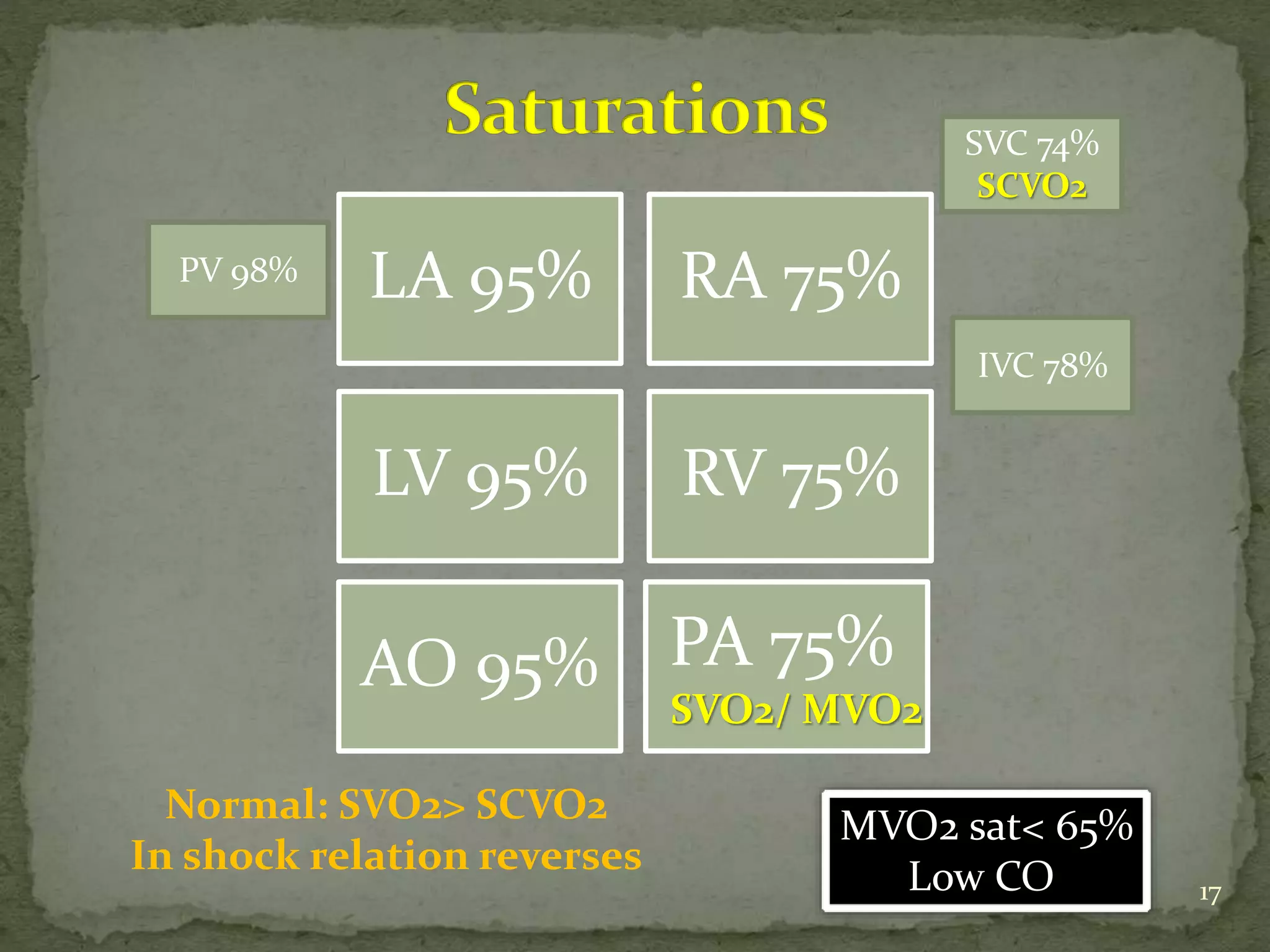
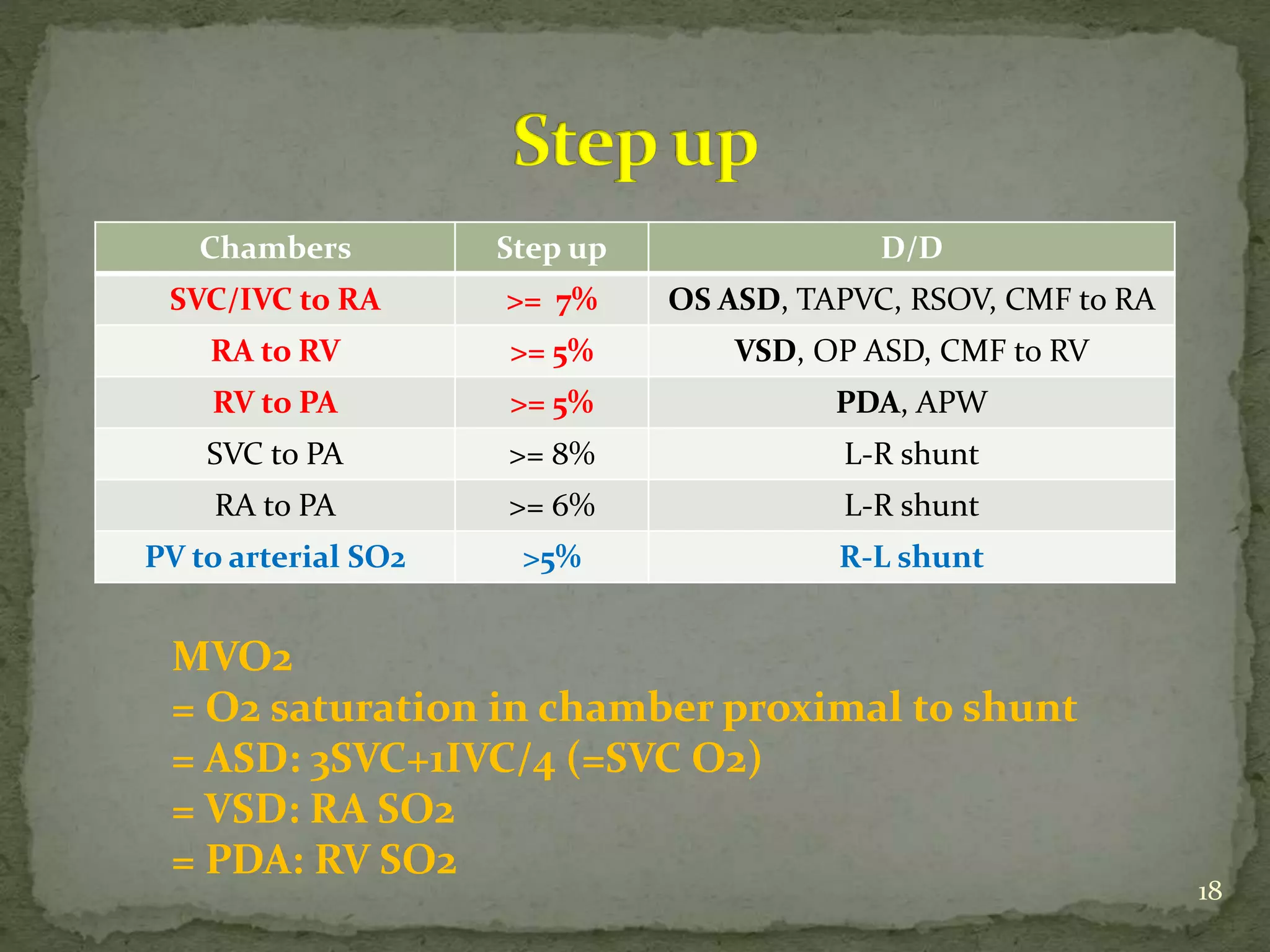
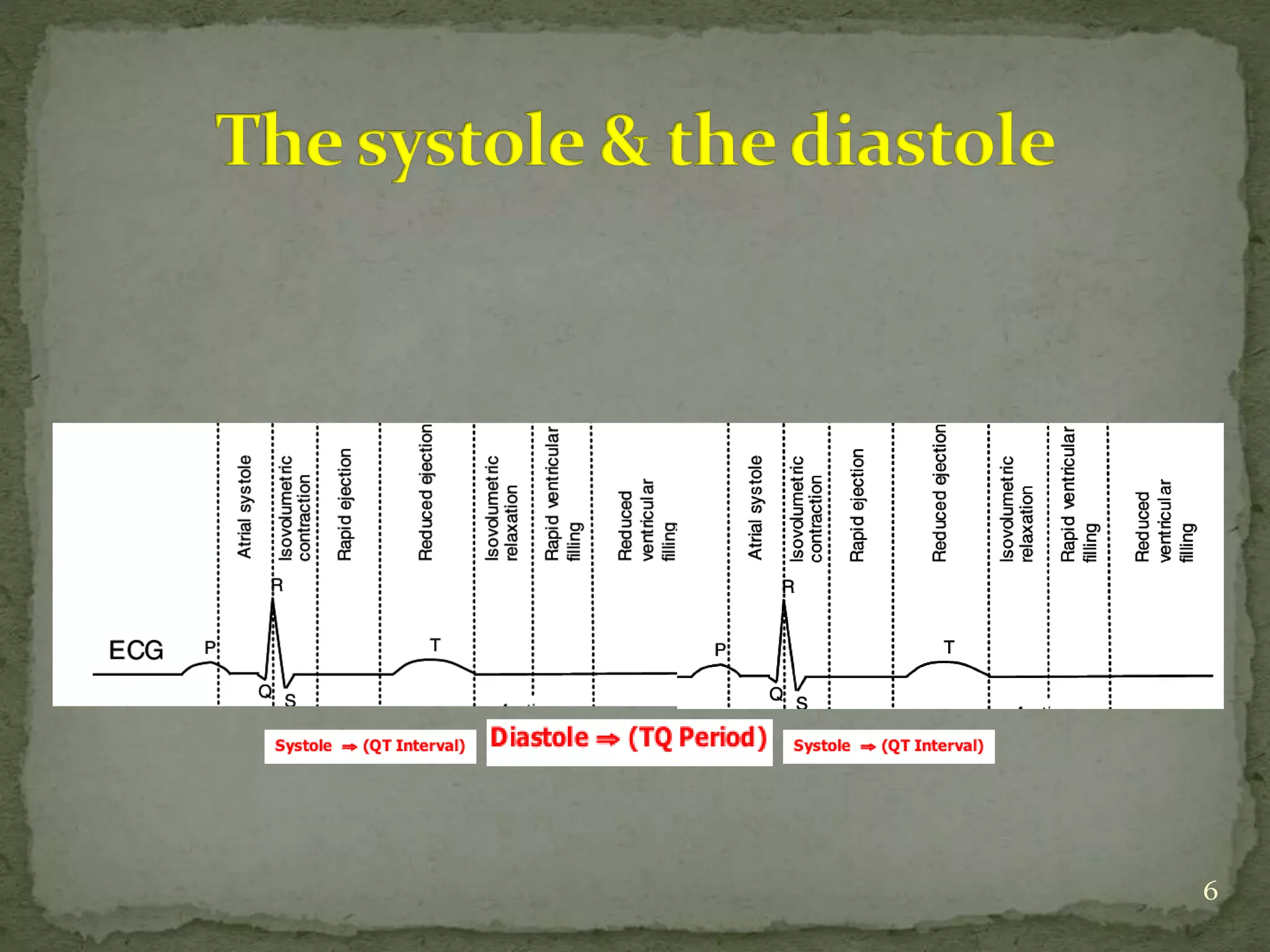
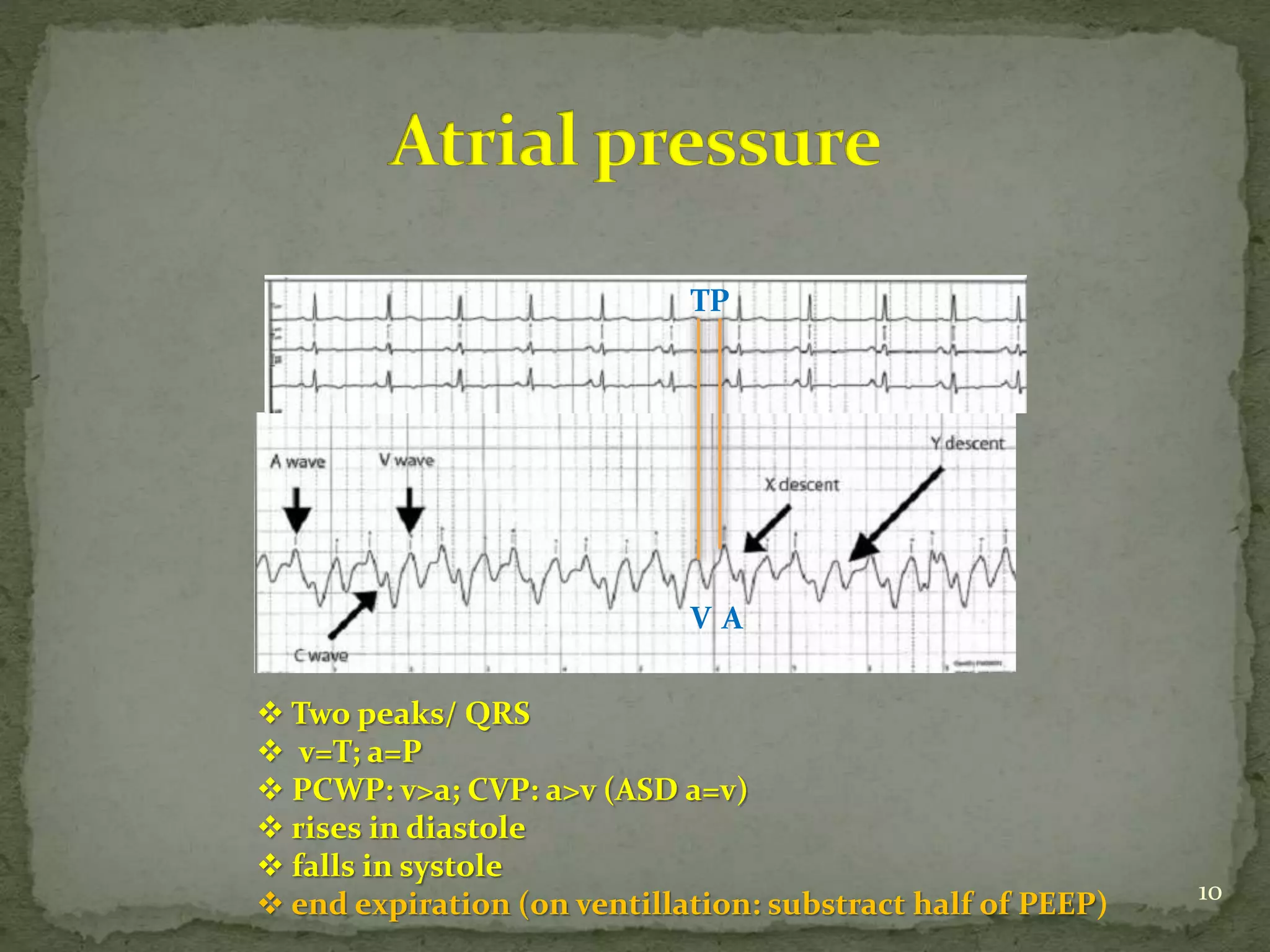
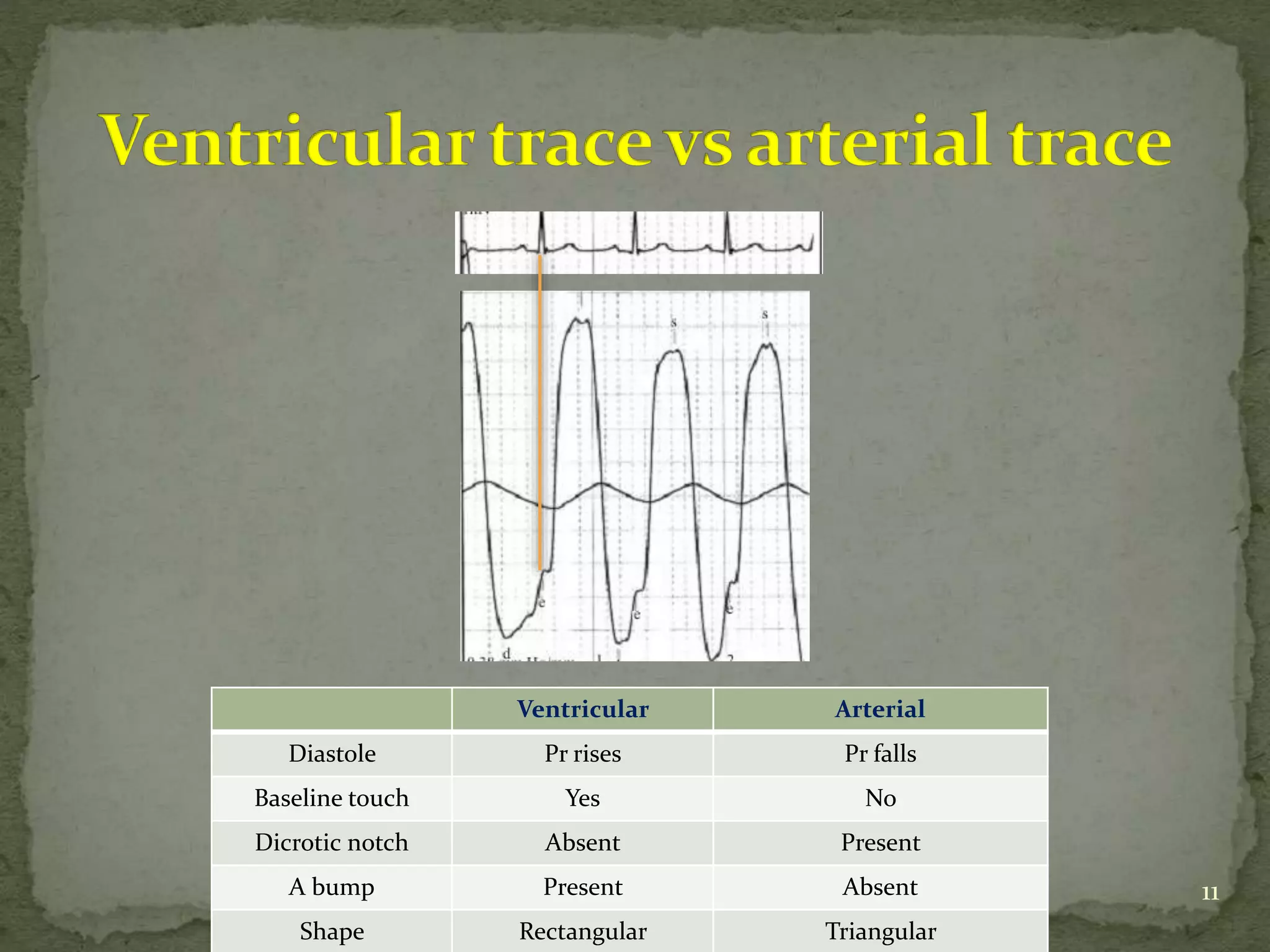
