Here are the key points indicated by each test result:
- Severe proteinuria indicates kidney damage allowing protein to pass into the urine.
- Casts with red blood cells suggest kidney inflammation or damage.
- Low specific gravity suggests decreased kidney concentration ability.
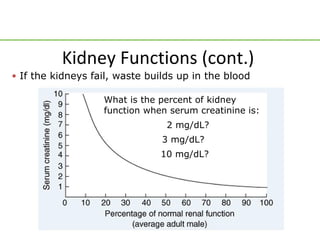
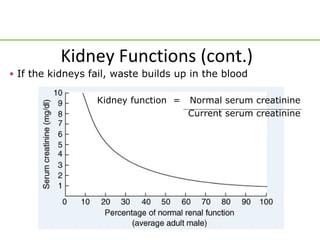
- Serum creatinine of 6 mg/dL indicates severe loss of kidney function (around 20% function).
- BUN of 35 mg/dL and creatinine of 1.2 mg/dL could indicate prerenal azotemia from decreased kidney perfusion rather than intrinsic kidney disease.










![When Urine Reaches Distal Tubule
• Juxtaglomerular cells
measure blood flow in
the afferent arteriole
and urine flow and
composition
Juxtaglomerular
cells • They can release renin
(Image modified from Bowne, P.S. [2004]. Kidneys tutorial. Used with
author’s permission.)](https://image.slidesharecdn.com/renalrevised-120618134417-phpapp01/85/Renal-revised-11-320.jpg)
![Renin Starts the RAA Pathway
• Which turns on
the Na+/K+
ATPase in the
distal tubule
• Na+ and water
Juxtaglomerular
cells
are reabsorbed
• K+ is secreted
(Image modified from Bowne, P.S. [2004]. Kidneys tutorial. Used with author’s permission.)](https://image.slidesharecdn.com/renalrevised-120618134417-phpapp01/85/Renal-revised-12-320.jpg)