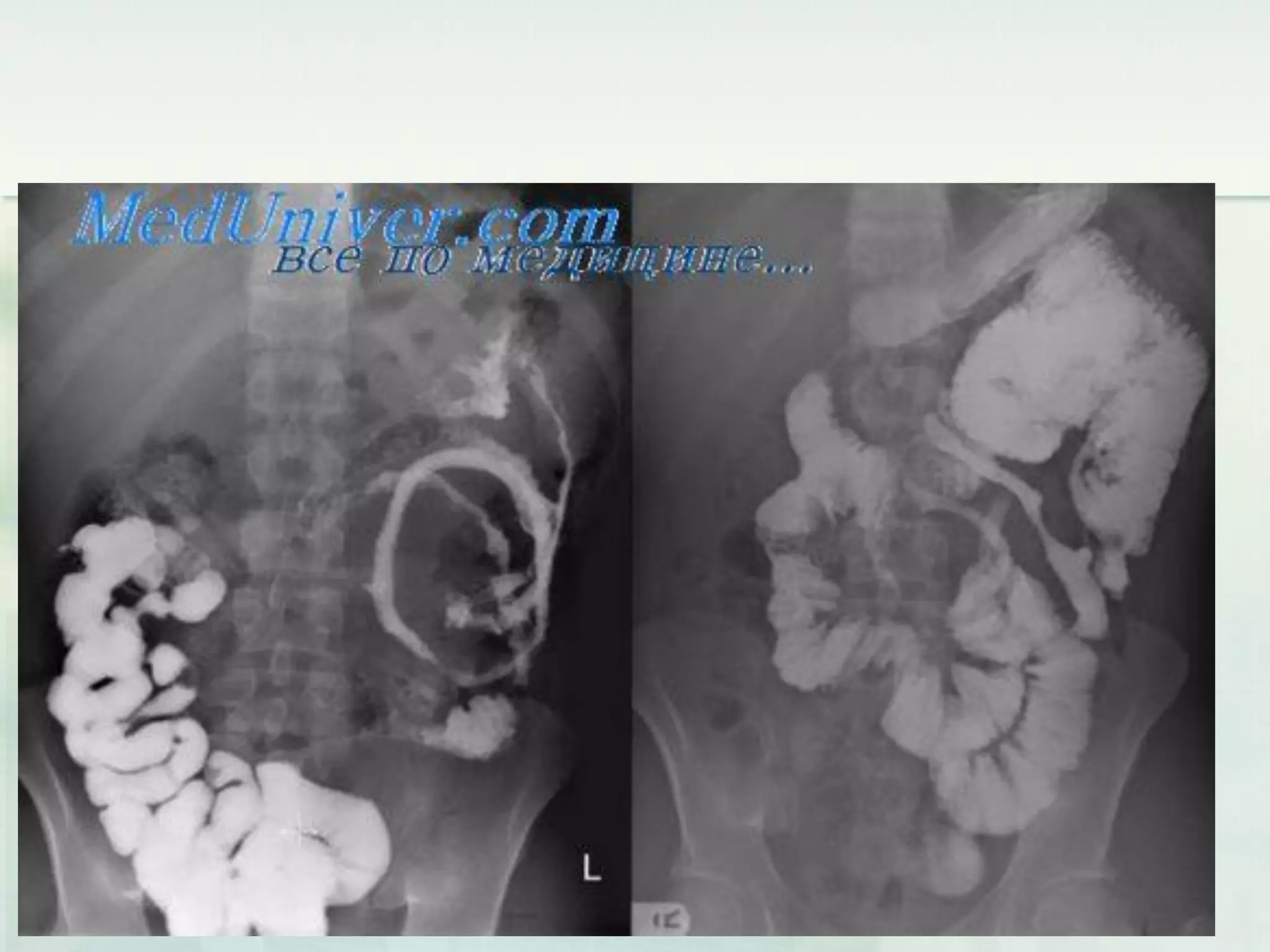
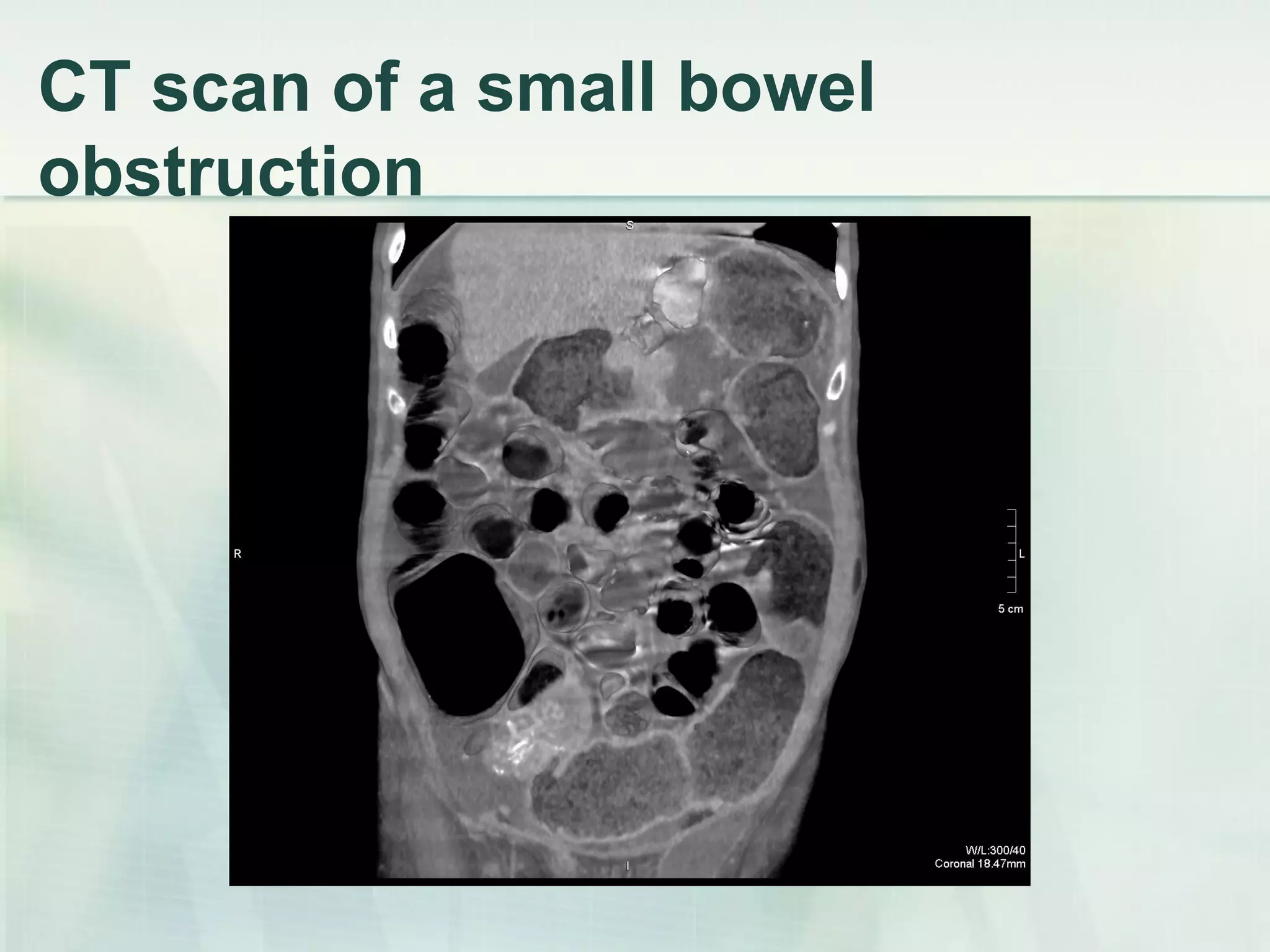
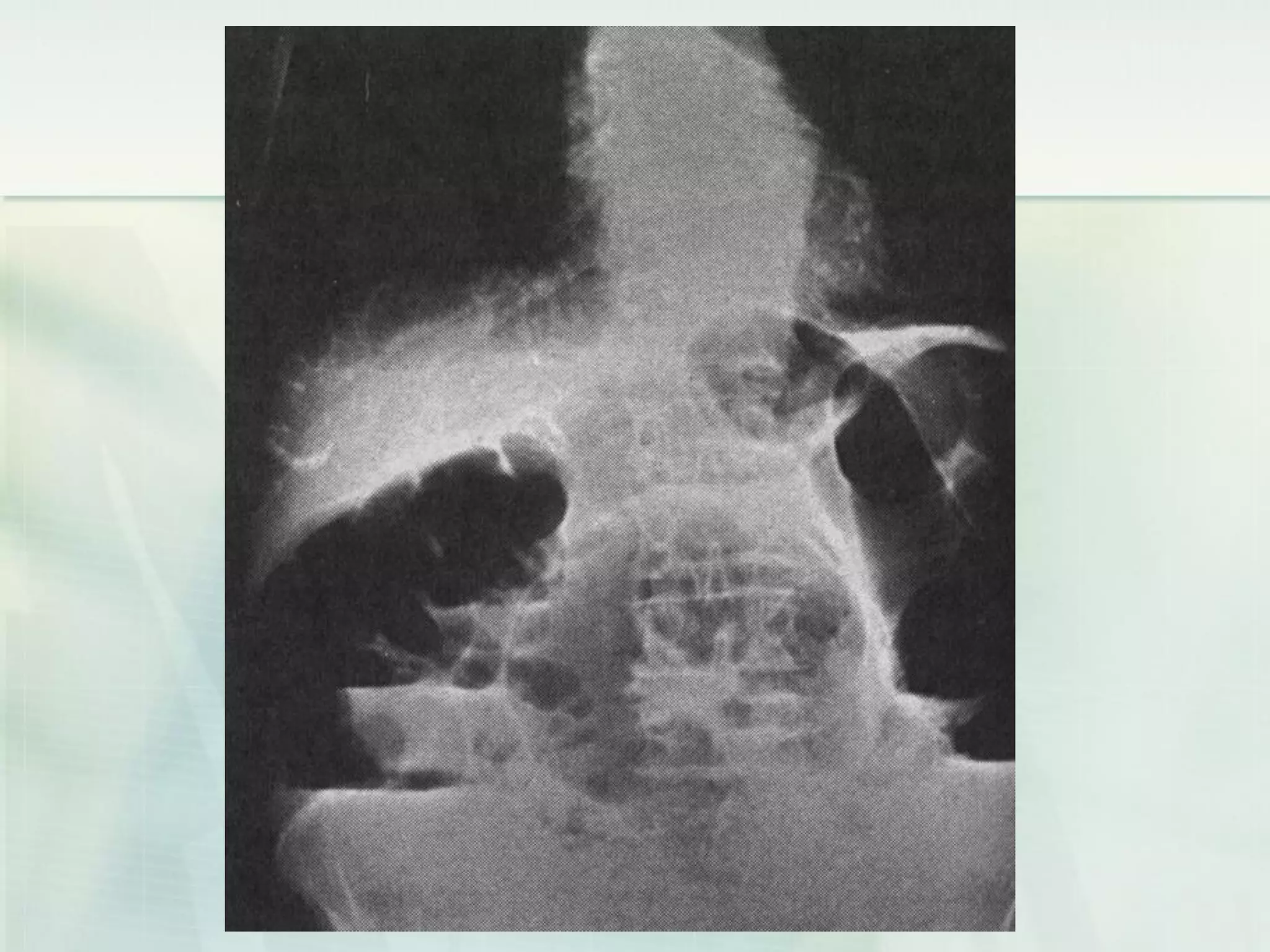
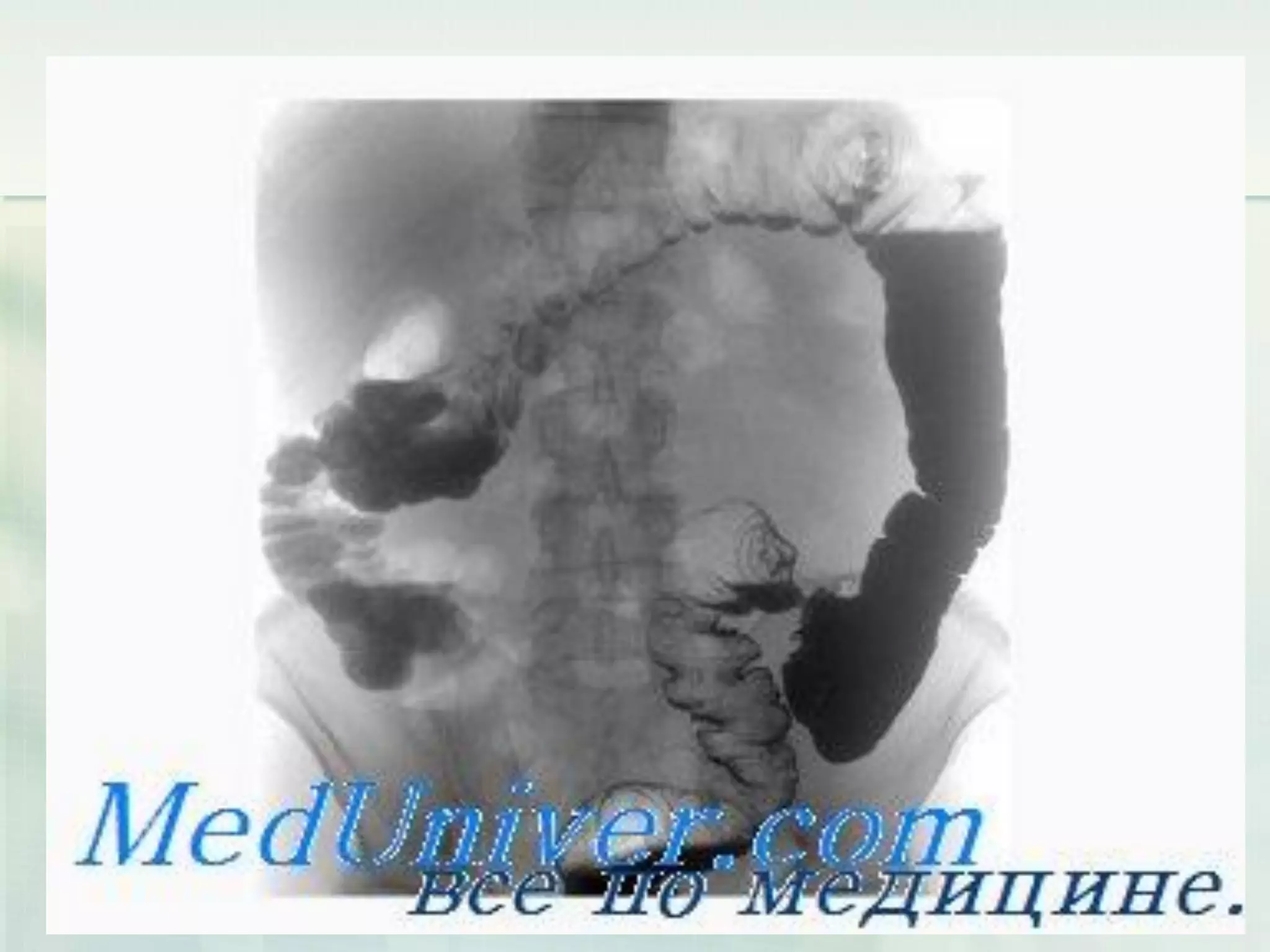
