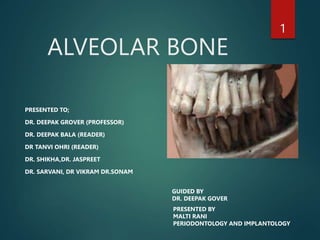
The alveolar bone is composed of the ridges of the jaw that support the teeth. The roots of the teeth are contained in deep depressions, the alveolar sockets in the bone. The alveolar bone develops around each tooth follicle during odontogenesis. It is composed primarily of hydroxyapatite and collagen. It contains an outer cortical plate, inner socket wall, cancellous trabeculae, interdental septum and alveolar crest. Osteoblasts and osteoclasts are the main cells involved in bone formation and resorption.