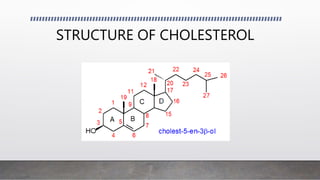
The document discusses cholesterol, its functions, and metabolism, highlighting its origins from both diet and liver synthesis. It details the importance of cholesterol testing, how the tests are conducted, and the interpretation of results, including recommended age for screening. Additionally, it outlines dietary recommendations, potential medications for managing cholesterol levels, and clinical implications of abnormal cholesterol levels.