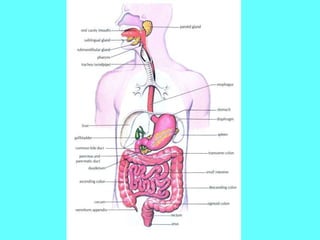
Gastric Dyspepsia
- 3. Dyspepsia - digestive disorders of different origin s. There are gastric and intestinal dyspepsia. T he term "gastric dyspepsia" combines symptom s such as heartburn, belching, regurgitation, na usea, vomiting, hiccups. They are observed not only in various diseases of the stomach, but in diseases of other organs and systems (central nervous system, endocrine system, liver, biliary tract, kidneys, and others.).
- 4. The organic reasons of dyspepsia: • Gastritis; • Stomach ulcer; • Reflux- esophagitis; • Stomach cancer; • Cholelithiasis; • Chronic pancreatitis.
- 5. Gastritis - inflammation of the mucous membrane of the stomach wall.
- 6. common causes of gastritis. The most common cause of gastritis is the bacterium Helicobacter pylori, however, co ntribute to the development of gastritis ma y be poor nutrition, constant stress, smoki ng, alcoholism, medications, error in nutriti on.
- 7. types of gastritis. etiological • 1. Helicobacter pylori (associated with Helicoba cter pylori) • 2. Autoimmune • 3. Reactive (due to duodenal reflux, bile reflux i nto the stomach or taking drugs) • 4. Special forms of gastritis (granulomatous, inc luding Crohn's disease, sarcoidosis, tuberculosi s, lymphocytic, eosinophilic)
- 8. types of gastritis. on the course of the disease. • acute gastritis • chronic gastritis topography • 1. Gastritis antrum • 2. The body of the stomach Gastritis • 3. pangastritis
- 9. types of gastritis. Endoscopic gastritis categories: • 1. erythematous-exudative (surface), gastritis • 2. atrophic gastritis • 3. hemorrhagic gastritis • 4. hyperplastic gastritis
- 10. Chronic H. pylori gastritis In the early stages of the disease developing atr ophic antral gastritis without secretory failure. Ulcer-like symptoms: • Pain in the epigastric 1-2 hours after a meal • Hunger pain (fasting) • Heartburn, acid regurgitation • A healthy appetite • The tendency to constipation
- 11. Objective clinical symptoms: • Language clean or slightly coated from root • Local tenderness in the area piloroduodenalnoy • Normal border stomach
- 12. In the late stages of the disease devel ops diffuse gastritis with atrophy of th e gastric mucosa and the secretory de ficiency.
- 13. Clinical symptoms: • Poor appetite, nausea • metallic taste in the mouth, dry mouth • Belching air, food, sometimes rotten • The feeling of heaviness in the epigastric • Dull epigastric pain after eating • Rumbling and flatulence • Frequent loose stools
- 14. Objective symptoms • Weight loss • Language thickly coated • Perleches in the corners of the mouth • Moderate diffuse pain in the epigastric region • Omission of the lower boundary of the stomach • Rumbling palpation of the large intestine due to t he pronounced flatulence
- 15. Perleches in the corners of the mouth
- 16. survey X - ray examination of the stomach: • Early stage (non-atrophic gastritis) - rough terrai n mucosa in the antrum, pyloric spasm, segmen ted peristalsis, disorderly evacuation of a contra st agent. • Late stage (pangastritis with atrophy) - relief of g astric mucosa smoothed, hypotension, sluggish perstaltika, fast evacuation of contrast material.
- 17. X - ray examination of the stomach
- 18. Gastroscopy • Early stage (non-atrophic gastritis) - blotchy red ness and swelling of the mucous membrane of t he antrum, frequent submucosal hemorrhage, e rosion, hyperplasia folds, exudation, antral spas ms, stasis. • Late stage (pangastritis with atrophy) - paleness , thinning, flattening of the mucous membrane i n the stomach and the antrum, blotchy flushing, candling vascular hypotension, increased vulne rability of the mucous, reflux of duodenal conten ts.
