The document provides an overview of the cardiovascular system and components of blood. It discusses the anatomy and function of the heart, including the four chambers and valves. It describes the circulation of oxygenated and deoxygenated blood through the heart and major blood vessels. It also explains the conduction system that regulates heart rhythm. Furthermore, it outlines the three main types of blood vessels and defines the roles of arteries, veins and capillaries. Finally, it identifies the key components of blood, such as plasma, red blood cells, white blood cells and platelets, and their main functions.

















![Functions of the blood
1. InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. What does blood do? [Updated 2019 Aug 29]. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK279392/
1. Transportation 1
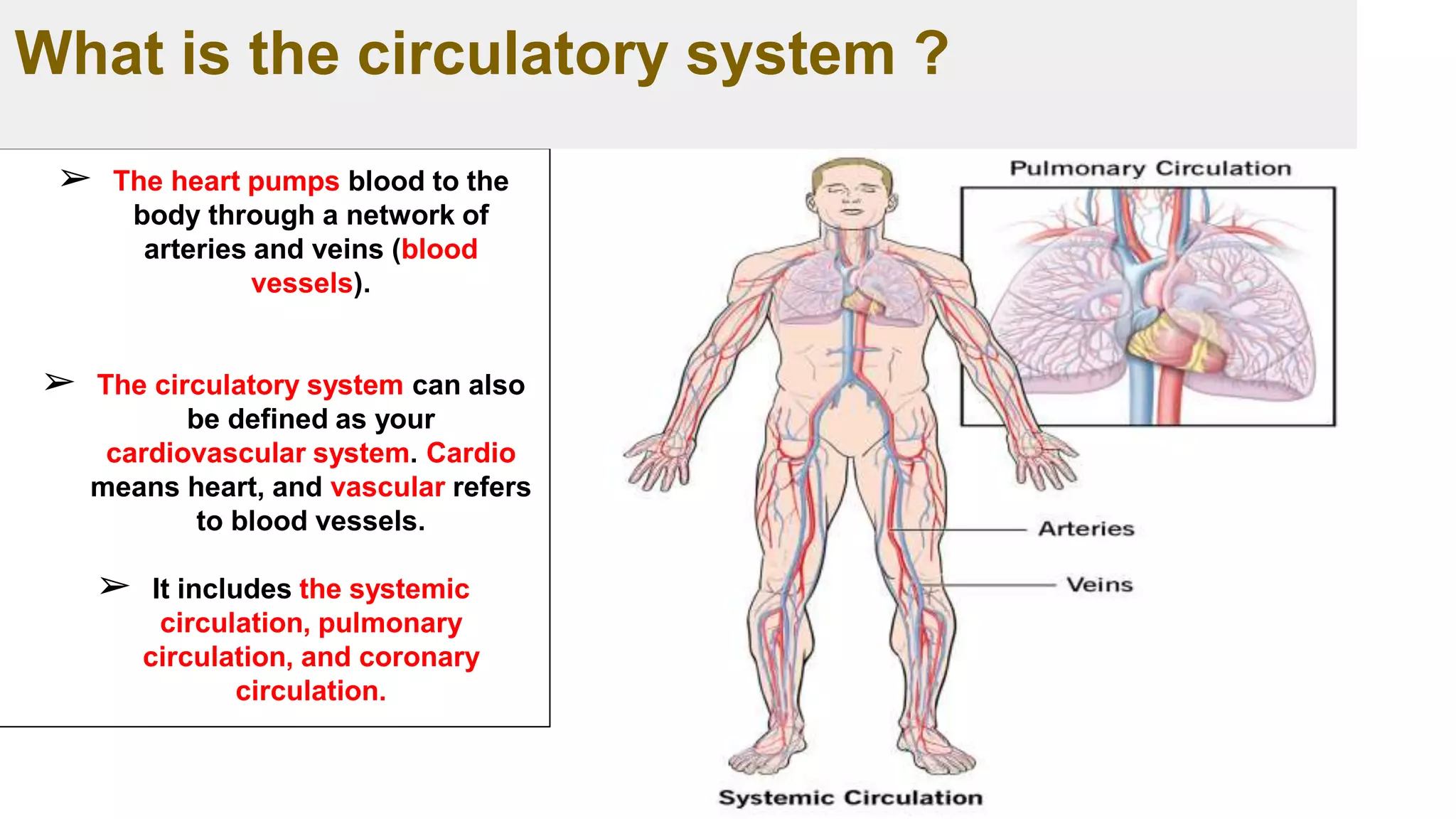
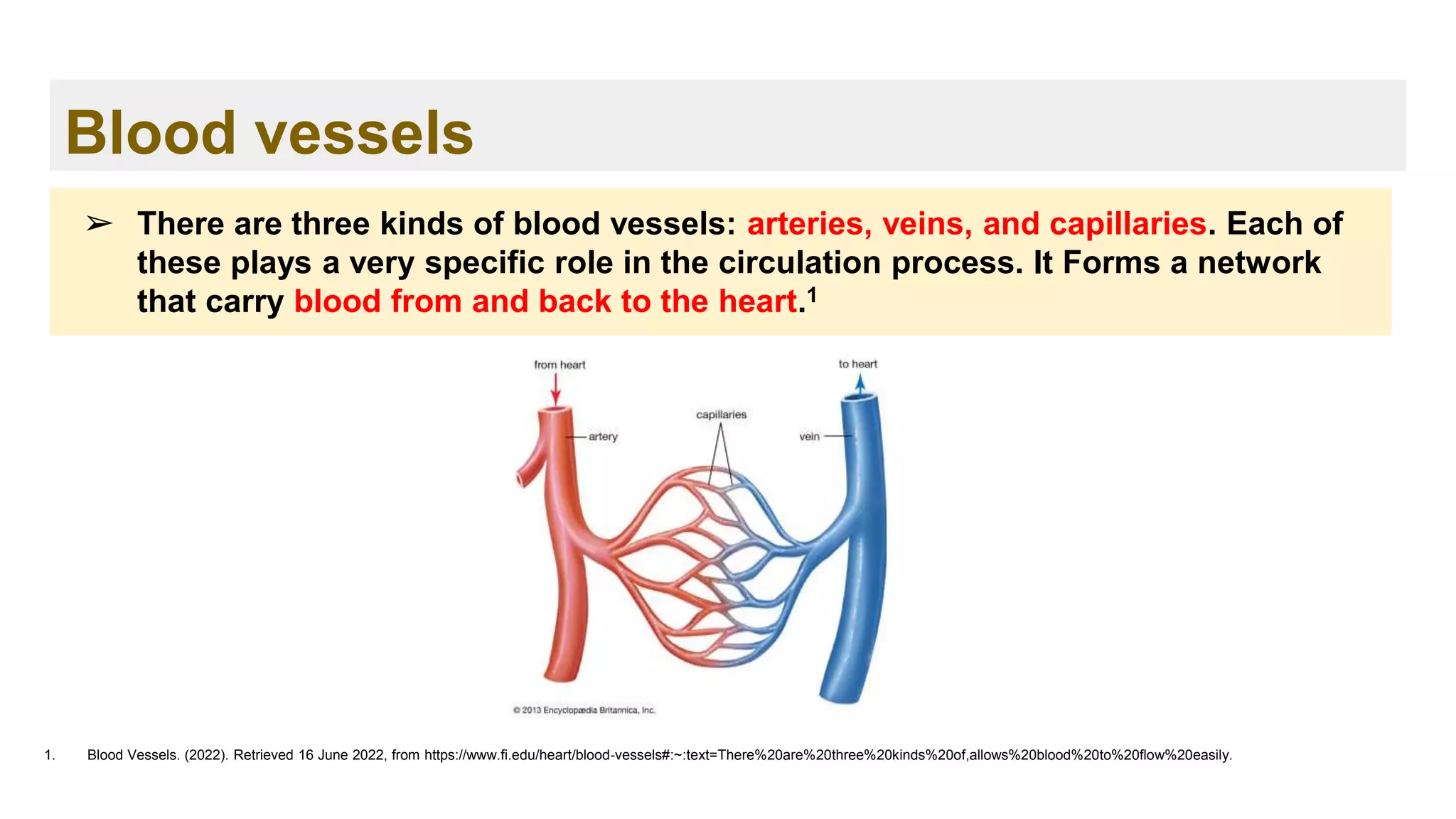
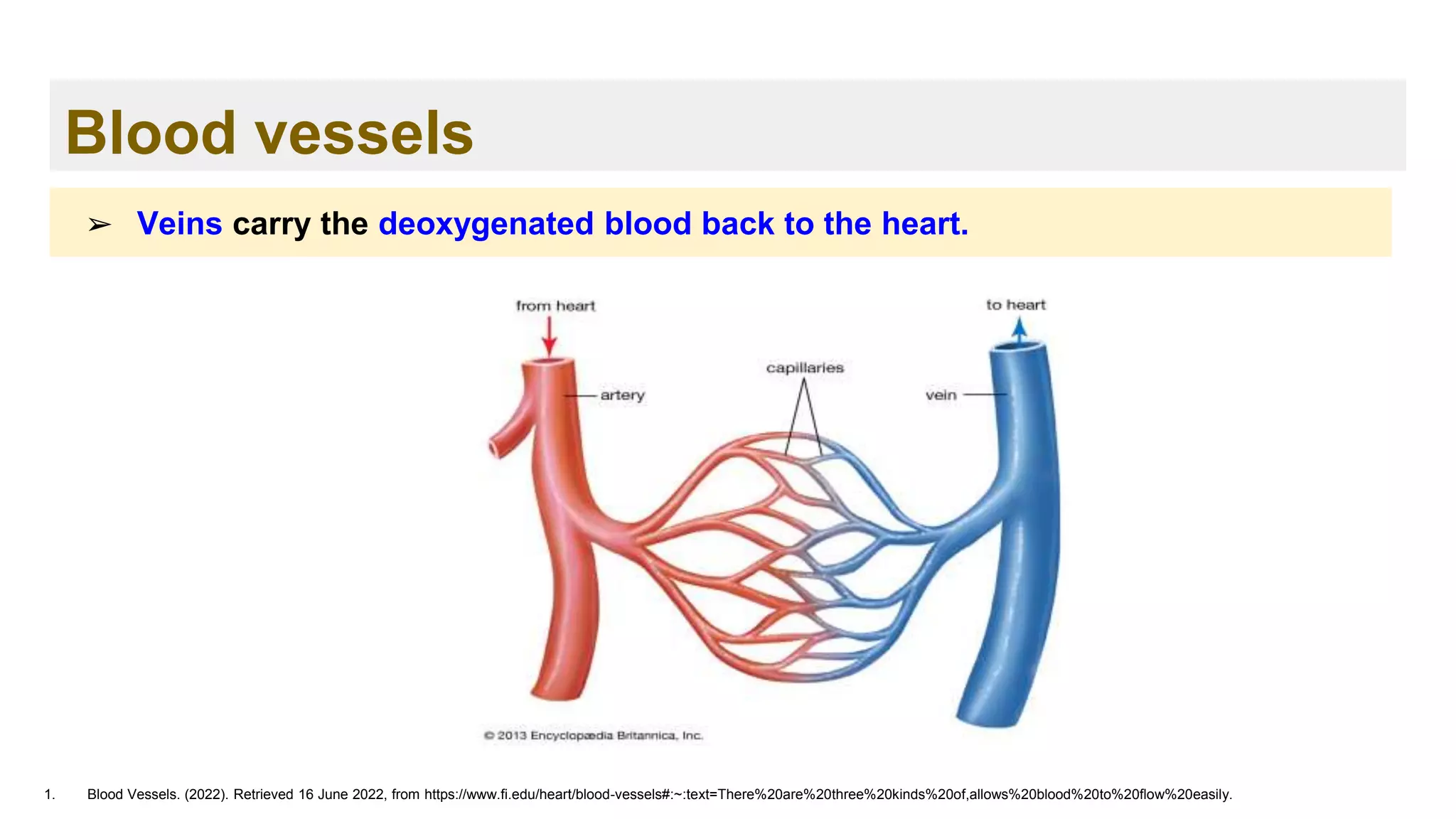
➢ The blood transports oxygen from the lungs to the cells of the body.
