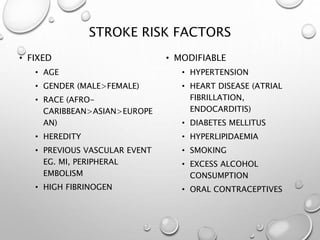
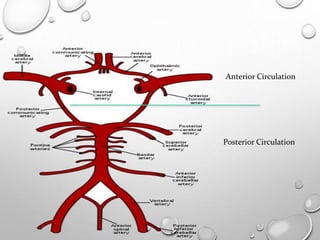
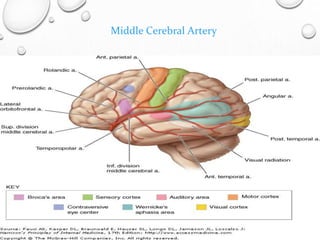
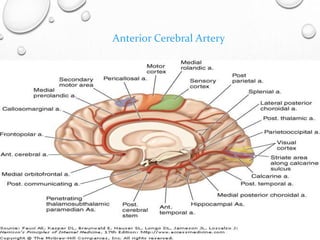
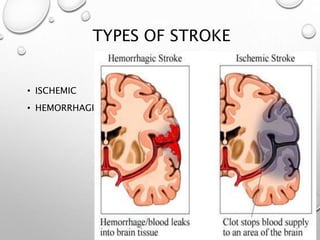
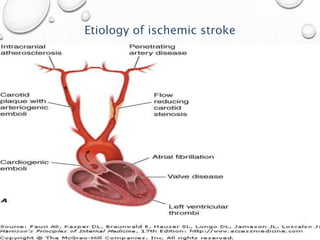
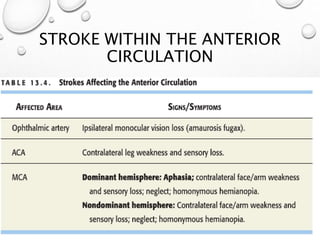
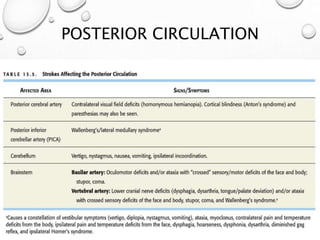
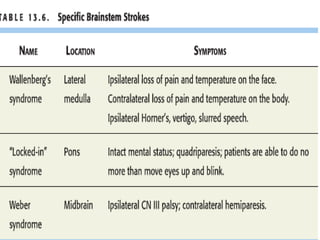
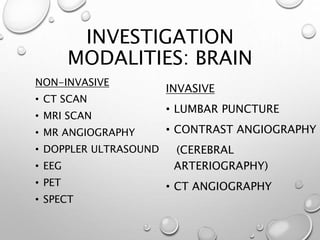
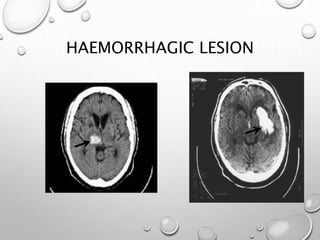
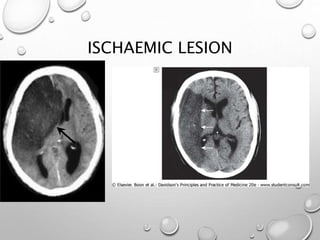
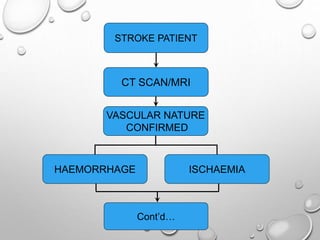
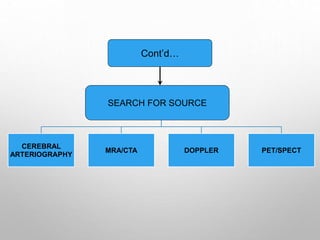
This document provides definitions and information about evaluating and managing patients presenting with stroke. It defines stroke, transient ischemic attack (TIA), and their subtypes. It discusses the epidemiology of stroke and risk factors. Evaluation of a stroke patient involves a neurological exam and considering differential diagnoses. Investigations aim to confirm the vascular nature and type of lesion. Management focuses on treating the underlying cause, preventing complications, and rehabilitation.