- 20. Gastroscopy
- 21. Gastroscopy
- 22. Mucosal erythema and edema co nsistent with acute gastritis.
- 23. Acute gastritis with superficial ero sions.
- 24. Histopathological examination (biopsy taken at least 2 pieces of the antrum and the body (front and rear), a lways with a muscular plate): • Early stage (non-atrophic gastritis) - pronounced active antral gastritis (infiltration own skin epithelial lymphocy tes, plasmocytes, neutrophils), foci of intestinal metapl asia, a lot of helicobacter surface and mucous pits. • Late stage (pangastritis with atrophy) - glandular epithe lium atrophy, intestinal metaplasia, a small amount of helicobacter in gastric mucosa and antrum, the minim al activity of inflammation.
- 25. Diagnosis of Helicobacter pylory: Histological method for determining Helicobacter pylori is the gold standard of diagnosis: • Thin slices of biopsy specimens stained by the method of Giemsa-Romanovsky, Helicobacter l ocated in the mucus, have a spiral shape. There are three degrees of contamination Helioba cter pylory: • Low () - 20 microbial cells in the s.v. • Average (++) - up to 50 microbial cells in the s.v . • High (+++) - more than 50 microbial cells in the s.v.
- 26. Chronic autoimmune gastritis. Chronic autoimmune gastritis is chara cterized by lesions of the gastric fund us, atrophy of the gastric mucosa and the secretory deficiency.
- 27. Subjective symptoms • feeling of heaviness and fullness after eating • Belching air, rotten, food sedennoy • metallic taste in the mouth • Poor appetite • Rumbling transfusions and stomach, unstable st ool • severe weakness, dizziness, sweating (function al dumping syndrome)
- 28. Objective symptoms • Weight Loss • pale skin (anemia), hair loss, brittle nails • Dry skin, hyperpigmentation (gipokortitsizm) • Signs gipopolivitaminoza (dry skin, blurred vision, blee ding of gums and loosening, Zayed corners of mouth, dermatitis, diarrhea) • coated tongue • Sore epigastrii • Morbidity and rumbling in the umbilical and the ileocec al region • Omission of the greater curvature of the stomach
- 29. X-ray examination of the stomach Improvement in the folds of the stomach lining
- 30. Gastroscopy • The folds of the gastric mucosa are reduced in v olume, in advanced cases of atrophy, they can be absent • stomach lining thinned, atrophic, pale, clearly vi sible vascular pattern, an excessive amount of mucus • hiatus gatekeeper, throw the stomach contents of 12 duodenal ulcer, gastric motility sluggish • antrum is not changed
- 31. Histopathological examination • atrophy of the mucous membrane of the fundus of the stomach with the replacement of speciali zed glands psevdopiloric glands and intestinal e pithelium.
- 32. Immunological blood tests • The presence of autoantibodies to parietal cells and gastromukoproteinu.
- 33. Special forms of gastritis. Hypertrophic gastritis (Menetries disease). Subjective symptoms: • Intense epigastric pain occurring after meals, he artburn, regurgitation, air and food • Frequent vomiting with blood • Anorexia • Weight loss, swelling of the feet and hands • Diarrhea • Hypoproteinemia
- 34. Special forms of gastritis. Hypertrophic gastritis (Menetries disease). Gastroscopy: • Hypertrophy of the mucous membrane in the for m of giant folds, covered with lots of sticky muc us. Histopathological examination: • The sharp thickening of the gastric mucosa, ext ension and expansion of the gastric pits
- 35. Hypertrophic gastritis (illness Menet ries).
- 36. treatment
- 37. treatment 1. Sparing diet. Vegetables boiled, steamed zucc hini, potatoes, carrots, cabbage, beans, beets, dairy products, fruit and berry juices, sauces, spices, snacks, tea, coffee and black with milk , broth hips, black currant). Excluded are indig estible, long linger in the stomach and dishes. Fractional meals 4-5 times a day.
