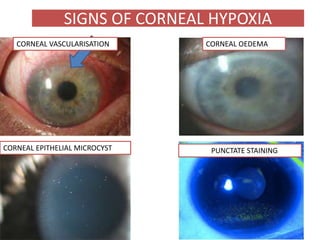
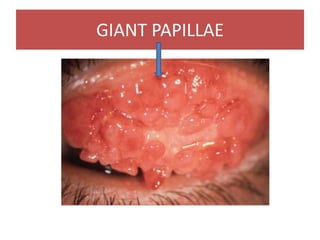
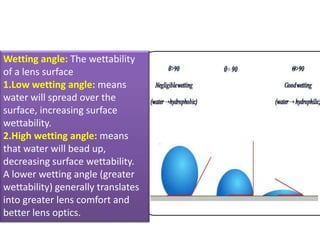
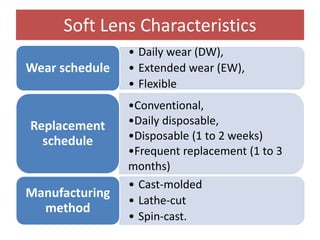
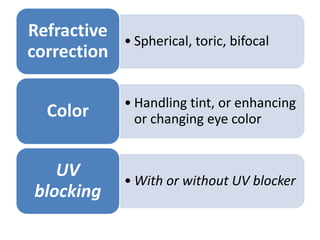
This document defines key terms related to contact lenses, including their materials and manufacturing processes. It discusses important optical considerations like the tear lens, correcting astigmatism, and presbyopia. Contact lens materials include PMMA, CAB, silicone acrylate, fluoropolymers, and HEMA hydrogels. Lenses are manufactured using processes like spin casting, lathe cutting, and cast molding. A thorough examination is required when fitting patients with contact lenses.

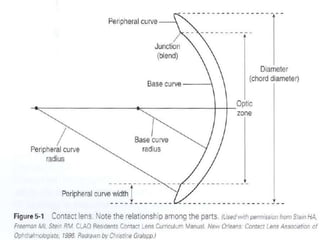


![• Diameter (chord diameter):The width of the
contact lens, which typically varies with the
lens material; the diameter of soft contact
lenses, for example. ranges from 13 to 15 mm,
whereas that of rigid gas-permeable (RGP)
lenses ranges from 9 to 10 mm.
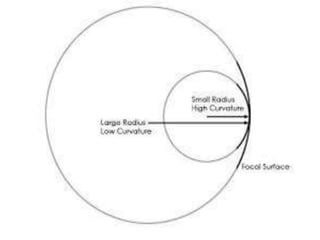
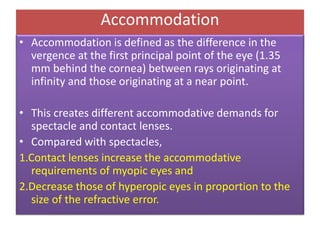
• Power: Determined by lens shape and
calculated indirectly by Snell's law: D ~ [n, -
nll/r]](https://image.slidesharecdn.com/contactlens-160518095922/85/Contact-lens-9-320.jpg)













