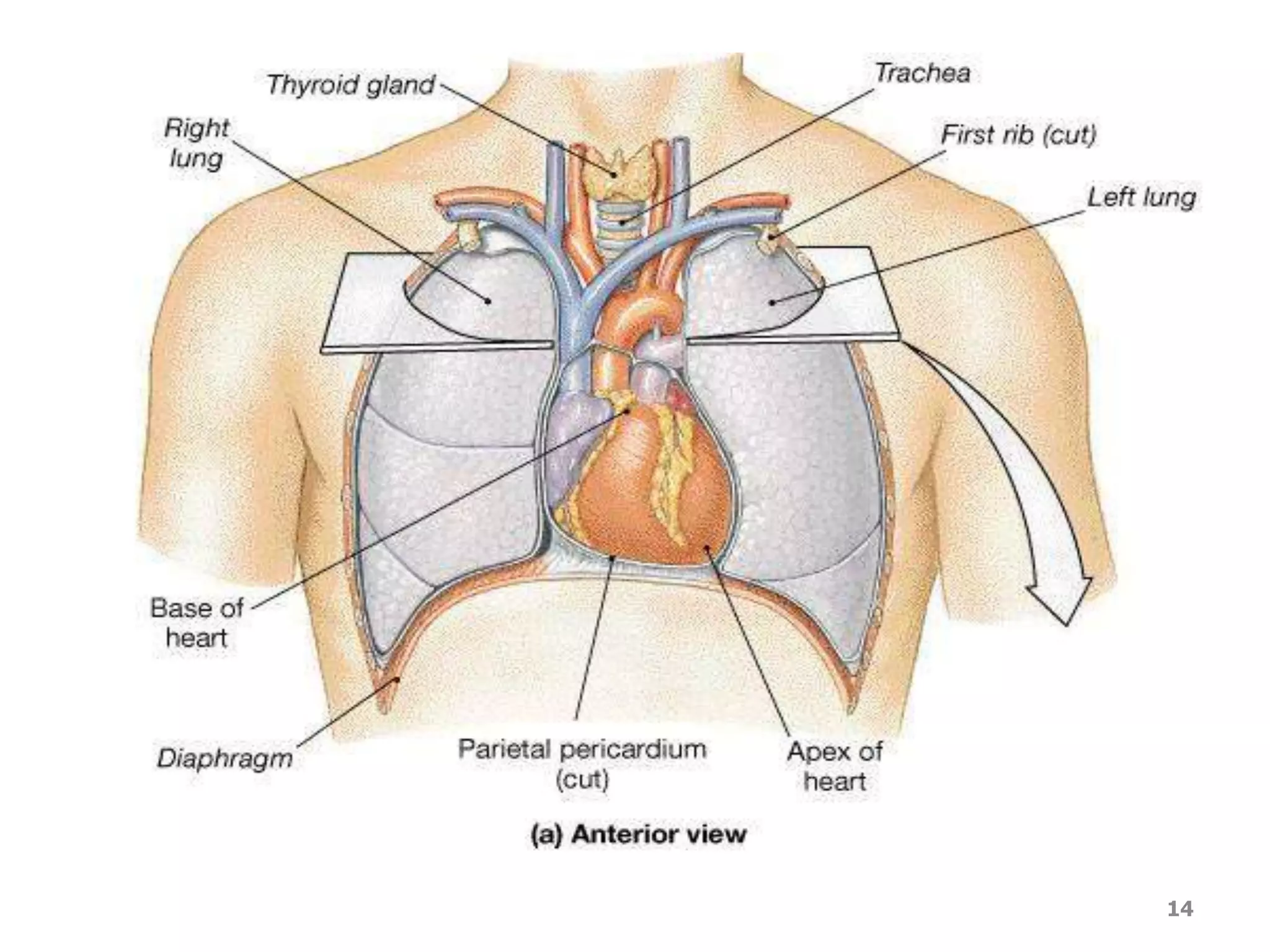
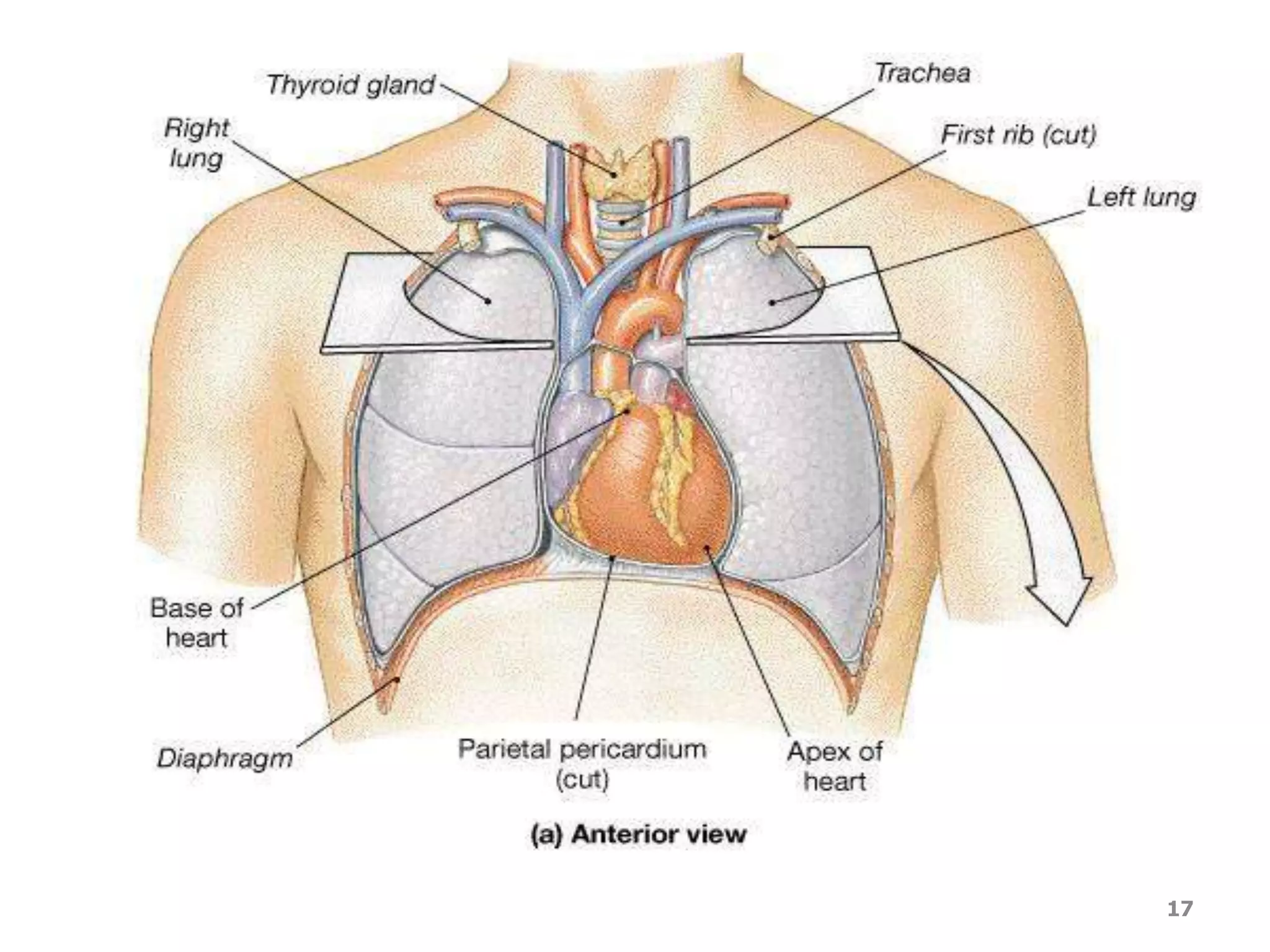
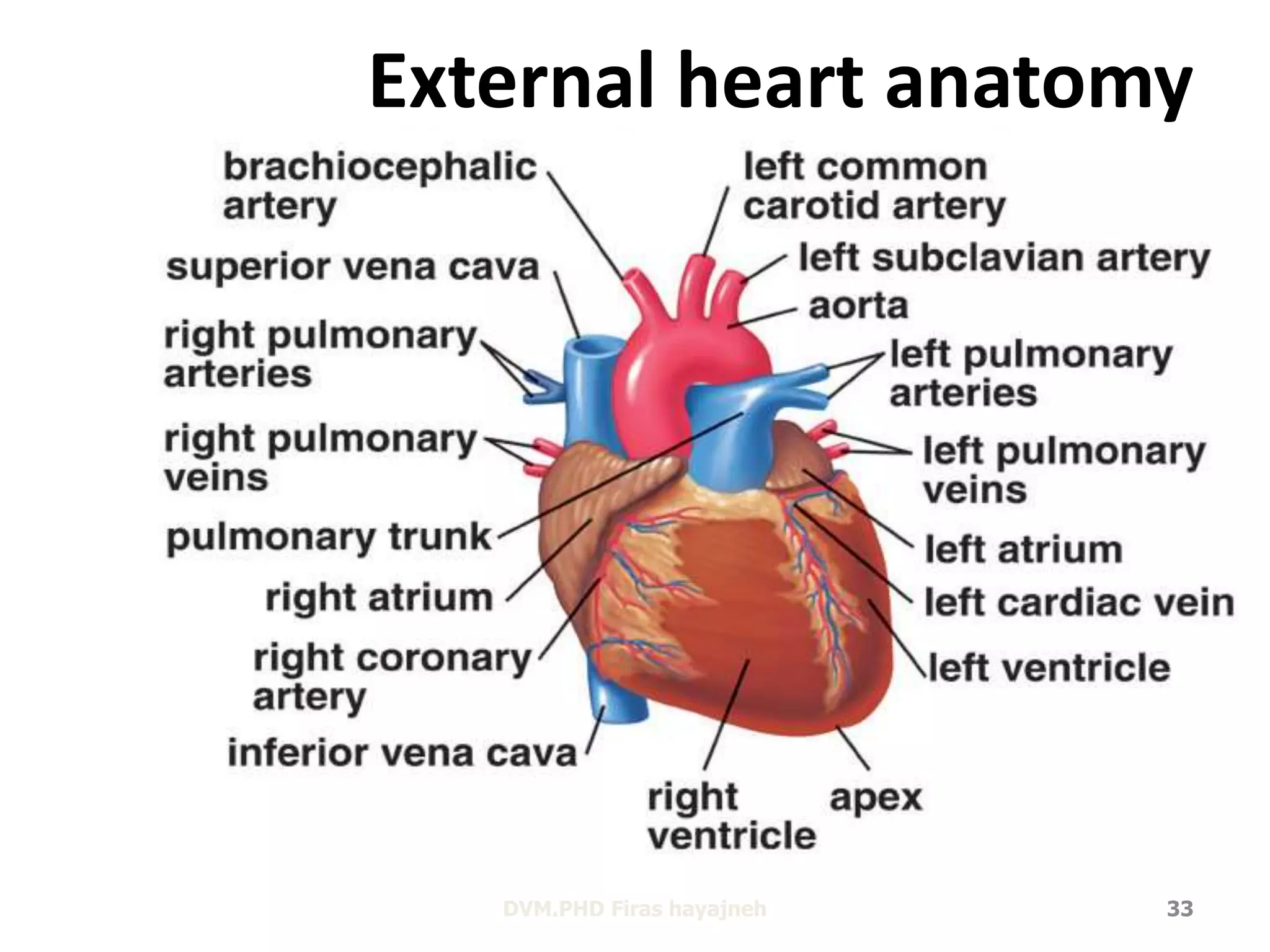
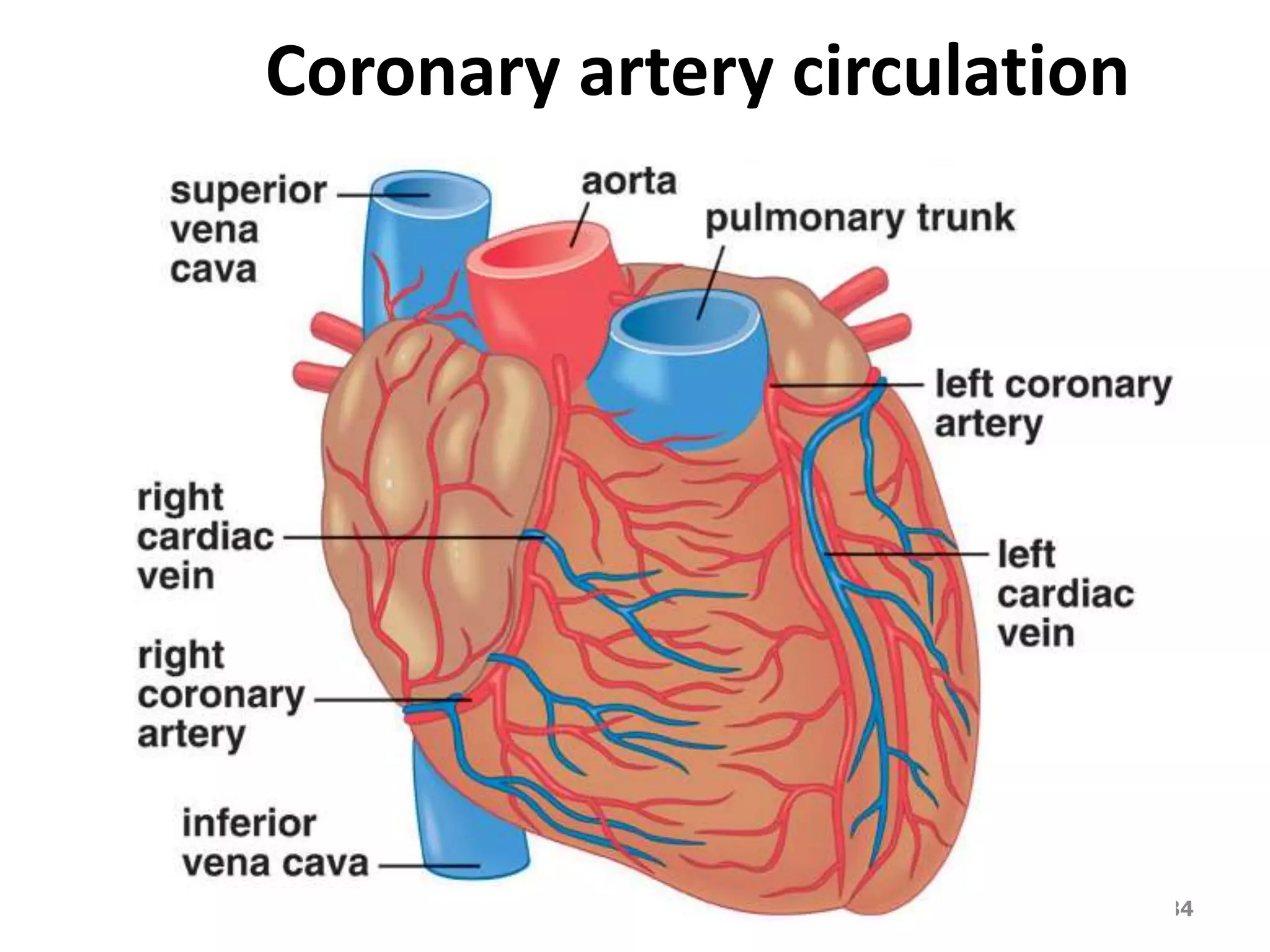
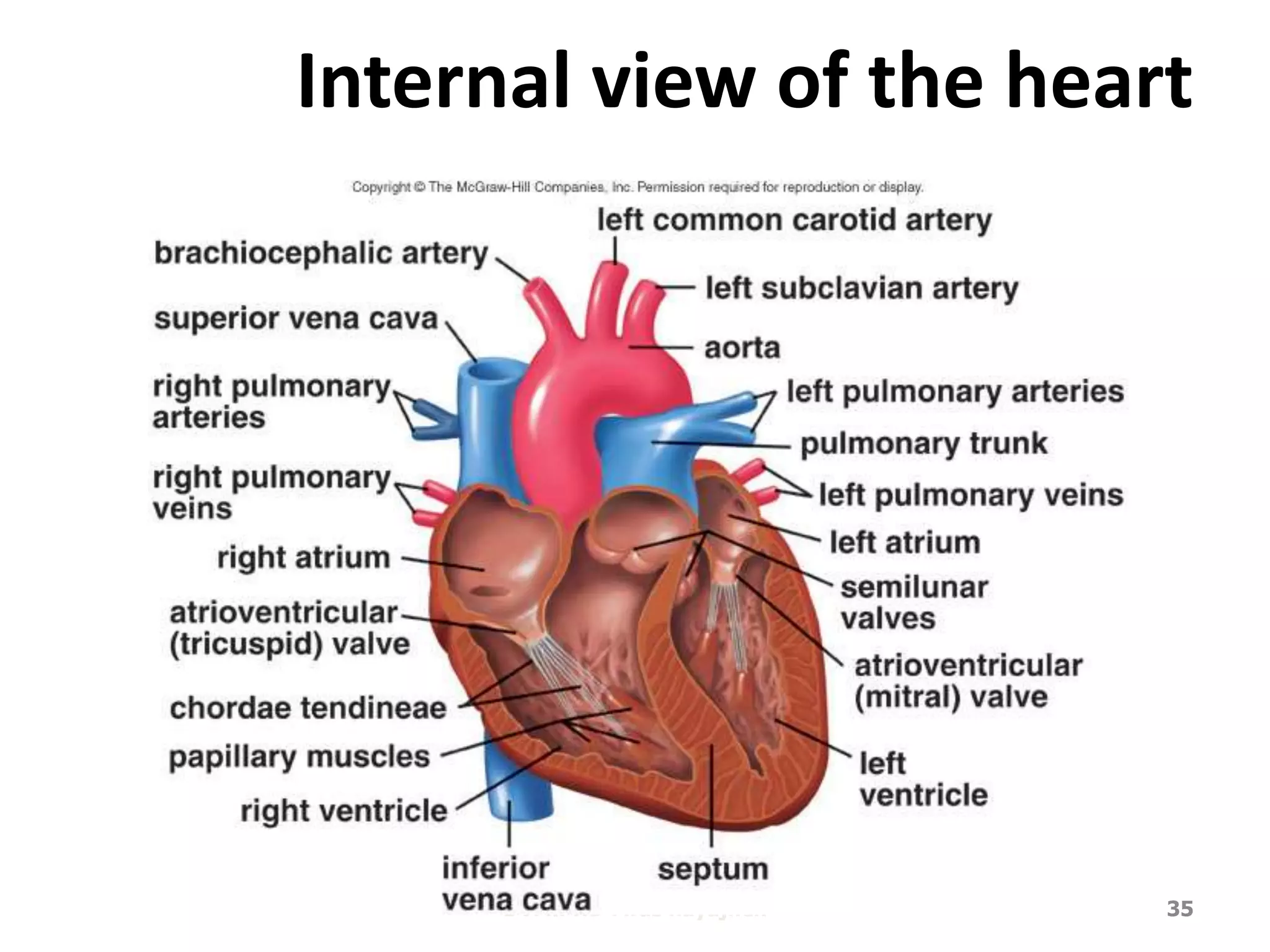
