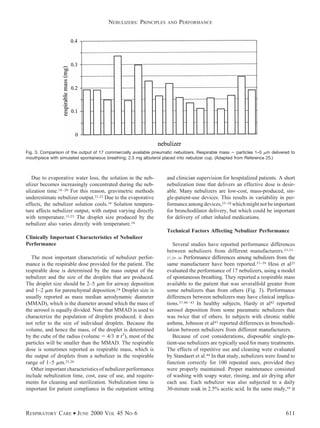
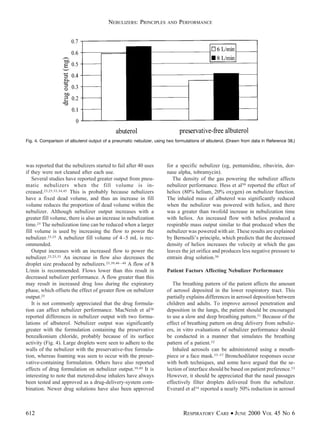
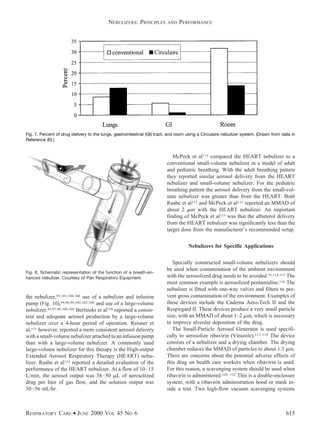
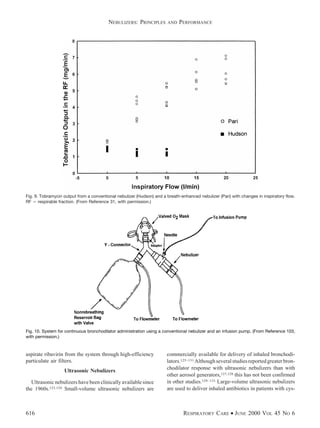
This document discusses the principles and performance of nebulizers. It describes how pneumatic nebulizers work by using compressed gas to break liquid medications into small respirable droplets. Key factors that influence nebulizer performance include the gas flow, fill volume, solution characteristics, and patient breathing pattern. The performance of different nebulizers can vary significantly in terms of respirable dose delivered, droplet size, and nebulization time. Both technical and patient factors need to be considered to optimize drug delivery from nebulizers.
![Nebulizers: Principles and Performance
Dean R Hess PhD RRT FAARC
Introduction
Pneumatic Nebulizers
Principle of Operation
Clinically Important Characteristics of Nebulizer Performance
Technical Factors Affecting Nebulizer Performance
Patient Factors Affecting Nebulizer Performance
Designs to Enhance Nebulizer Performance
Use of Reservoir Bags to Collect Aerosol During the Expiratory Phase
Breath-Enhanced Nebulizers
Breath-Actuated Nebulizers
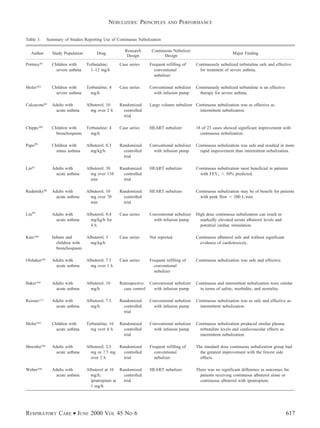
Continuous Nebulization
Nebulizers for Specific Applications
Ultrasonic Nebulizers
Summary
[Respir Care 2000;45(6):609–622] Key words: nebulizer, pneumatic nebu-
lizer, ultrasonic nebulizer, continuous nebulization, aerosol therapy.
Introduction
Nebulizers are used to convert liquids into aerosols of a
size that can be inhaled into the lower respiratory tract.
The process of pneumatically converting a bulk liquid into
small droplets is called atomization. Pneumatic nebulizers
have baffles incorporated into their design so that most of
the droplets delivered to the patient are within the respi-
rable size range of 1–5 m. Ultrasonic nebulizers use
electricity to convert a liquid into respirable droplets.
Although the first choice of aerosol generator for the
delivery of bronchodilators and steroids is the metered-
dose inhaler,1,2 nebulizers remain useful for several rea-
sons. First, some drugs for inhalation are available only in
solution form. Second, some patients cannot master the
correct use of metered-dose inhalers or dry powder inhal-
ers. Third, some patients prefer the nebulizer over other
aerosol generating devices. The physiologic benefits of
metered-dose inhalers and nebulizers are virtually equiv-
alent,3,4 and the choice of device is often based on clini-
cian or patient preference rather than clear superiority of
one approach over the other. Although cost savings have
been suggested with the use of metered-dose inhalers com-
pared to nebulizers, these benefits may be overestimated.3
The purpose of this paper is to review the performance
characteristics of nebulizers. Both pneumatic and ultra-
sonic nebulizer designs will be considered.
Pneumatic Nebulizers
Nebulizers are the oldest form of aerosol generation.
Although they have been commonly used for many years,
their basic design and performance has changed little over
the past 25 years. Nebulizers are most commonly used for
bronchodilator administration, and it is well established
that nebulized bronchodilators produce a physiologic re-
sponse. Because bronchodilators are relatively inexpen-
sive, there is little market pressure to improve nebulizer
performance. In fact, the market generally prefers an in-
expensive nebulizer rather than a high-performance neb-
Dean R Hess PhD RRT FAARC is affiliated with Massachusetts General
Hospital and Harvard Medical School, Boston, Massachusetts.
A version of this paper was presented by Dr Hess during the RESPIRA-
TORY CARE Journal Consensus Conference, “Aerosols and Delivery De-
vices,” held September 24–26, 1999 in Bermuda.
Correspondence: Dean R Hess PhD RRT FAARC, Respiratory Care,
Ellison 401, Massachusetts General Hospital, 55 Fruit Street, Boston MA
02114. E-mail: dhess@partners.org
RESPIRATORY CARE • JUNE 2000 VOL 45 NO 6 609](https://image.slidesharecdn.com/principlesfornebulization-170711150403/75/Principles-for-nebulization-1-2048.jpg)