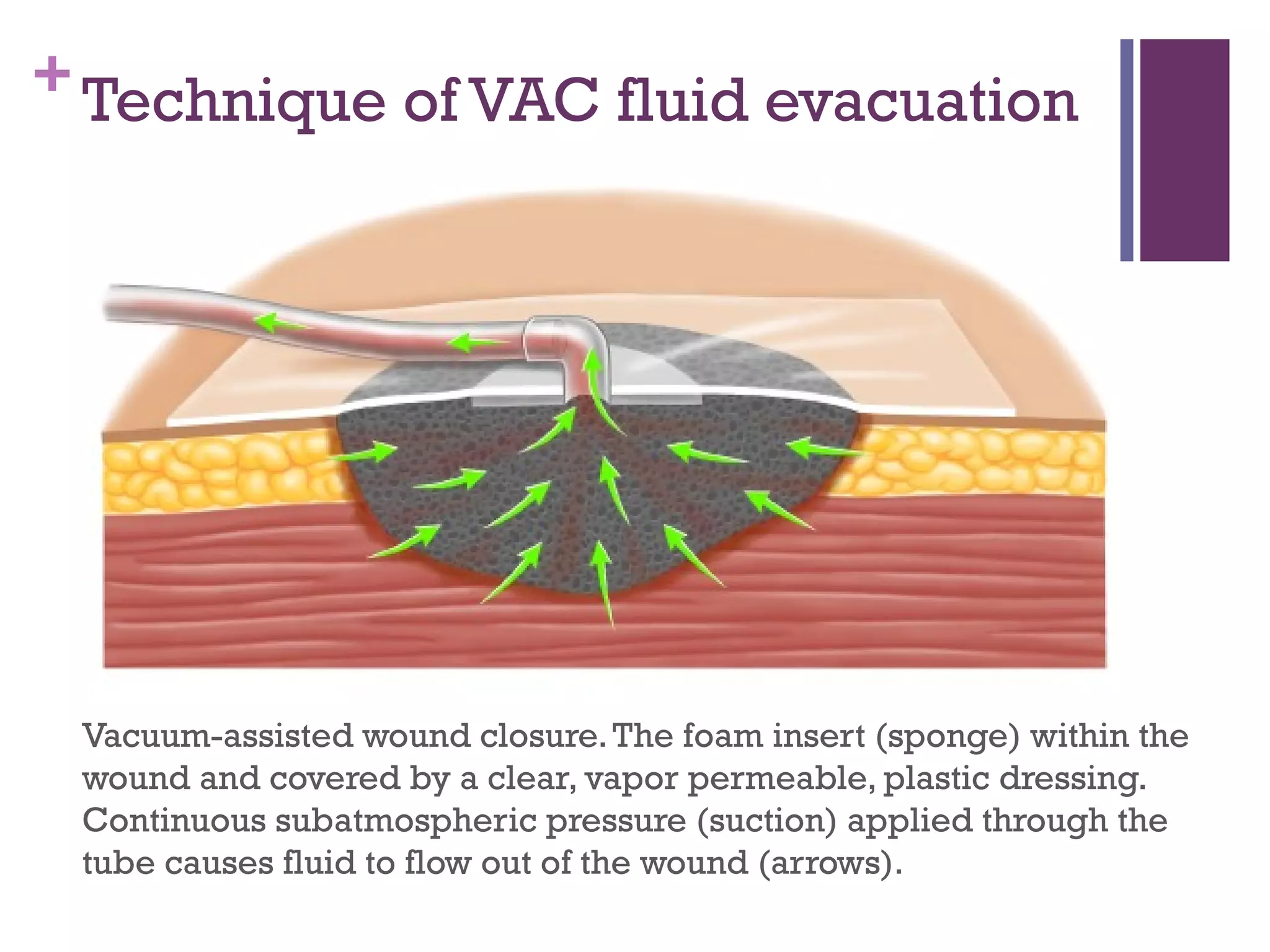
This document discusses pathophysiology of wound healing and factors affecting it. It begins with an introduction to wound classification and the normal phases of acute wound healing. It then discusses factors that can impair wound healing and cause chronic wounds, such as diabetes, peripheral artery disease, radiation therapy, malnutrition, and infection. Recent developments to expedite healing, such as negative pressure wound therapy, are also covered. NPWT applies subatmospheric pressure to a wound which increases blood flow and stimulates cellular processes to promote granulation tissue growth and accelerate wound closure.