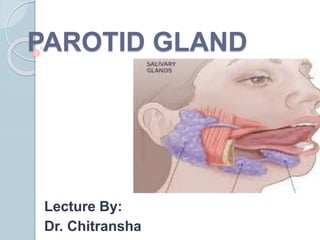
Parotid Gland
- 1. PAROTID GLAND Lecture By: Dr. Chitransha
- 2. DEFINITION : These are compound tubuloacinar exocrine glands found in oral cavity that secrete complex fluid known as saliva.
- 3. CLASSIFICATION OF SALIVARY GLANDS Based on size Based on type of secretory cells.
- 4. Based on size: 1. Major salivary glands 2. Minor salivary glands
- 5. Major Salivary Glands Collection of secretory cells aggregated into large bilaterally paired extraoral glands with extended duct system through which the gland secretions reach the mouth. Parotid Submandibular Sublingual
- 7. Minor Salivary Glands Collection of secretory cells scattered throughout the mucosa & submucosa of the oral cavity with short ducts opening directly onto mucosal surface. Eg. : Serous glands of Von Ebner. Anterior lingual glands. Buccal, labial, palatal glands,
- 8. Based on type of secretory cells I. Serous : Parotid II. Mixed (seromucous): Submandibular III. Mucous: Minor salivary glands
- 9. OBJECTIVES 1) Introduction 2) Situation 3) Shape, measurements & presenting parts 4) Capsule 5) Relations 6) Structures within the parotid gland 7) Parotid duct 8) Blood supply 9) Nerve supply 10) Lymphatic drainage 11) Applied anatomy
- 10. INTRODUCTION Largest salivary gland. Serous type. Produce saliva. Keeps the oral cavity moist. Helps in chewing & swallowing.
- 11. Situation Parotid region Parotid = para (around) + otic (ear)
- 12. Shape, measurements and parts Shape: • Inverted pyramidal Weight: • 15-25 grams Presenting parts: • Apex • Base -(superior surface) • 3 Surfaces • 3 Borders
- 13. 3 Surfaces 1. Superficial or lateral 2. Anteromedial 3. Posteromedial
- 14. 3 Borders Anterior Posterior Medial
- 15. Coverings (capsule) 2 capsules: a) Inner true capsule b) Outer false capsule True capsule: condensation of fibrous stroma of gland. False capsule (parotid sheath): Investing layer of deep cervical fascia- parotidomassetric fascia.
- 16. False Capsule Splitting of investing layer of deep cervical fascia Superficial lamella – Parotido- masseteric fascia Deep lamella- thin Lower border form Stylomandibular ligament (separates parotid from submandibular gland)
- 18. Parts & their Relations Apex: (directed below) Overlaps post. belly of digastric Apex appears in carotid triangle Structures passing through apex 1. Cervical br. of facial nerve 2. Anterior division of retromandibular vein 3. Formation of ext. jugular vein
- 20. Base Directed upwards & concave Relation: Ext. acoustic meatus post. Part of TMJ Structures passing thro’ base: 1. Temporal br. of facial nerve 2. Superficial temporal vessels 3. Auriculo-temporal nerve
- 22. Superficial or lateral surface Covered by skin, superficial fascia with lymph nodes & great auricular nerve, Posterior fibres of platysma. Superficial lamella of parotid sheath (Parotido- masseteric fascia)
- 24. Antero-medial surface Grooved for ramus of mandible. Relations: Postero-inferior part of masseter Ramus of mandible Capsule of TMJ Medial pterygoid muscle Outer lip of groove transmits- branches of facial nerve Inner lip of groove transmits – maxillary artery
- 26. Postero-medial surface Mastoid process with attached muscles. Facial nerve pierces & enter the gland Styloid process with attached muscles Deep to styloid – ICA, IJV & last 4 cranial nerves ECA in a groove (before piercing
- 28. Anterior border Separates superficial & anteromedial surface. Structures passing thro’ this border (above downwards) Zygomatic br. of facial N Transverse facial vessels Upper buccal br. of facial N Parotid duct Lower buccal br. of facial N Marginal mandibular br. of facial N
- 30. Posterior border Structures passing thro’ this border Posterior auricular branch of facial nerve Posterior auricular
- 31. Medial border Pharyngeal border Related to wall of pharynx
- 32. Structures passing through the parotid From outside inwards:- 1. Facial nerve & its branches 2. RMV 3. ECA
- 36. Parotid duct (Stensen’s duct) 5 cm length & 3 mm width Emerges thro’ anterior border of the gland. Runs on the masseter between upper & lower buccal nerves. At anterior border of masseter turns medially. Opens in to vestibule of mouth –opp. crown of upper 2nd molar tooth.
- 40. Blood supply Arterial supply: Branches from external carotid artery (superficial temporal & maxillary artery). Venous drainage: Drain into tributaries of external jugular vein.
- 41. Nerve supply 1. Parasympathetic – secretomotor (watery) 2. Sympathetic – secretomotor (mucous rich sticky) & vasomotor (blood vessels) 3. Sensory – auriculotemporal nerve (gland) & great auricular nerve ( parotid fascia)
- 42. Parasympathetic (secretomotor) supply It is provided through auriculotemporal nerve. The preganglionic fibres arise from the inferior salivatory nucleus in the medulla and pass successively through glossopharyngeal nerve, tympanic branch of glossopharyngeal (Jacobson’s nerve), tympanic plexus and lesser petrosal nerve to relay into otic ganglion. Postganglionic fibres arise from the ganglion and pass through the auriculotemporal nerve to supply the parotid gland. The stimulation of parasympathetic supply produces watery secretion.
- 44. Sympathetic supply The preganglionic sympathetic fibres arise from the lateral horn of T1 spinal segment relay in superior cervical sympathetic ganglion. postganglionic fibres is derived from sympathetic plexus around external carotid artery & supply through auriculotemporal nerve. The sympathetic fibres are vasomotor and their stimulation produces thick sticky secretion.
- 46. Sensory supply It is derived from: (a) Auriculotemporal nerve. (b) Great auricular nerve (C2 and C3).
- 47. Lymphatic drainage Superficial parotid nodes ( superficial fascia) Deep parotid nodes ( within the gland)
- 48. Applied anatomy Mumps: Viral Infection of the parotid gland. Mumps (parotiditis / non- suppurative) Parotid abscess: The parotid abscess occur by spread of infection from the oral cavity. Bell’s palsy.
- 49. Sialography of the Parotid Duct Blockage of the Parotid Duct Parotidectomy
- 50. Mixed parotid tumor Facial nerve not involved. It is slow-growing lobulated painless tumor of parotid gland. It is so called because of its mixed histological appearance. Currently it is termed pleomorphic adenoma. After many years of slow benign growth, it may undergo a malignant change.
- 51. Frey's Syndrome Auriculo-temporal nerve syndrome. Penetrating wound of parotid injured to auriculotemporal (secretomotor) & great auricular nerve. During healing process Secretomotor fibres of auriculotemporal nerve grow out & join with distal end of great auricular nerve and reach sweat glands.
- 53. The presenting features of Frey’s syndrome are: When a person eats, the ipsilateral cheek (parotid region) becomes red, hot, and painful & sweating.