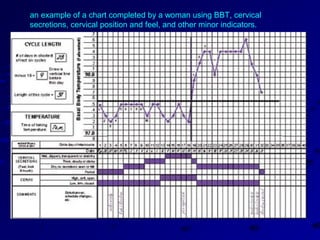
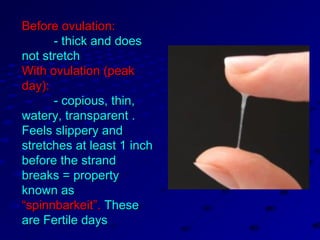
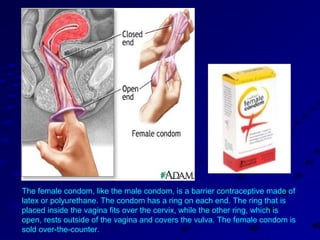
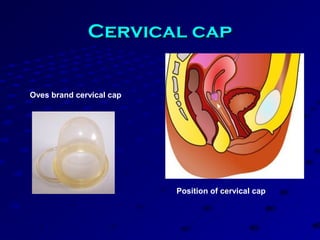
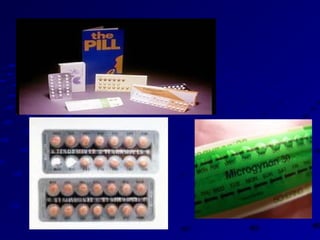
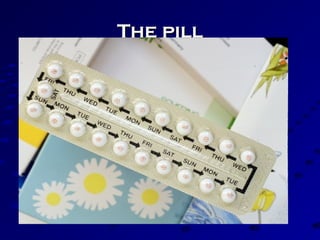
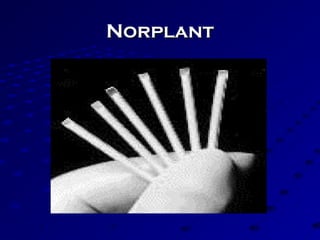
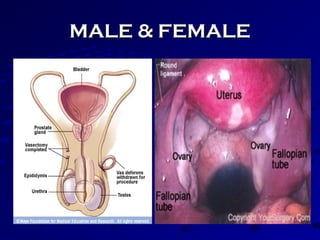
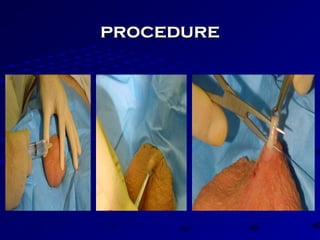
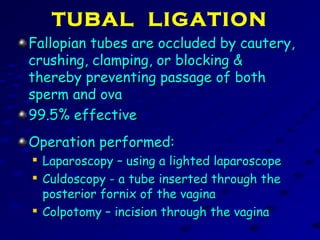
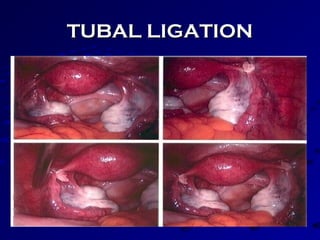
Vital statistics are systematically collected facts related to vital events like births, deaths, and marriages. They are compiled from sources like censuses, registration records, and health surveys. Vital statistics are used for policymaking, administration, research, and public health programs. Some key vital statistics include birth rate, death rate, crude death rate, maternal mortality ratio, and infant mortality rate. Recent advancements in contraceptives allow individuals to plan their families and avoid unwanted births. Natural family planning methods like rhythm method and basal body temperature tracking require abstaining from sex during fertile periods, while barrier methods like condoms use physical barriers.