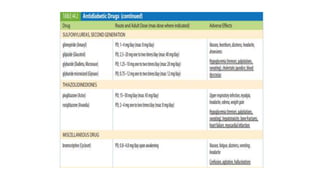
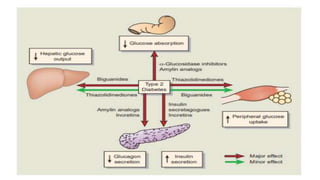
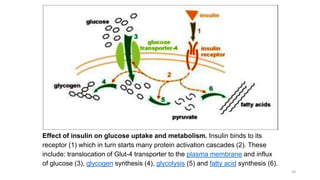
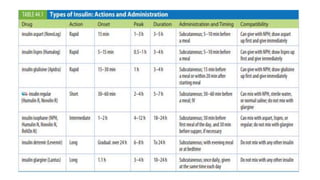
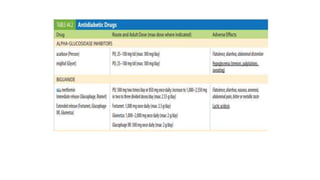
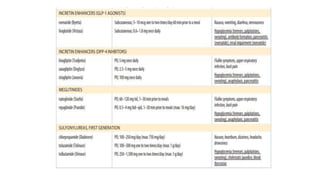
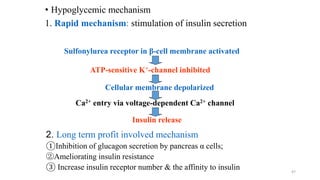
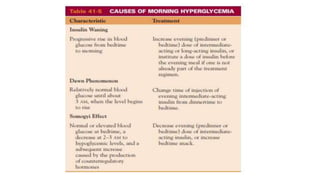
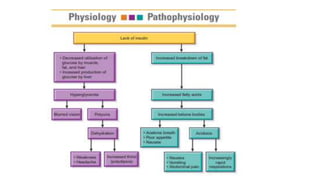
The document provides a comprehensive overview of diabetes mellitus, including its classification, pathophysiology, and management strategies. It discusses the two main types of diabetes, Type 1 and Type 2, highlighting their causes, clinical manifestations, and the importance of lifestyle and pharmacological interventions in management. Additionally, it covers diagnostic tests and the role of healthcare professionals in providing educational support and individualized care plans for patients.