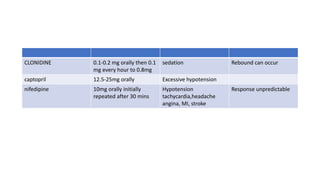
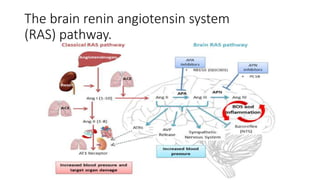
Recent guidelines classify hypertension into four stages based on increasing levels of systolic and diastolic blood pressure. Hypertension increases risks for cardiovascular and kidney diseases, and adequate control can reduce risks by 20-50%. Primary hypertension is usually essential and related to multiple genetic and lifestyle factors in 95% of cases. Treatment involves lifestyle changes, medication, and interventional procedures for resistant cases. Goals are to control blood pressure and reduce long-term health risks.