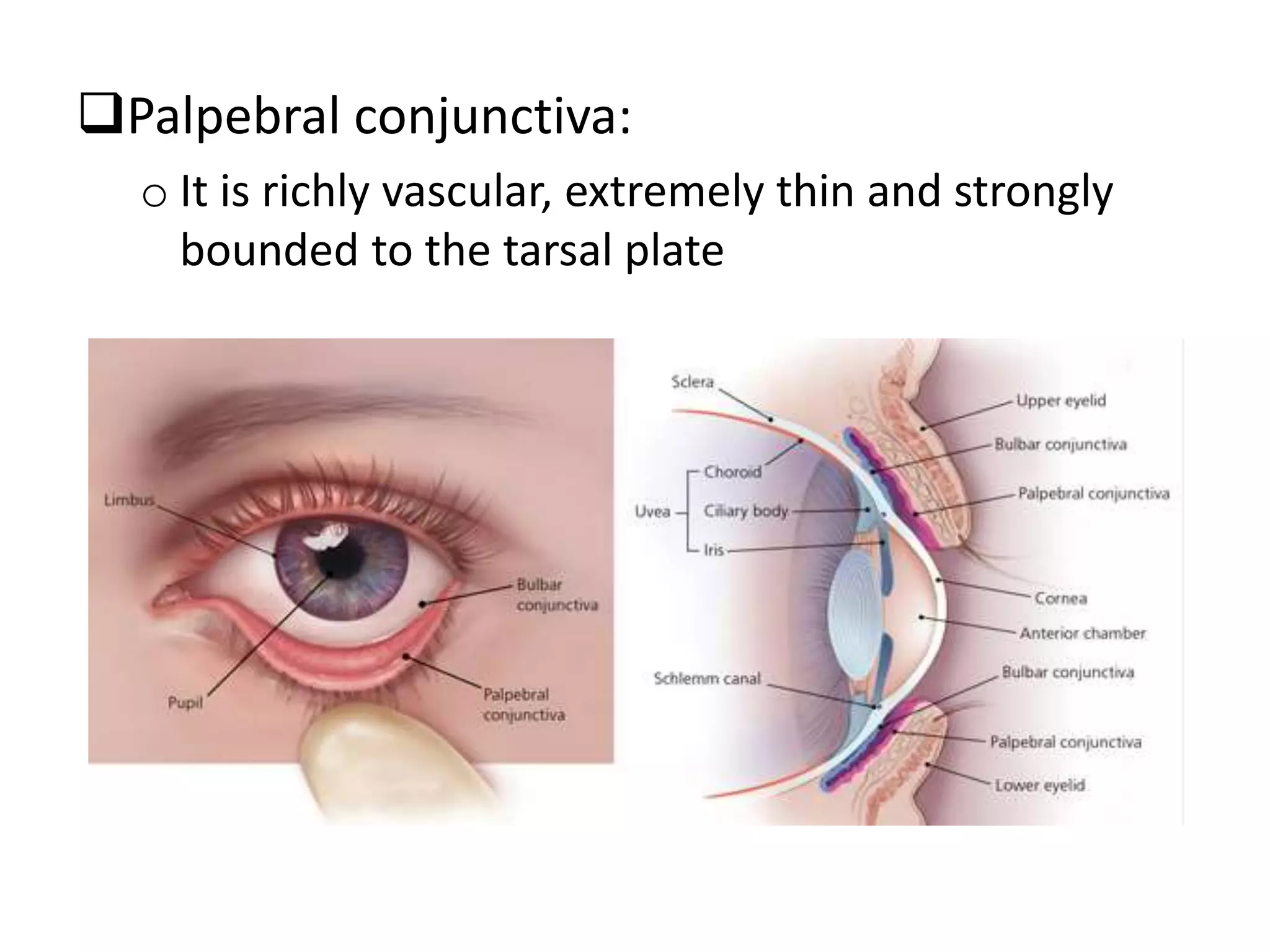
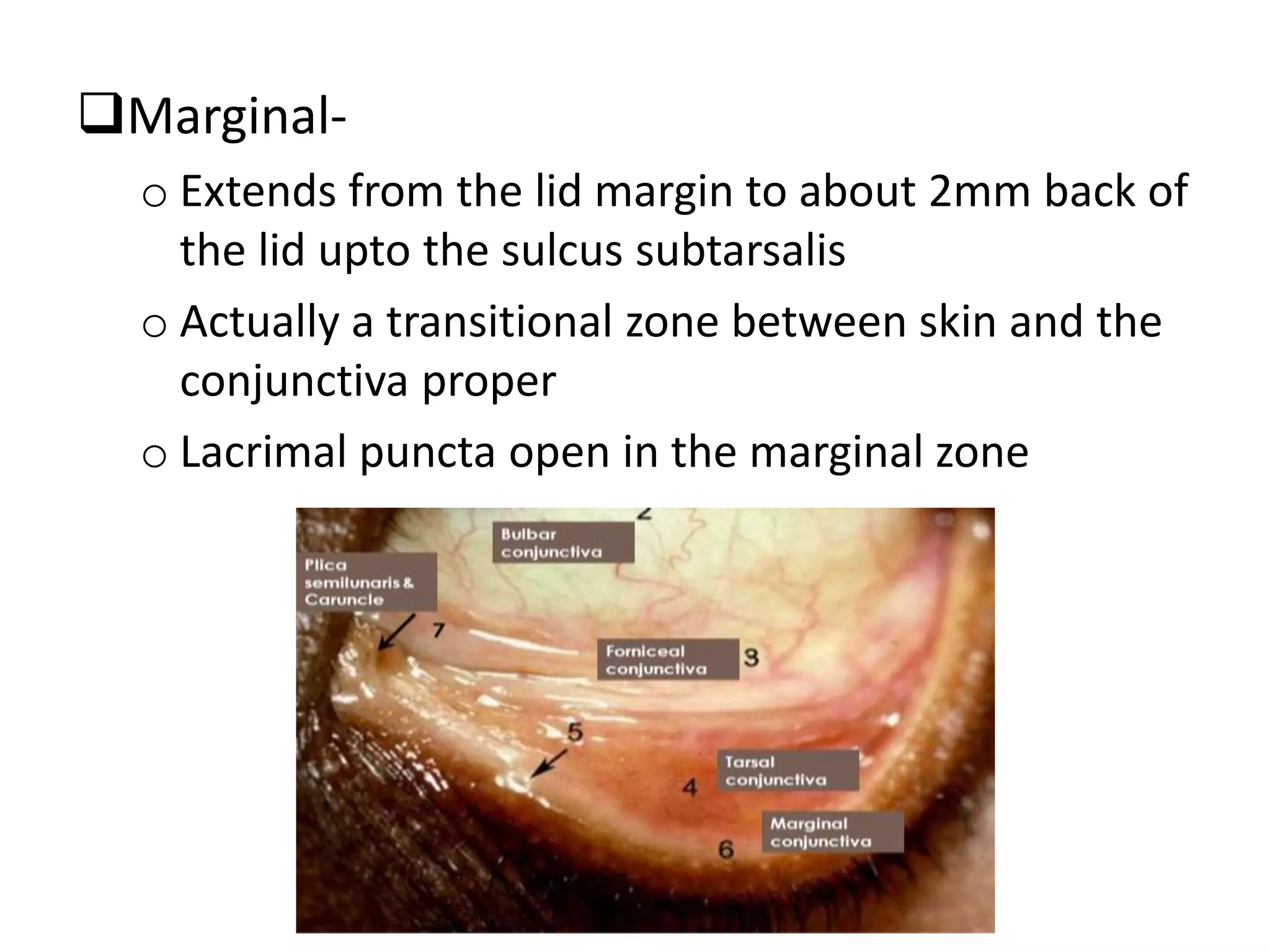
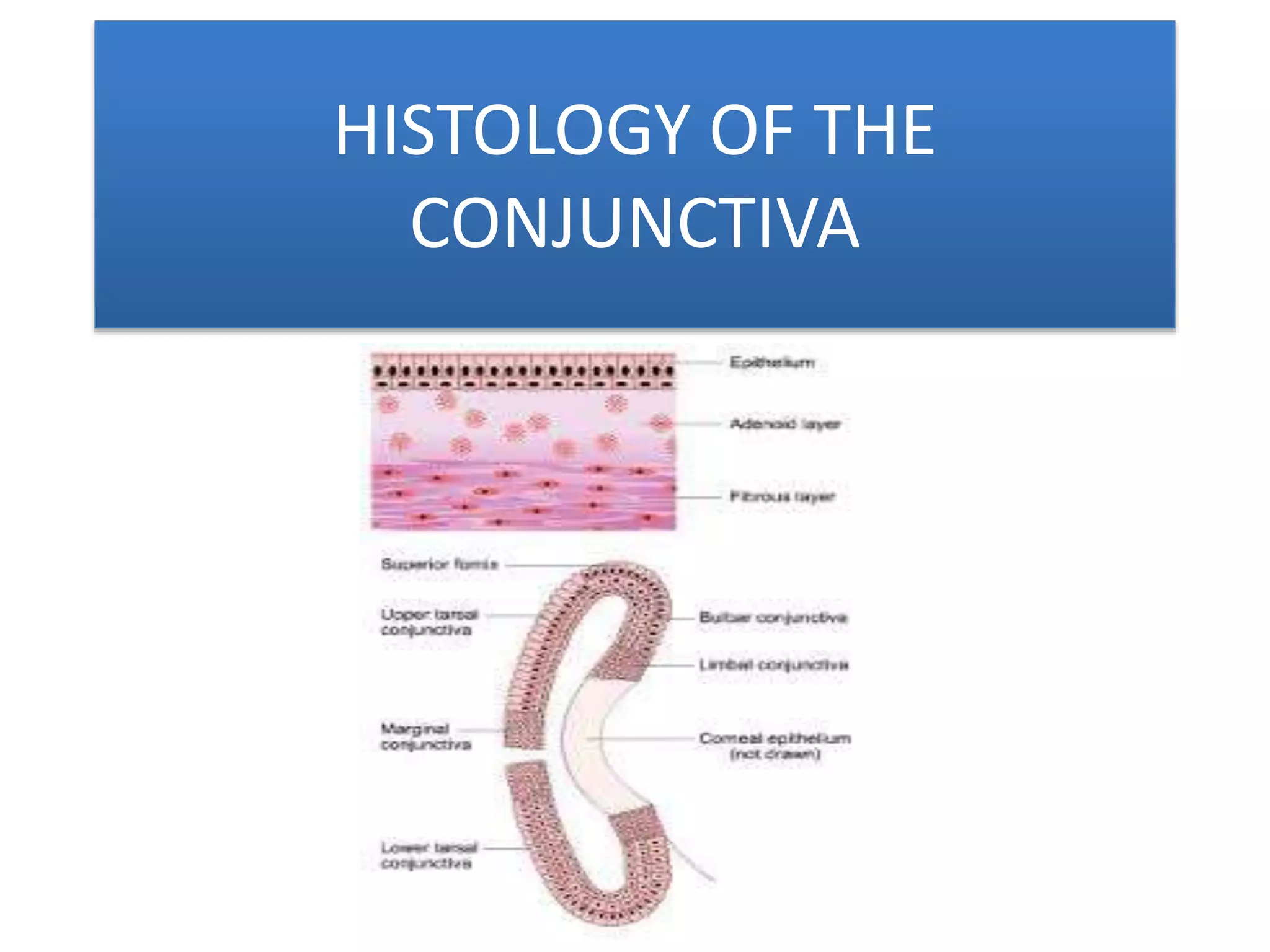
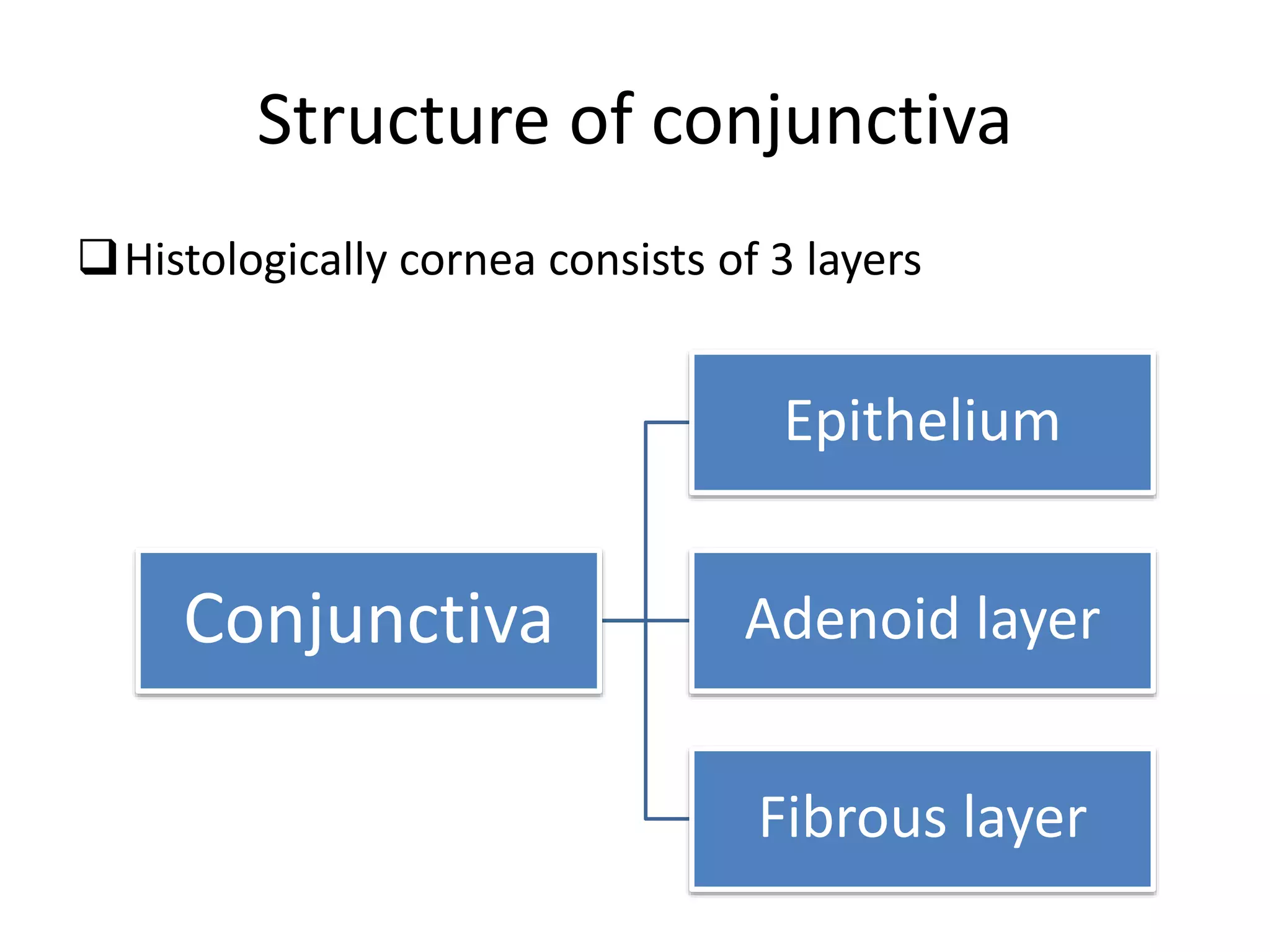
