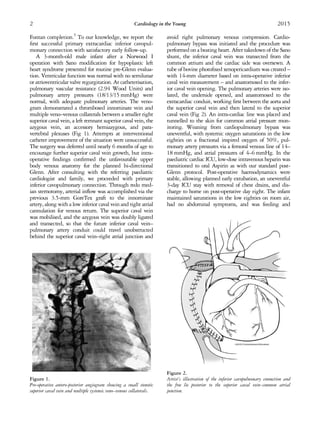
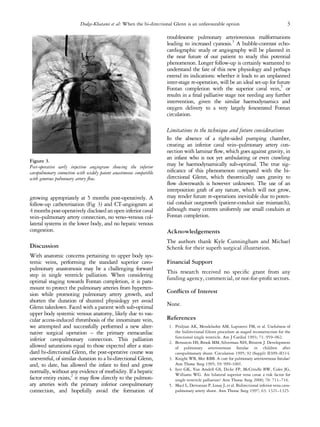
This document describes a case where a primary extracardiac inferior cavopulmonary connection was performed instead of a bi-directional Glenn procedure. The standard Glenn procedure was not possible due to stenosis and thrombosis of the superior caval vein and inadequate collateral veins. The alternative procedure involved connecting the inferior vena cava directly to the pulmonary arteries using an extracardiac conduit. The postoperative course was uneventful and follow-up showed the connection remained open without complications. This procedure avoided potential Glenn failure and provided an alternative palliation for patients where Glenn is not possible.