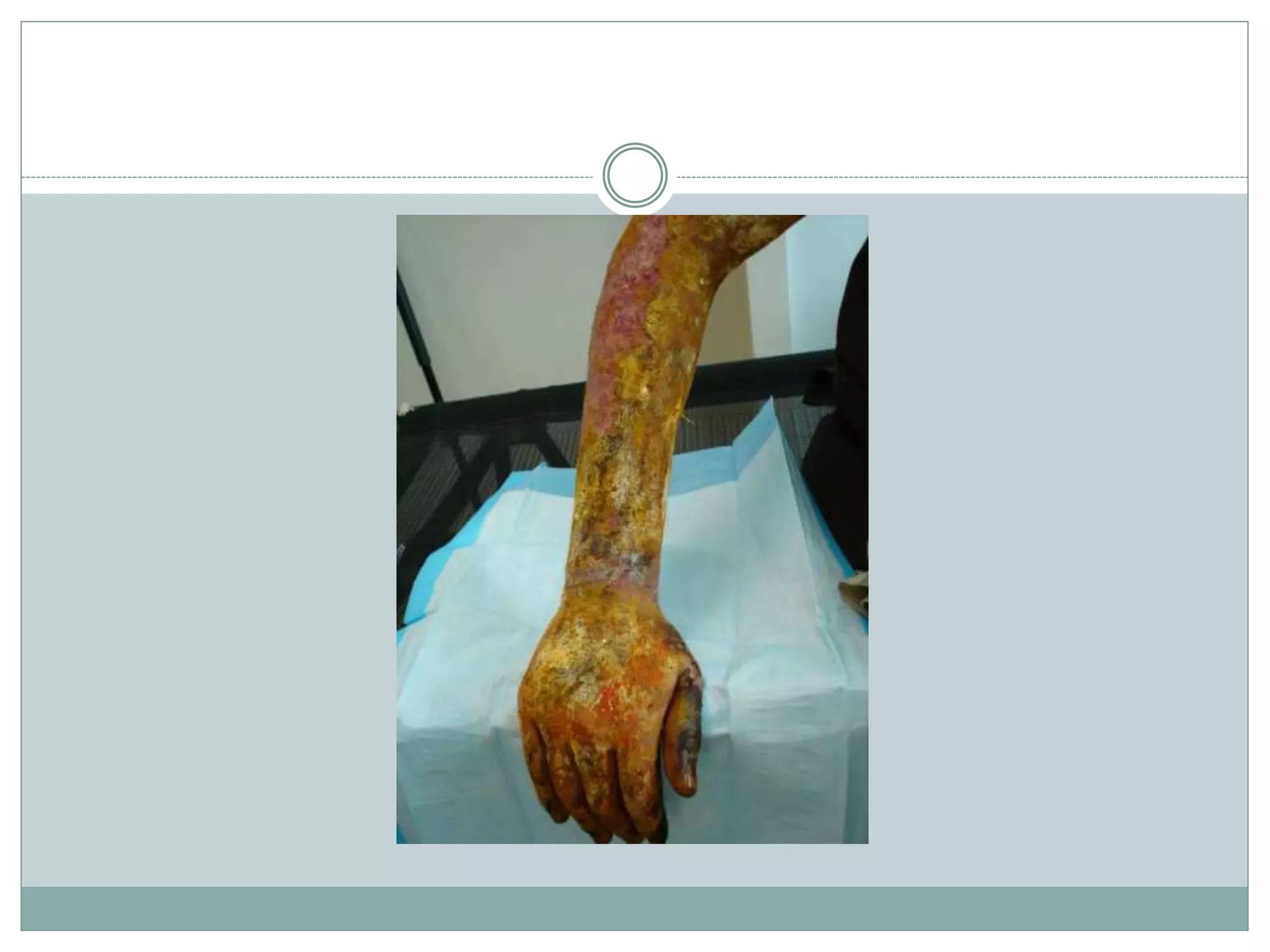
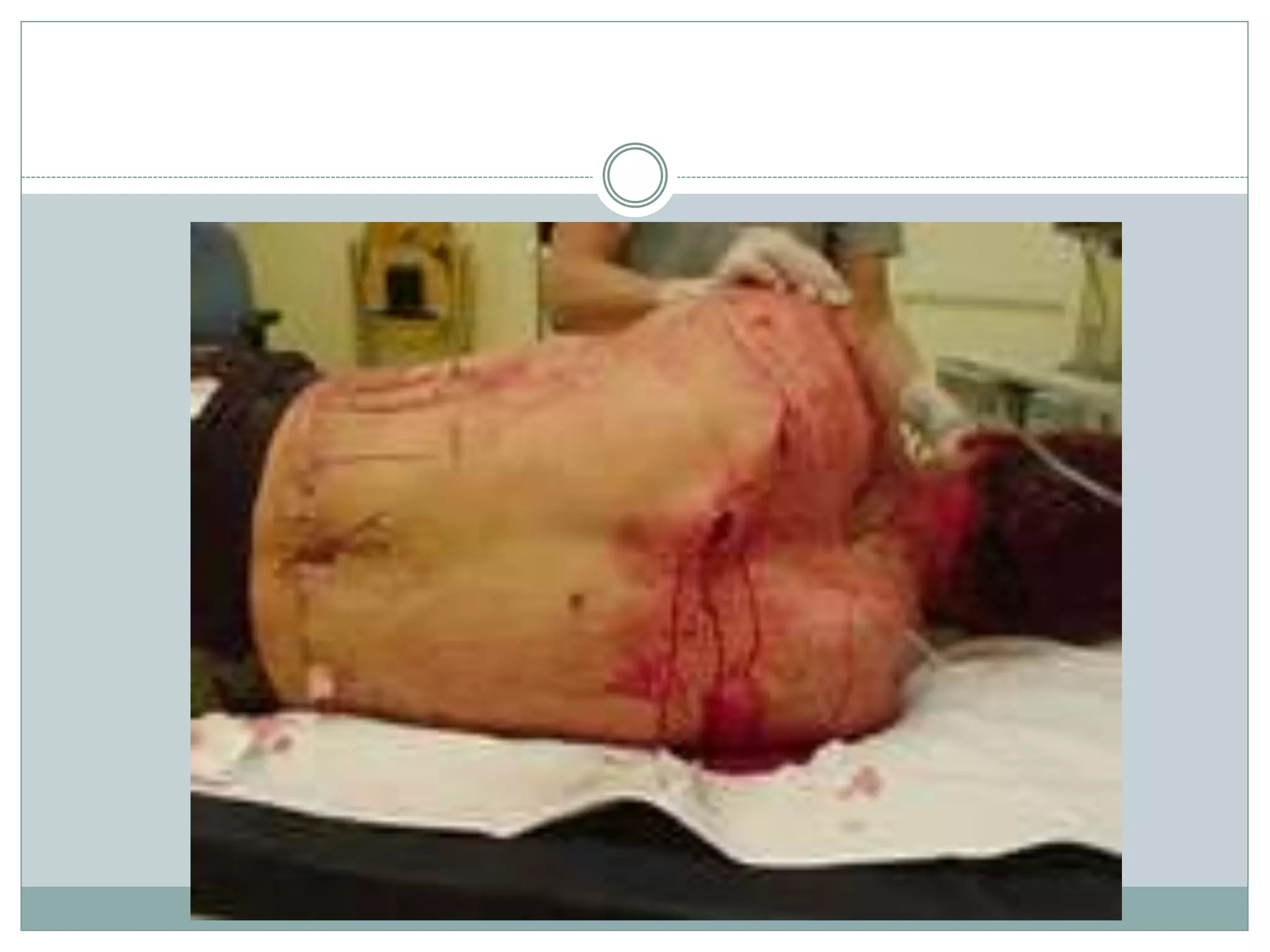
2) Secondary injuries are caused by bomb fragments and debris that can penetrate the body. Tertiary injuries occur when the victim's body is propelled by the blast, often causing fractures and amputations upon impact. Quaternary injuries include burns, crush injuries, and complications from toxic inhalation/contamination.
3) Blast lung is a common primary injury where the rapid pressure change ruptures the lungs. Symptoms include hypoxemia. Treatment involves oxygen supplementation