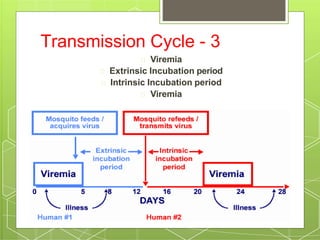
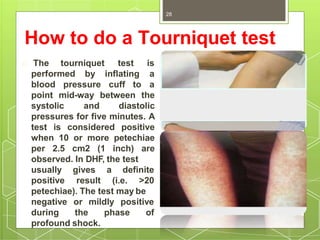
Dengue fever is caused by the dengue virus transmitted by Aedes mosquitoes. It causes flu-like symptoms including fever, headache, muscle and joint pains, and skin rash. In some cases it can develop into severe dengue hemorrhagic fever or dengue shock syndrome, which can be life-threatening. There is no vaccine, so prevention focuses on reducing mosquito habitats and exposure to bites. Treatment involves oral or intravenous rehydration depending on severity of symptoms.