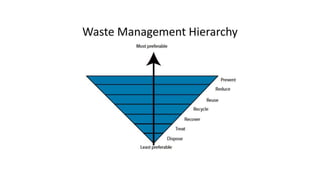
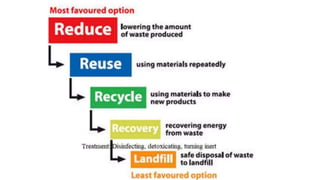
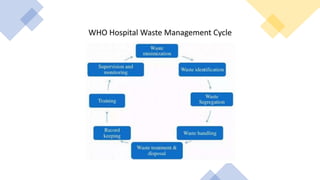
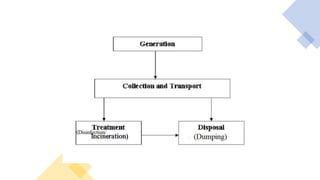
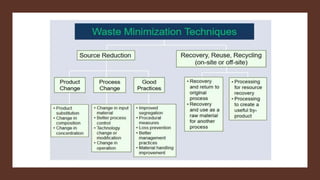
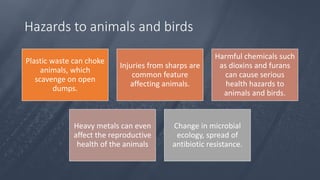
Healthcare waste can be categorized as infectious, sharps, pharmaceutical, hazardous, or domestic waste. Proper management is important to minimize health risks. Healthcare waste should be segregated at the source into color-coded containers. A waste management plan should address waste quantification, handling, treatment, disposal, personnel training, and costs. Key aspects of an effective plan include waste segregation, minimization of hazardous waste, staff education, and regular monitoring. Improper management poses infection and injury risks to healthcare workers and the public.