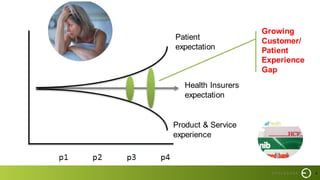
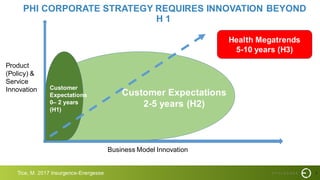
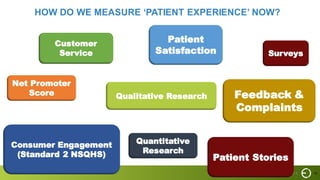
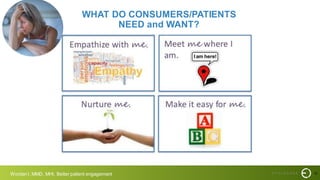
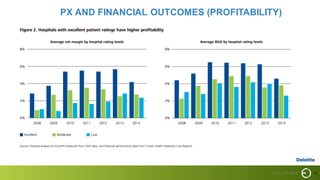
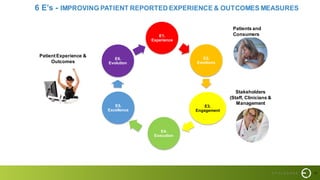
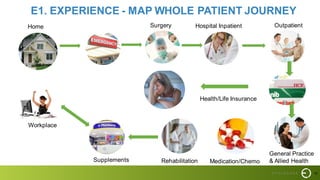
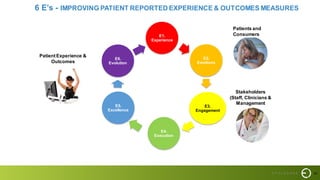
This document summarizes a presentation on improving patient experience. It discusses measuring patient experience through surveys, analyzing feedback to identify pain points, and translating insights into improvements. Key challenges include engaging staff, measuring experience across different settings, and demonstrating the benefits of improved experience such as better outcomes, safety, and cost savings. The presentation provides a framework of 6 E's to guide experience improvement efforts: capturing experiences, understanding emotions, engaging stakeholders, executing on insights, benchmarking excellence, and continuous evolution.