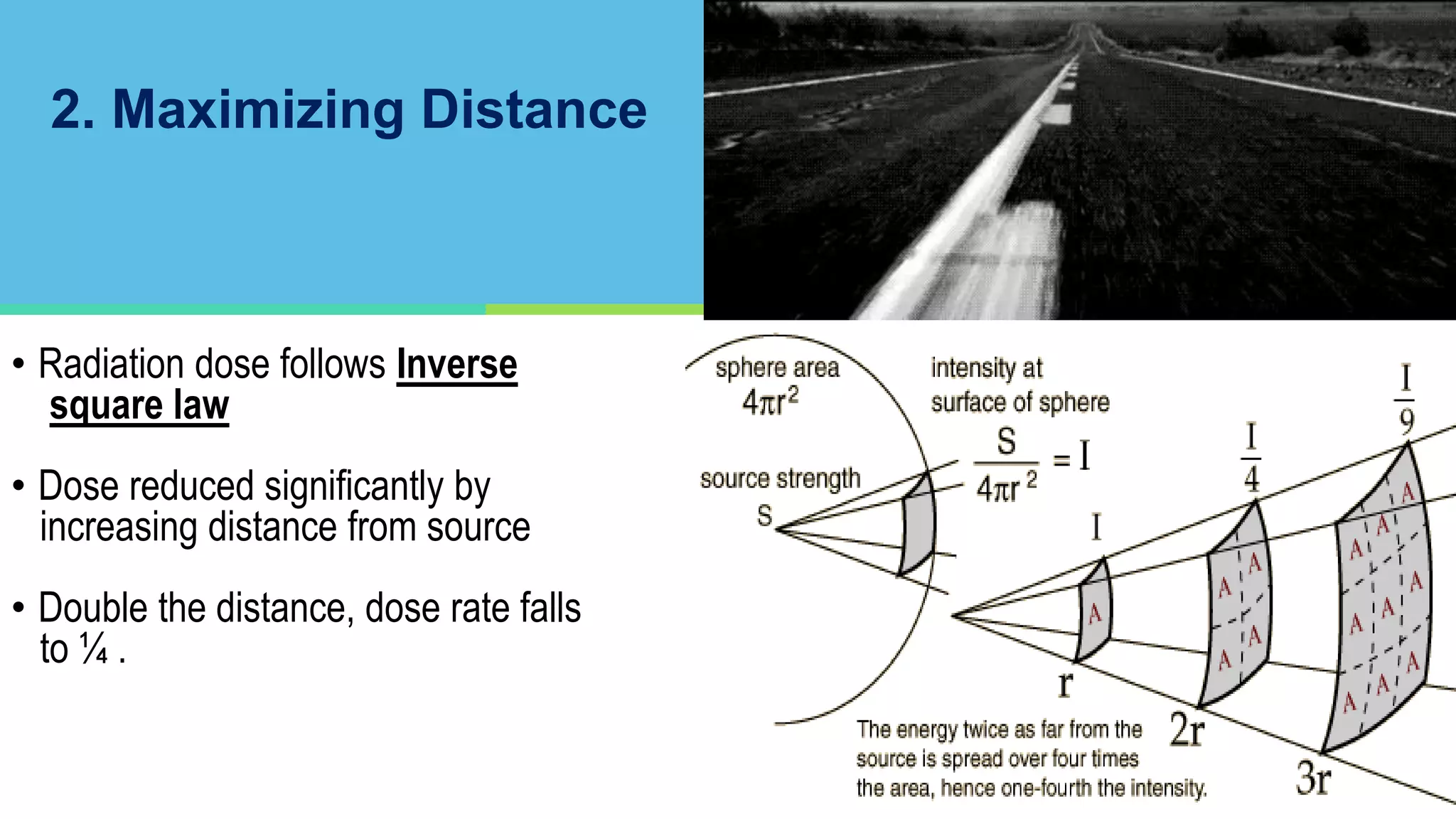
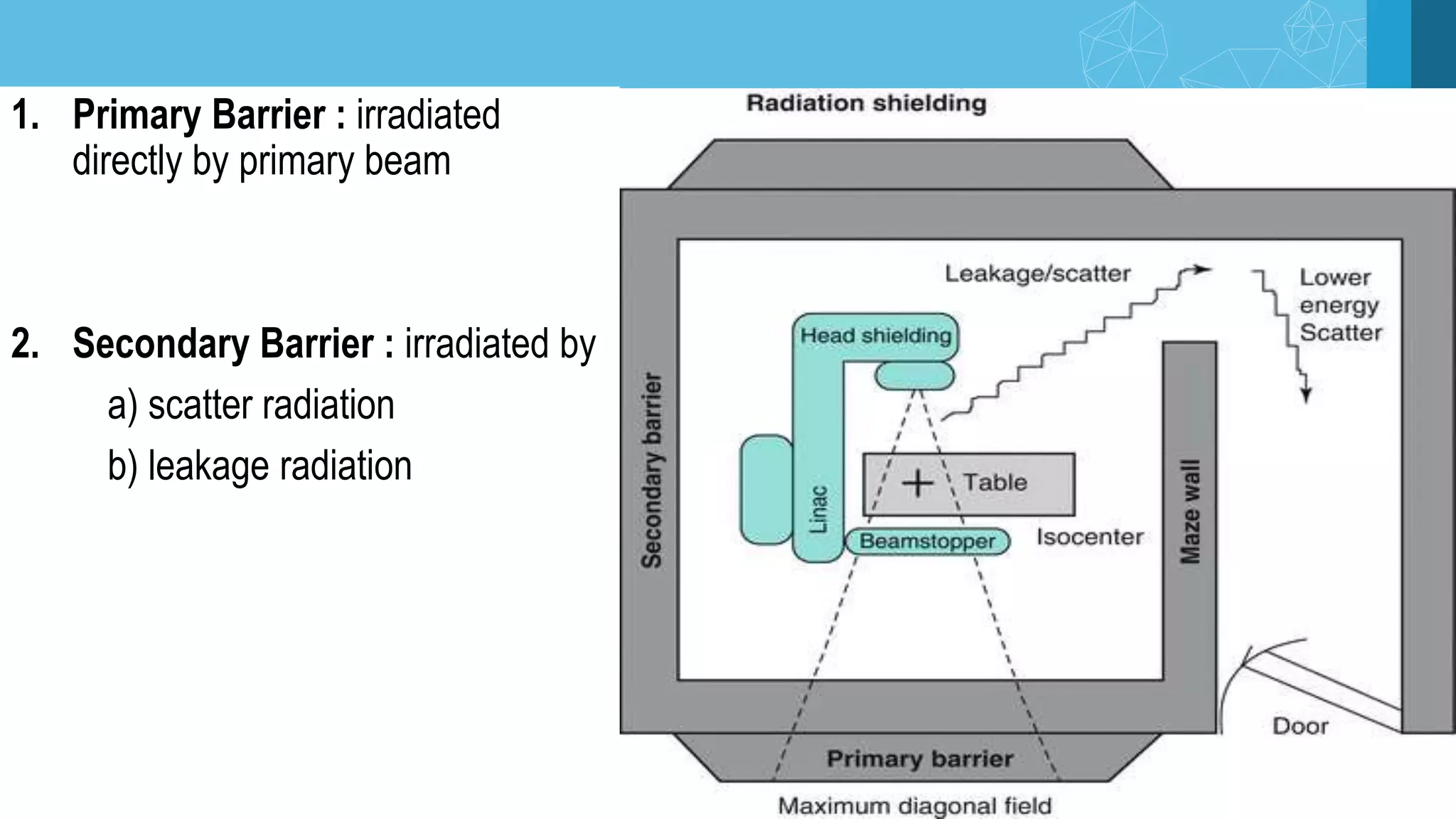
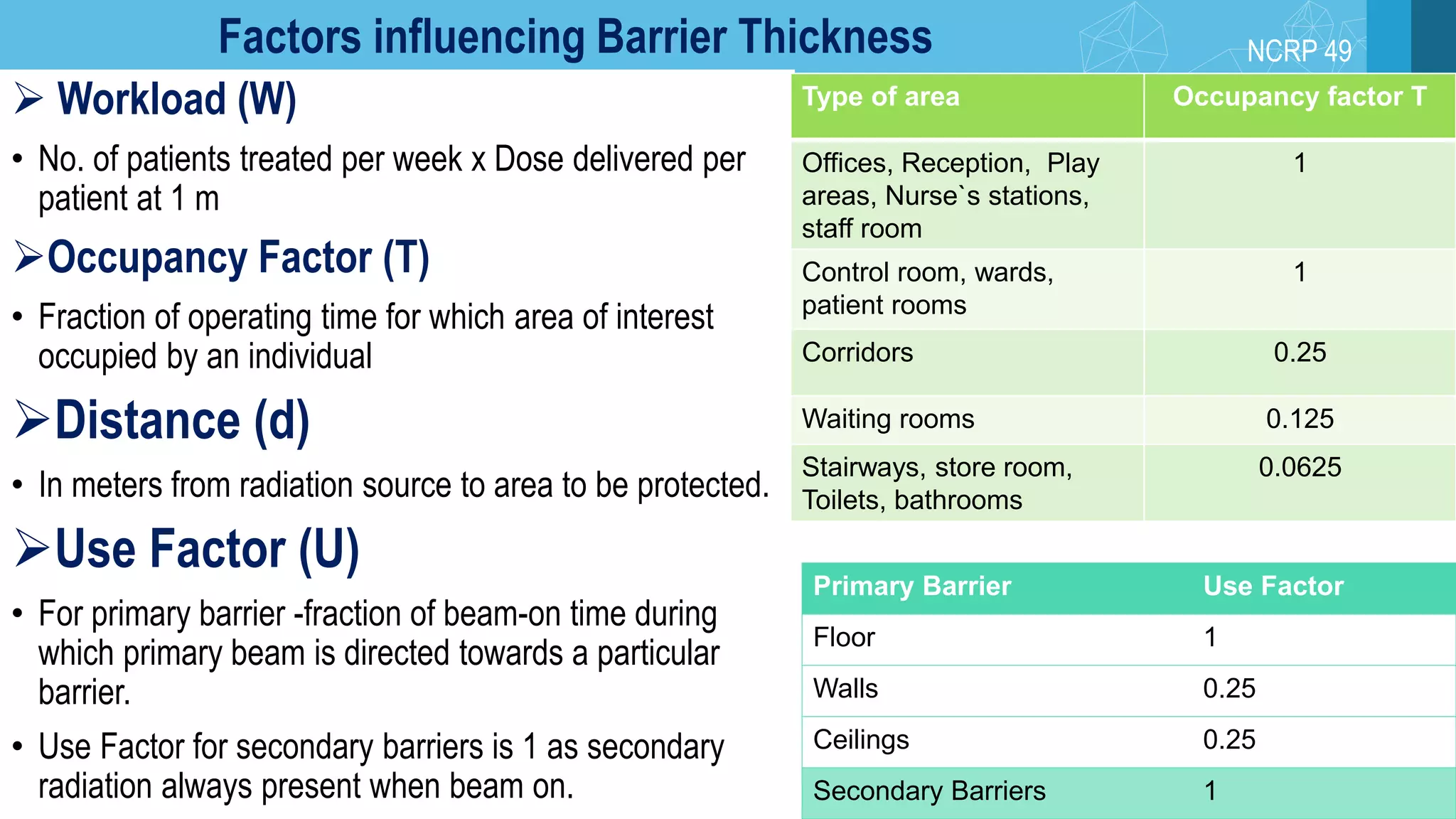
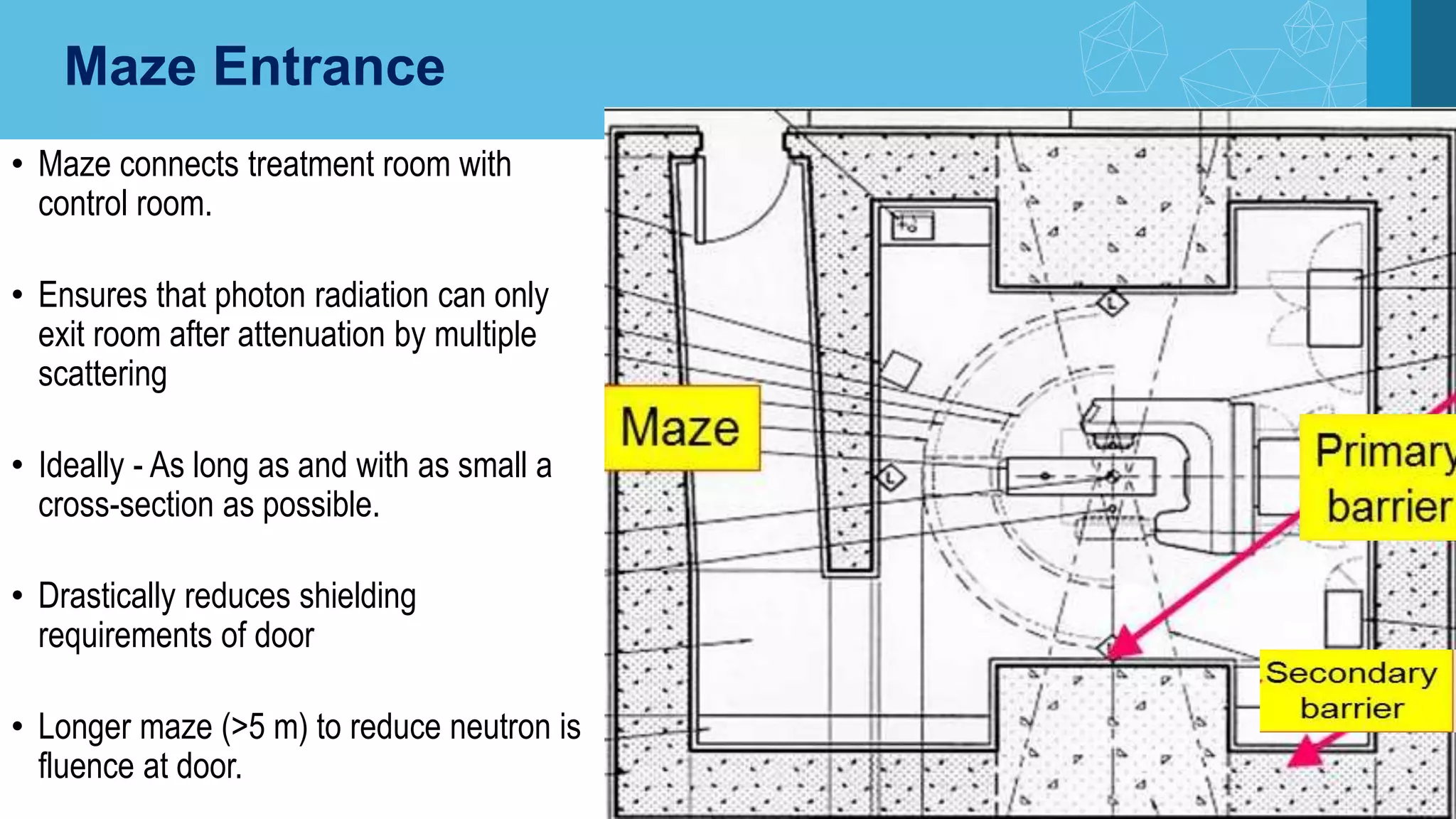
The document covers key aspects of radiation protection including its history, principles, monitoring, and safety regulations. It outlines the roles of various organizations, effects of different types of radiation, and design considerations for radiation facilities. The document also addresses emergency procedures for lost or stuck sources and the responsibilities of employers and safety officers in maintaining safety standards.