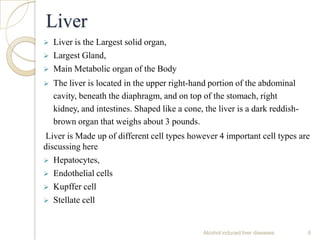
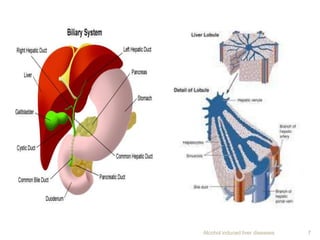
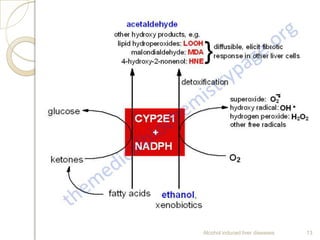
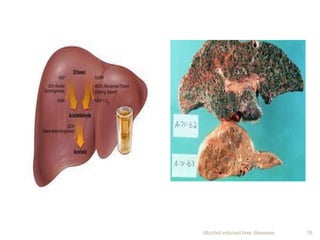
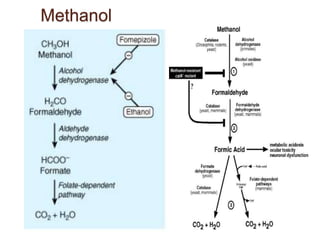
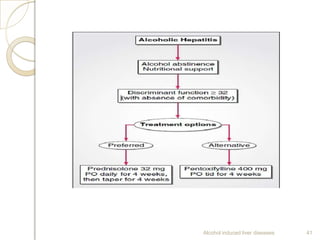
Alcohol consumption can lead to various liver diseases known as alcoholic liver disease (ALD). Chronic heavy drinking is responsible for 50% of chronic liver disease cases in India. Symptoms of ALD may not appear until the disease is advanced and include fatigue, abdominal swelling and pain, and jaundice. Alcohol is metabolized in the liver, producing reactive oxygen species that can cause oxidative stress, fatty liver, inflammation, fibrosis and eventually cirrhosis over many years. Diagnosis involves assessing drinking history, symptoms, lab tests and biopsy. Treatment focuses on abstaining from alcohol. Corticosteroids and antioxidants may help in some cases. Liver transplantation is an option for end-stage ALD but is not usually recommended for