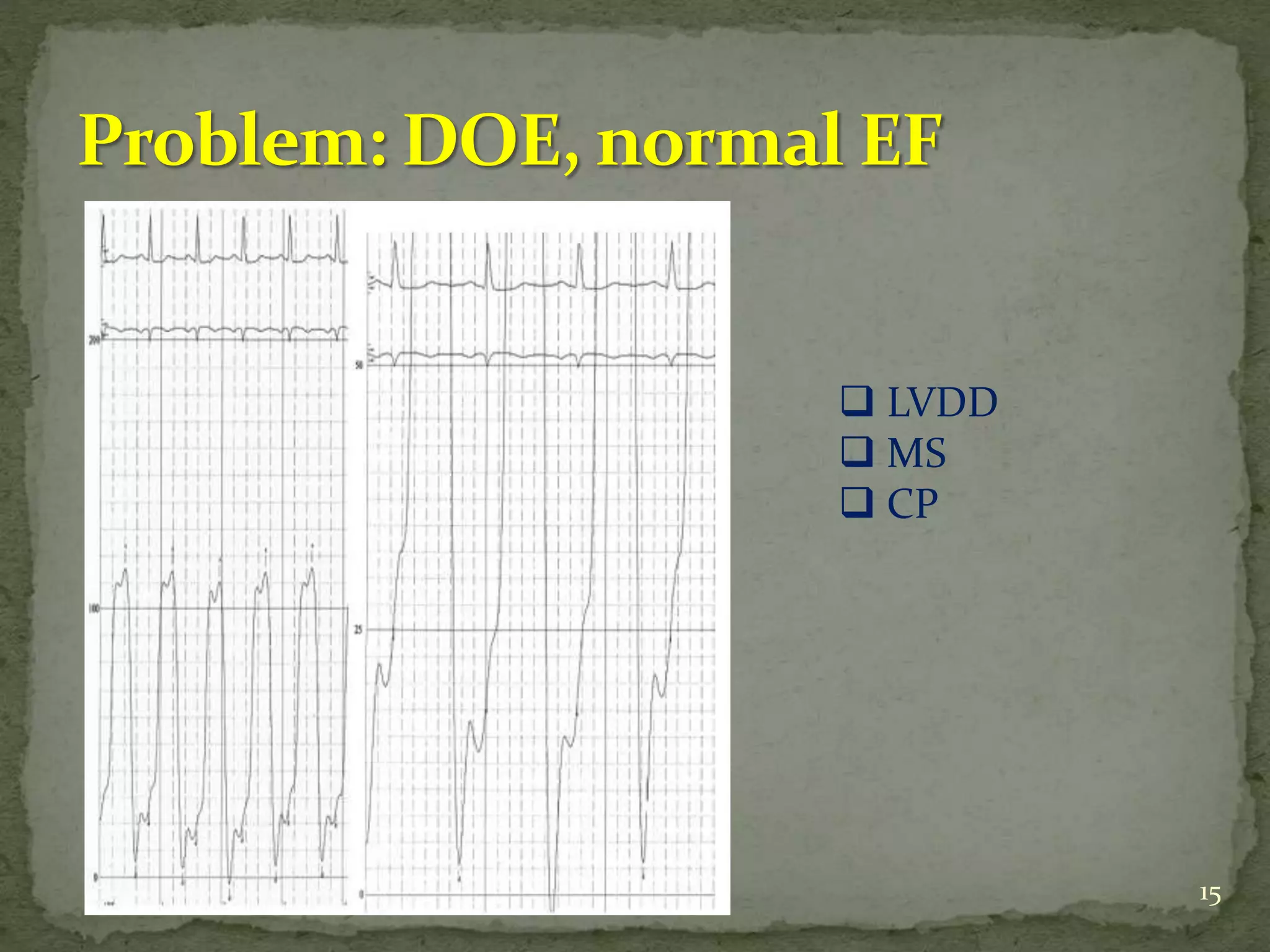
This document discusses various hemodynamic parameters and waveforms seen in different cardiac conditions:
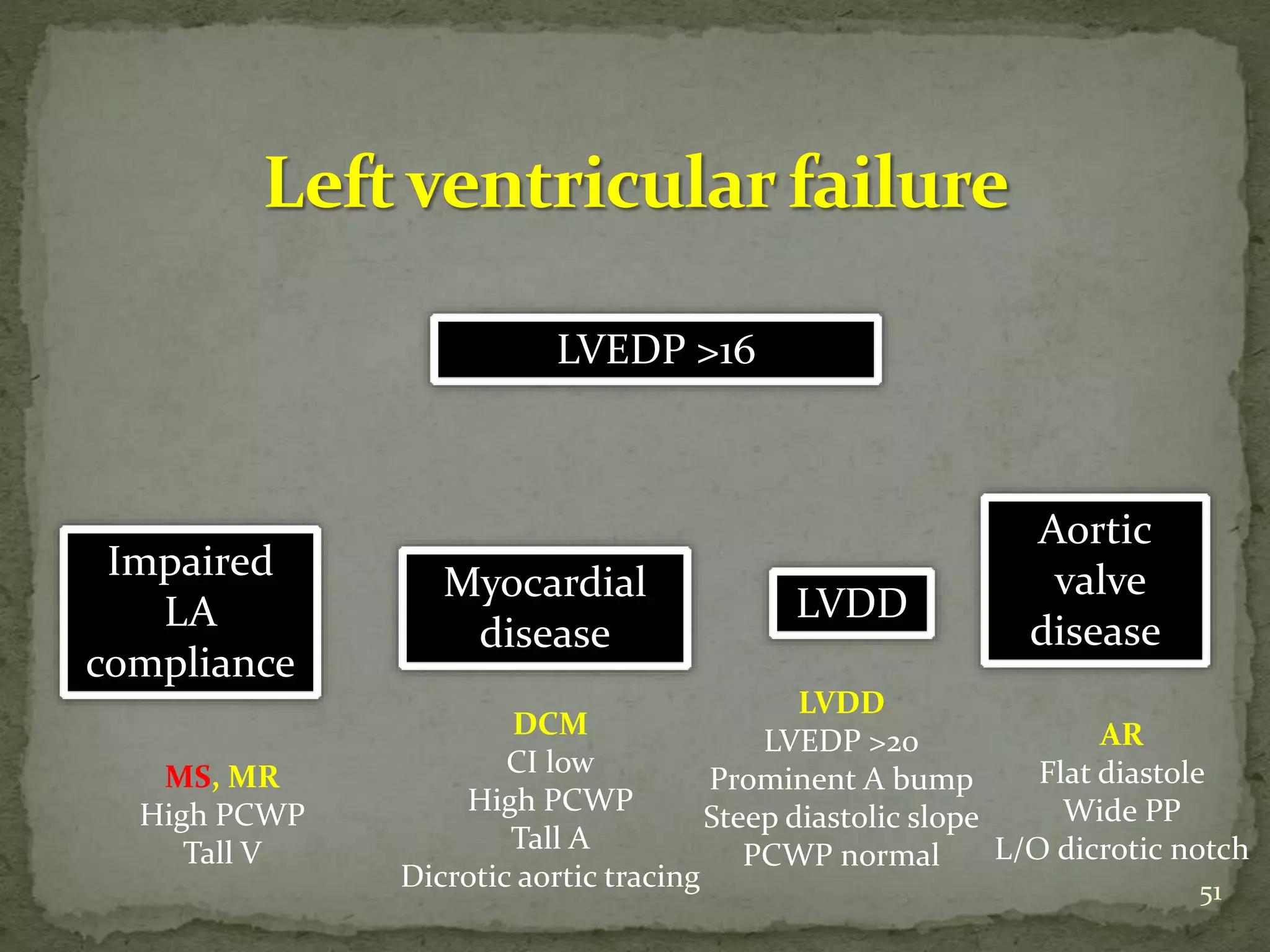
- It compares pressures, waveforms and compliance in conditions like constrictive pericarditis, right ventricular failure, cardiac tamponade and pulmonary hypertension.