➢ The carbon dioxide produced is carried back to the lungs by the blood.
➢ Blood also provides the cells with nutrients, transports hormones and removes
waste products, which organs such as the liver, the kidneys or the intestine
then get rid of.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-24-2048.jpg)
![Functions of the blood
1. InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. What does blood do? [Updated 2019 Aug 29]. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK279392/
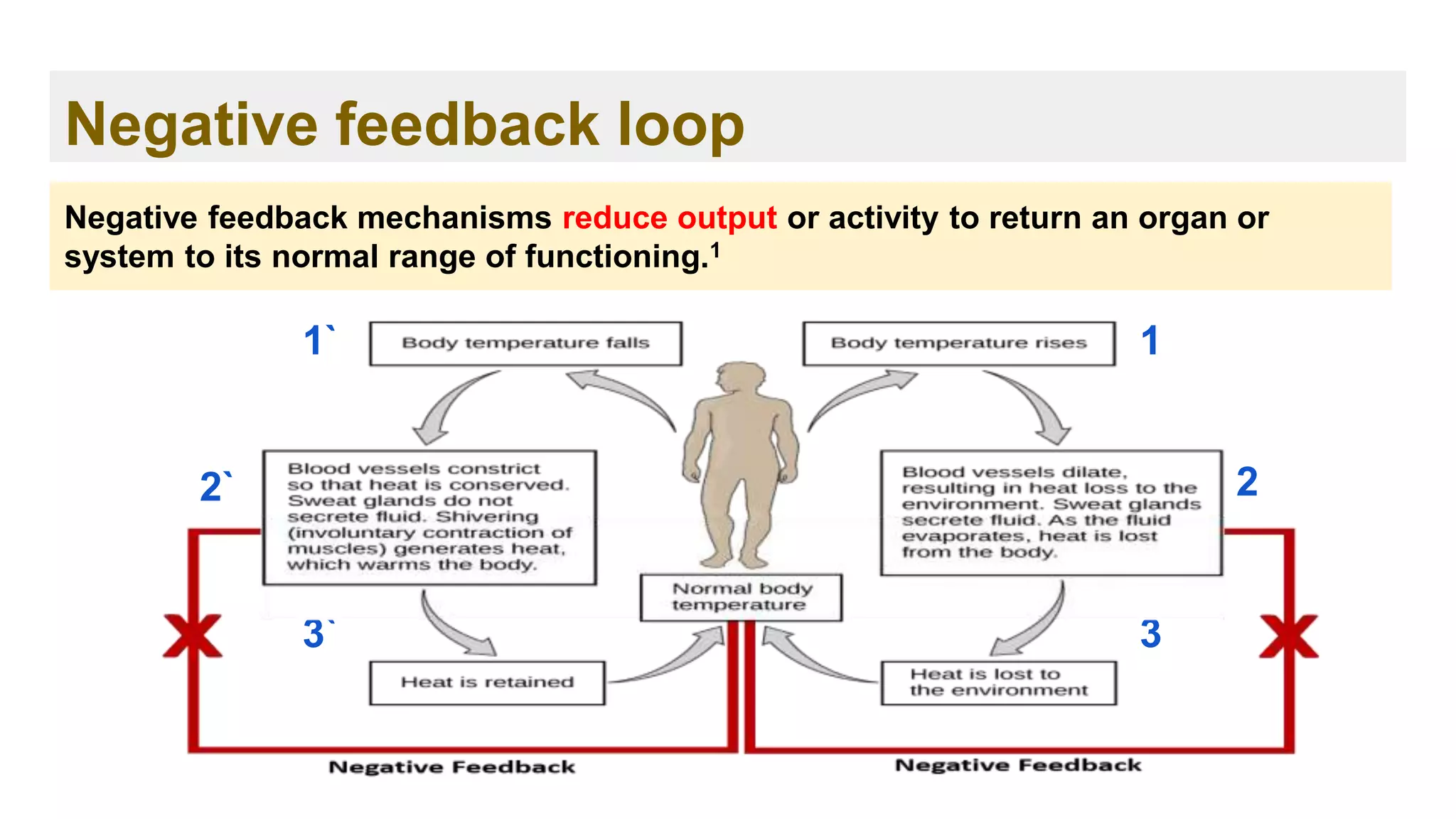
2. Regulation 1
➢ The blood makes sure that the right body temperature is maintained.
➢ When the blood vessels expand, the blood flows more slowly and this
causes heat to be lost. When the temperature outside the body is low,
the blood vessels can contract to reduce the amount of heat lost.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-25-2048.jpg)
![Functions of the blood
1. InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. What does blood do? [Updated 2019 Aug 29]. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK279392/
3. Protection1
➢ This involves parts of the blood such as blood platelets and coagulation factors
that are dissolved in the blood plasma, these parts of the blood stick together
(clot) very quickly and make sure that it stops bleeding.
➢ White blood cells and certain chemical messengers also play an important role
in the immune system.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-26-2048.jpg)
![Components of the blood
1. Blood Components. (2022). Retrieved 16 June 2022, from https://www.redcrossblood.org/donate-blood/how-to-donate/types-of-blood-donations/blood-components.html
2. Mathew J, Sankar P, Varacallo M. Physiology, Blood Plasma. [Updated 2022 Apr 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK531504/
Adapted from reference 1
Plasma contains 91% to 92% of water and 8% to 9% of solids. It
mainly comprises of:2
➢ Coagulants, mainly fibrinogen, aid in blood clotting.
➢ Plasma proteins, such as albumin and globulin, that help
maintain the colloidal osmotic pressure at about 25 mmHg.
➢ Electrolytes like sodium, potassium, bicarbonate, chloride,
and calcium.
