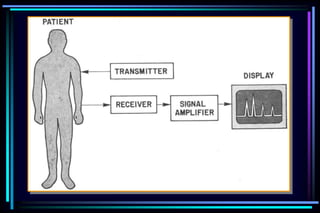
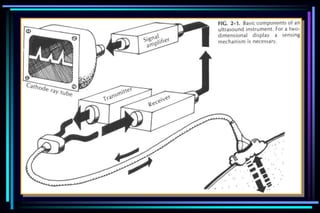
1. Ultrasound uses high frequency sound waves to generate images of the inside of the body without harming tissue.
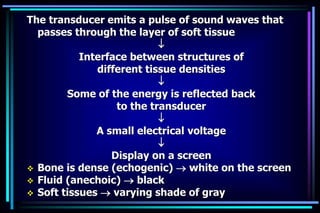
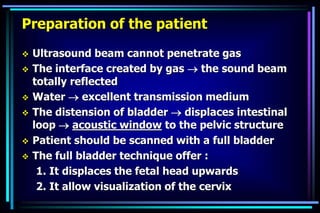
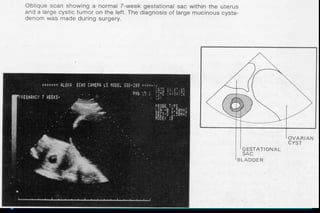
2. In obstetrics, ultrasound is used to confirm pregnancies, determine gestational age, assess fetal anatomy and growth, monitor fetal well-being, and investigate uterine bleeding or other potential complications.
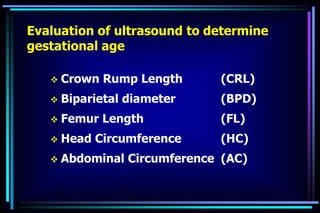
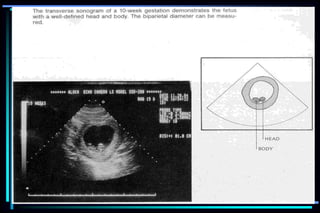
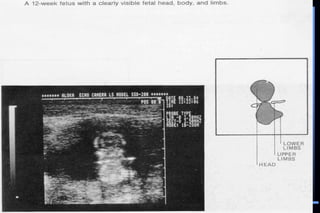
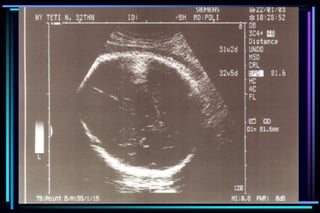
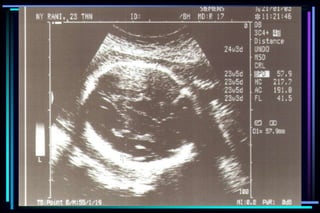
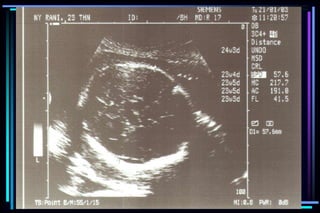
3. Key measurements like crown-rump length, biparietal diameter, femur length, head circumference, and abdominal circumference are used to accurately determine gestational age within a few days or weeks.