- 38. treatment Anti-inflammatory therapy • Sucralfate (Venter) Tablets (1 g) 1 tab four time s daily (for 1 hour before meals and at bedtime) or 2 g in the morning and evening. The course of treatment 2-4 weeks or • De-nol (colloidal bismuth subcitrate) Tablets (12 0 mg) 1 tablet three times a day 30 minutes bef ore meals and at bedtime. The course of treatm ent 4 - 8 weeks. For 30 minutes before and afte r taking the drug should not take antacids, milk, beverages, solid food.
- 39. treatment Cementing and enveloping substance • Allonton (drug inula) Tablets (0.1) 1 tab. 2-4 tim es for 30 min. before meals or • Kaleflon (extract from marigold flowers) Tablets (0.1) Table 1-2. 3 times per day after meals
- 40. treatment Stimulators of gastric secretion • Trental (metabolic drug in combination with the i mprovement of microcirculation) 100 mg 1-2 tab . 3 times for 30 min. before meals for 1-2 month s. or • Pentagastrin (synthetic analog of histamine) Am poule 0.025% -1.0 s/c before meal 1-2 times a day for two weeks
- 41. treatment replacement therapy drugs. • Gastric juice natural vials of 1-2 tablespoons int o ½ cup of water through a straw while eating or • Citric acid powder on the tip of a knife into ¼ cu p of water with meals or • Atsidin-pepsin tablets (0.5) Table 1. dissolved in ½ cup of water with meals
- 42. treatment prokinetics. • Metoclopramide (raglan, Reglan) Tablets (0.01) Ampules (1 ml-0.005) 10-20 mg 3-4 times a day for 15-30 minutes before meal, maximum daily dose of 60 mg or • Motilium (domperidone) Tablets 0.01 mg 10-20 3-4 times a day for 15-30 minutes before meals, daily dose - 60 mg
- 43. treatment • Pancreatin Tablets 0.5-1.0 The enzyme prepara tion from the pancreas of beef cattle. Table 1-2. before meals 3-4 times or • Mezim forte preparation containing pancreatic e nzymes 1-2 tab. 3 times daily before or during meals
- 44. treatment Antibiotics to treat Helicobacter pylori
- 45. Peptic ulcer
- 46. Peptic ulcer - an independent (primary) chronic relapsing disease gastroduodenal region with th e formation of ulcers of the stomach and duode num.
- 47. Peptic ulcer Peptic ulcer duodenal bulb (PUD) occurs 4 time s more often than gastric ulcer (GU). Peptic ulcer duodenal bulb - is more common in t he age range 25-75 years (rarely less than 15 y ears). GU - occurs more often aged 55-65 (rarely young er than 40 years).
- 48. The criteria for early diagnosis. • epigastric pain - in the center or left of the midlin e at a stomach ulcer, epigastric right of the midli ne - duodenal ulcer and prepiloric area with ga stric cardia of the stomach - in the sternum. • Early pain (30 minutes - 1 hour after a meal) - at the top of the stomach ulcer, recent pain (1.5 - 2 hours after a meal), night and hungry (after 6- 7 hours after eating) - ulcer antral department a nd duodenal ulcer.
- 49. The criteria for early diagnosis. • Dumb nature of pain can be aching, boring • The frequency of pain • Relief of pain - after antacids, milk, food, of ten after vomiting • Seasonality pain - spring, autumn, charact erized more for duodenal ulcer • Heartburn
- 50. The criteria for early diagnosis. • Belching, often occurs in the localization fi eld mesogastric • Nausea – characteristic for mediogastral ul cers, but not characteristic of ulcer 12 duo denal ulcer • Vomiting - at an altitude of pain • Appetite - kept, good
- 52. The criteria for early diagnosis. objective: • Asthenia • The tendency to bradycardia • Tendency to hypertension • Moderate or severe pain in the epigastric in acut e: gastric ulcer - midline or left, ulcer 12 duoden al ulcer over the right • percussion tenderness over the area of the ulcer - a symptom of Mendel • Local protective tension anterior abdominal wall
- 53. The criteria for early diagnosis. Laboratory research: • CBC - a slight increase in red blood cells and h emoglobin • Fecal occult blood test (reaction Gregersen) - p ositive for bleeding from the ulcer
- 54. The criteria for early diagnosis. Endoscopy: • Ulcers round, polygonal or slit form • Borders ulcers crisp, edge bloodshot, swollen • Undermining the ulcer edge (facing the cardiac department), the distal end flat • The bottom of the ulcer is covered with fibrin
- 58. Gastric ulcer with punched-out ulcer base with whitish fibrinoid exudates.