➢ Immunoglobulins help fight infection and various other
small amounts of enzymes, hormones, and vitamins.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-27-2048.jpg)

















![Blood Clotting
1. Blood Clots [Internet]. Hematology.org. 2022 [cited 19 June 2022]. Available from: https://www.hematology.org/education/patients/blood-clots
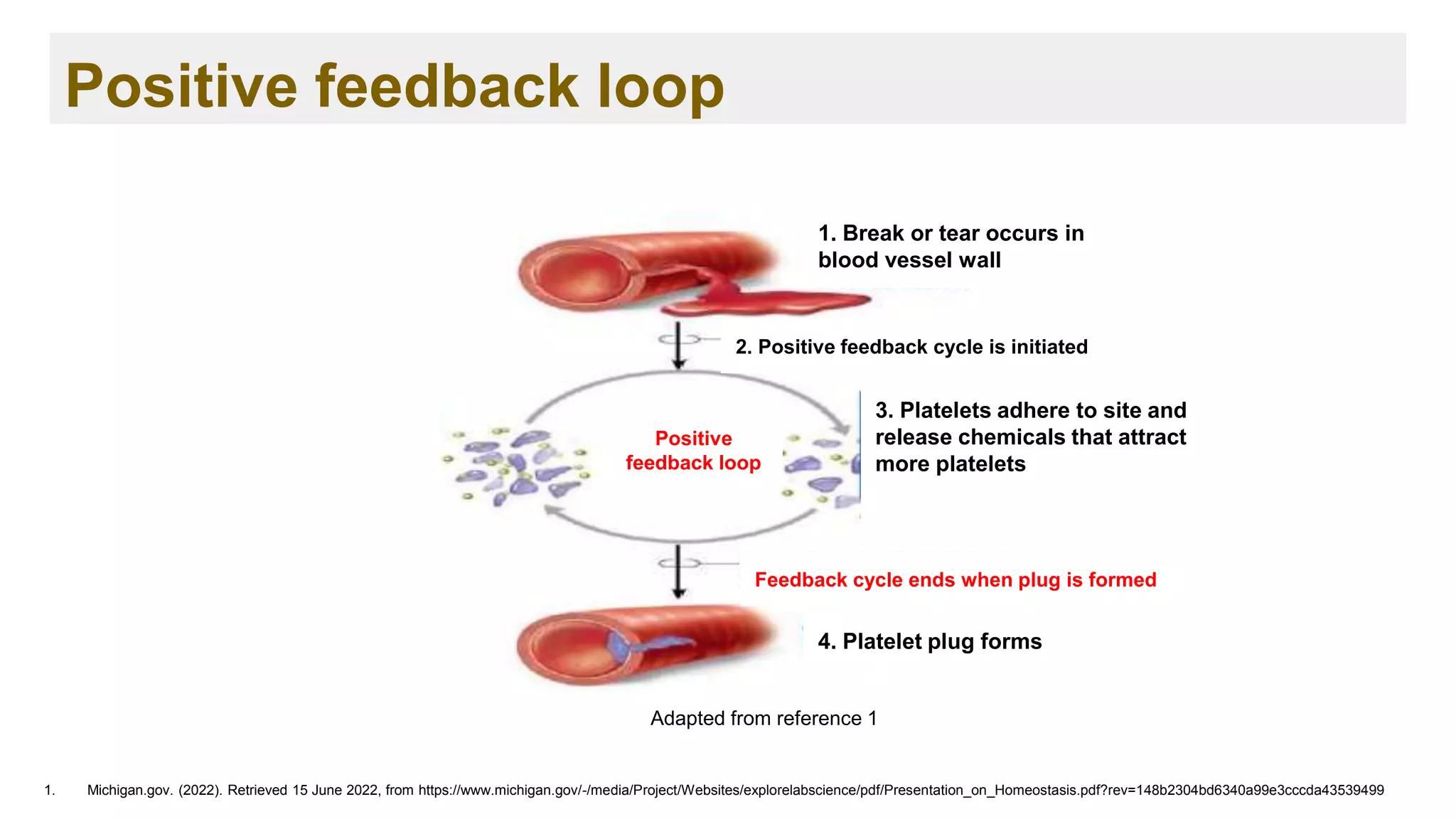
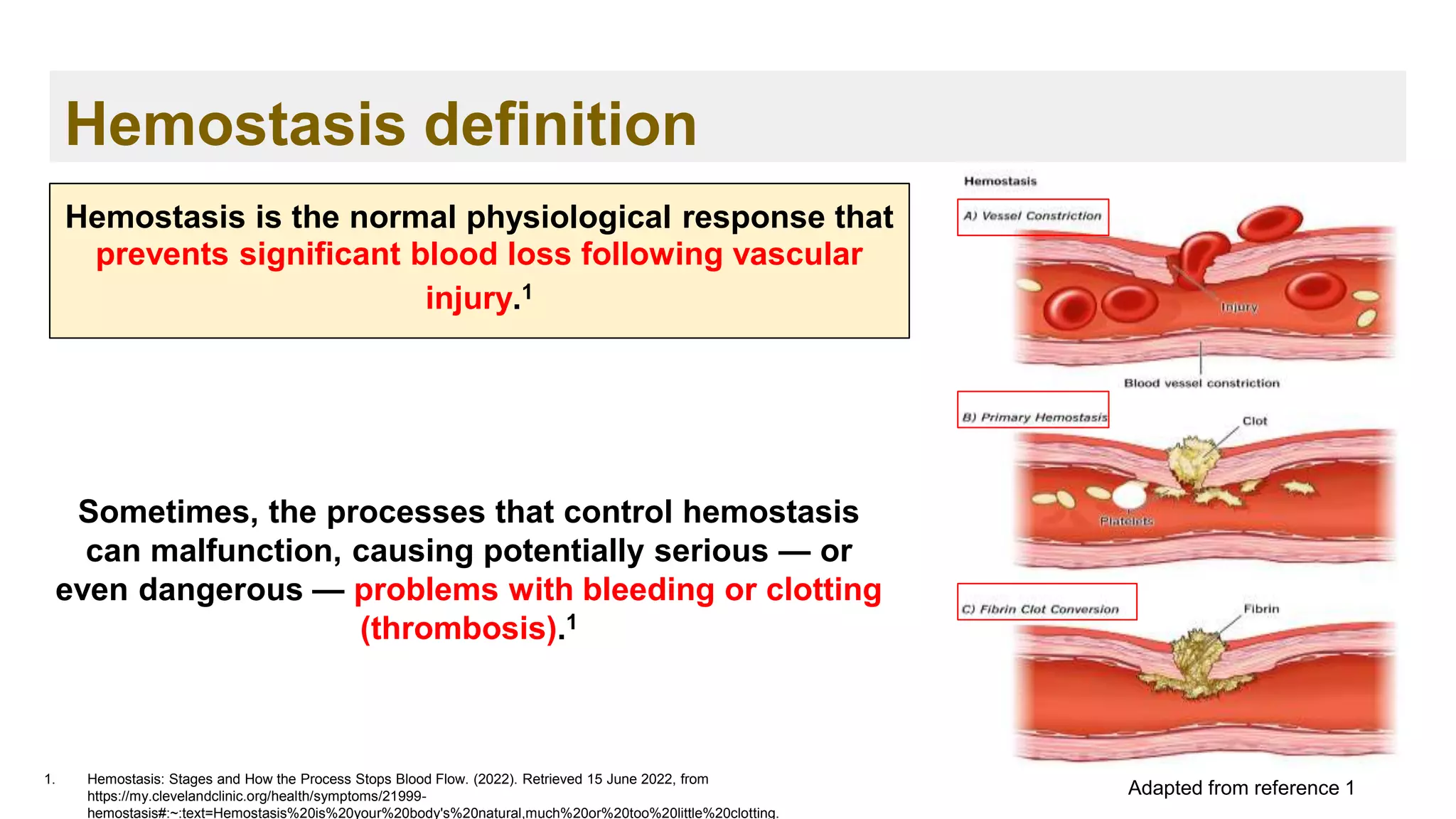
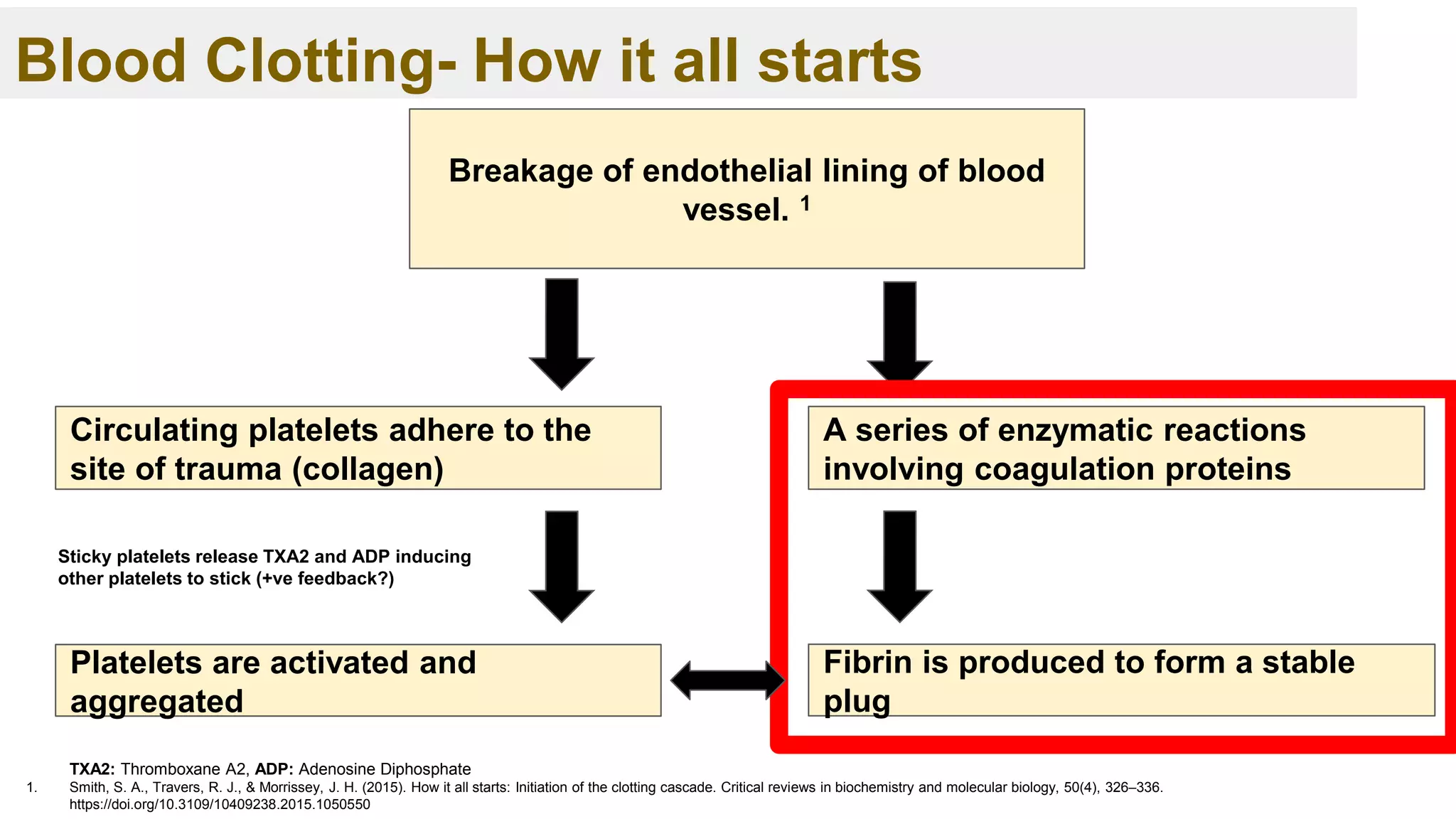
➢ Blood clotting, or coagulation, is an important process that prevents excessive
bleeding when a blood vessel is injured. 1
Promote hemostasis ( hemo = blood and stasis = standing)