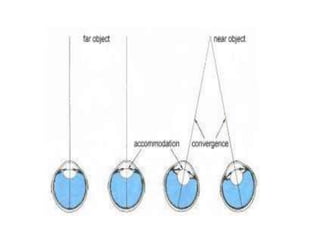




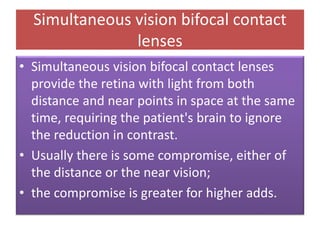
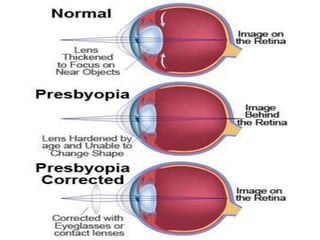
![Correcting presbyopia
• Correcting presbyopia with contact lenses can be done in
several different ways:
1.Reading glasses over contact lenses
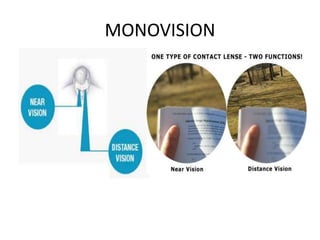
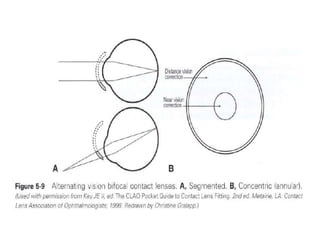
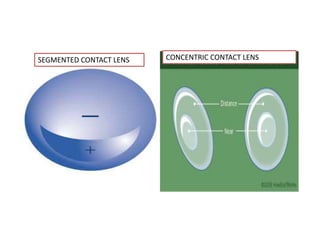
2.Alternating vision contact lenses (segmented or annular)
3.Simultaneous vision contact lenses (aspheric [multi focal] or
diffractive)
4.Monovision
5.Modified monovision
• From an optical point of view, using reading glasses or
alternating vision contact lenses is most like standard
spectacle correction for presbyopia.](https://image.slidesharecdn.com/contactlens-160518095922/85/Contact-lens-38-320.jpg)



























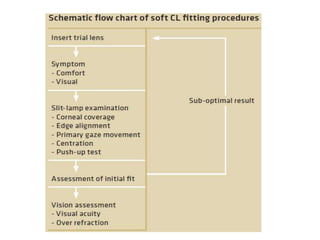








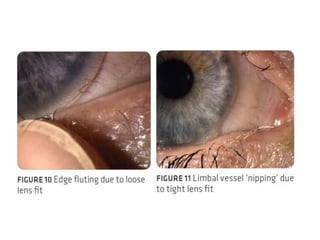

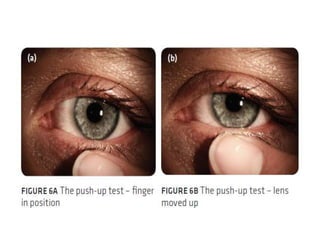


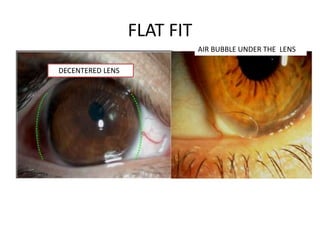





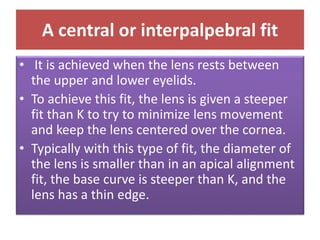




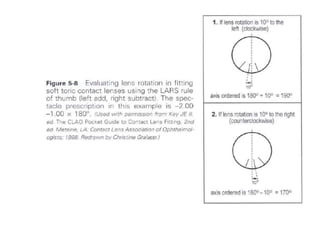
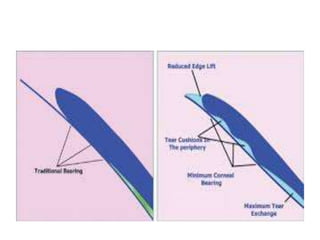
![• Lens position in the alignment fitting should be such
that the lens rides high, with the upper one-third or so
of the contact lens under the upper eyelid.
• With each blink, the lens should move as the eyelid
moves.
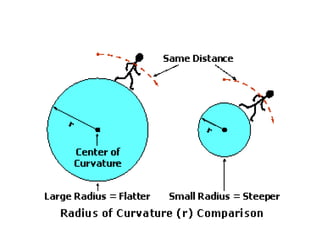
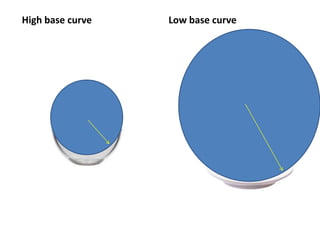
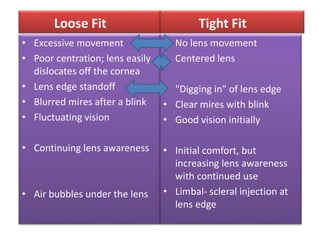
• Insufficient movement means the lens is too tight, so
the base curve should be flattened (larger number [in
millimeters]) or the diameter made smaller.
• Excessive movement means the lens is too loose, so
the base curve should be steepened (smaller number
[in millimeters]) or the lens diameter made larger.](https://image.slidesharecdn.com/contactlens-160518095922/85/Contact-lens-99-320.jpg)