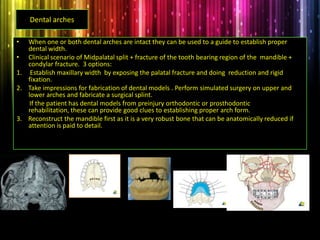
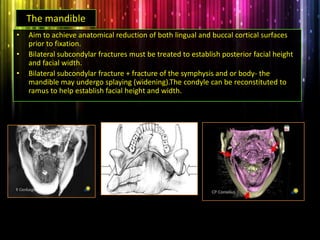
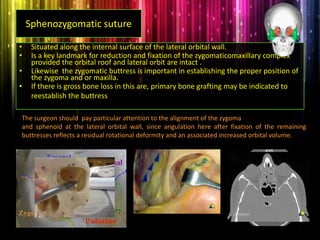
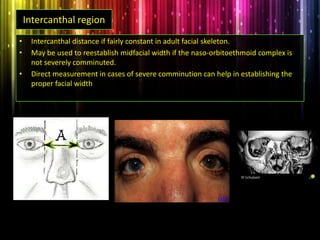
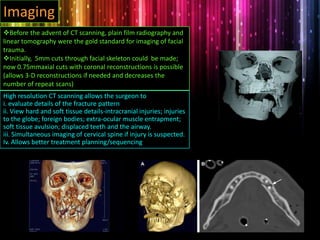
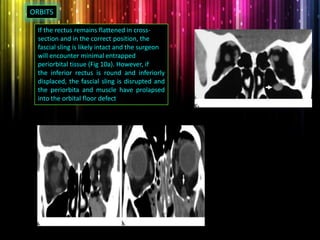
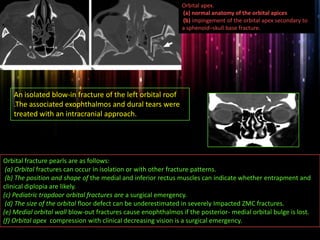
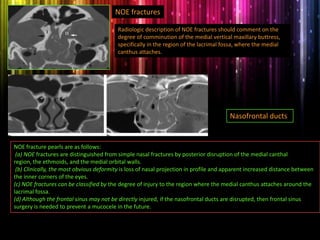
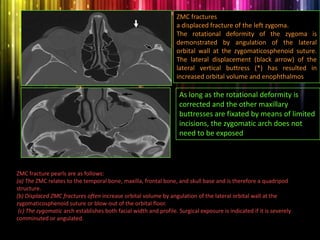
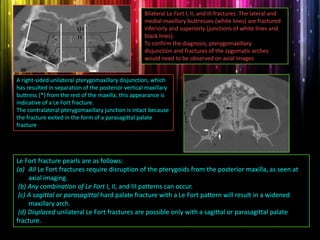
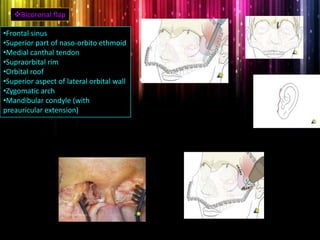
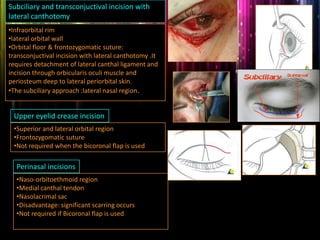
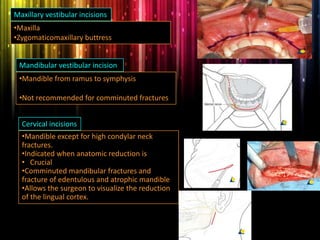
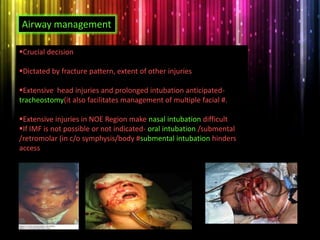
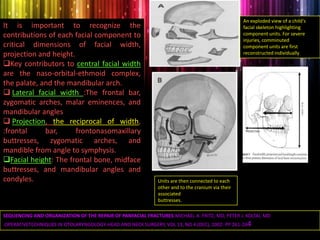
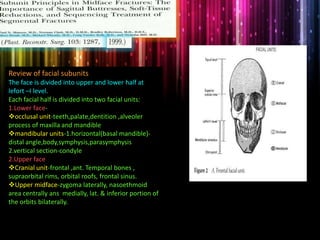
Panfacial fractures involve multiple facial bones, including the frontal bones, zygomaticomaxillary complex, naso-orbitoethmoid region, maxilla and mandible. Due to the complex nature of these injuries, management requires careful planning and sequencing of treatment to restore facial functions, features and symmetry. Key goals are to reestablish occlusion, stabilize major facial supports to restore three-dimensional contour, and provide a stable scaffold for soft tissue healing. Proper imaging, surgical approaches and attention to anatomical landmarks are important to achieve accurate reduction and fixation.