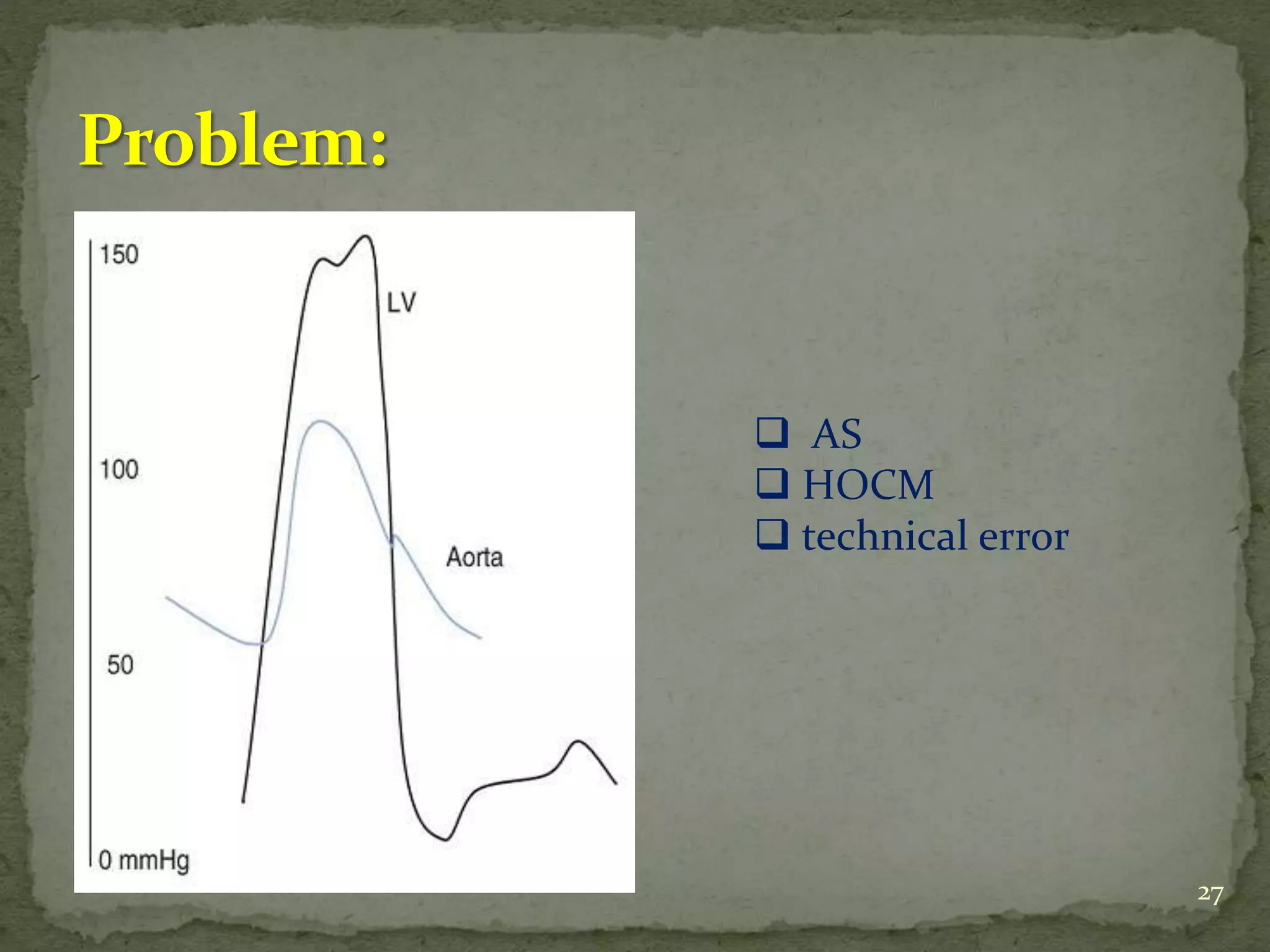
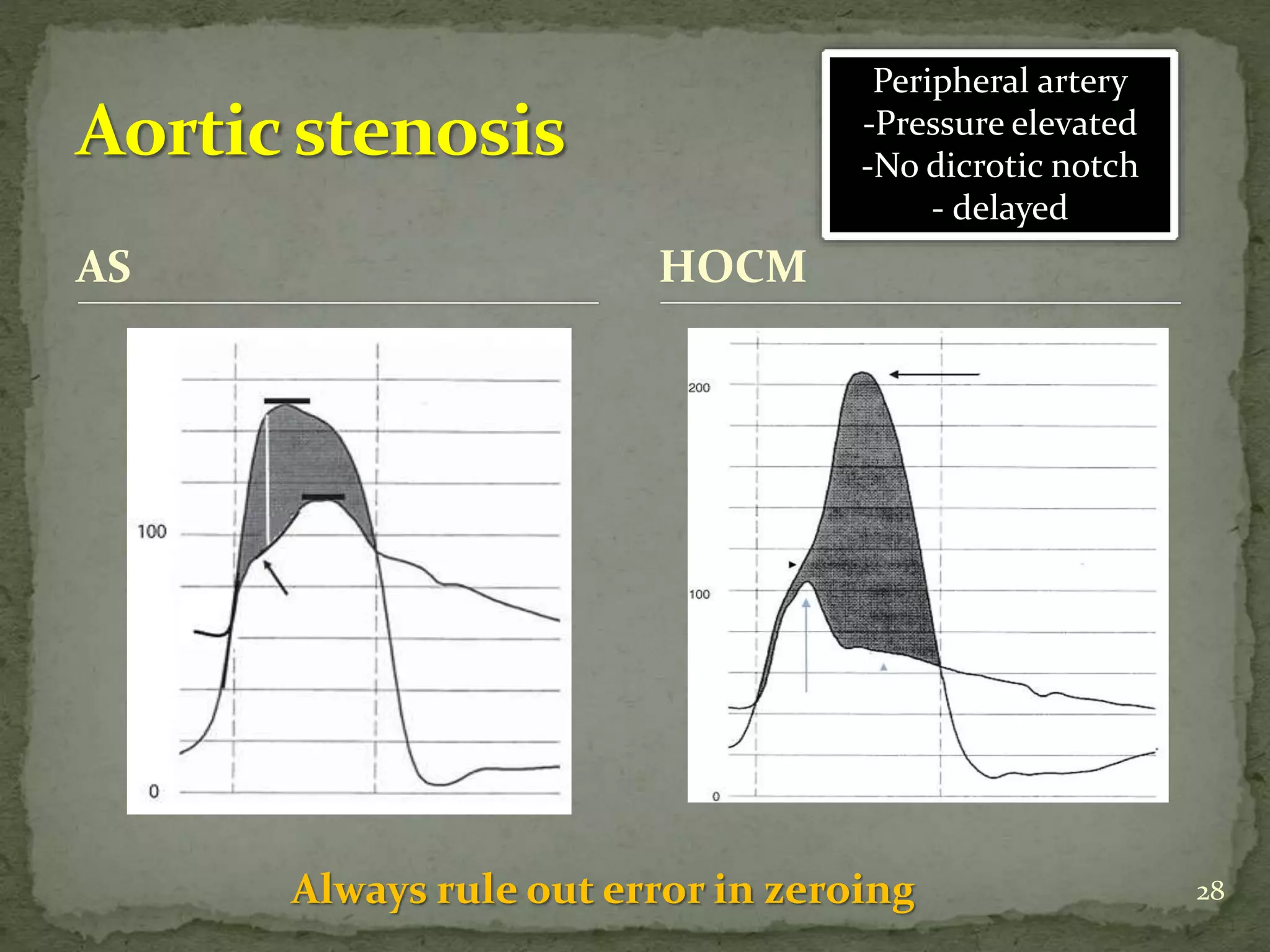
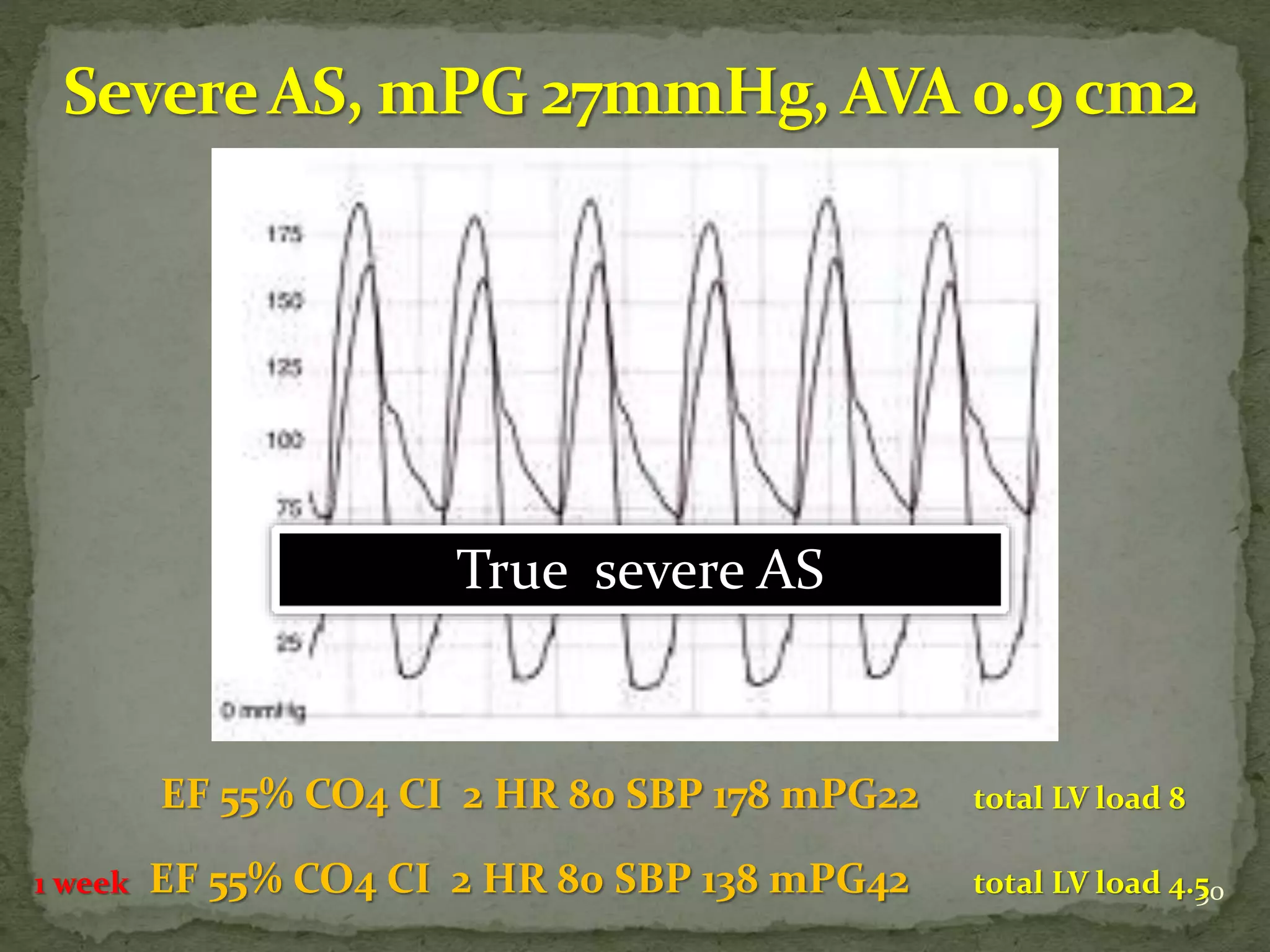
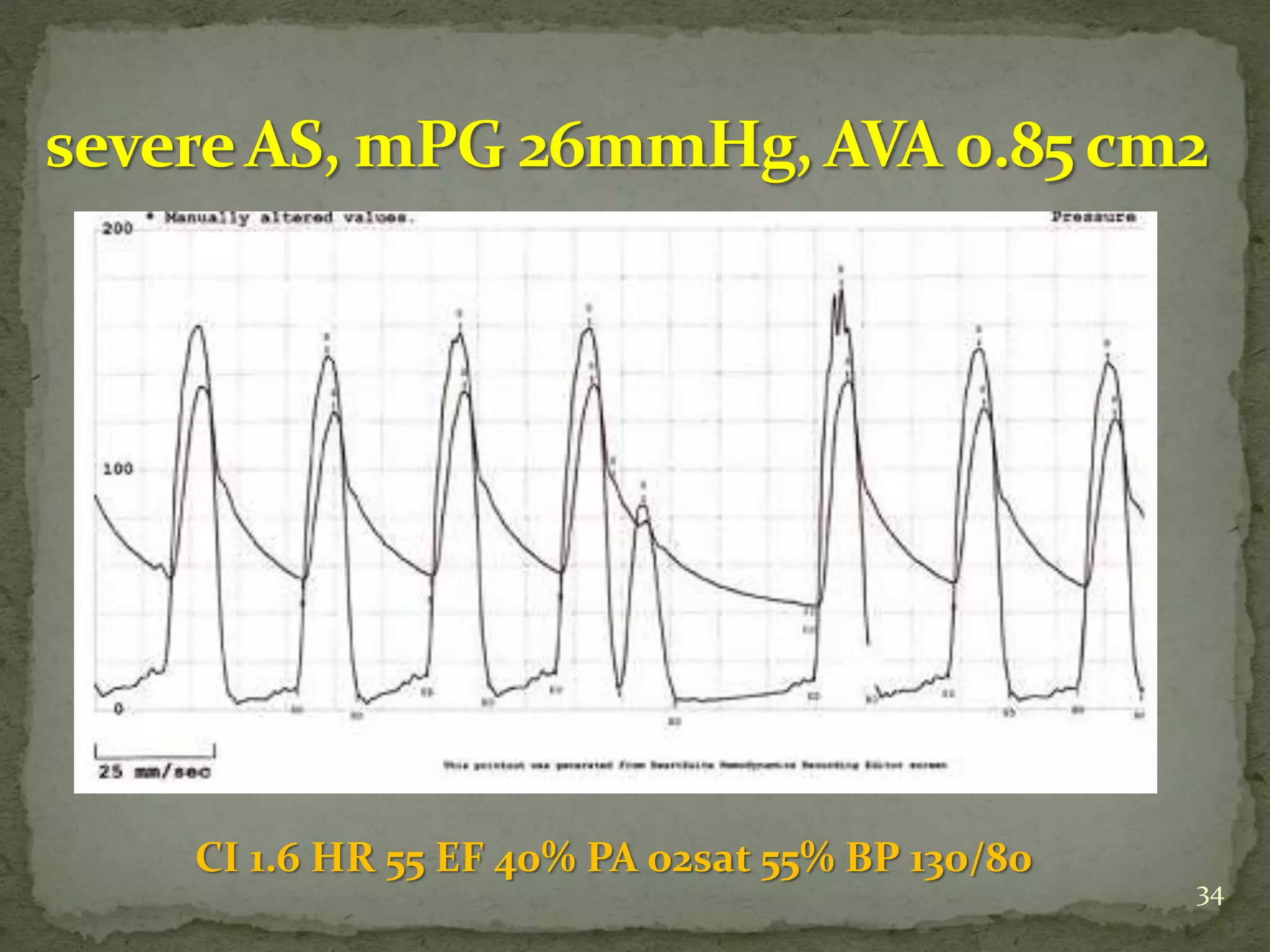
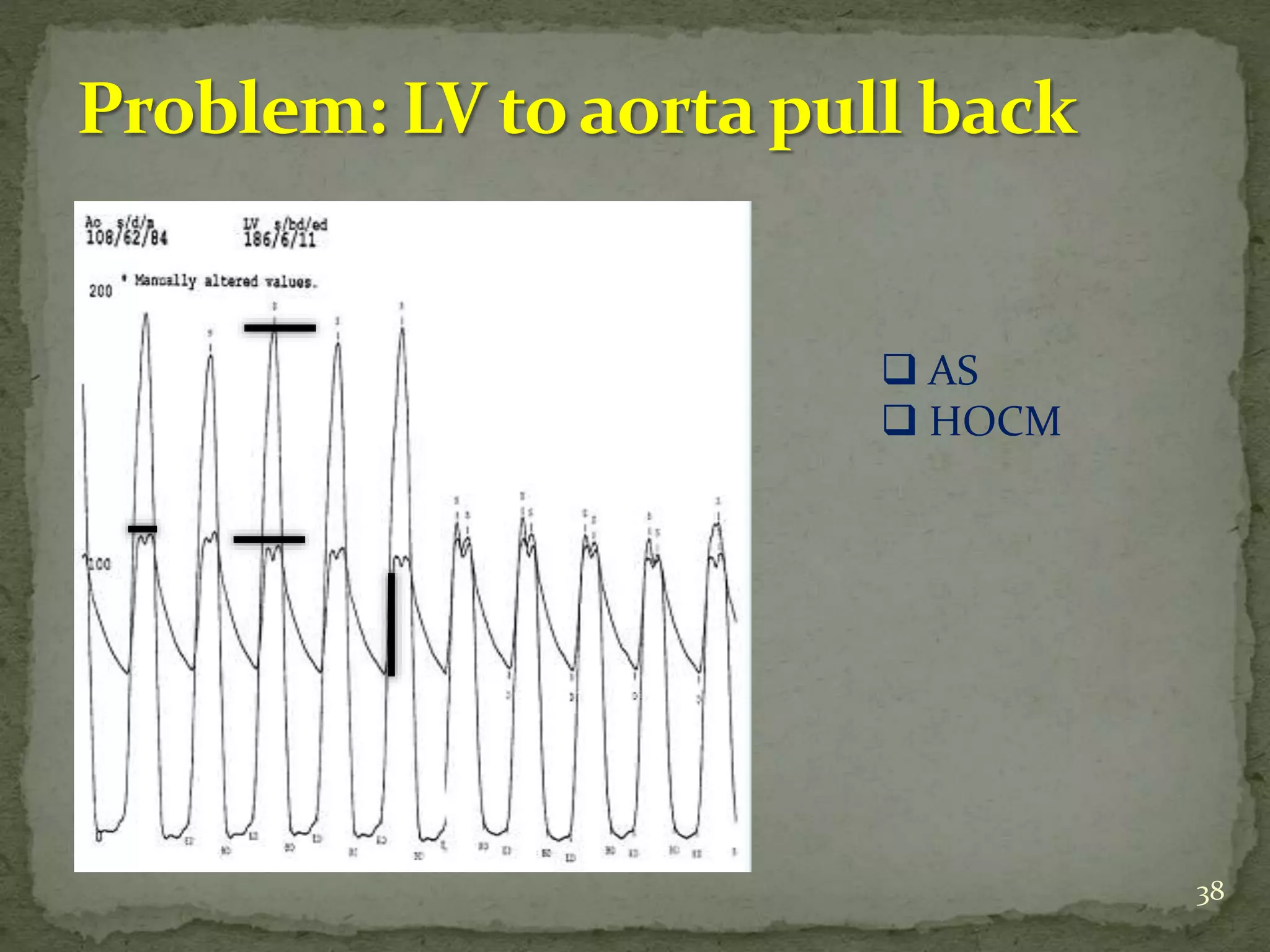