- 59. Gastric ulcer (lesser curvature) with punched -out ulcer base with whitish exudate.
- 60. The criteria for early diagnosis. X-rays: Direct indication of the "niche" Indirect signs: • Delay barium mass at the site of the ulcer (contrast stai n resistant) • Delayed or accelerated passage of barium sulfate of st omach • Duodenalnogastralny reflux • Convergence folds at locations ulcers • Lack of cardia, gastroesophageal reflux • Local stomach cramps or 12 duodenal ulcer • Symptom De Quervain - circular retraction of the muscl es on the opposite side of the stomach ulcer - deforma tion of the stomach and duodenum
- 61. X-rays
- 62. Determination Helicobacter pylori • urease breath test - identifying exhaled C13 isotopes w hich are formed in the stomach during digestion drunk labeled urea by the action of urease HP • histological methods - detection of HP in biopsies stain ed by the method of Giemsa • urease biopsy test - determination of urease activity of HP in biopsies • The bacteriological test - the growth of HP biopsy • Immunological methods - determination of antibodies in the blood to HP, HP detection of antigen in stool
- 63. Required laboratory tests • Complete blood count - once (In the event of rep eated study of 1 every 10 days) • Blood type • Fecal occult blood test
- 64. The severity of the ulcer Mild - is characterized by the following features: • Exacerbations 1 time in 1-3 years • Pain syndrome moderate pain stoped for 4-7 da ys • shallow ulcer • The remission disabled preserved
- 65. The severity of the ulcer moderate severity: • Relapse 2 times a year • Pain syndrome pronounced pain stoped in the h ospital for 10-14 days • Characterized dyspepsia • Ulcers deep, often bleeds, accompanied by phe nomena perigastritis, periduodenitis
- 66. The severity of the ulcer Severe: • Relapse 2-3 times a year and more • Pain and pronounced cropped in the hospital for 2 weeks or more • Sharply expressed dyspeptic symptoms and wei ght loss • The ulcer is often complicated by bleeding, deve lopment of pyloric stenosis, perigastritis, peridu odenitis
- 67. Complications of peptic ulcer disease. • Peptic ulcer bleeding is observed in 15-25% of patie nts with peptic ulcer disease, often with stomach ulcer s localization • Ulcer perforation occurs in 5% of patients with peptic ulcer disease, more common in men. • Penetration - penetration of gastric ulcer or duodenal ulcer in the surrounding tissues: the pancreas, a small gland, gall bladder, and others. • Perivistserit - adhesive process that evolves with ulce rs between the stomach or duodenum and adjacent or gans (pancreas, liver, gall bladder). duodenum.
- 69. Complications of peptic ulcer disease. • Pyloric stenosis usually formulated after ulc er healing located in the pyloric channel or the i nitial part of the duodenum, is found in 5% of pa tients. • The risk of malignancy (adenocarcinoma devel opment) benign ulcers when infected with HP 9 times more likely than uninfected patients.
- 70. treatment 1. Medical treatment - mental and physical rest, n ot strict bed rest for 7-10 days, then free. 2. Diet - table 1 a, 1 b for 2-3 days, then the table 1. The food is cooked, but not shabby, eat 5-6 ti mes a day are not recommended sharp, pickled , smoked food. The optimum amount of protein i n the diet of 120-125 g / day. 3. Giving up smoking. 4. Pharmacotherapy.
