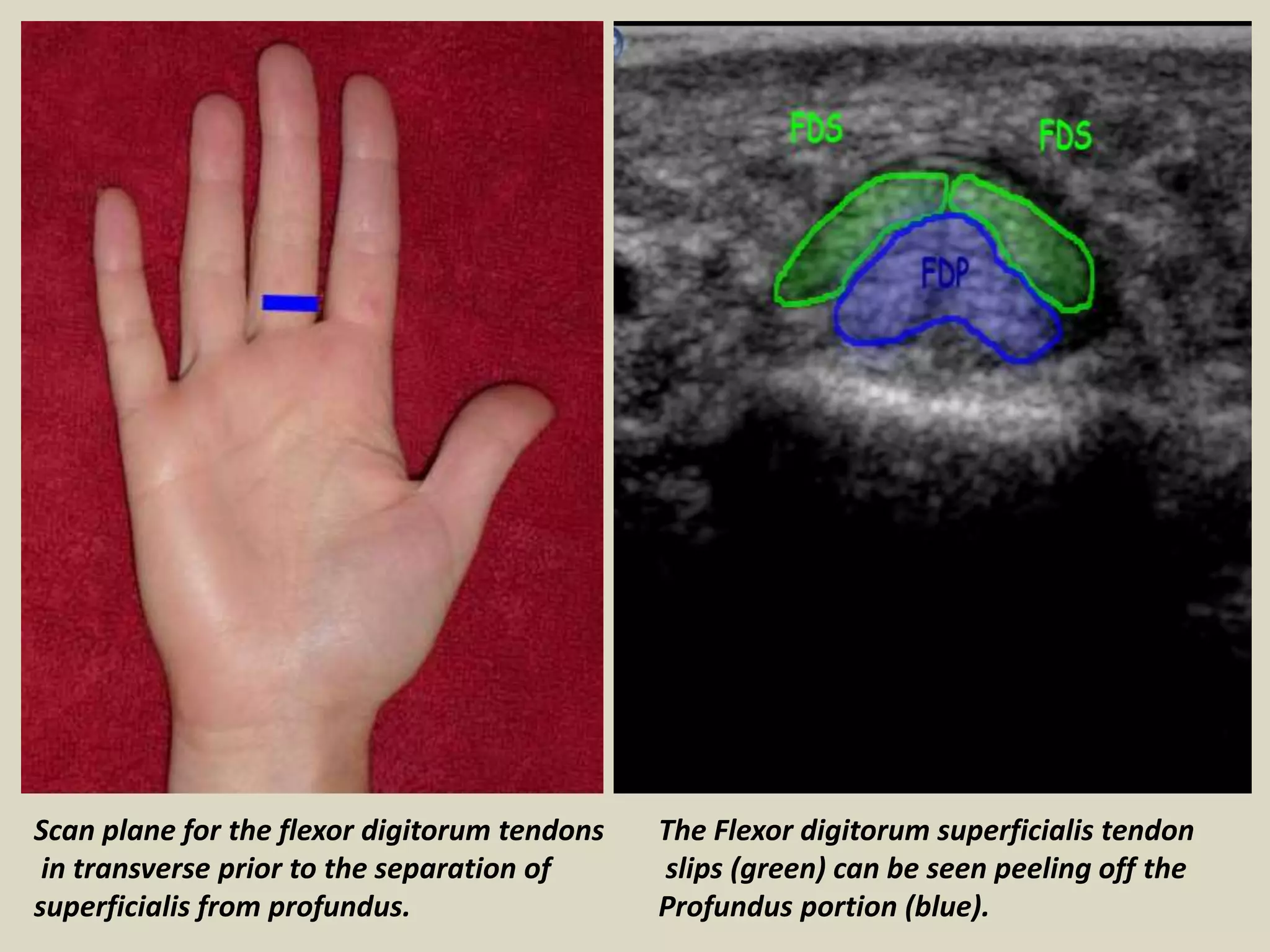
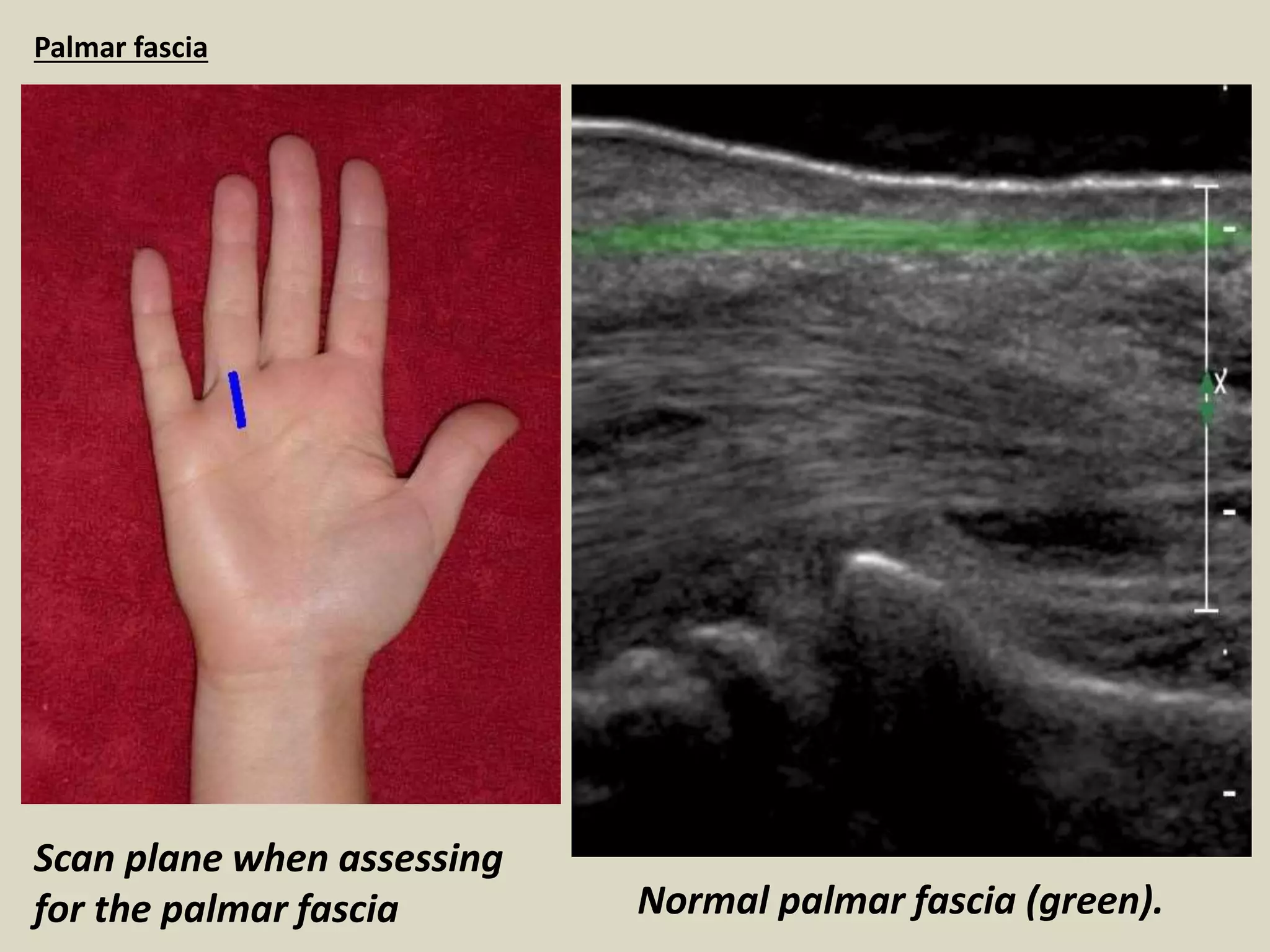
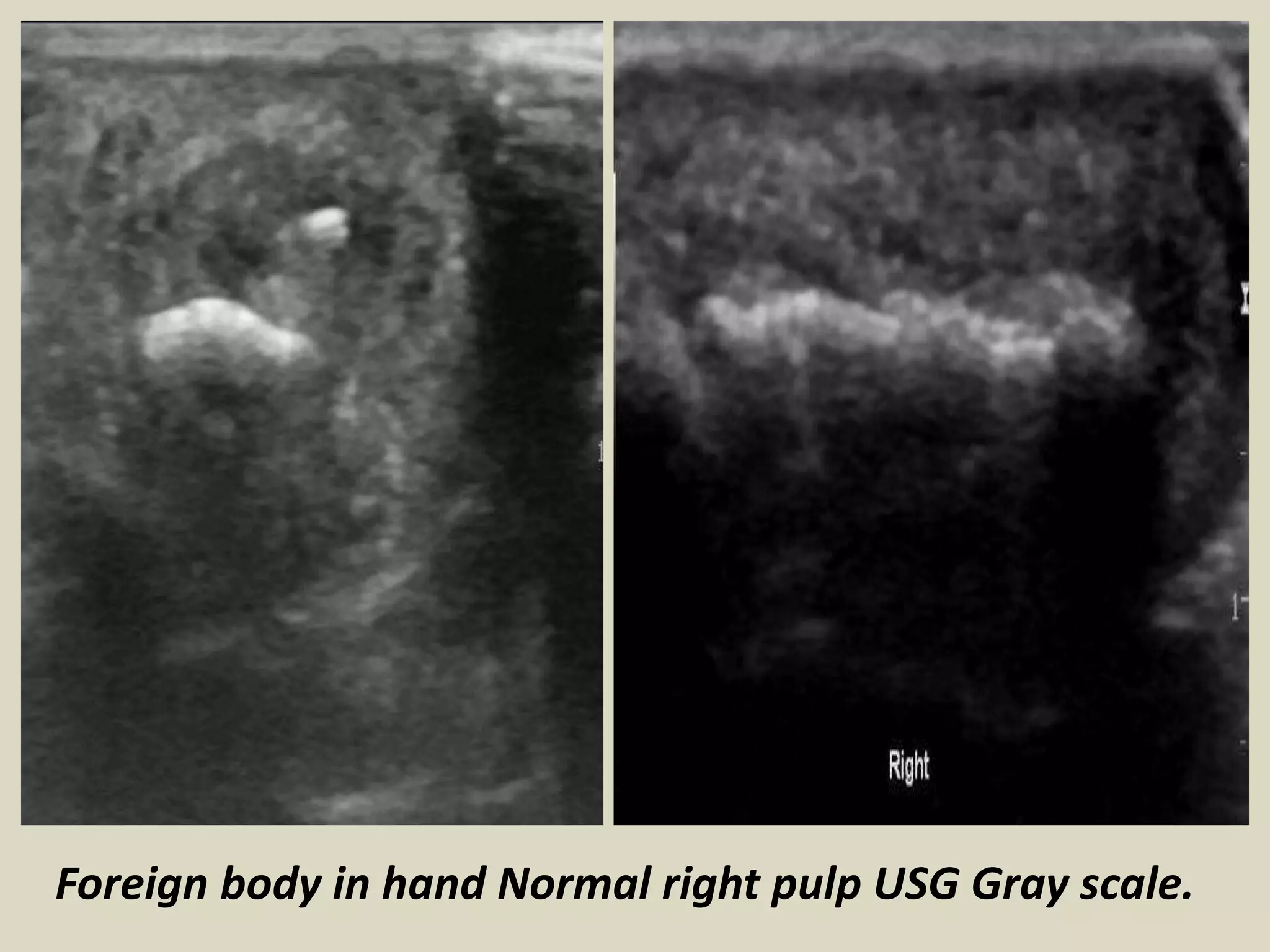
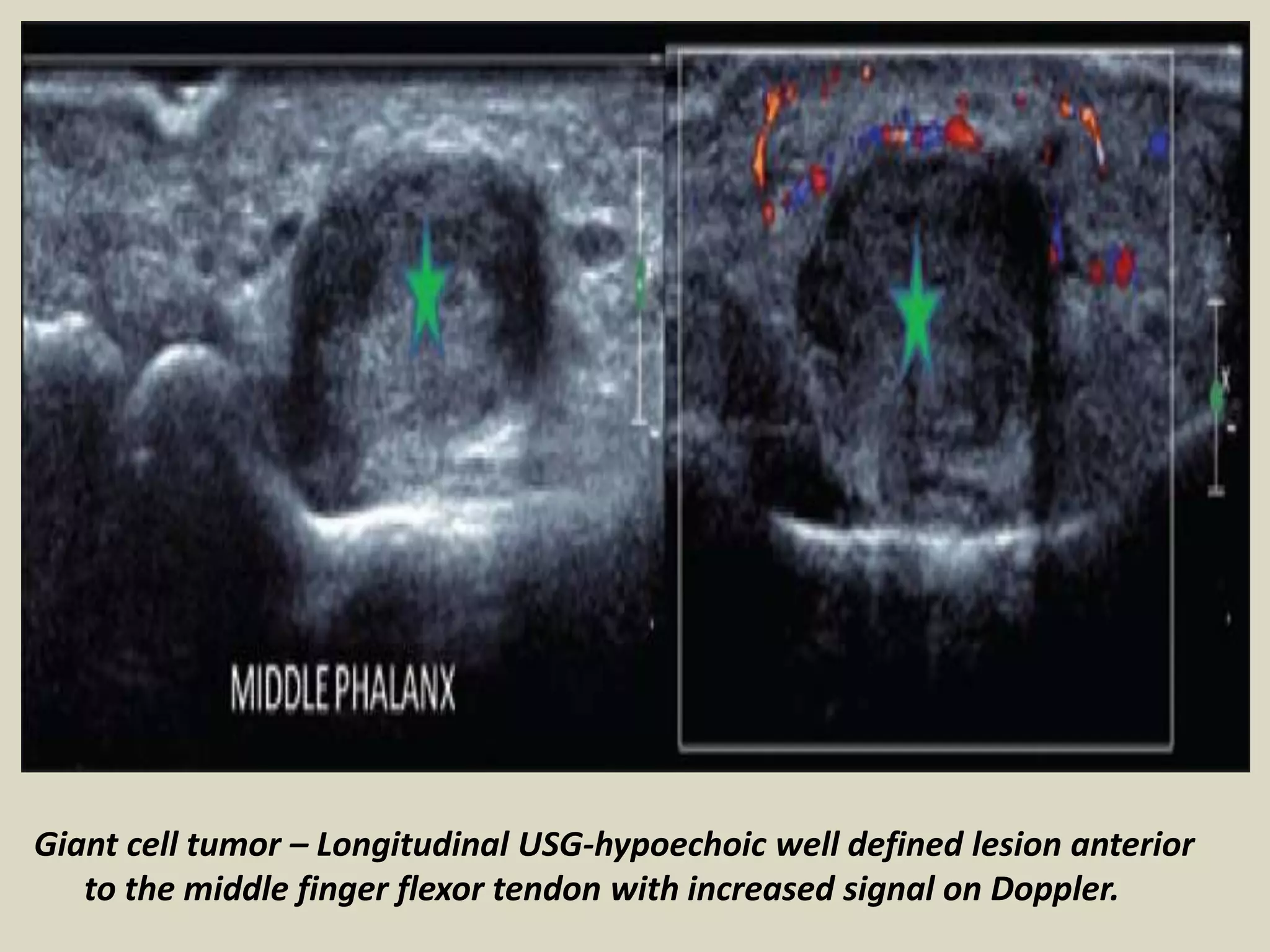
This document provides guidance on performing ultrasound examination of the hand and fingers. It describes optimal scanning techniques and positioning for visualizing key anatomical structures like flexor and extensor tendons, pulleys, ligaments and joints. Pathologies that can be identified include tendinosis, tenosynovitis, trigger finger, Dupuytren's contracture and inflammatory arthritis. Ultrasound allows accurate assessment of tendon integrity, fluid collections, synovitis and Doppler flow to evaluate degree of inflammation.