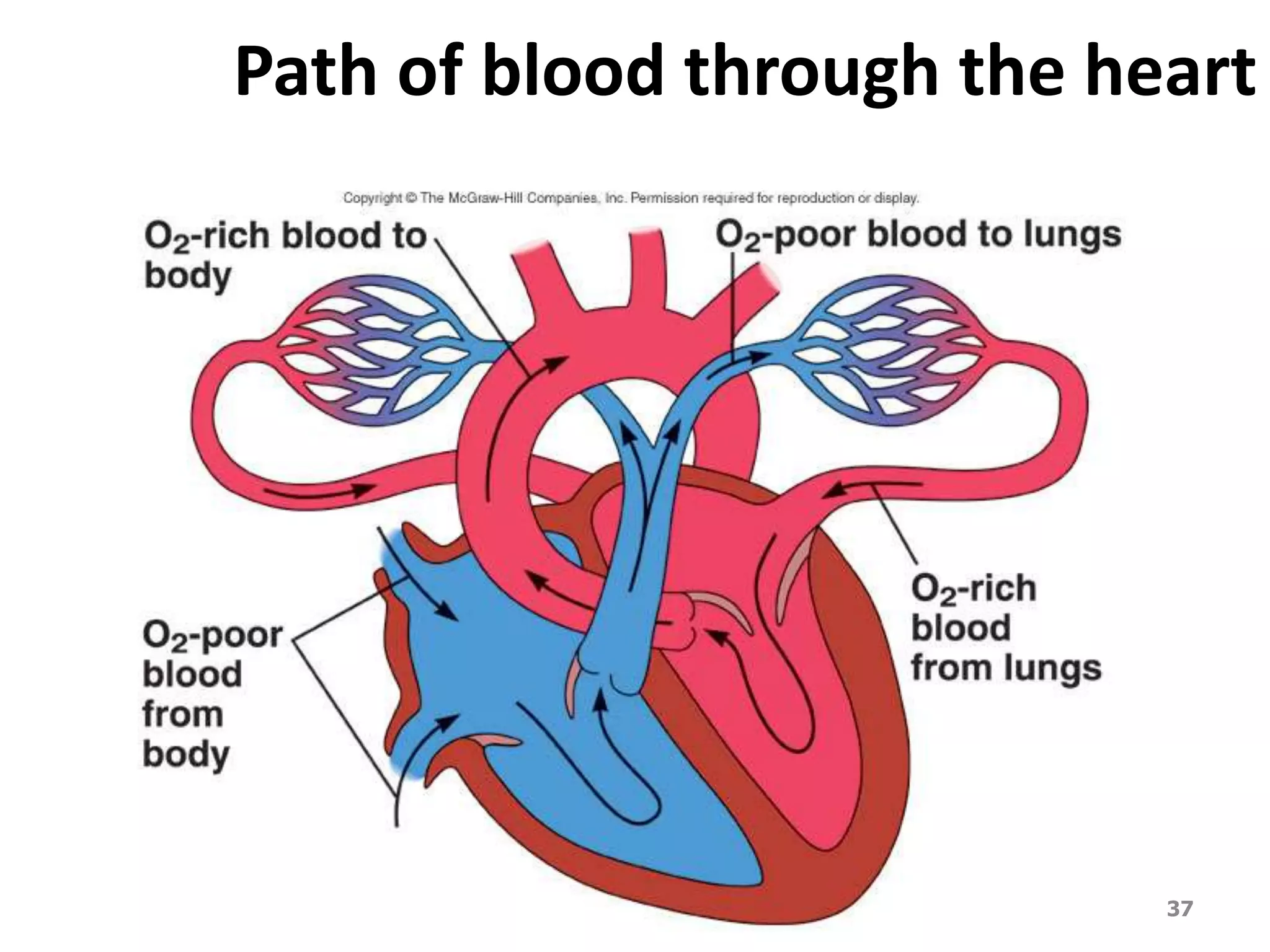
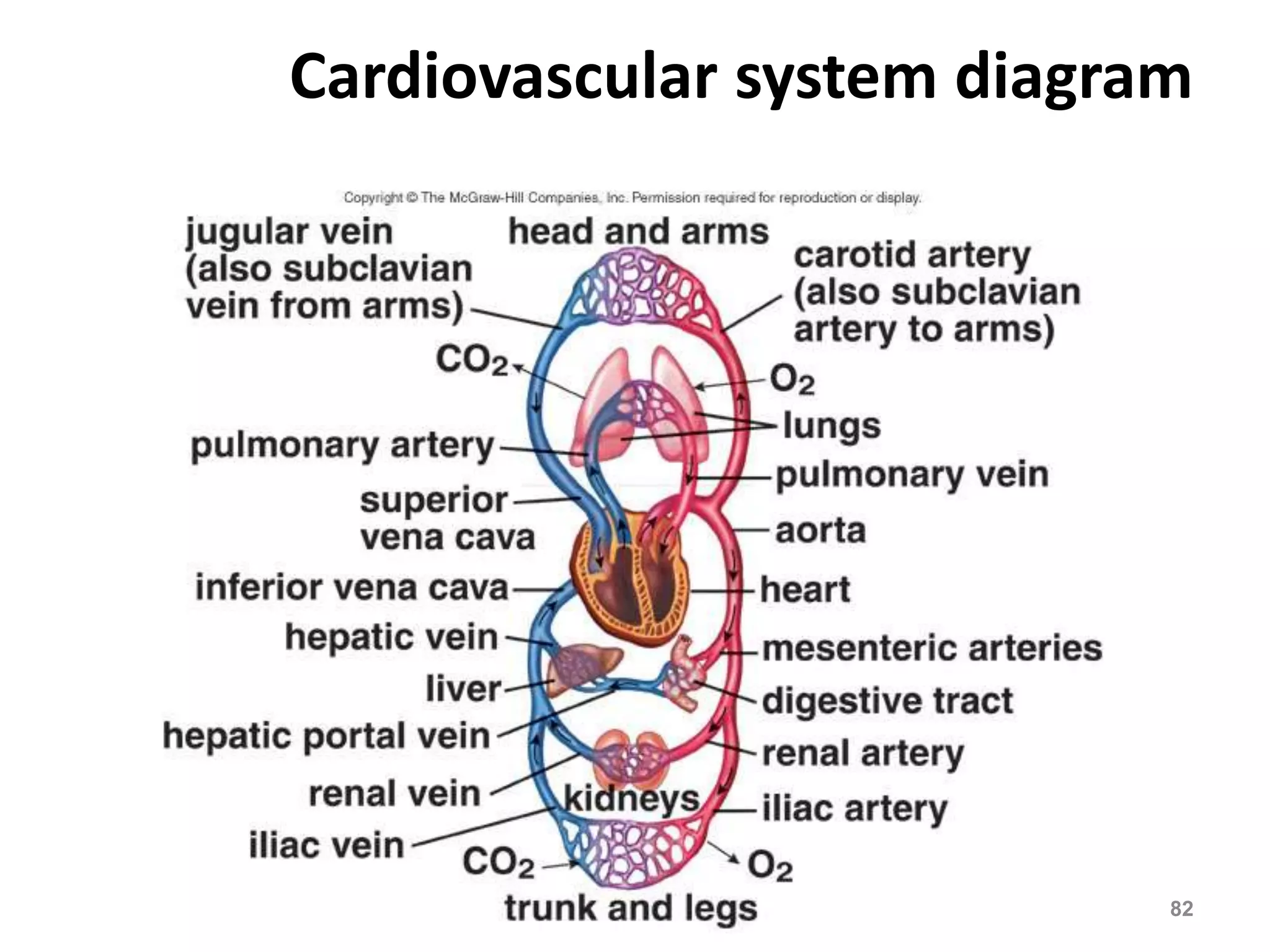
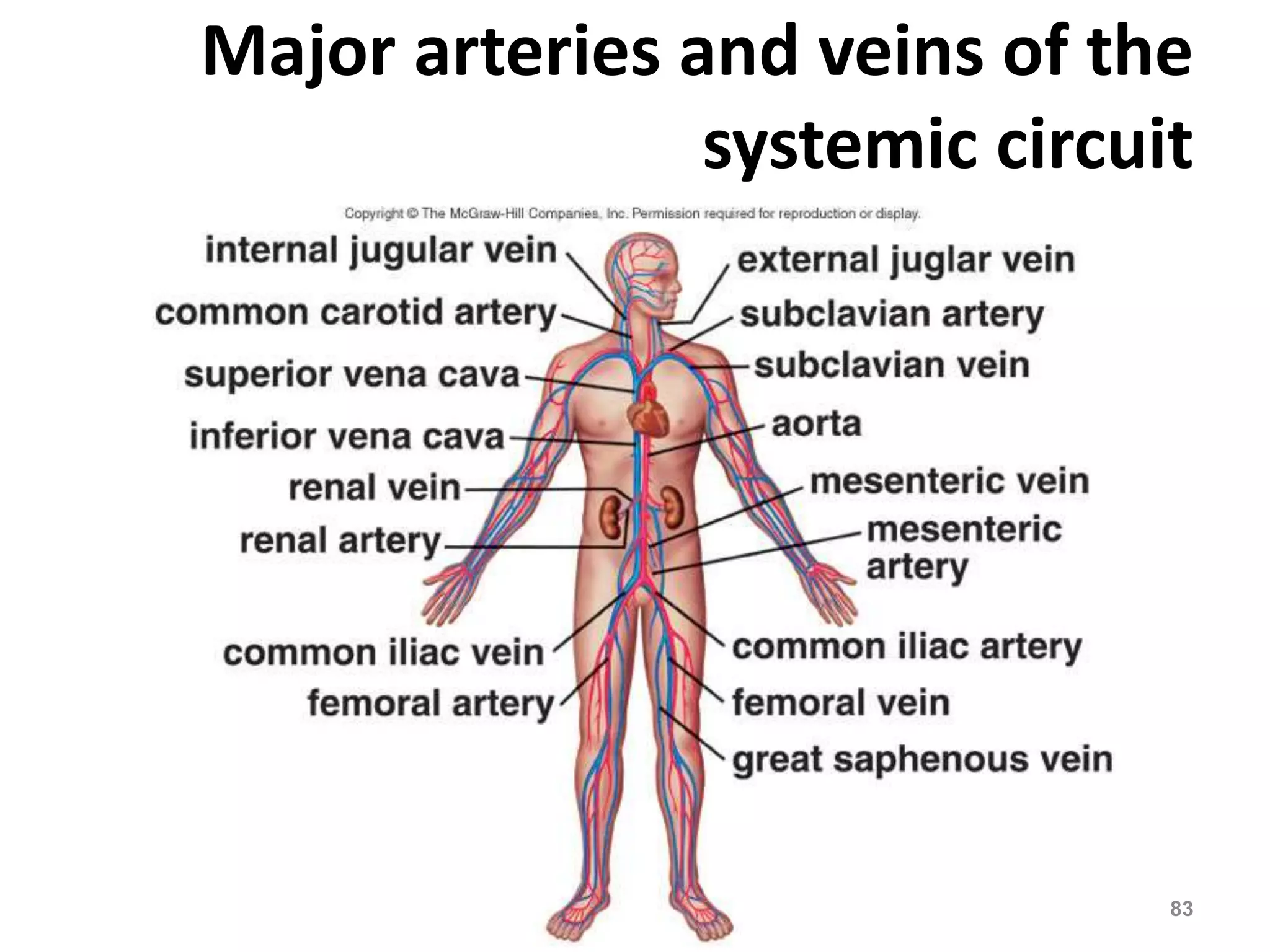
The cardiovascular system delivers oxygen and nutrients to tissues and removes waste. It has three main components:
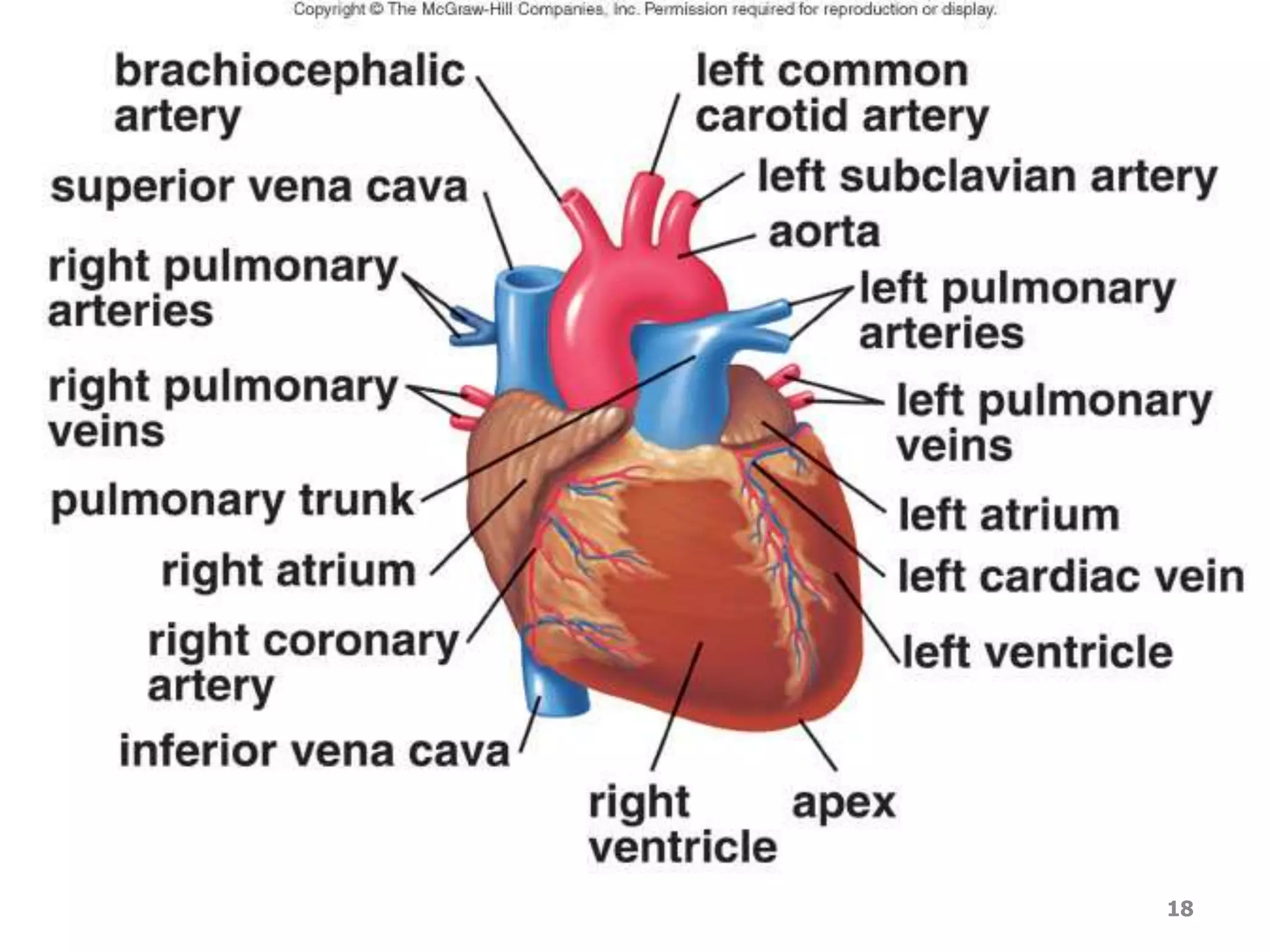
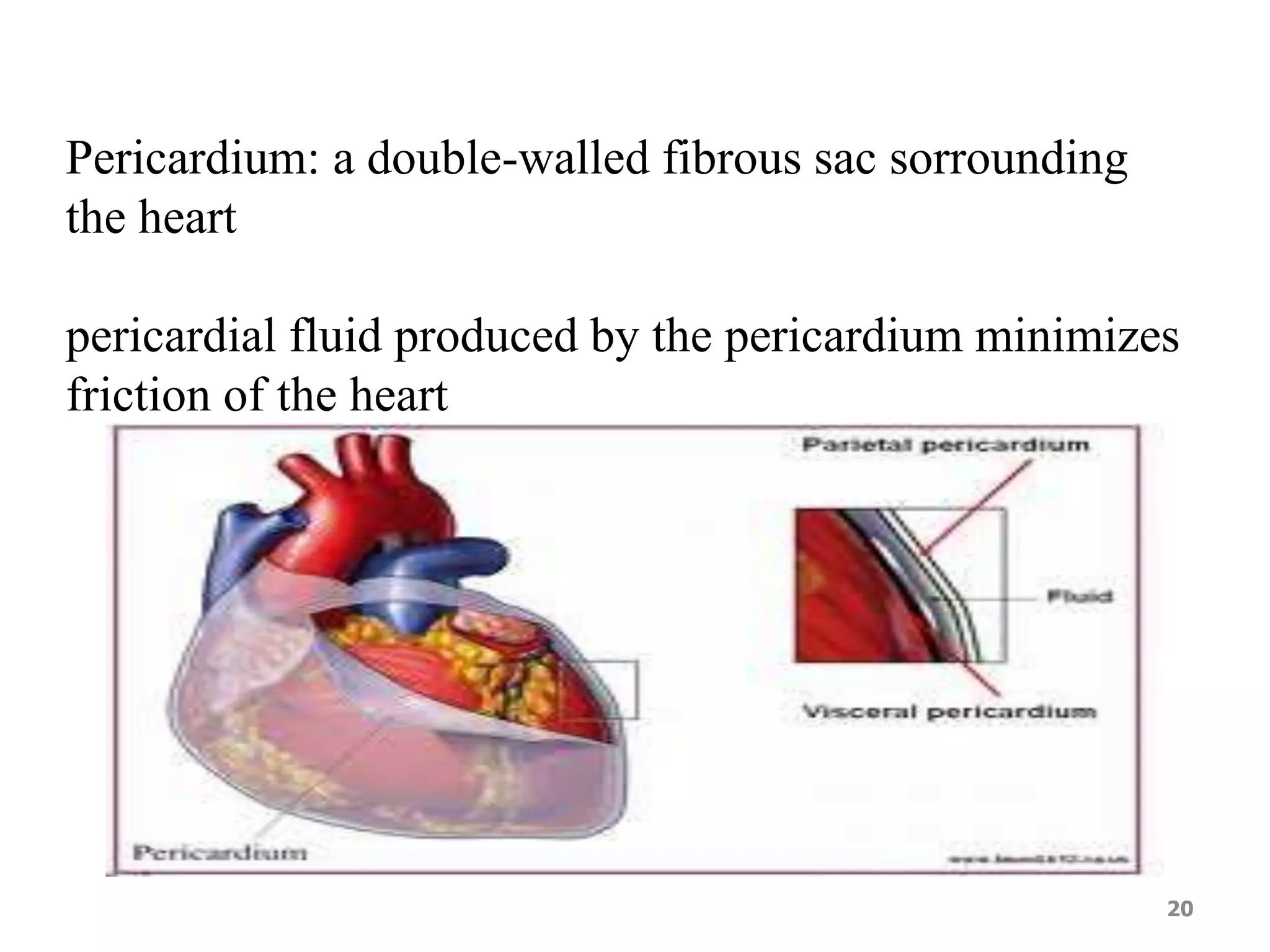
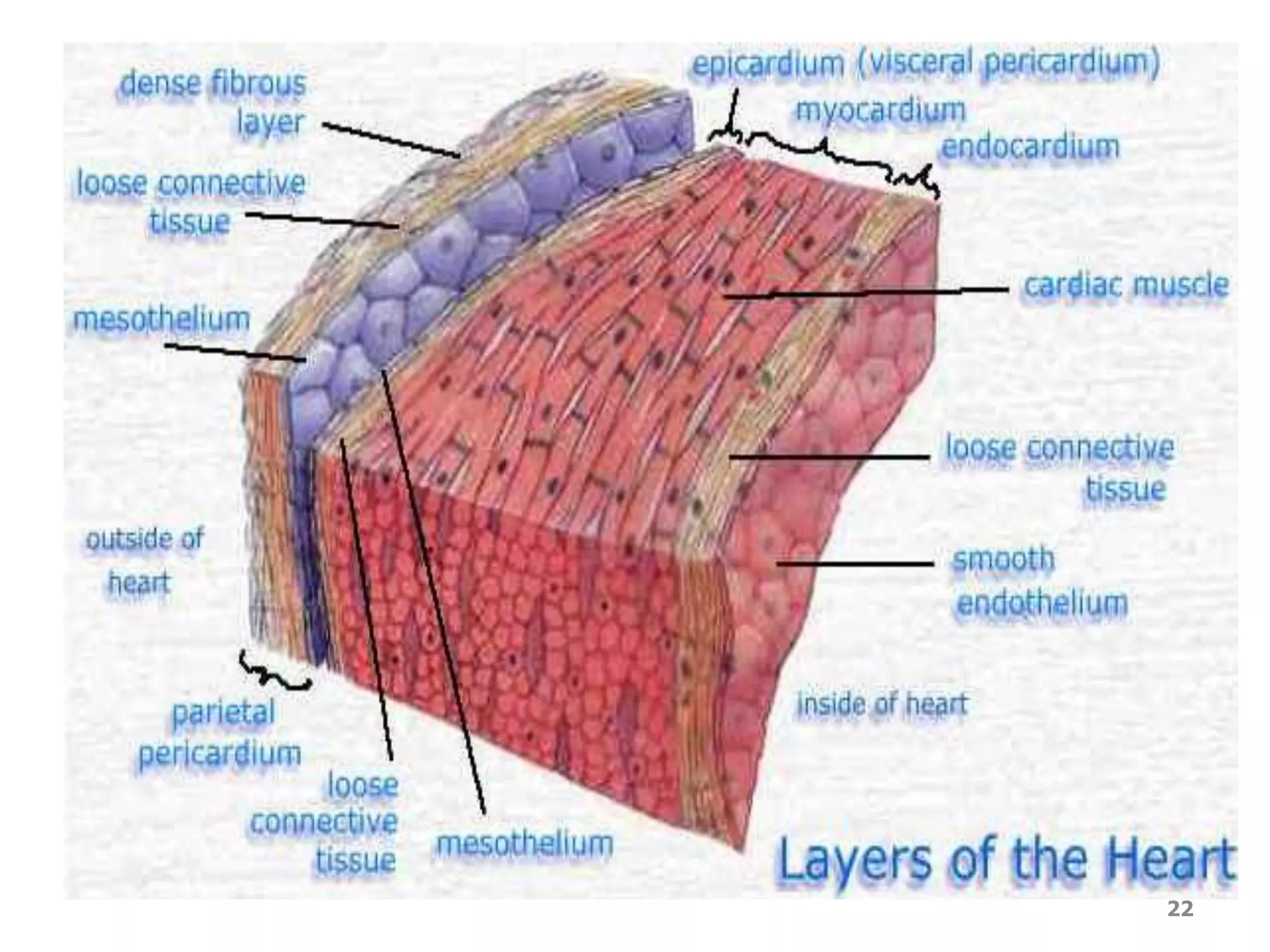
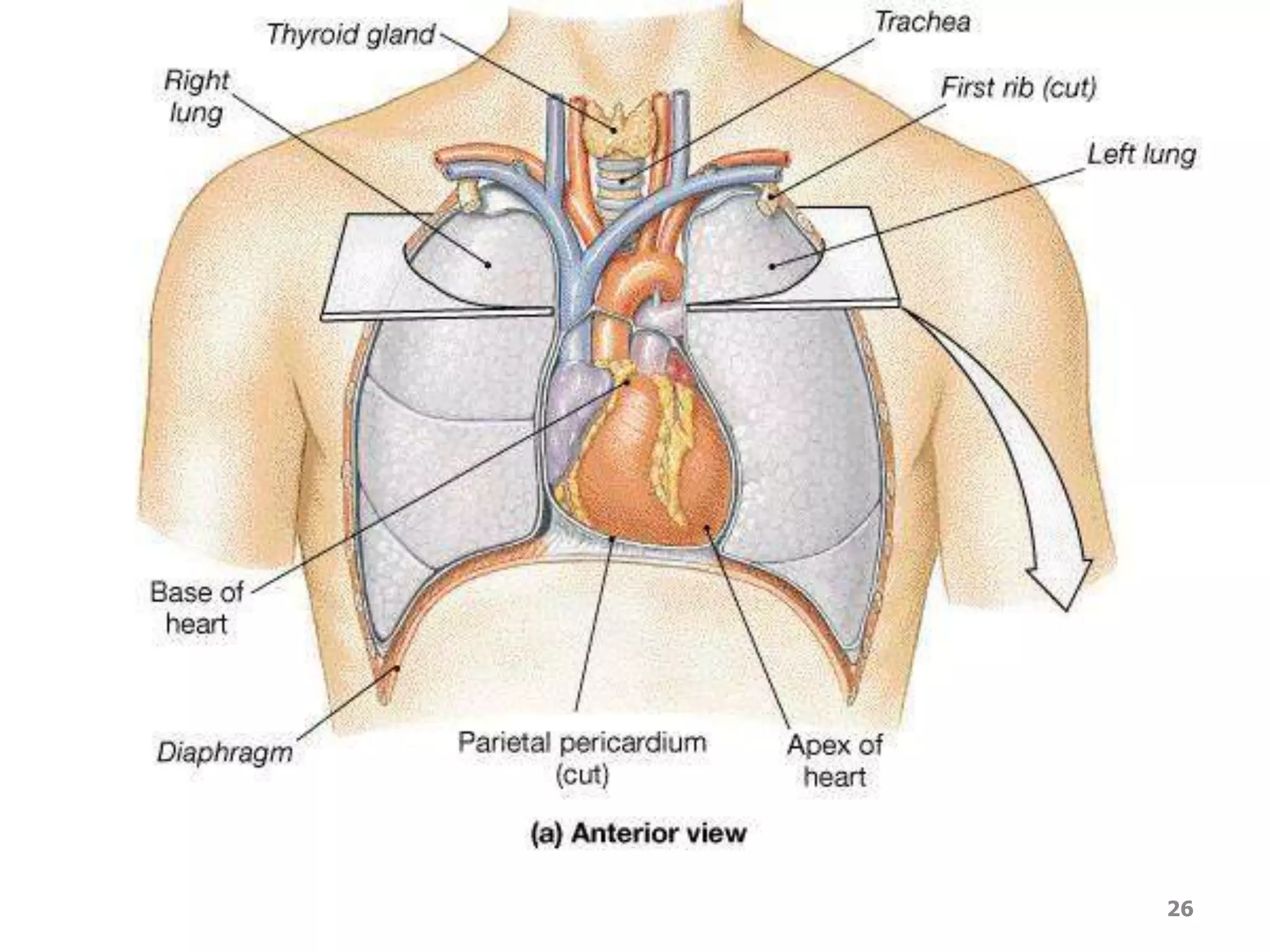