➢ Platelets and proteins known as coagulation factors in your plasma work
together to stop the bleeding by forming a clot over the injury. 1
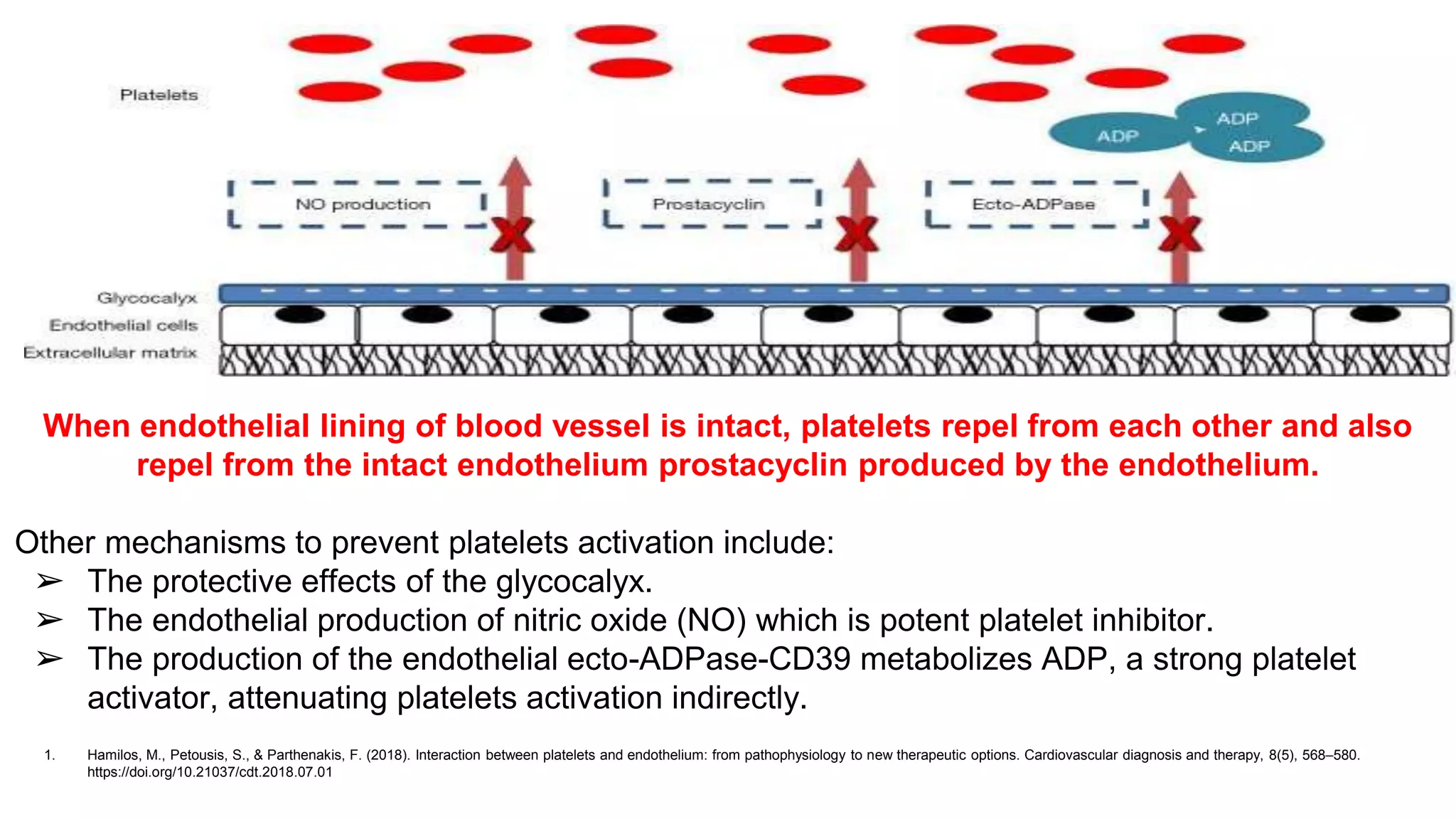
Under physiologic conditions platelets circulate without
adhering to intact and inactive endothelium.1](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-49-2048.jpg)






![Extrinsic Pathway
1. Chaudhry R, Usama SM, Babiker HM. Physiology, Coagulation Pathways. [Updated 2021 Sep 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK482253/
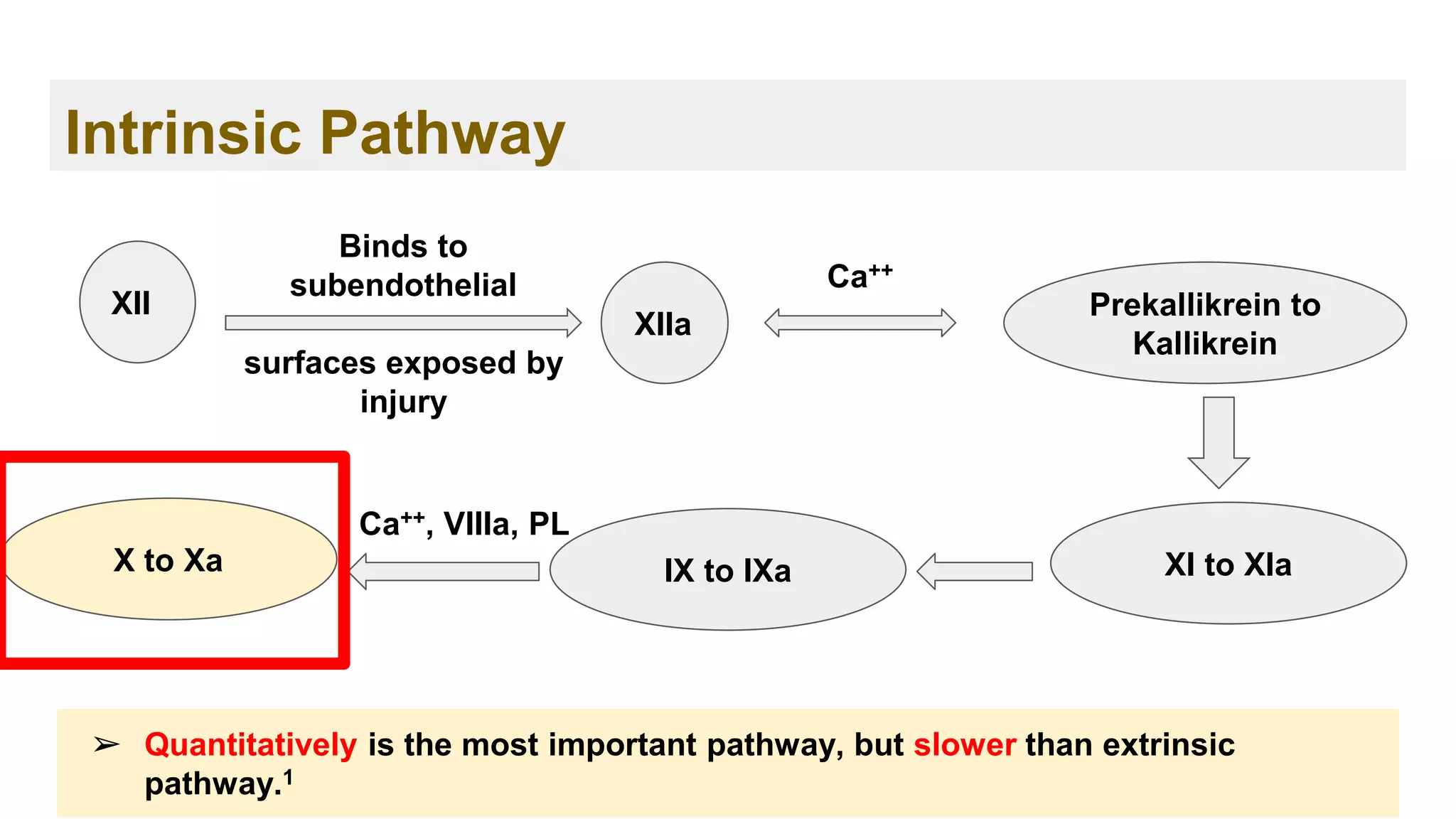
➢ The principle initiating pathway of invivo blood coagulation.