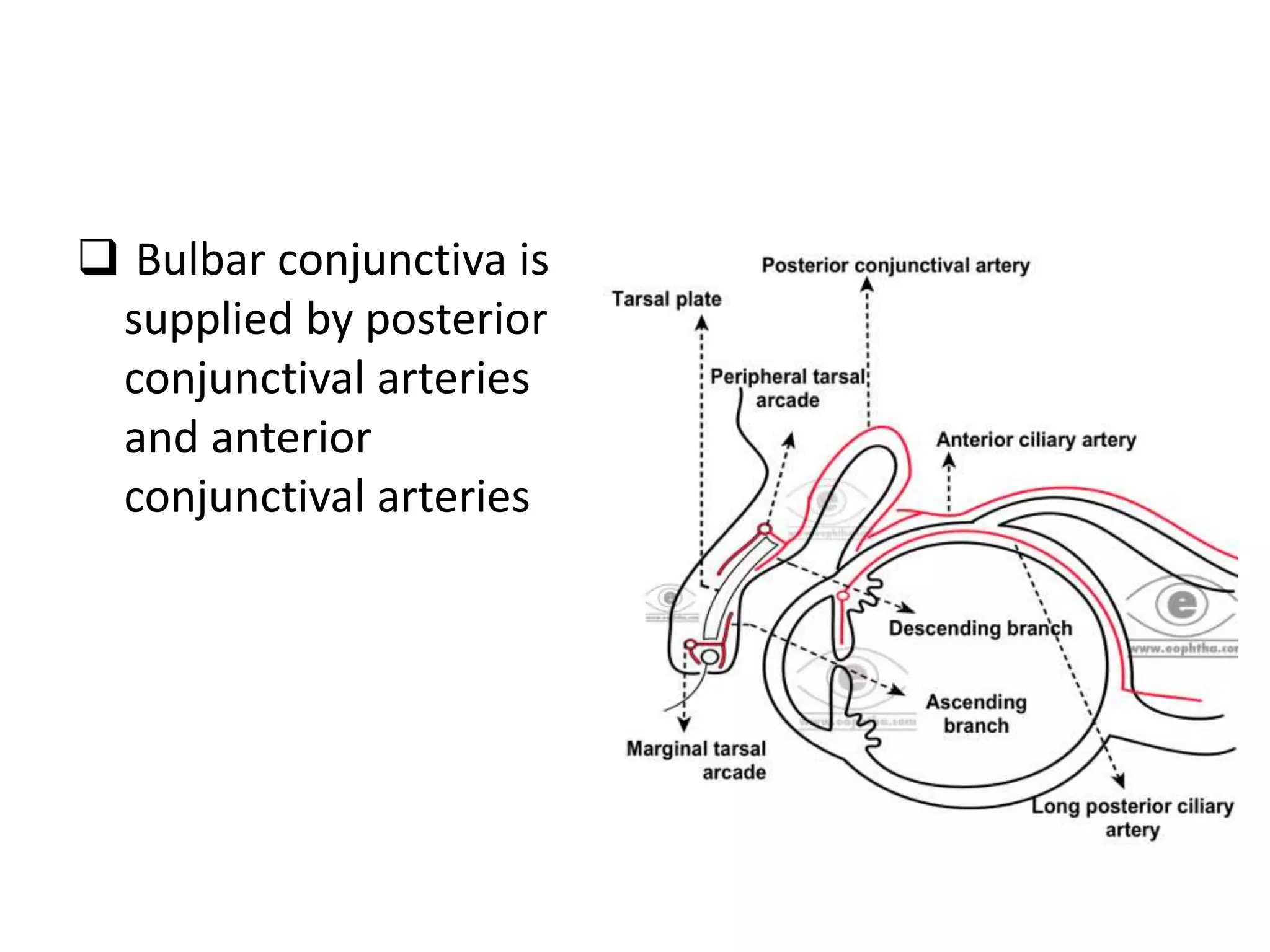
The conjunctiva is a mucous membrane that lines the inner surface of the eyelids and covers the anterior sclera of the eye. It has several functions including lubricating the eye and contributing to immune surveillance. The conjunctiva consists of the palpebral, bulbar, and forniceal conjunctiva. The palpebral conjunctiva lines the inner surface of the eyelids and is subdivided into the marginal, tarsal, and orbital conjunctiva. The bulbar conjunctiva covers the anterior sclera and is separated from it by the episcleral tissue. It consists of the limbal and scleral conjunctiva. The conjunctival fornices are cul