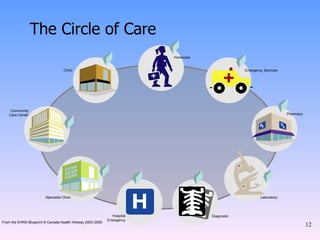
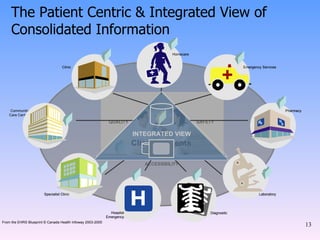
The document discusses the topic of e-health and its importance in the 21st century healthcare system. It provides definitions of e-health from different organizations and outlines some of the key benefits it provides, including improving efficiency, quality of care, and empowering patients. It also discusses challenges facing healthcare systems like an aging population and the role e-health can play in addressing issues like patient safety and independent living for those with chronic illnesses.

![Contact Details Cell Phone: 250-507-4343 Victoria , BC Canada [email_address] 15 years healthcare specialist experience and practice management consulting. Utilizing extensive industry experience within medical equipments, IT healthcare (PACS/RIS/CIS & CVIS), pharma, biotech, clinical research and healthcare to execute and implement certain process as well as methodology into diverse operational roles at all organizational levels.](https://image.slidesharecdn.com/presentation2010-12844544601718-phpapp02/85/e-health-2-320.jpg)