➢ The critical component is tissue factor embedded within and around blood
vessels and other tissue, under normal conditions it’s not exposed to blood.
➢ It’s main function is to augment the activity of the intrinsic pathway, it provides
a very rapid response to tissue injury.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-59-2048.jpg)
![Extrinsic Pathway
1. Chaudhry R, Usama SM, Babiker HM. Physiology, Coagulation Pathways. [Updated 2021 Sep 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK482253/
Tissue
factor
activation
VII to VIIa
Tissue factor
+ VIIa + PL +
Ca++
X to Xa](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-60-2048.jpg)
![The common Pathway
1. Chaudhry R, Usama SM, Babiker HM. Physiology, Coagulation Pathways. [Updated 2021 Sep 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from:
https://www.ncbi.nlm.nih.gov/books/NBK482253/
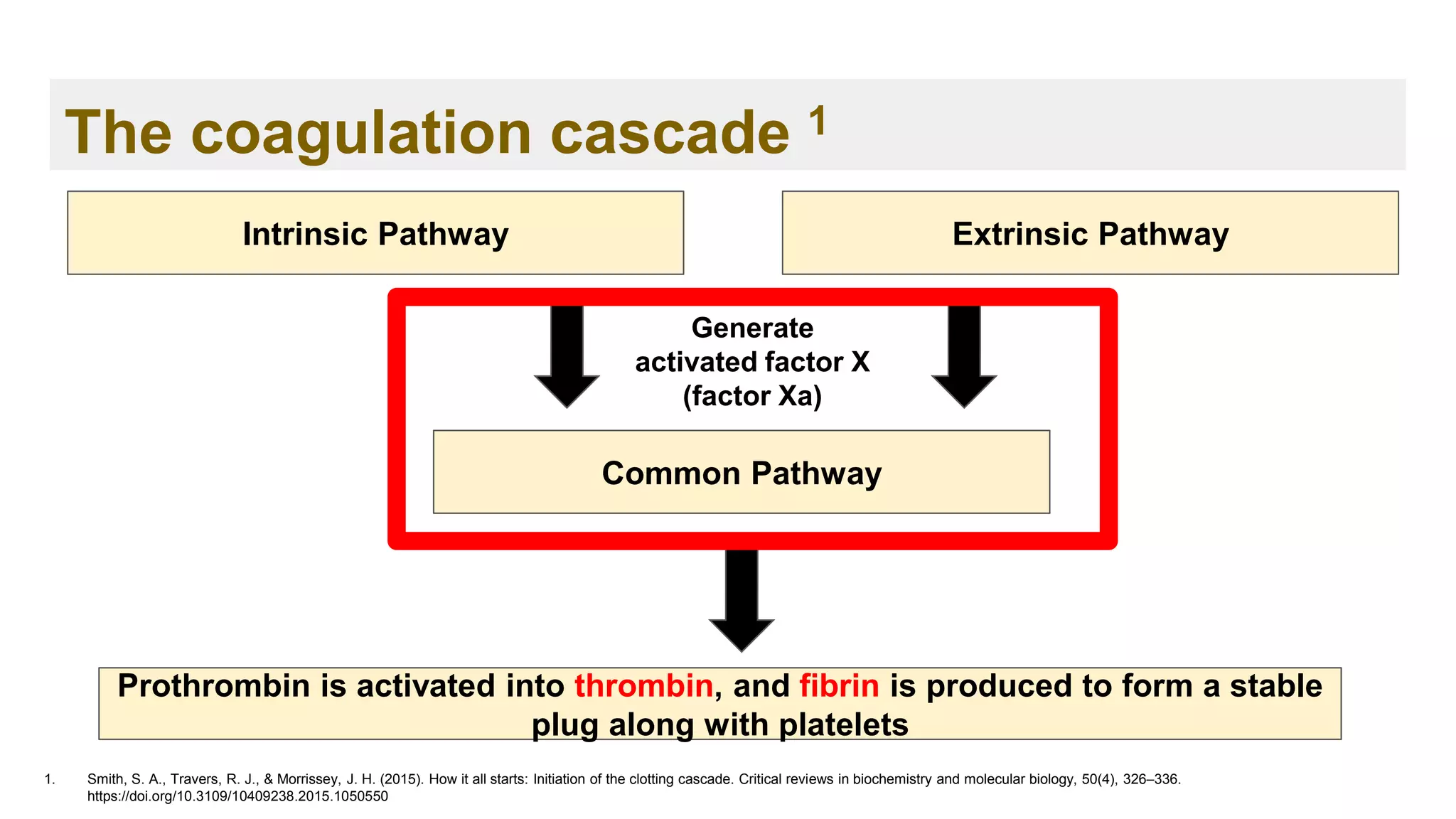
X to Xa
Extrinsic Pathway Intrinsic
Pathway
Prothrombin (II)
to Thrombin
(IIa)
Fibrinogen (I)
into Fibrin (Ia)
Stable blood
clot
Fibrin
stabilizing
factor (XIII) to
XIIIa
Ca++, Va, PL](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-62-2048.jpg)














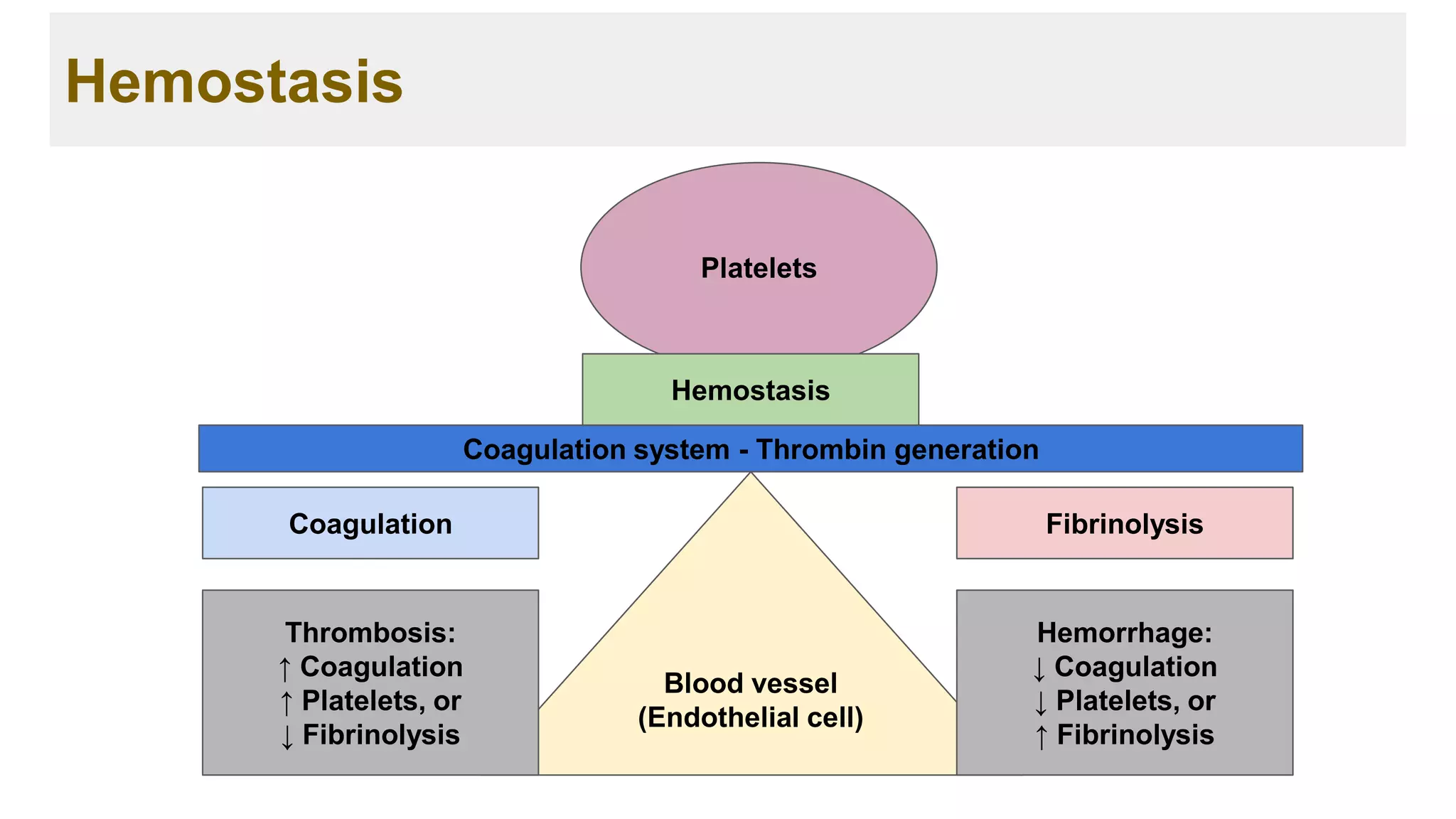

![Major diseases associated with thrombosis:
➢ Venous thromboembolism (VTE):
a disorder that includes deep vein thrombosis (DVT) and
pulmonary embolism (PE).1
DVT: Deep Vein Thrombosis, PE: Pulmonary Embolism
1. Thrombosis: Types, Causes, Symptoms & Treatment [Internet]. Cleveland Clinic. 2022 [cited 20 June 2022]. Available from: https://my.clevelandclinic.org/health/diseases/22242-thrombosis
➢ Cardioembolic stroke:
occlusion of cerebral vessels with debris from a cardiac source.1
➢ Atherothrombosis:
a condition that occurs when a thrombus forms over an unstable
atherosclerotic plaque.](https://image.slidesharecdn.com/ch-221114131524-9dc7d7f4/75/Hemostasis-and-Coagulation-cascade-81-2048.jpg)