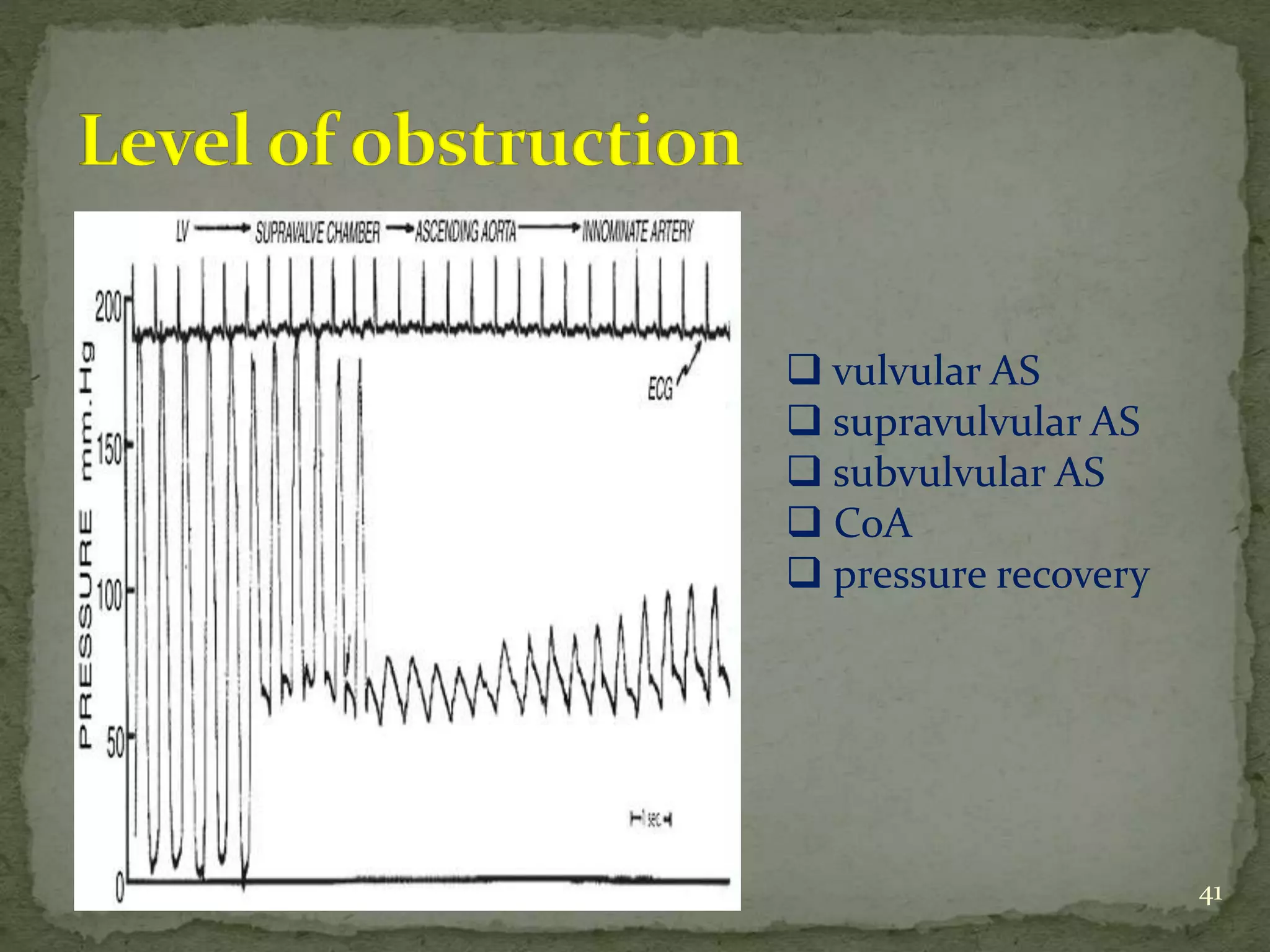
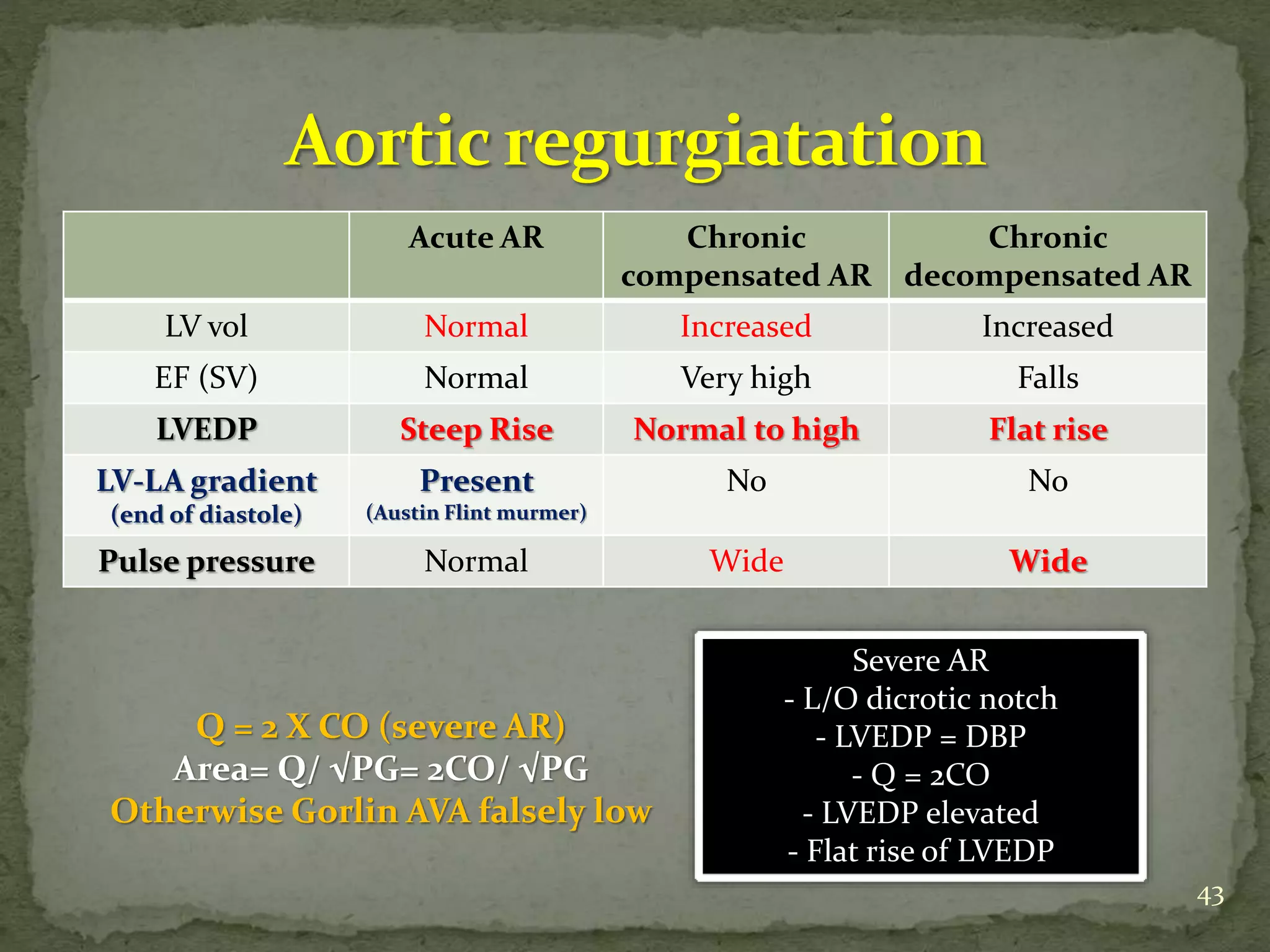
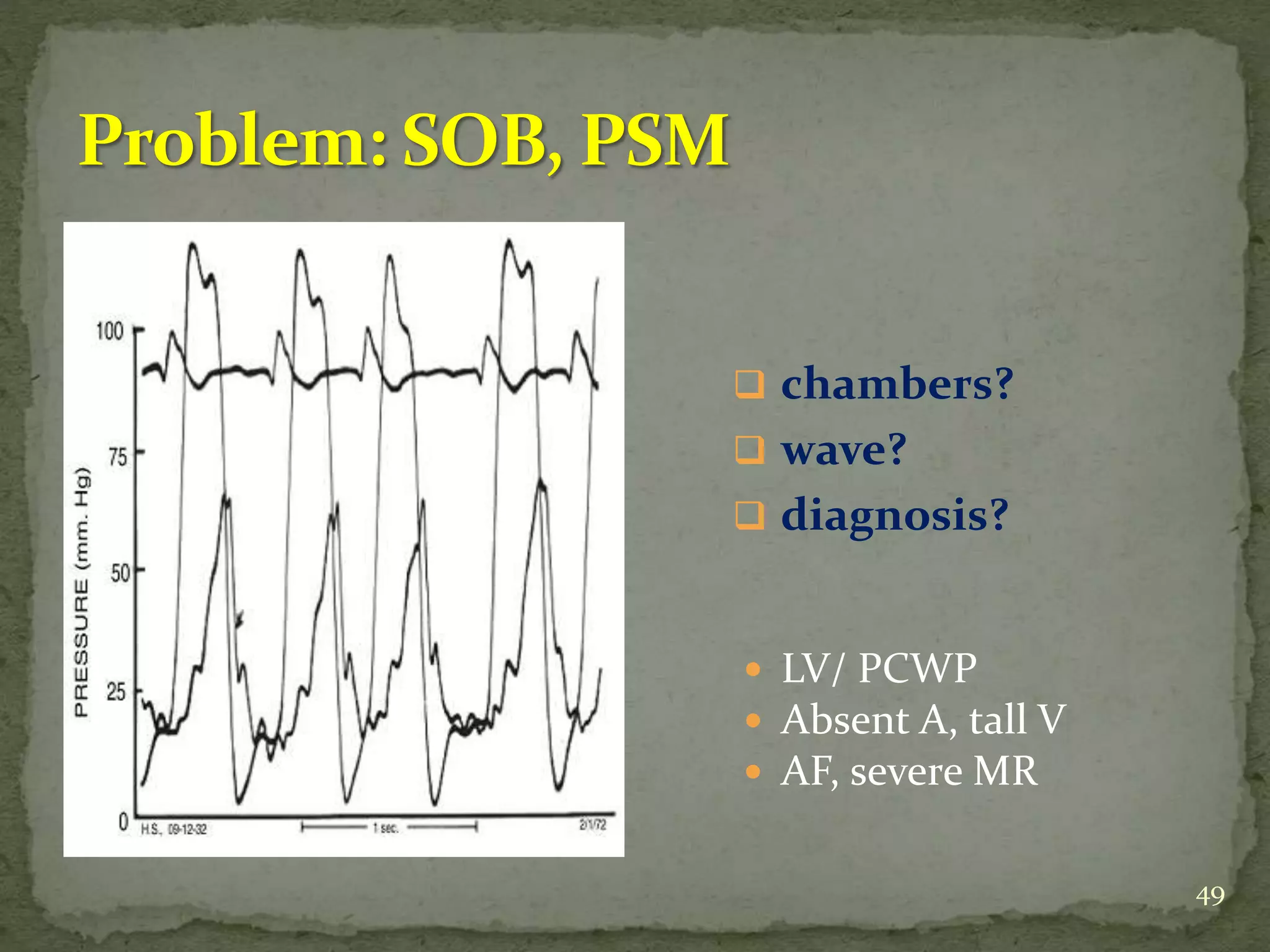
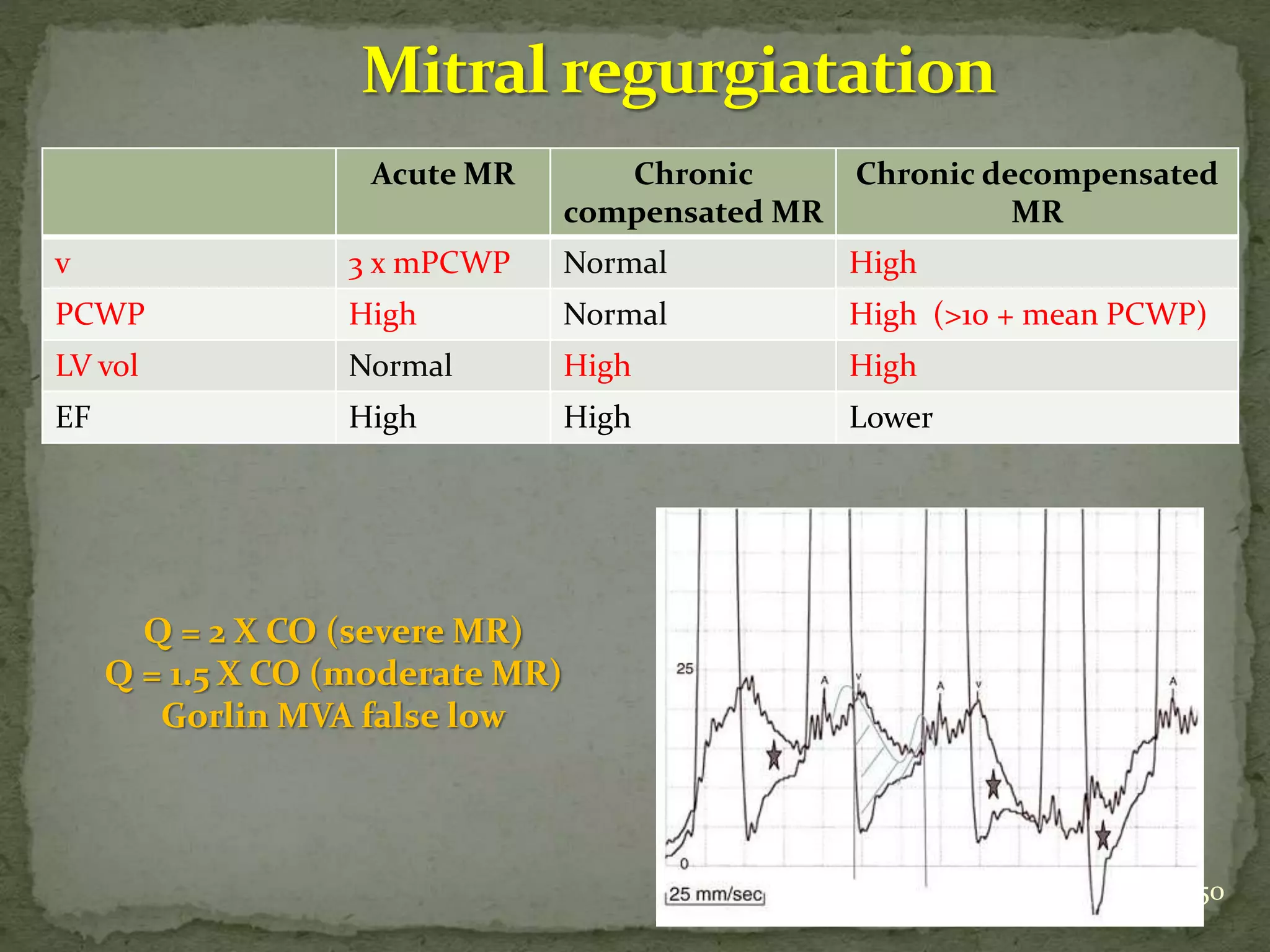
- Key waveforms and pressures are