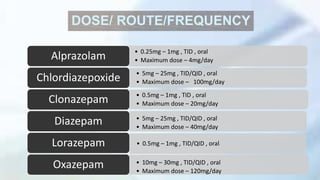
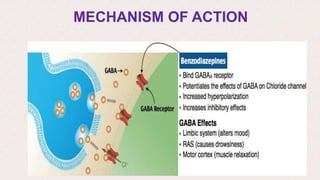
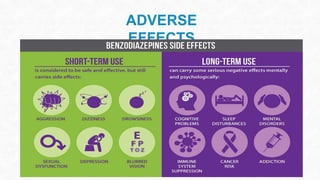
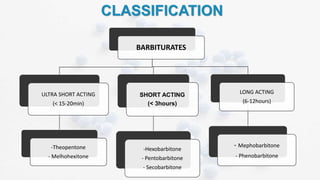
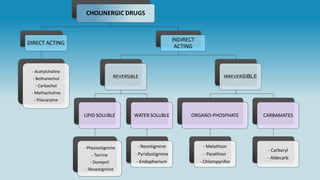
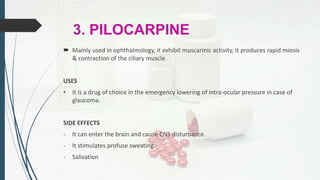
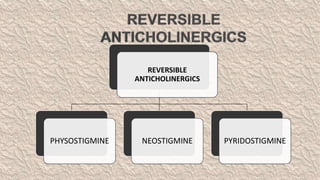
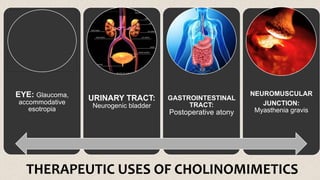
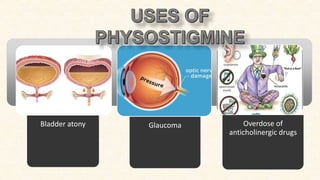
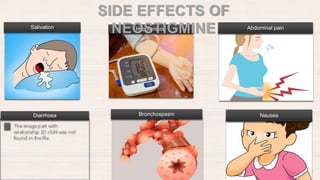
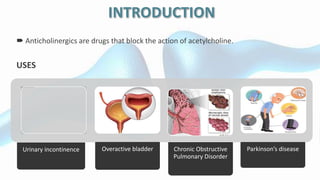
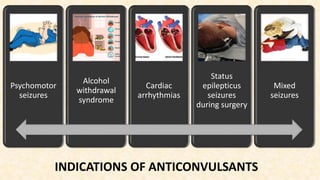
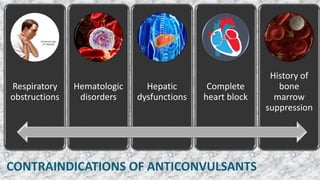
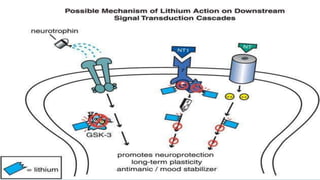
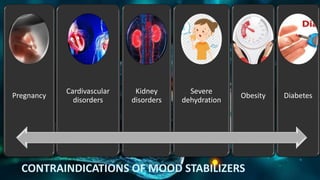
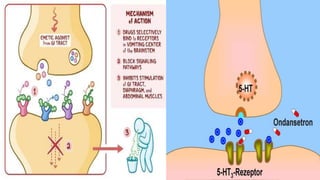
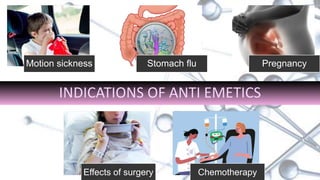
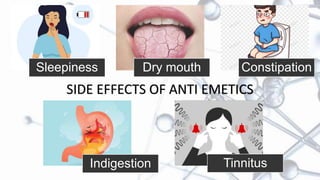
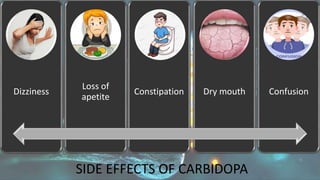
This document provides an overview of neuropharmacology and various central nervous system agents that act on the brain and spinal cord. It discusses the two main branches of neuropharmacology - behavioural and molecular neuropharmacology. It then covers various drug classes that act on the central nervous system including sedatives/hypnotics like benzodiazepines, barbiturates, and cholinergic drugs. Specific drugs are discussed in terms of their mechanisms of action, indications, dosages, and side effects. The document concludes with nursing responsibilities when administering these central nervous system agents.