This study evaluated a new minimally invasive technique for inserting an equine stented pulmonary valve through a right ventricular approach without using cardiopulmonary bypass. The valve consisted of an equine jugular vein sutured into a self-expanding nitinol stent with a sinus portion. In seven lambs, the valve was successfully inserted through a right minithoracotomy and released in the pulmonary position using a flexible hydraulic delivery system. At follow-up of up to six months, echocardiography showed the valves were well-positioned and functioning properly. Histological analysis demonstrated endothelialization of the valves. This new approach may provide an alternative to existing surgical and percutaneous pulmonary valve replacement methods.

![include either surgical reoperation with cardiopulmo-
nary bypass [1], or percutaneous PVR under fluoro-
scopic guidance [2]. In animal experimental models,
research is underway to investigate off-pump insertion
of a functional pulmonary valve, using a combination
of minimal invasive surgical technique and percutane-
ous release systems [3–6], which have also been
reported in scant case reports in humans [7,8]. Inde-
pendently of the mode of insertion, the extant biologi-
cal valvar implants all have a limited life span, so that
the grail in the search of the ideal pulmonary valve
replacement remains to be found. Furthermore, percuta-
neous valve insertion has inherent limitations due to
the size of the device, the vessels and the patients, ren-
dering new solutions to approach mandatory to expand
the indications for an ever-growing patient population
in need of a competent pulmonary valve.
Attempting to overcome the drawbacks inherent to
the current systems, we describe the first time implan-
tation of a decellularized biological valve made from
an equine jugular vein, sutured into a self-expanding
nitinol stent with a sinus portion using a hydraulic
stent-delivery and release system, and describe our ex-
perience with regards to minimally invasive surgical
insertion of this prosthesis in a sheep survival model.
MATERIAL AND METHODS
A new equine stented pulmonary valve, with a built-
in sinus portion, and a hydraulic mechanism release de-
vice to allow transventricular valve release were newly
developed. The valve consisted of an equine jugular
vein, freshly harvested from the slaughterhouse. After
removal of surrounding tissue, the valve areas were
identified and the vein was cut in pieces containing
working valves. The grafts were decellularized and
sutured with running sutures into a self-expanding niti-
nol stent.
The self-expanding stent is laser-cut out of a nitinol
tube, with a sinus portion fitting to the natural shape of
the valve area. Two sizes of stents were used: the di-
ameter of the stent at the tubular part was 22 and 25
mm, respectively, and the sinus portion had a maxi-
mum diameter of 25 and 27.5 mm, respectively. The
length of the stent in its expanded shape was 29 mm.
Thanks to the sinus portion of the stent, the valve is
able to work in its natural manner to reduce or elimi-
nate the so-called ‘‘hammock effect.’’ The stent has
eyes at the proximal end to allow for a controlled
release (Fig. 1).
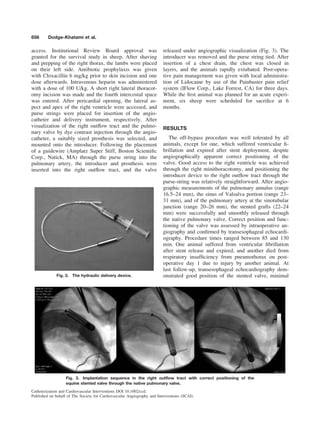
The delivery instrument consists of a stent chamber
with an outer diameter of 25 F and a very flexible
delivery catheter with a diameter of 6 F. The stent con-
taining the valve is crimped down to the necessary di-
ameter and loaded into the stent chamber prior to
delivery. A silicone tip is fixed to the distal end of the
delivery instrument to ease insertion of the instrument
through the myocardium, and reduce the risk of injury
to the vessels (Fig. 2). At the distal end of the instru-
ment, a luer lock connection allows safe and leak-proof
hydraulic connection of a standard 5 ml syringe. The
stent release is carried out by loading hydraulic pres-
sure on the stent chamber using sterile saline. During
release, the instrument can be locked into position,
which eases positioning. The instrument can be deliv-
ered over a 0.03500
guide wire.
Between November 2009 and August 2010, seven
Gotlandsfar lambs weighing 34–56 kg underwent a
right minithoracotomy for surgical insertion of the
stented equine valves, through direct right ventricular
Fig. 1. Stented equine graft displaying the sinus configuration of the stent and the tricuspid leaflets.
Equine Stented Pulmonary Valve Insertion 655
Catheterization and Cardiovascular Interventions DOI 10.1002/ccd.