described for valvular lesions like mitral stenosis, aortic stenosis, mitral regurgitation and aortic regurgitation.
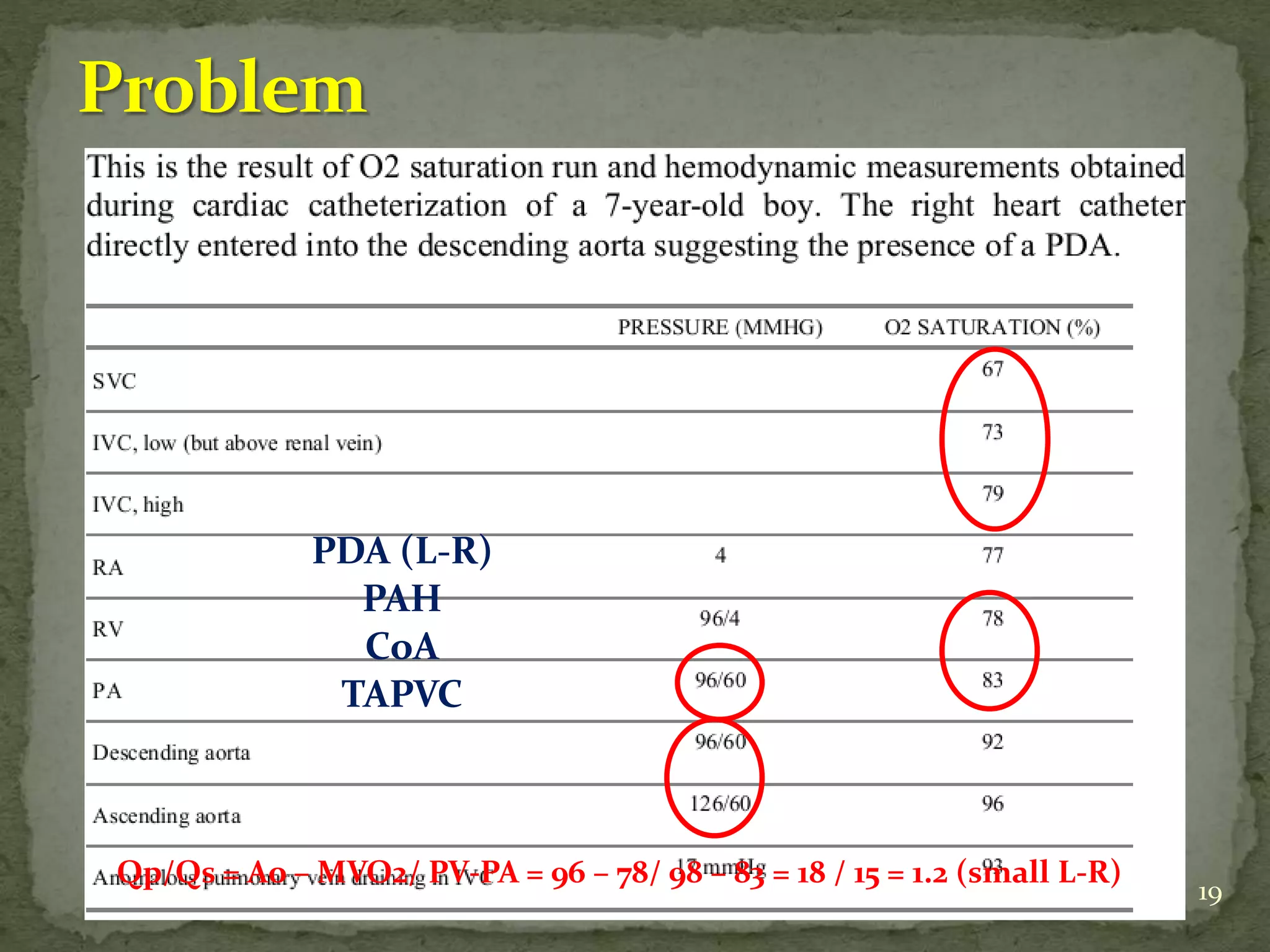
- Equations for calculating cardiac output, shunt