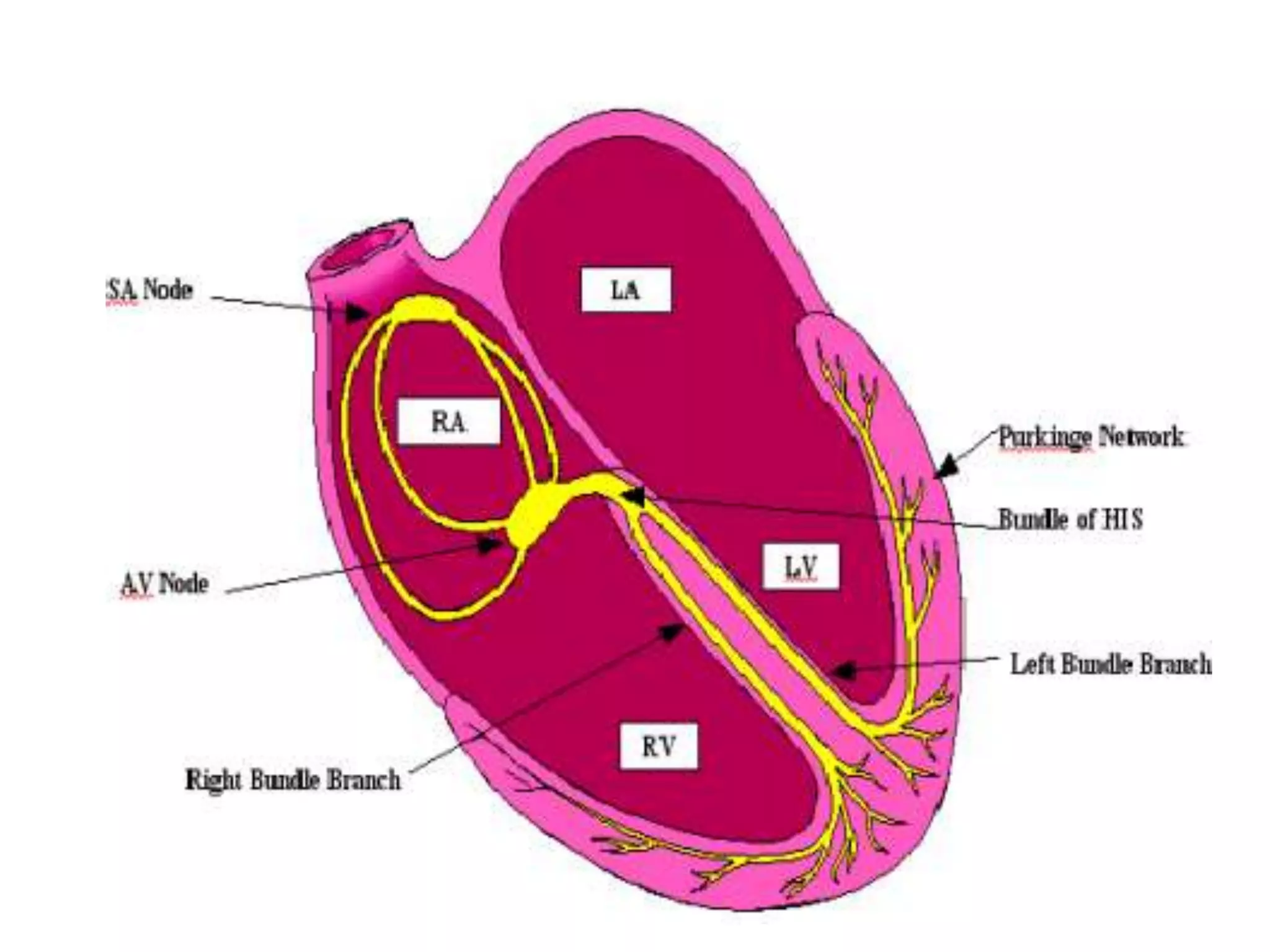
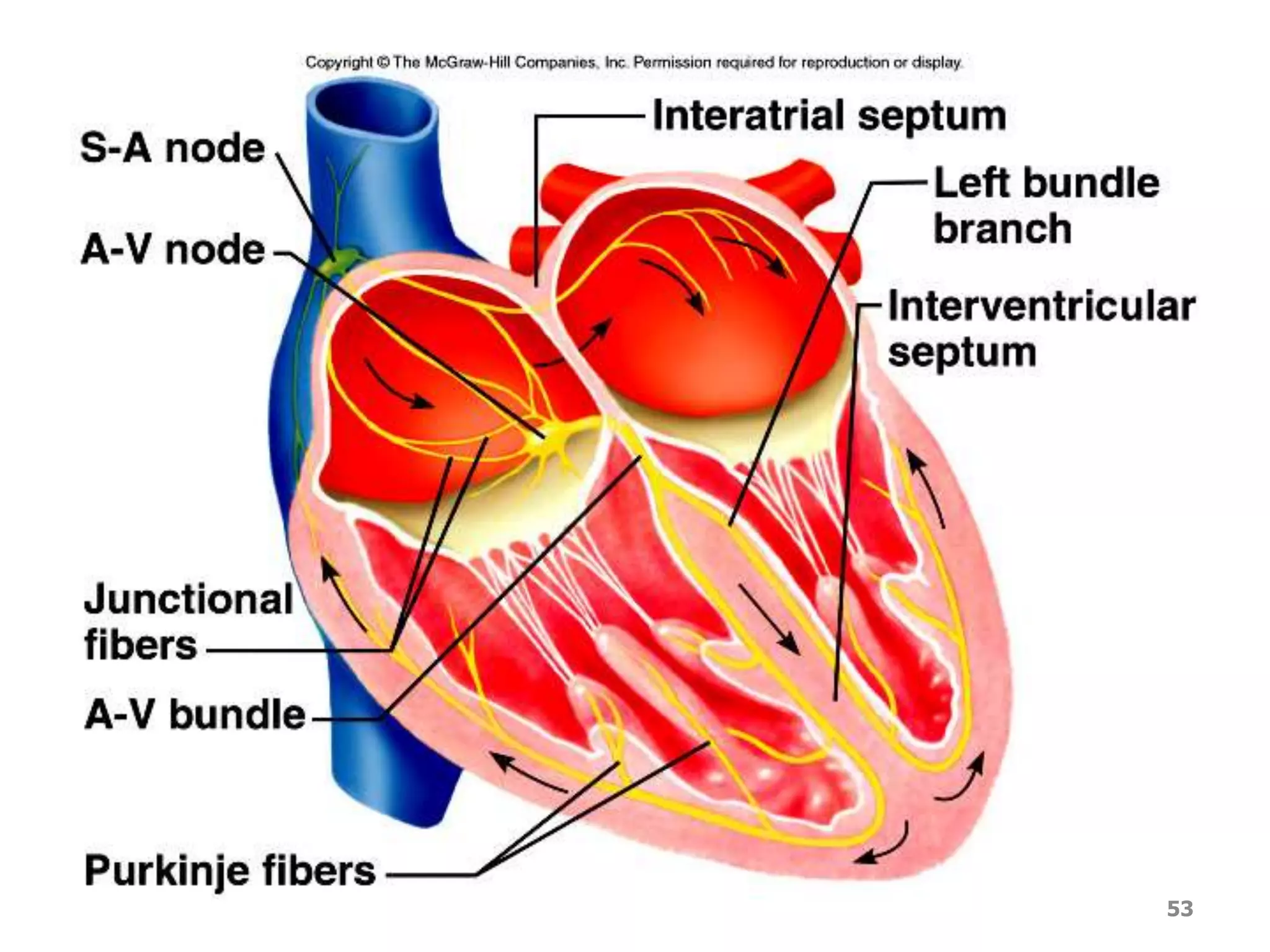
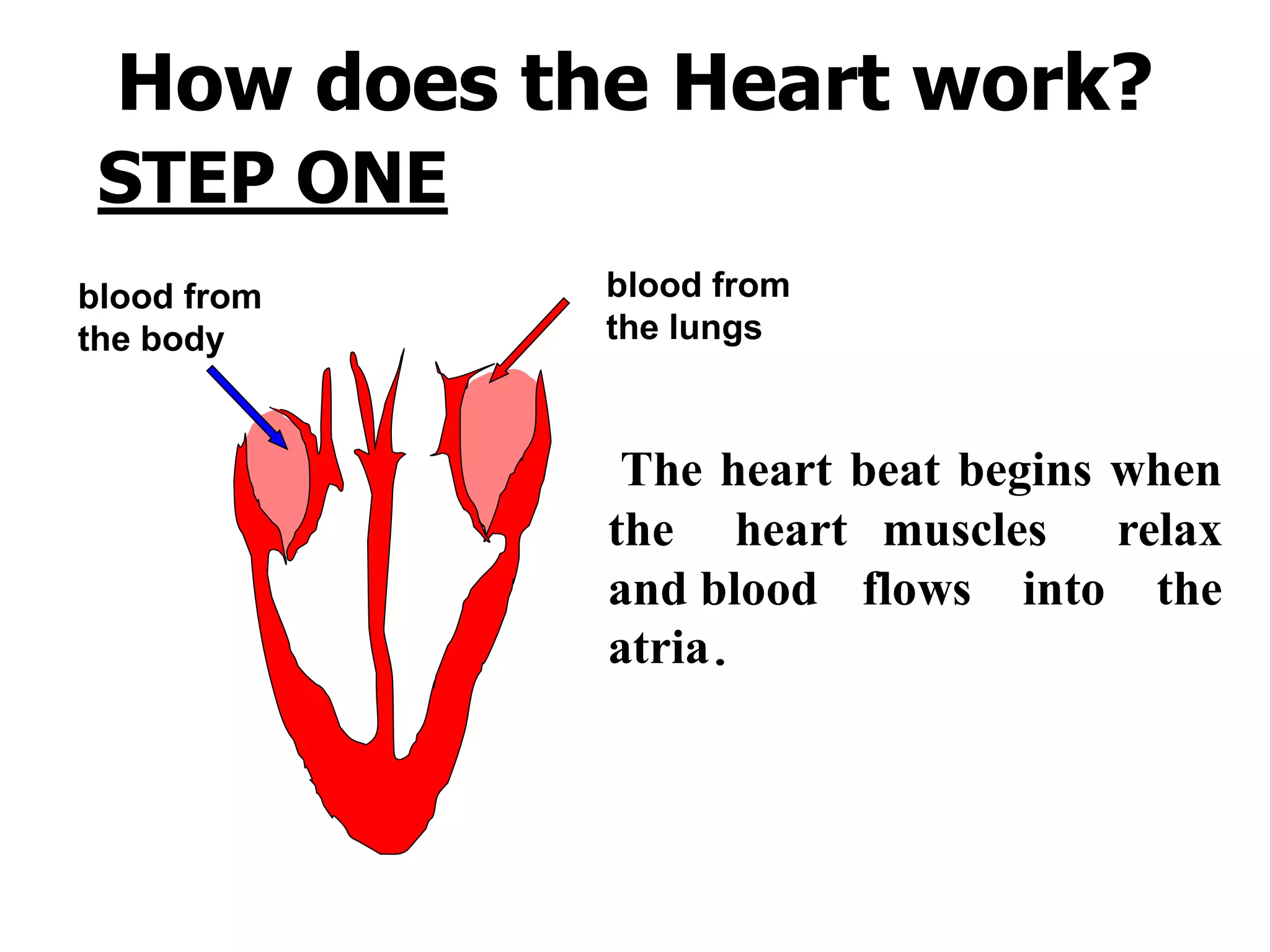
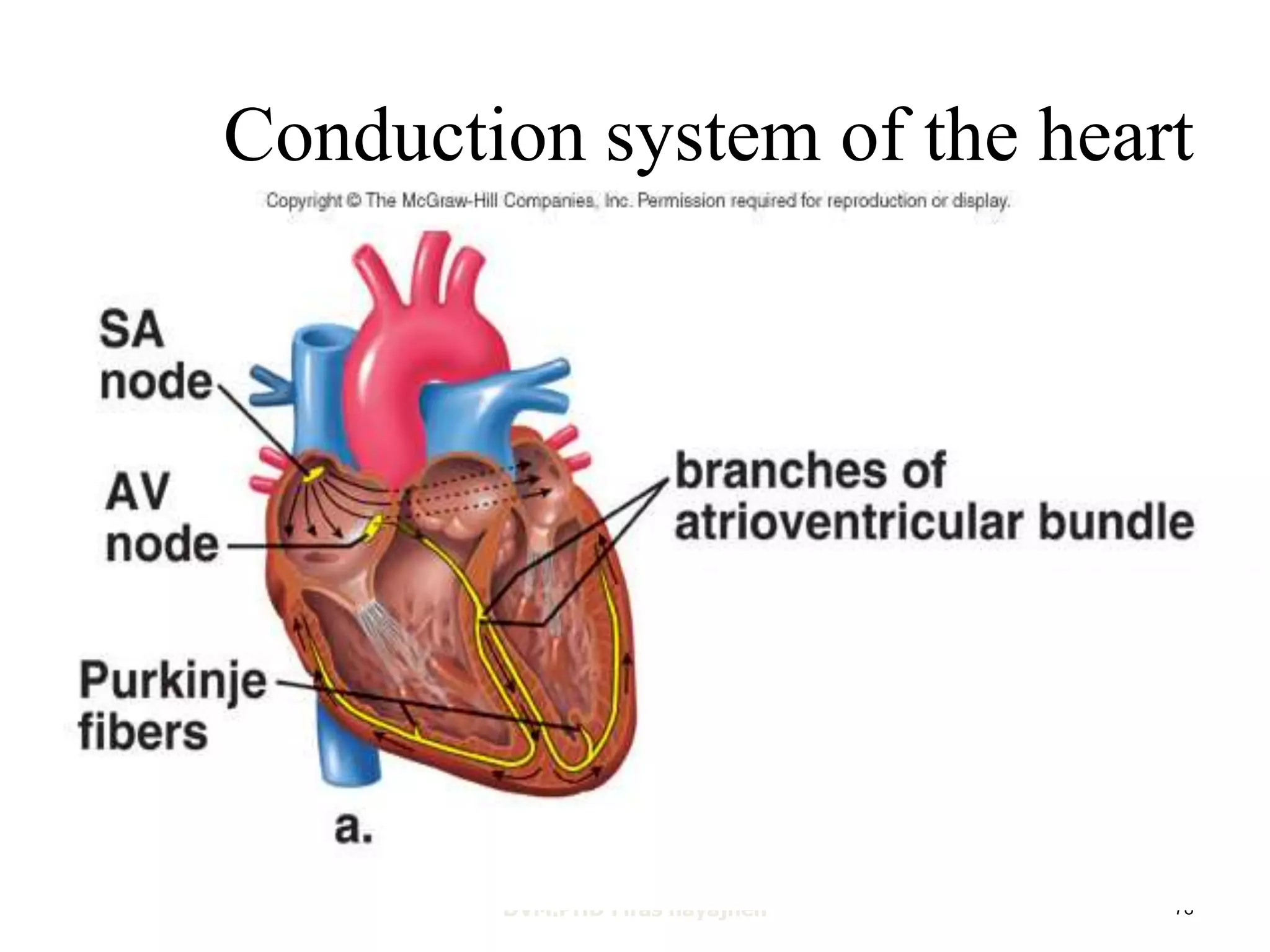
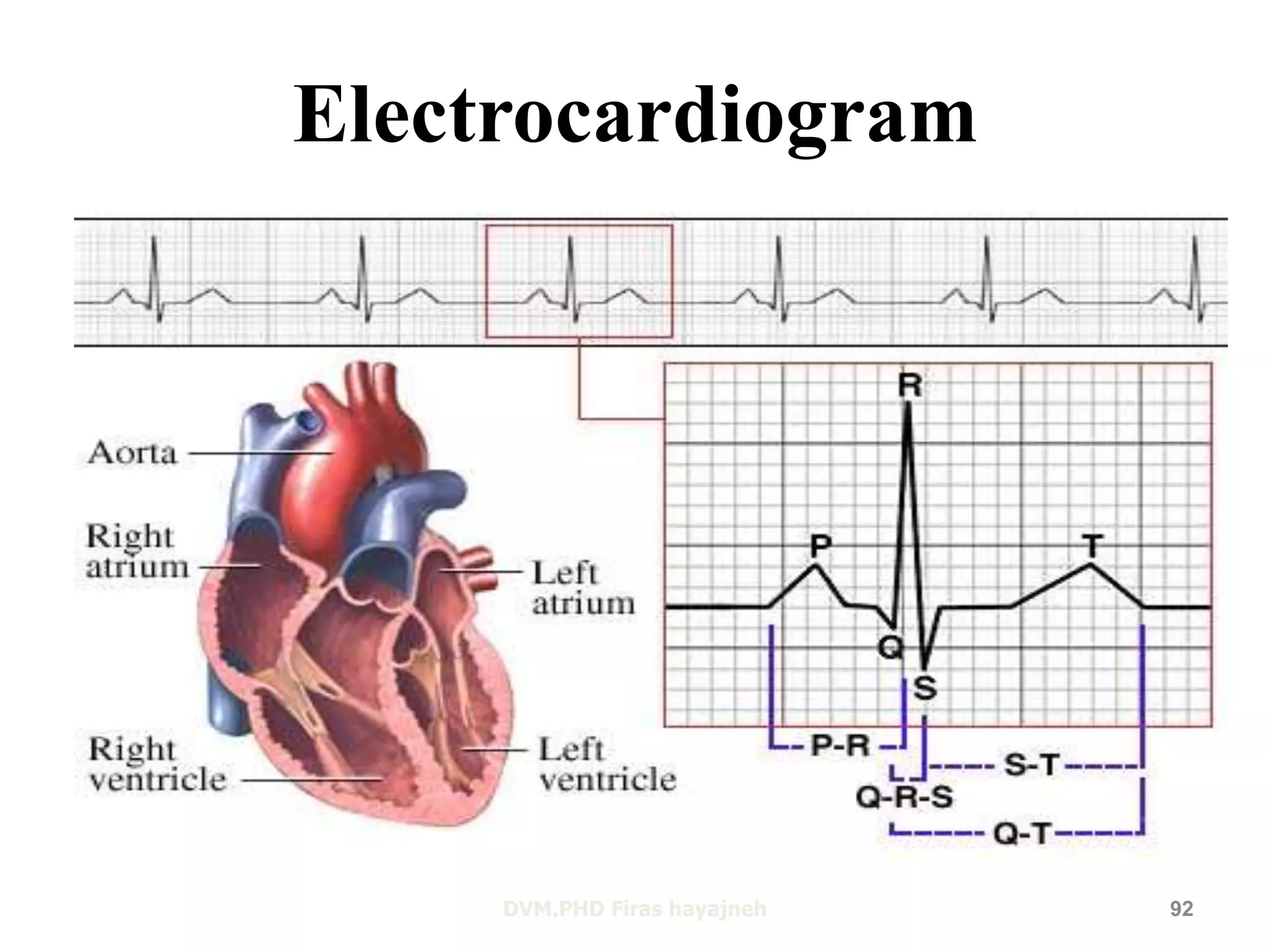
