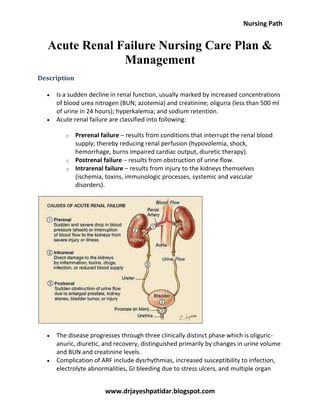
Acute renal failure nursing care plan & management
- 1. Nursing Path www.drjayeshpatidar.blogspot.com Acute Renal Failure Nursing Care Plan & Management Description Is a sudden decline in renal function, usually marked by increased concentrations of blood urea nitrogen (BUN; azotemia) and creatinine; oliguria (less than 500 ml of urine in 24 hours); hyperkalemia; and sodium retention. Acute renal failure are classified into following: o Prerenal failure – results from conditions that interrupt the renal blood supply; thereby reducing renal perfusion (hypovolemia, shock, hemorrhage, burns impaired cardiac output, diuretic therapy). o Postrenal failure – results from obstruction of urine flow. o Intrarenal failure – results from injury to the kidneys themselves (ischemia, toxins, immunologic processes, systemic and vascular disorders). The disease progresses through three clinically distinct phase which is oliguric- anuric, diuretic, and recovery, distinguished primarily by changes in urine volume and BUN and creatinine levels. Complication of ARF include dysrhythmias, increased susceptibility to infection, electrolyte abnormalities, GI bleeding due to stress ulcers, and multiple organ
- 2. Nursing Path www.drjayeshpatidar.blogspot.com failure. Untreated ARF can also progress to chronic renal failure, end-stage renal disease, and death from uremia or related causes. Pathophysiology
- 3. Nursing Path www.drjayeshpatidar.blogspot.com Assessment: 1. Oliguric-anuric phase: urine volume less than 400 ml per 24 hours; increased in serum creatinine, urea, uric acid, organic acids, potassium, and magnesium; lasts 3 to 5 days in infants and children, 10 to 14 days in adolescents and adults. 2. Diuretic phase: begins when urine output exceeds 500 ml per 24 hours, end when BUN and creatinine levels stop rising; length is availabe. 3. Recovery phase: asymptomatic; last several months to 1 year; some scar tissue may remain. 4. In prerenal disease: decreased tissue turgor, dryness of mucous membranes, weight loss, flat neck veins, hypotension, tachycardia. 5. In postrenal disease: difficulty in voiding, changes in urine flow. 6. In Intrarenal disease: presentation varies; usually have edema, may have fever, skin rash. 7. Nausea, vomiting, diarrhea, and lethargy may also occur. Diagnostic Evaluation: 1. Urinalysis shows proteinuria, hematuria, casts. Urine chemistry distinguishes various forms of ARF(prerenal, postrenal, intrarenal). 2. Serum creatinine and BUN levels are elevated; arterial blood gas (ABG) levels, serum electrolytes may be abnormal. 3. Renal ultrasonography estimates renal size and rules out treatable obstructive uropathy. Primary Nursing Diagnosis Fluid volume deficit related to excessive urinary output,vomiting,hemorrhage Other Diagnoses that may occur in Nursing Care Plans For Acute Renal Failure Ineffective tissue perfusion (renal) Excess fluid volume Risk for infection Therapeutic and Pharmacologic Interventions: 1. Surgical relief of obstruction may be necessary. 2. Correction of underlying fluid excesses or deficits. 3. Correction and control of biochemical imbalances.
- 4. Nursing Path www.drjayeshpatidar.blogspot.com 4. Restoration and maintenance of blood pressure through I.V. fluids and vasopressors. 5. Maintenance of adequate nutrition: Low protein diet with supplemental amino acids and vitamins. 6. Initiation of hemodialysis, peritoneal dialysis, or continuous renal replacement therapy for patients with progressive azotemia and other life-threatening complications. Nursing Interventions: 1. Monitor 24-hour urine volume to follow clinical course of the disease. 2. Monitor BUN, creatinine, and electrolyte. 3. Monitor ABG levels as necessary to evaluate acid-base balance. 4. Weigh the patient to provide an index of fluid balance. 5. Measure blood pressure at various times during the day with patients in supine, sitting, and standing positions. 6. Adjust fluid intake to avoid volume overload and dehydration. 7. Watch for cardiac dysrhythmias and heart failure from hyperkalemia, electrolyte imbalance, or fluid overload. Have resuscitation equipment available in case of cardiac arrest. 8. Watch for urinary tract infection, and remove bladder catheter as soon as possible. 9. Employ intensive pulmonary hygiene because incidence of pulmonary edema and infection is high. 10.Provide meticulous wound care. 11.Offer high-carbohydrate feedings because carbohydrates have a greater protein- sparing power and provide additional calories. 12.Institute seizure precautions. Provide padded side rails and have airway and suction equipment at the bedside. 13.Encourage and assist the patient to turn and move because drowsiness and lethargy may reduce activity. 14.Explain that the patient may experience residual defects in kidney function for a long time after acute illness. 15.Encourage the patient to report routine urinalysis and follow-up examinations. 16.Recommend resuming activity gradually because muscle weakness will be present from excessive catabolism.
- 5. Nursing Path www.drjayeshpatidar.blogspot.com Documentation Guidelines Physical findings:Urinary output and description of urine, fluid balance, vital signs, findings related to original disease process or insult,presence of pain or pruritus,mental status,GI status, and skin integrity Condition of peritoneal or vascular access sites Nutrition: Response to dietary or fluid restrictions, tolerance to food, maintenance of body weight Complications:Cardiovascular,integumentary infection Discharge and Home Healthcare Guidelines All patients with ARF need an understanding of renal function,signs and symptoms of renal failure ,and how to monitor their own renal function. Patients who have recovered viable renal function still need to be monitored by a nephrologist for at least a year. Teach the patient that she or he may be more susceptible to infection than previously. Advise daily weight checks. Emphasize rest to prevent overexertion. Teach the patient or significant others about all medications, including dosage, potential side effects, and drug interactions. Explain that the patient should tell the healthcare professional about the medications if the patient needs treatment such as dental work or if a new medication is added. Explain that ongoing medical assessment is required to check renal function. Explain all dietary and fluid restrictions. Note if the restrictions are life-long or temporary. Patients who have not recovered viable renal function need to understand that their condition may persist and even become chronic. If chronic renal failure is suspected, further outpatient treatment and monitoring are needed. Discuss with significant others the lifestyle changes that may be required with chronic renal failure.