- 71. treatment H. pylori therapy • First-line therapy (triple therapy) for 7 days Omeprazole 20 mg 2 times a day, or Lansoprazole 30 mg 2 times a day, or Pantoprozol 40 mg 2 times a day + Clarithromycin 500 mg 2 times a day + Amoxicillin 1000 mg 2 times a day or Clarithromycin 500 mg 2 times a day + Metronidazole 500 mg 2 times a day
- 72. treatment H. pylori therapy • First-line therapy (triple therapy) for 7 days Omeprazole 20 mg 2 times a day, Clarithromycin 500 mg 2 times a day Amoxicillin 1000 mg 2 times a day
- 73. treatment H. pylori therapy Second-line therapy (quadruple) for 7 days Omeprazole 20 mg 2 times a day, or Lansoprazole 30 mg 2 times a day, or Pantoprozol 40 mg 2 times a day + Bismuth subsalicylate 120 mg four times a day + Metronidazole 500 mg three times a day + Tetracycline 500 mg four times a day
- 74. treatment H. pylori therapy Second-line therapy (quadruple) for 7 days Omeprazole 20 mg 2 times a day, Bismuth subsalicylate 120 mg four times a day Metronidazole 500 mg three times a day Tetracycline 500 mg four times a day
- 75. stomach cancer
- 76. stomach cancer Stomach cancer - a malignant tumor growing fro m the epithelial cells of the mucosa (inner) mem brane of the stomach. Swelling can occur in diff erent parts of the stomach: at the top, where it c onnects with the esophagus, in the main part (b ody) of the stomach or in the bottom where the stomach is connected to the intestines.
- 77. stomach cancer Risk factors for gastric cancer • Genetic predisposition - if someone in the family d iagnosed with stomach cancer, then all the other r elatives (blood) relatives likely to develop increase d by 20%; • eating habits - overreliance smoked, spicy, salty, f ried (overcooked) and canned food, long stored fo ods containing nitrates, significantly increases the risk of stomach cancer; • long-existing diseases of the stomach: gastritis (w ith low acidity), ulcers and polyps of the stomach; • gastric surgery increases the risk of gastric cance r development is 2.5 times;
- 78. stomach cancer Risk factors for gastric cancer • the presence of the stomach bacterium Helicobact er pylori: In 1994 the World Health Organization (W HO) has recognized the link between Helicobacter Pylori and stomach cancer and the bacteria broug ht it into the category of carcinogens of the first cl ass; • Work with asbestos and nickel; • deficiency of vitamin B12, and C; • primary and secondary (e.g., AIDS), immunodefici ency states; • 20 times more common in gastric cancer patients with pernicious (malignant) anemia; • Some viruses, such as Epstein-Barr virus; • alcoholism and smoking.
- 79. stomach cancer clinical picture • decreased appetite; • changes in eating habits, for example, they feel an aversion to meat, fish and etc .; • rise in temperature (usually 37-38 ° C); • anemia (decreased hemoglobin).
- 80. stomach cancer clinical picture With the growth of stomach cancer, new symptoms: • a feeling of heaviness in the stomach after eating, nau sea and vomiting, fast saturation; • violation stool (diarrhea, constipation); • pain in the upper abdomen, girdle pain, smack in the b ack (in the propagation of the tumor in the pancreas); • increasing the size of the stomach, fluid accumulation i n the abdomen (ascites); • weight loss; • the destruction of tumor blood vessels may develop ga strointestinal bleeding.
- 81. Physical examination Objective methods of inspection (survey, pa lpation, percussion) allow revealing a stom ach cancer only at late stages of disease.
- 82. TOOL METHODS of INVESTIGATION • gastroscopy with biopsies. • computed tomography • US • x-ray study.
- 83. Gastric cancer. Note the irregul ar heaped up overhanging margi ns.
- 84. Gastric cancer with ulcerated ma ss.
- 85. Thank you for the attention.