1. The heart, which is a muscular pump located in the chest cavity with four chambers that drive blood circulation.
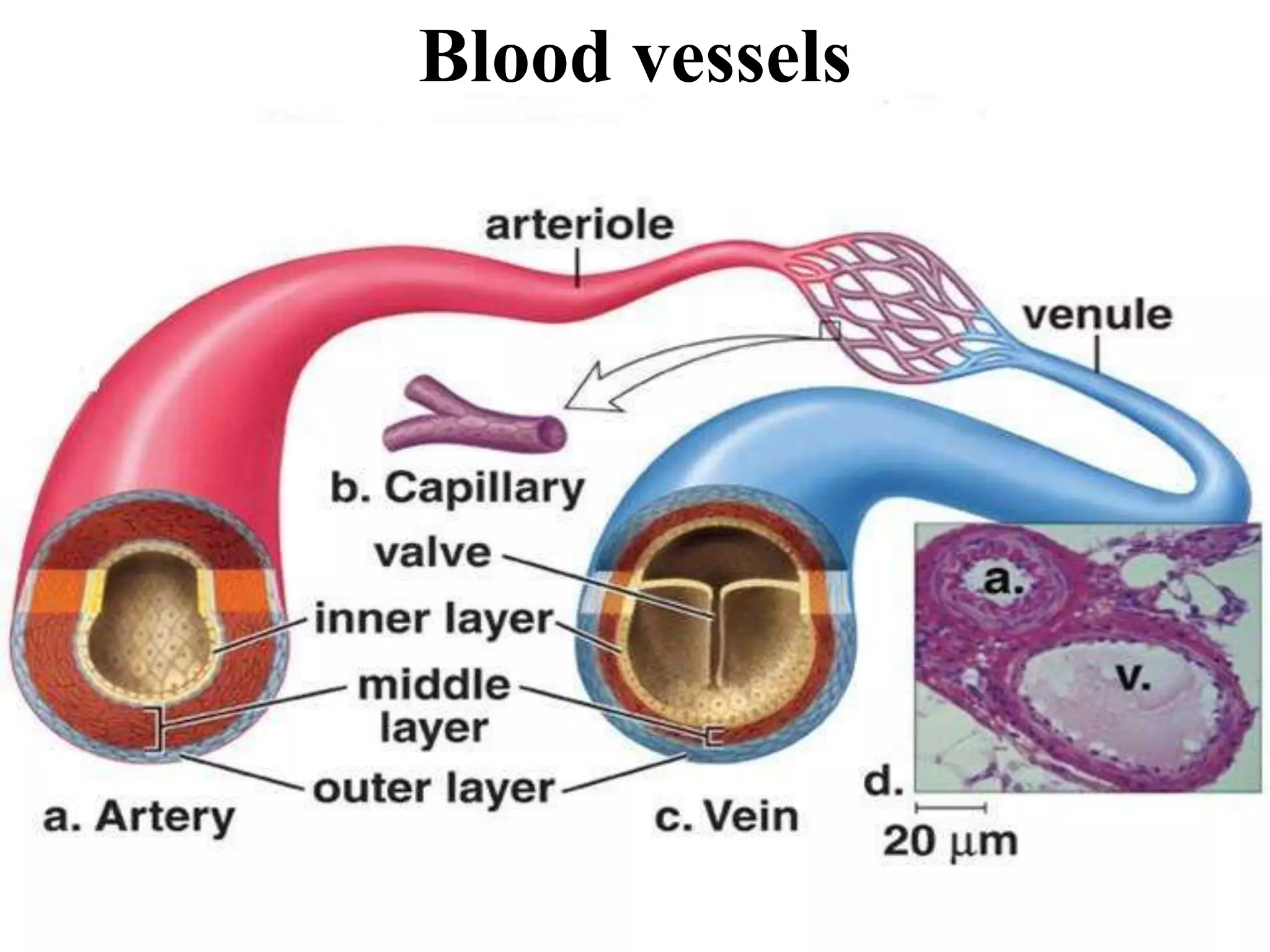