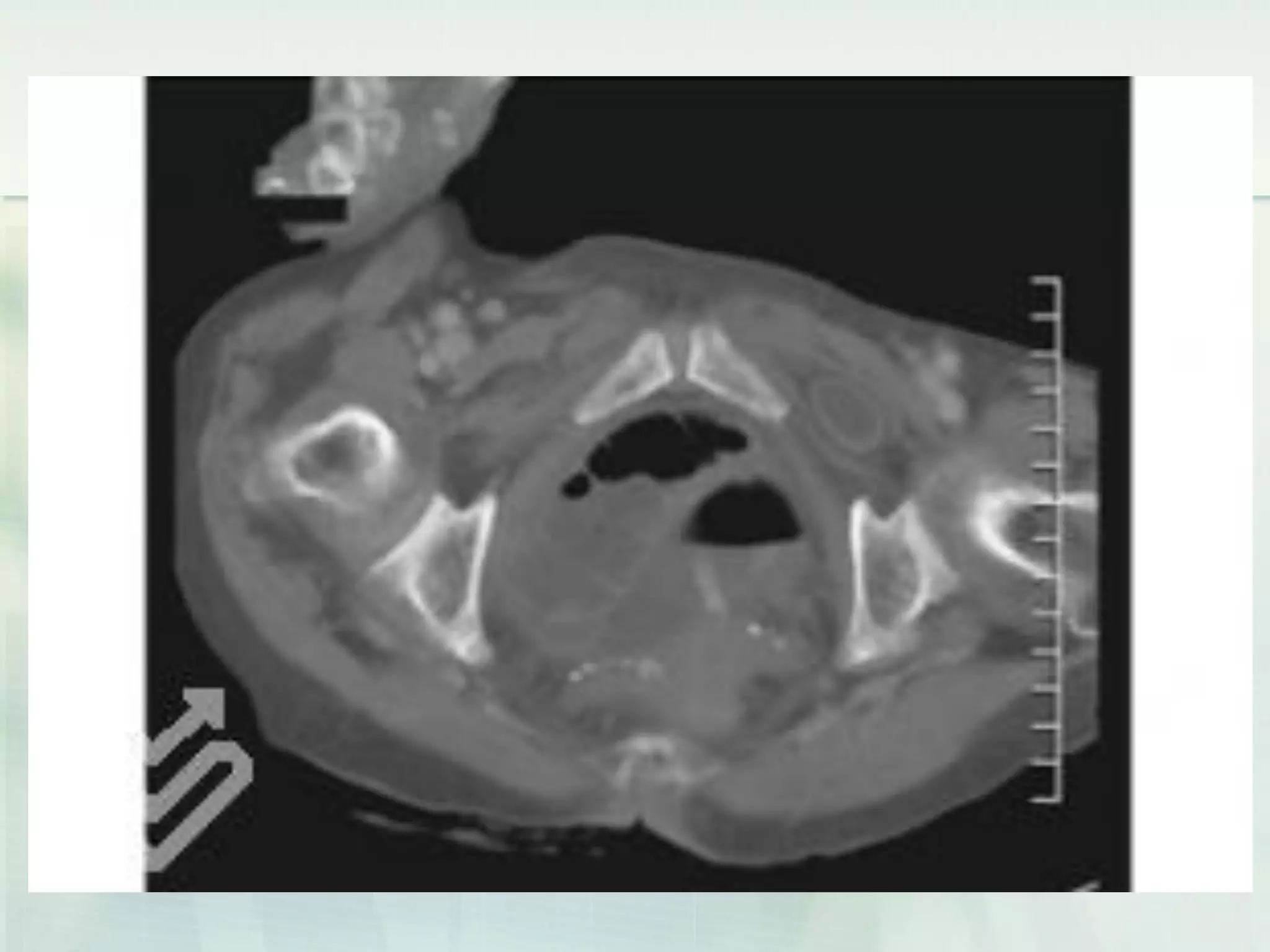
This document discusses acute intestinal obstruction, including classifications, causes, clinical features, investigations and treatments. It classifies obstruction based on origin, method of occurrence, blood flow and clinical course. Mechanical obstruction is distinguished from functional obstruction. Signs of small bowel obstruction include abdominal pain, nausea, vomiting and distention. Large bowel obstruction causes dull abdominal cramps and distention. Treatment involves decompression, fluid resuscitation, antibiotics and surgery to remove obstructions and non-viable bowel segments.