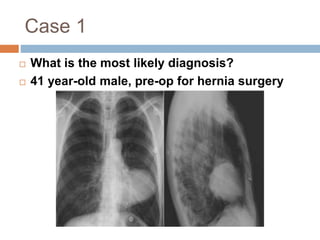
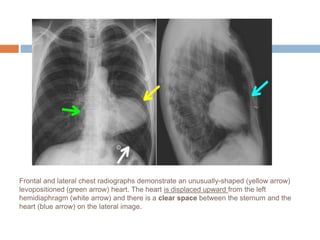
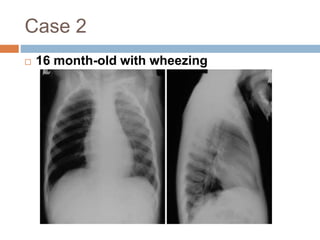
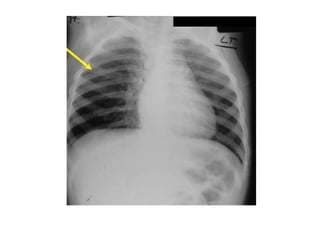
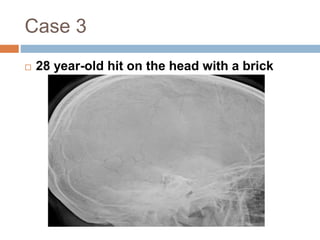
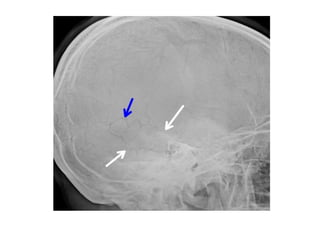
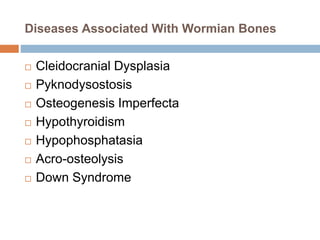
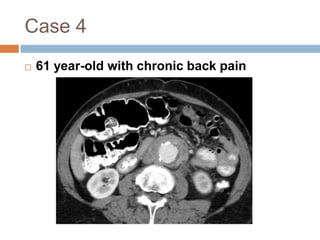
The document discusses four clinical cases: congenital defect in the pericardium, aspirated foreign body, wormian bones, and retroperitoneal fibrosis, detailing their diagnoses, clinical findings, imaging characteristics, and treatment options. Each case highlights specific demographics, common symptoms, and associated anomalies or complications. The discussions emphasize the importance of imaging in diagnosis and variations in presentation among different age groups.