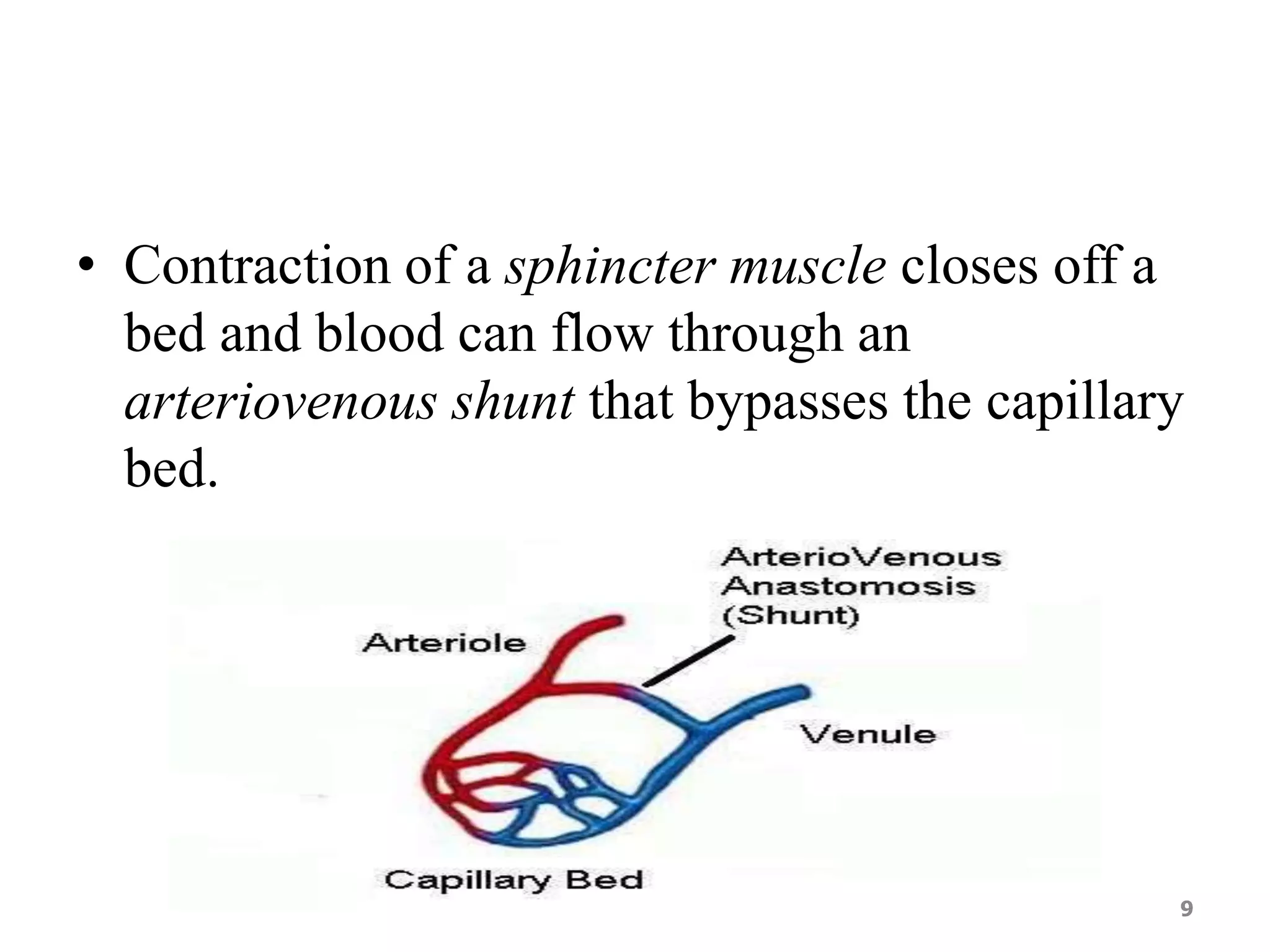
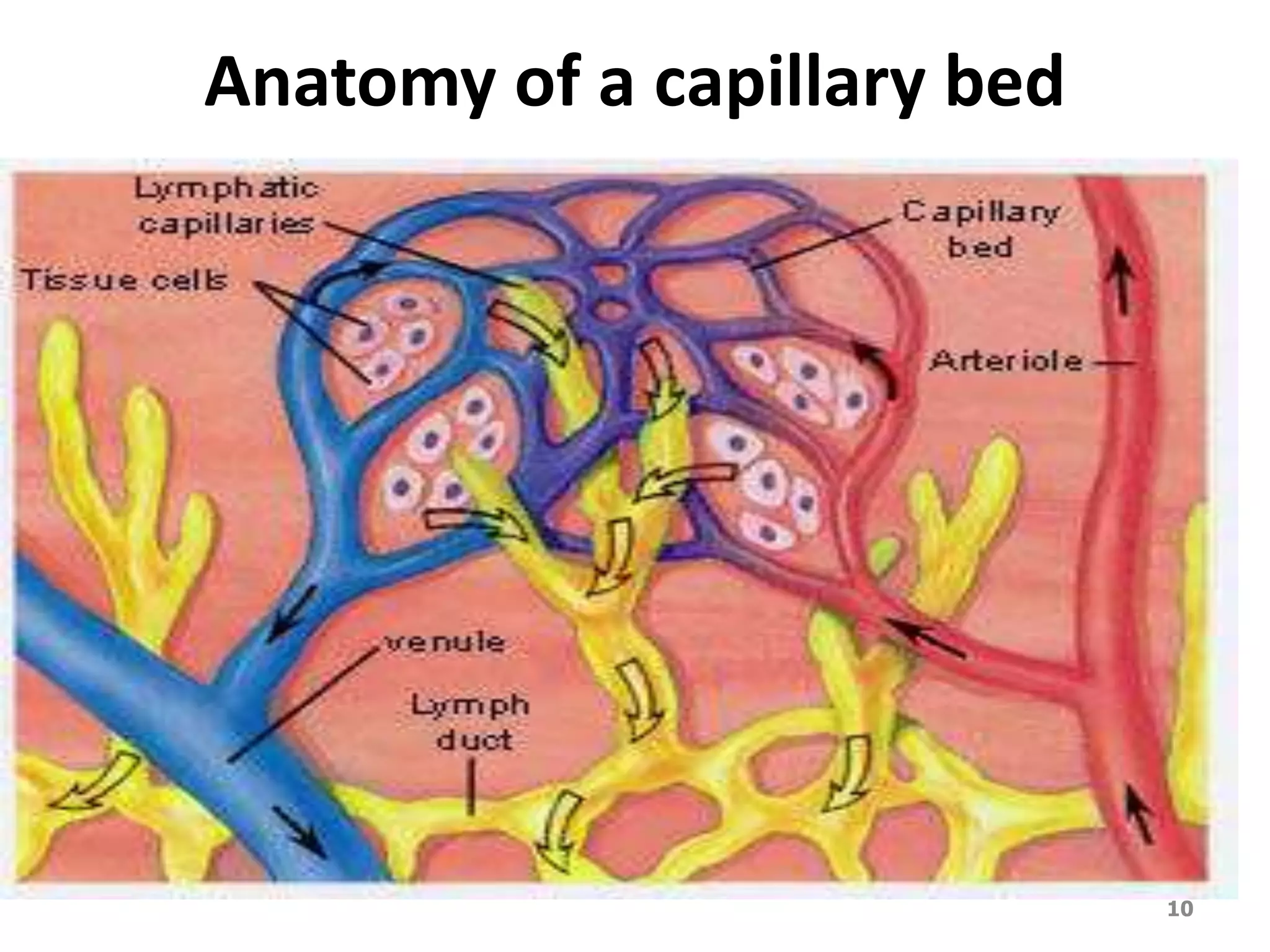
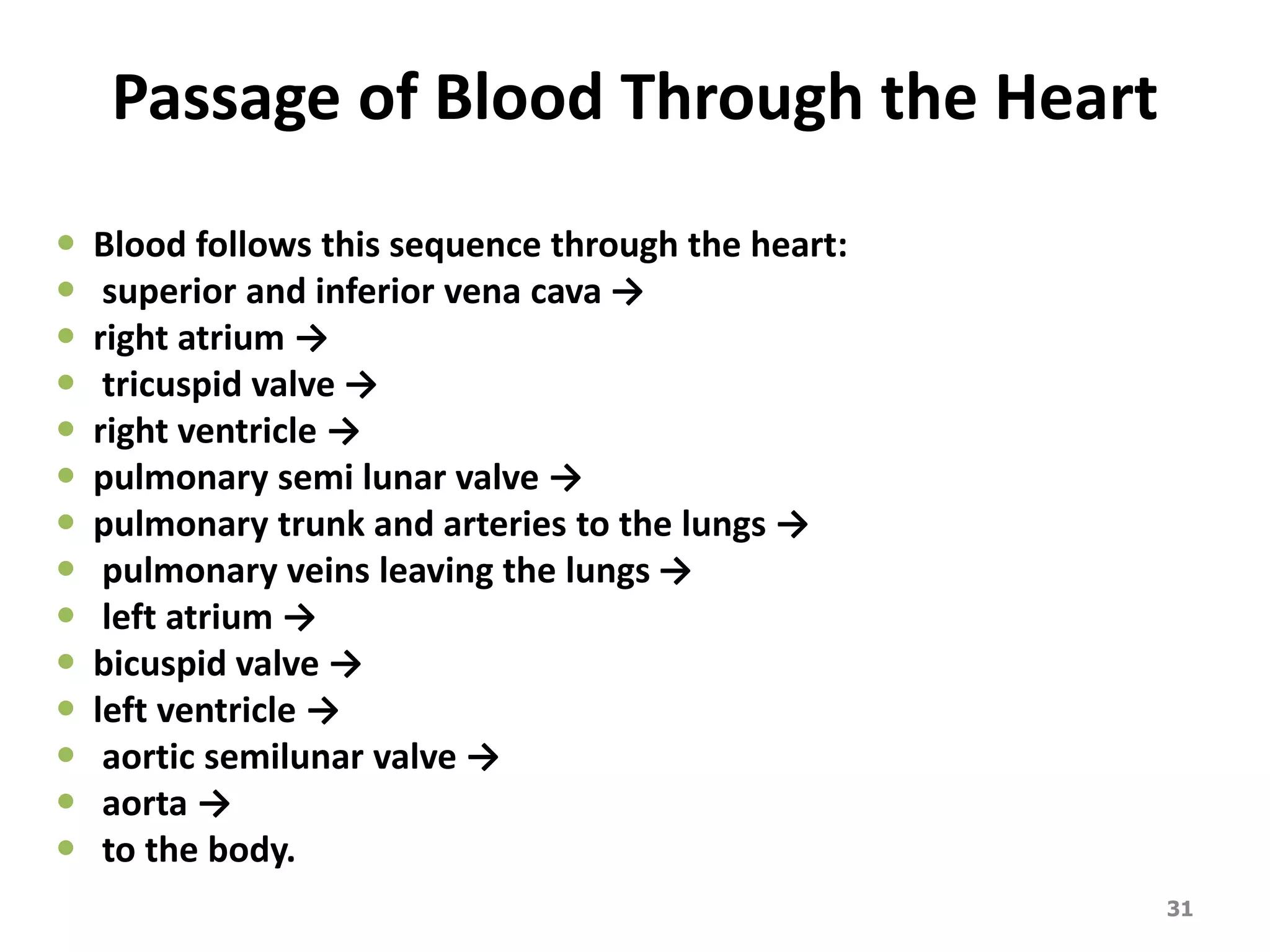
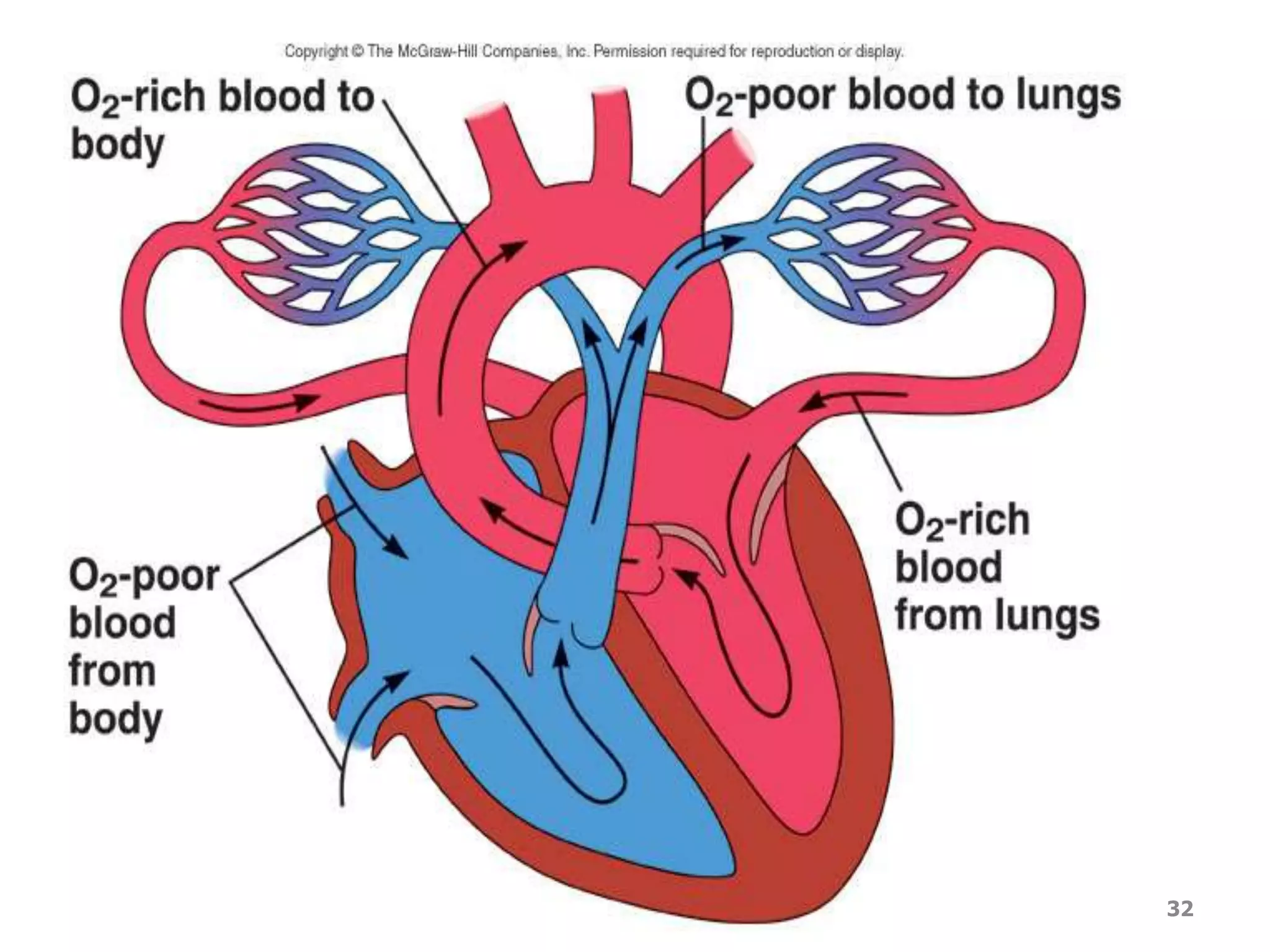
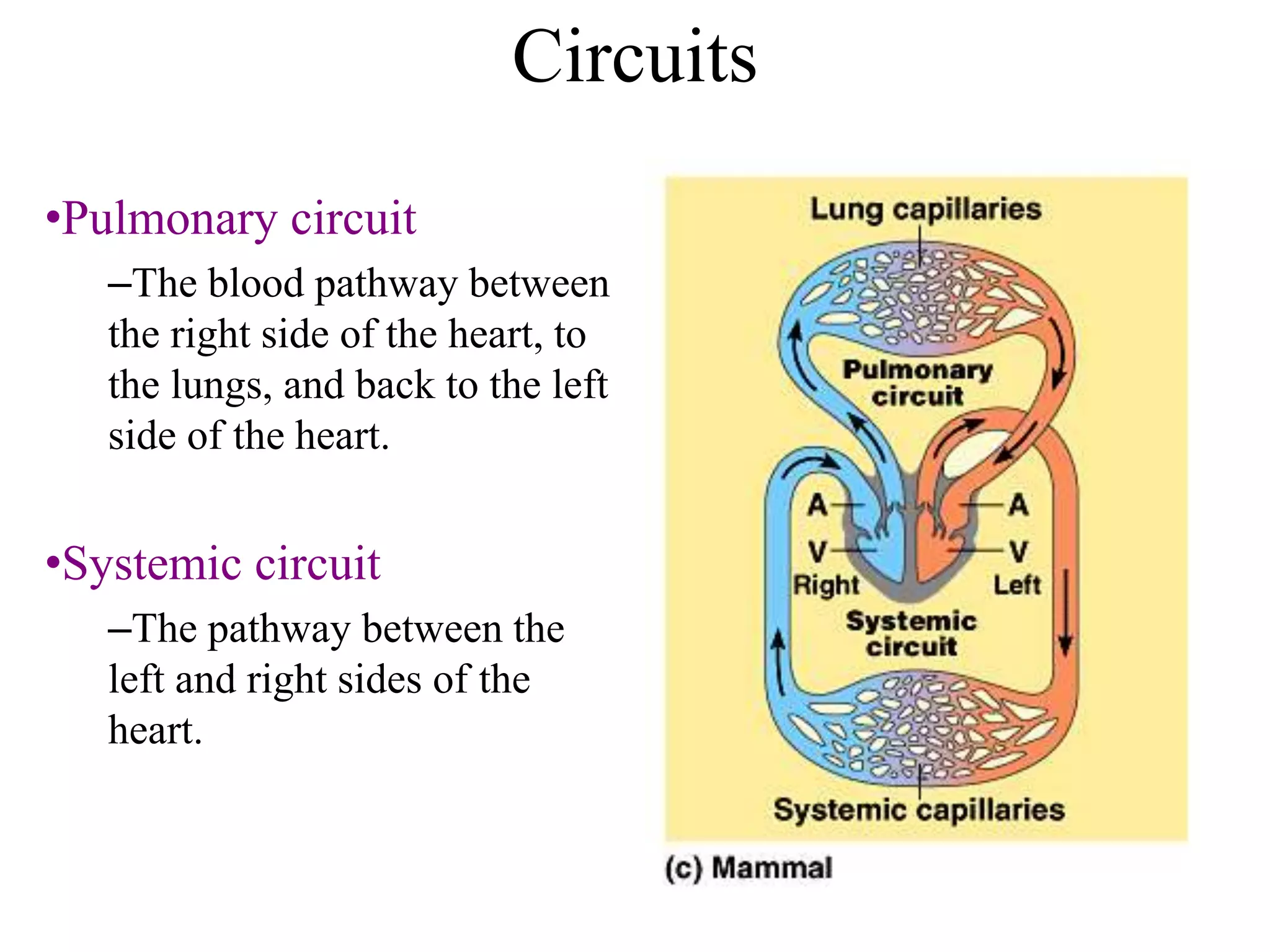
2. Arteries, which carry oxygenated blood away from the heart. Capillaries allow for gas and nutrient exchange before veins return deoxygenated blood to the heart.