fractions and valvular areas are provided.
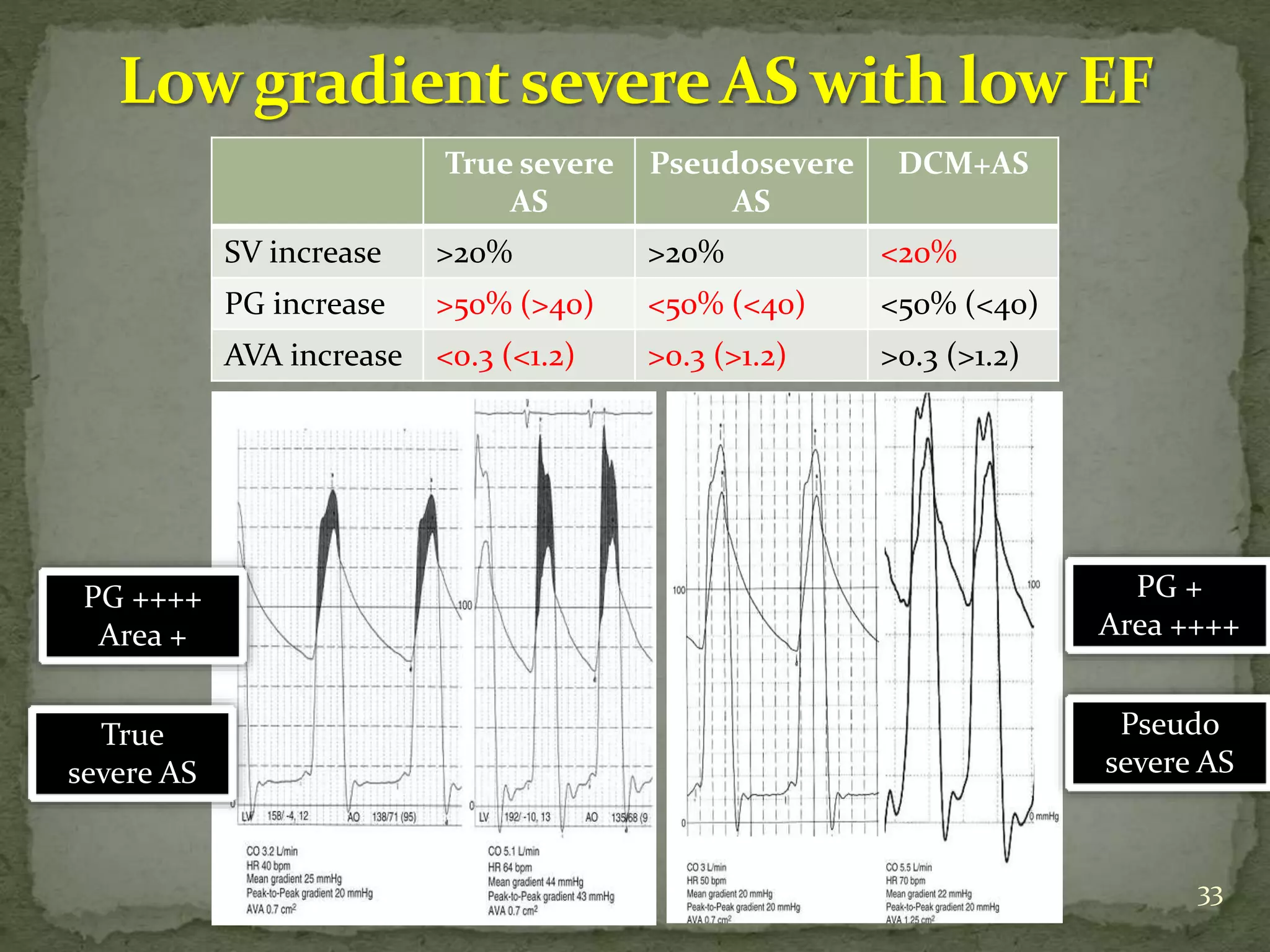
- Diagnostic criteria for pseudosevere versus true severe aortic stenosis on stress echocardiography are outlined.
