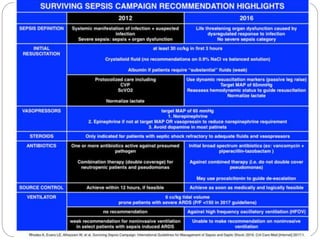
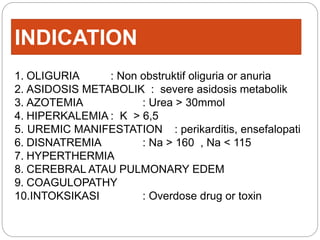
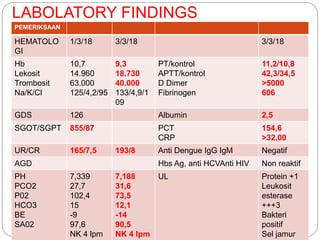
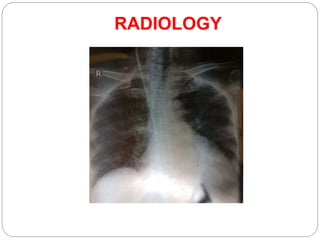
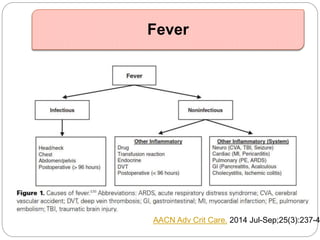
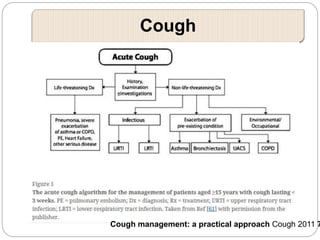
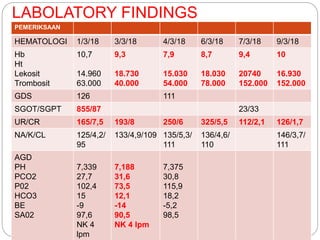
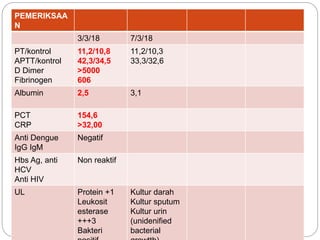
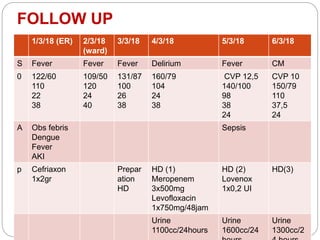
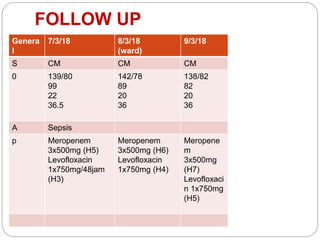
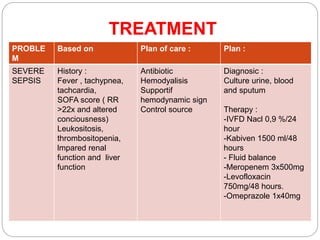
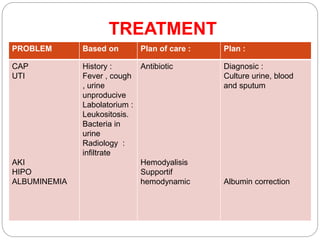
A 71-year-old woman presented with fever, cough, and altered mental status. She was diagnosed with sepsis and acute kidney injury. She received empiric antibiotics and underwent hemodialysis to manage her organ dysfunction. Her condition improved over several days of treatment, though cultures did not identify a definite microbe.