Published on behalf of The Society for Cardiovascular Angiography and Interventions (SCAI).](https://image.slidesharecdn.com/fe9b8b7f-8128-4787-b794-2d30281f90e5-161219233548/85/equine-valve-Gothenburg-Catheterization_and_Cardiovascular_Interventions-2-320.jpg)
![to mild central pulmonary insufficiency, and peak gra-
dients of 3–16 mm Hg over the right outflow tract.
Histological analysis of the explanted grafts was per-
formed in one sheep after 1 month (unplanned death
from pneumonia), in another after 3 months (unplanned
death from bacteremia, heart failure with pericardial
effusion and tamponnade), and in two animals as
planned at 6 months. Macroscopically, pliable free-
moving transparent non-calcified leaflets were observed
in all four animals. At 3 months in one animal, no
reendothelialization on the decellularized graft was
observed. Bacterial colonies together with findings
from pathology confirmed a postoperative bacterial
infection leading to sepsis, with valve leaflets sur-
rounded by fibrin. Histological examination at 6
months showed a layer of endothelial cells on the sur-
face of the valve (Fig. 4). Scant lymph follicles in one
graft wall indicated a mild unspecific immunogenic
reaction. Light vascularization of the graft wall was
observed.
DISCUSSION
Surgical pulmonary valve replacement through
repeat sternotomy using cardiopulmonary bypass is a
standardized procedure with excellent results [1], but is
considered a relatively invasive procedure. Percutane-
ous approaches for PVR may reduce the invasiveness,
are also widely accepted, but currently still have lim-
ited application due to prosthesis-vascular access mis-
match. Common to both approaches is the biological
fate and reduced longevity of the extant prostheses
available, be they of human or animal origin, rendering
any measure at best palliative. More recently, research
and clinical attempts are striving for transventricular
access to the right outflow, using a combination of
minimally invasive surgical techniques and percutane-
ous technology [3–8].
Advantages of the newly designed stent with a sinus
portion include the creation of vortex flow, which is
very important to promote active closure of the valve,
also avoiding the so called ‘‘hammock effect’’ [9].
Vortex flow reduces wear and shear stress, and there-
fore increases the durability of the valve cusps [10,11].
In contrast, in extant stents without a sinus portion, the
valve closes only passively because of backflow. The
direct apical approach to the right ventricle allows for
insertion of stented valves with a larger diameter than
is otherwise possible with the current percutaneous sys-
tems. Stent release with a hydraulic mechanism allows
for a very flexible and narrow shaft of the instrument.
The design permits easily following of the guide wire
to the desired position. The release mechanism can be
controlled with one hand, keeping the other free to
secure the position of the device during release. The
stented valves have been echocardiographically docu-
mented to function correctly up to 6 months, with his-
tological evidence of vascularization of the graft wall,
and endothelialization of the valve.
CONCLUSIONS
In an experimental sheep survival model, we have
demonstrated the feasibility and ease of insertion of a
new stented equine valve with a sinus portion, using a
new hydraulic device release system through a mini
right thoracotomy, on a beating heart. This approach
may become a complement to the percutaneous trans-
catheter one, either in much younger patients with
small vascular access, or on the contrary in very large
patients with much wider outflow tracts than the extant
percutaneous valves. With direct access to the right
outflow, problems pertaining to these two extremes in
patient vessel or outflow versus device mismatch
potentially allow a broader patient population to benefit
from this type of therapy. Insertion through a small
incision avoiding repeat sternotomy, as well of the fea-
sibility to insert the prosthesis without the use of car-
diopulmonary bypass make this a more attractive and
less invasive procedure. Mid to long-term functional
and histological results are required for further evalua-
tion of this new valve.
ACKNOWLEDGEMENTS
The authors thank Monika Hilbe, MD, Institute of
Veterinary Pathology, Vetsuisse Faculty Zurich,
Fig. 4. Histology of an explanted competent valve at 6
months, with pliable noncalcified leaflets (*), and an endothe-
lial layer (arrows).
Equine Stented Pulmonary Valve Insertion 657
Catheterization and Cardiovascular Interventions DOI 10.1002/ccd.
Published on behalf of The Society for Cardiovascular Angiography and Interventions (SCAI).](https://image.slidesharecdn.com/fe9b8b7f-8128-4787-b794-2d30281f90e5-161219233548/85/equine-valve-Gothenburg-Catheterization_and_Cardiovascular_Interventions-4-320.jpg)
