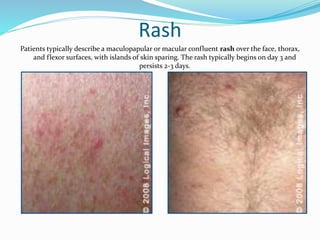
This document provides information on dengue fever, a mosquito-borne viral infection. It discusses the clinical presentation and pathophysiology of dengue fever and the more severe forms of dengue hemorrhagic fever and dengue shock syndrome. Key points include that dengue fever presents as an acute febrile illness and is caused by one of four related viruses. In rare cases it can progress to dengue hemorrhagic fever or dengue shock syndrome, characterized by bleeding and shock. Treatment involves supportive care and fluid replacement for dehydration.