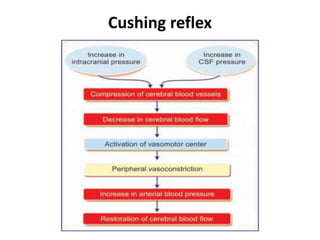
The document summarizes cerebral circulation. The brain receives blood from the carotid and basilar arteries, with normal blood flow being 750-800 mL per minute. Cerebral blood flow is regulated by autoregulation within a mean arterial pressure range of 60-140 mmHg, as well as chemical and neural factors. Autoregulation depends on effective perfusion pressure and cerebral vascular resistance, which can be impacted by intracranial pressure, blood viscosity, and carbon dioxide levels.