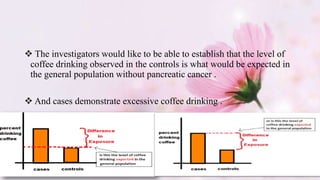
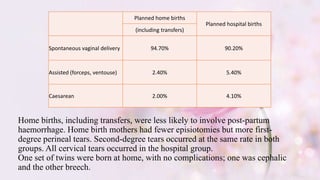
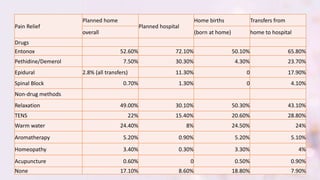
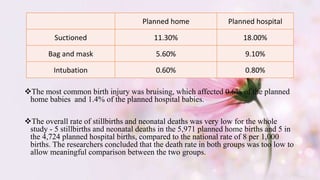
- This study followed women who booked home births in the UK in 1994 and matched them to similar women who booked hospital births.
- Outcomes were recorded for 5,971 home birth women and 4,724 matched hospital birth women. The groups were low-risk and well-matched.
- Planning a home birth was found to halve the chances of assisted or caesarean births compared to planning a hospital birth. Home births also had less reported high blood pressure and less stressful antenatal care.
- However, bias may exist since home birth women tended to be more educated/affluent and high-risk women who transferred care were excluded.