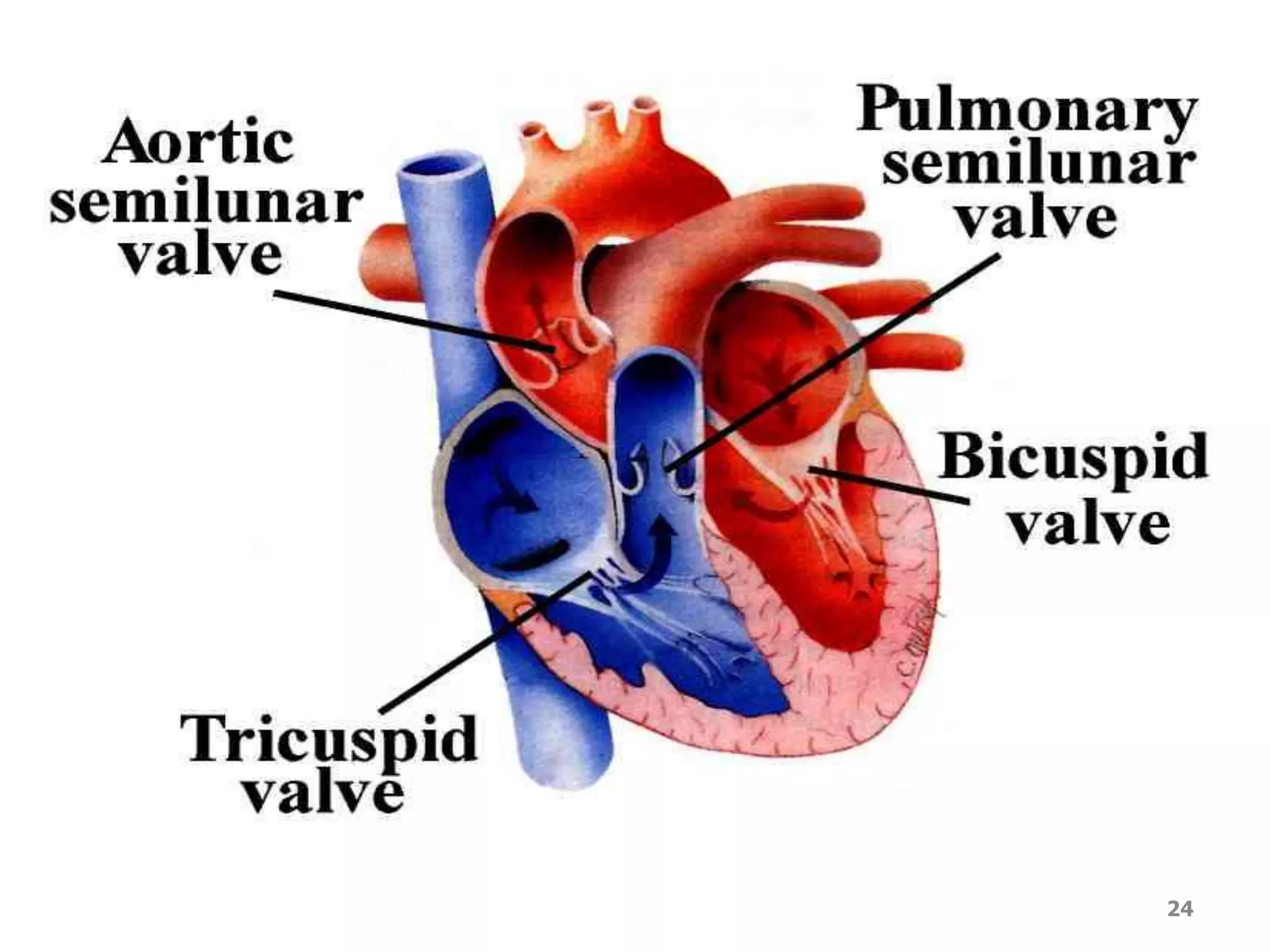
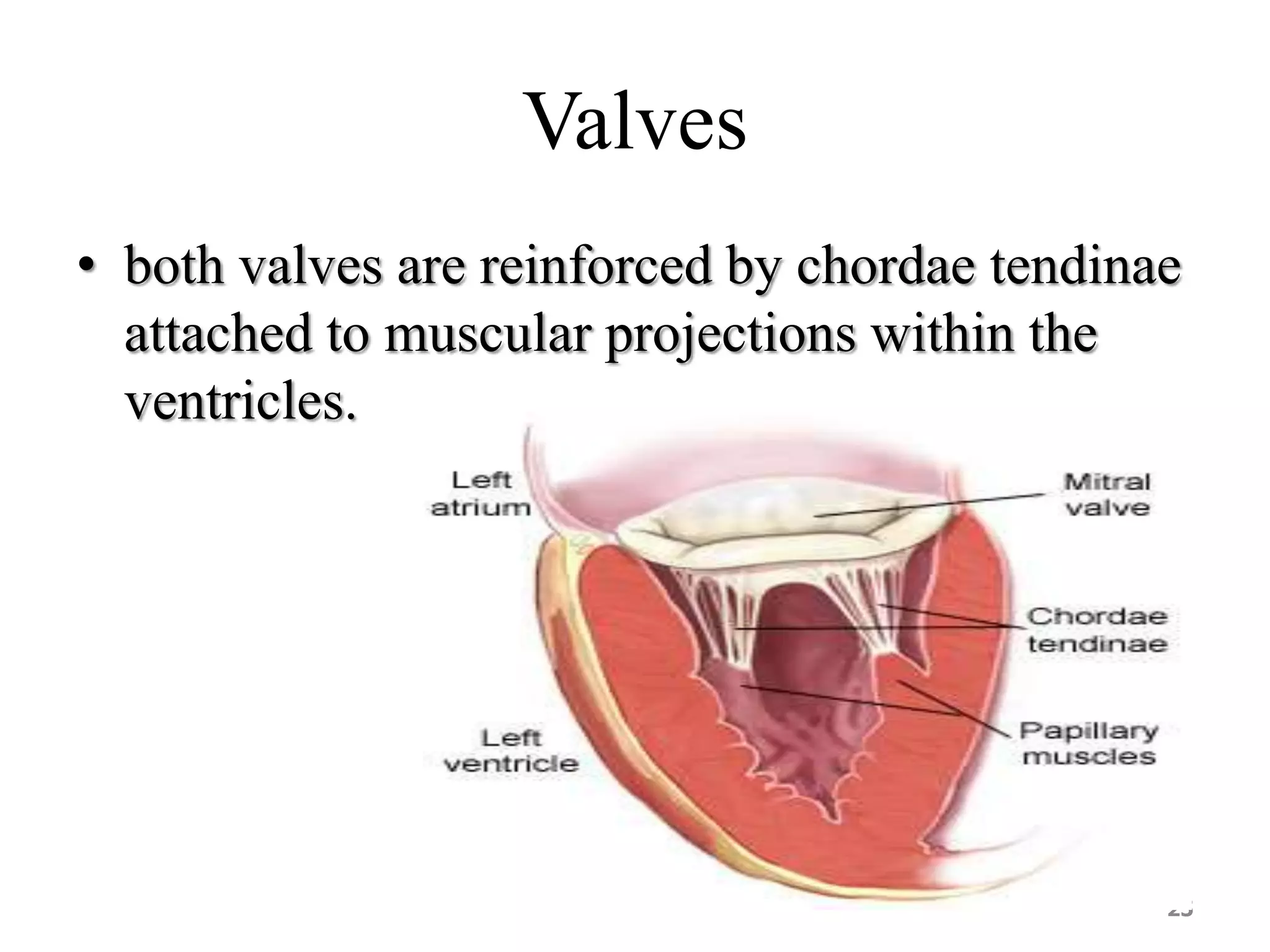
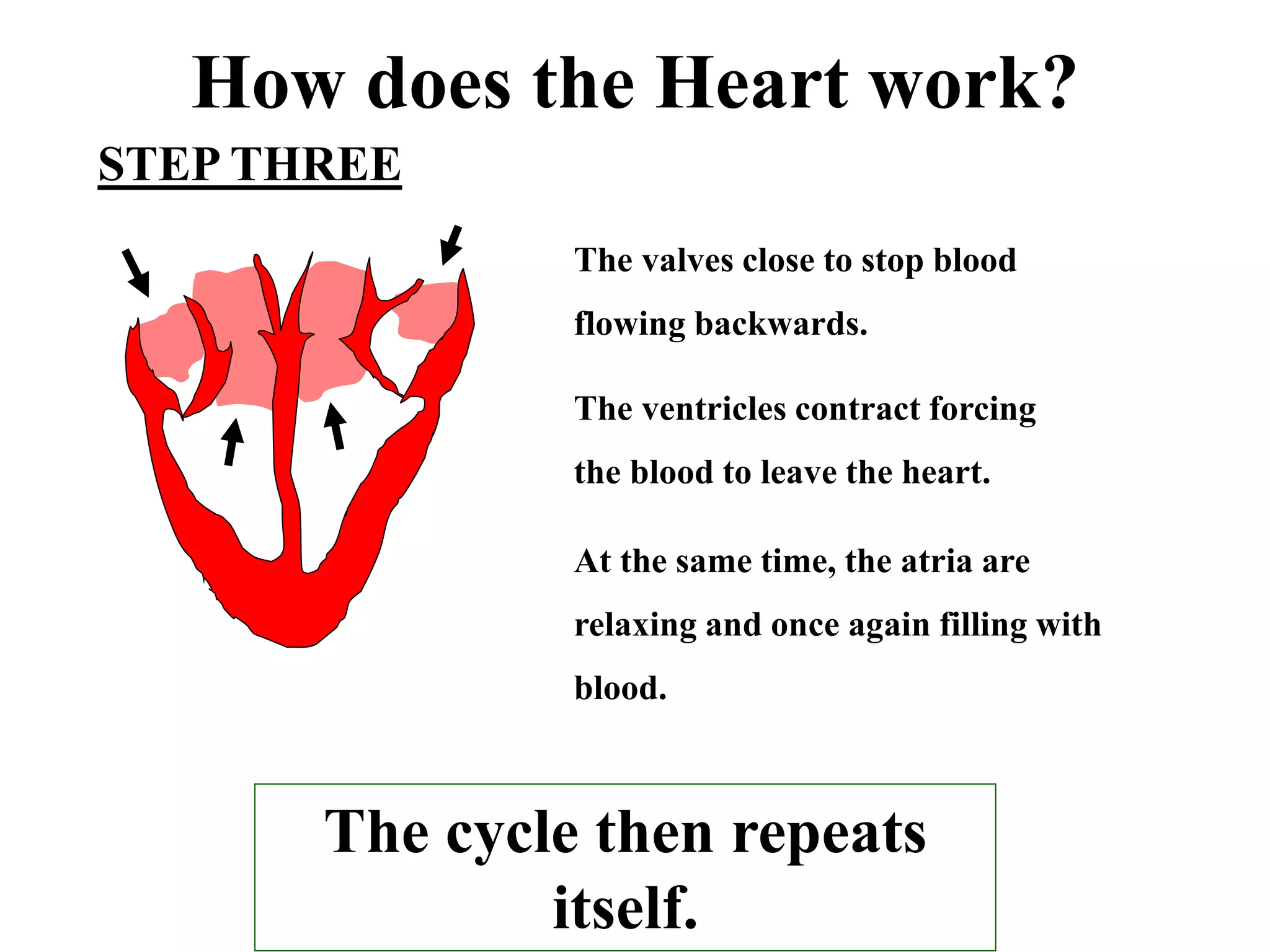
3. Valves ensure one-way blood flow, with the tricuspid and bicuspid valves located between the heart's upper and lower chambers.