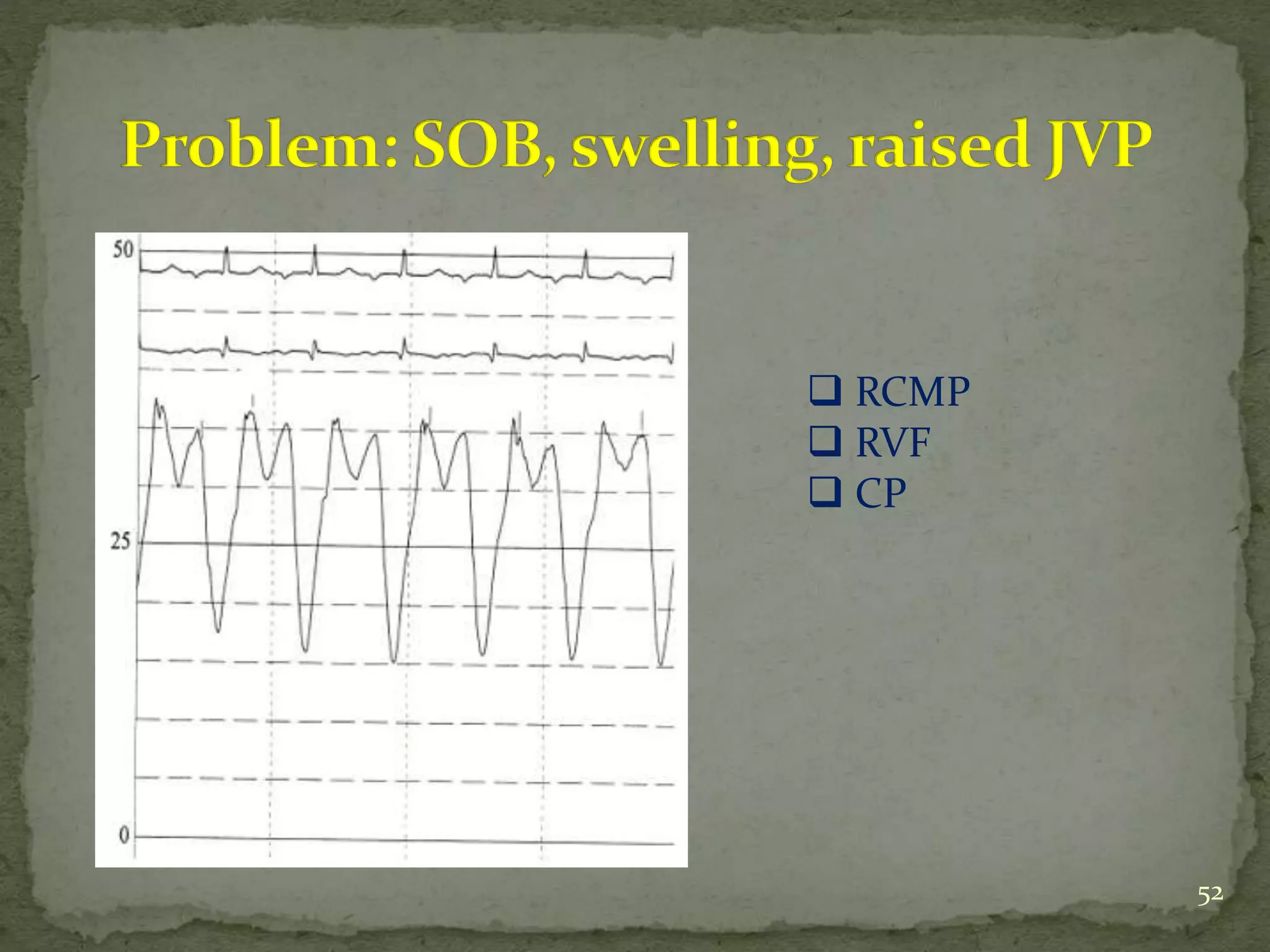
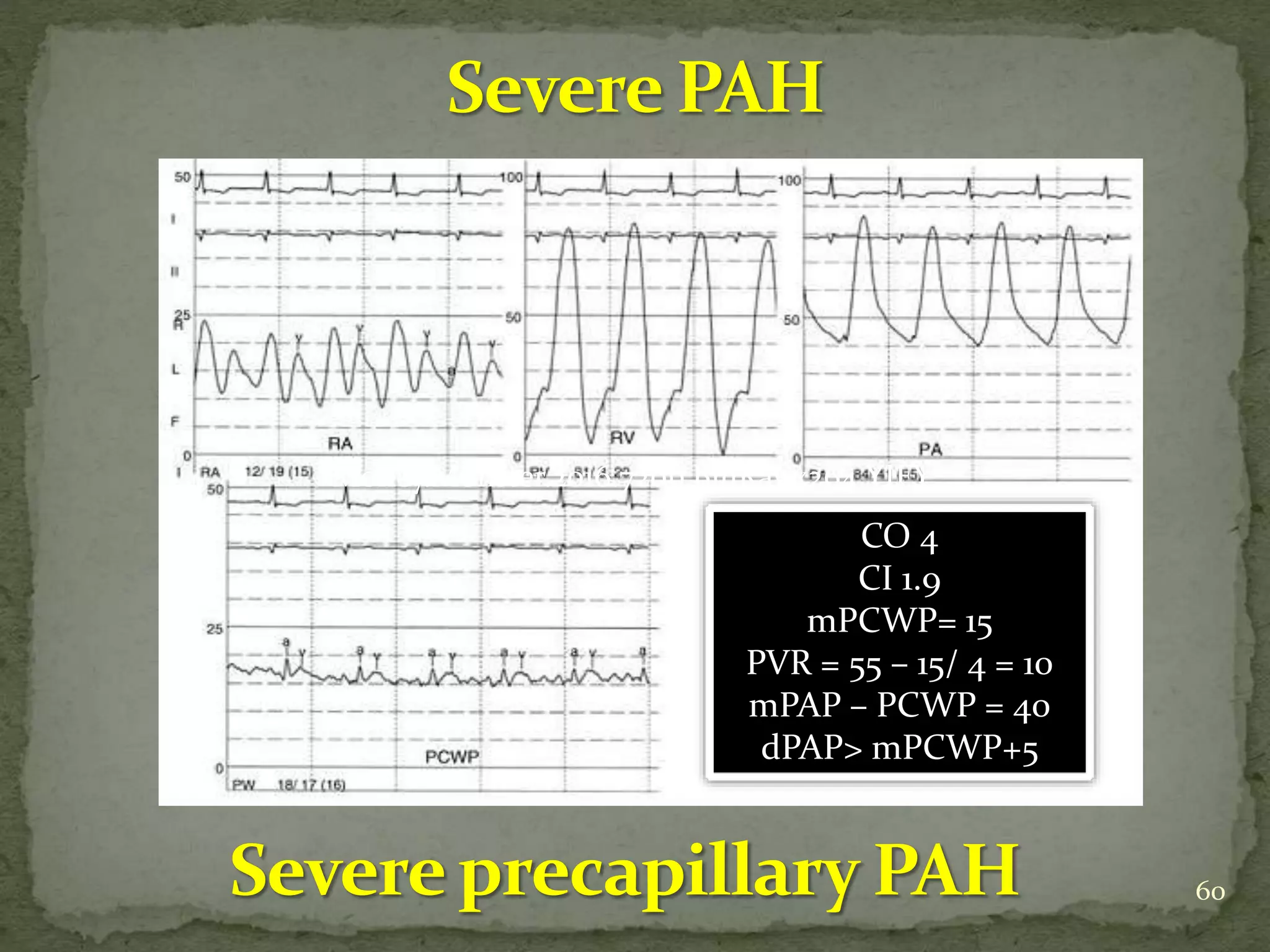
- A case example is presented of a patient evaluated for pulmonary