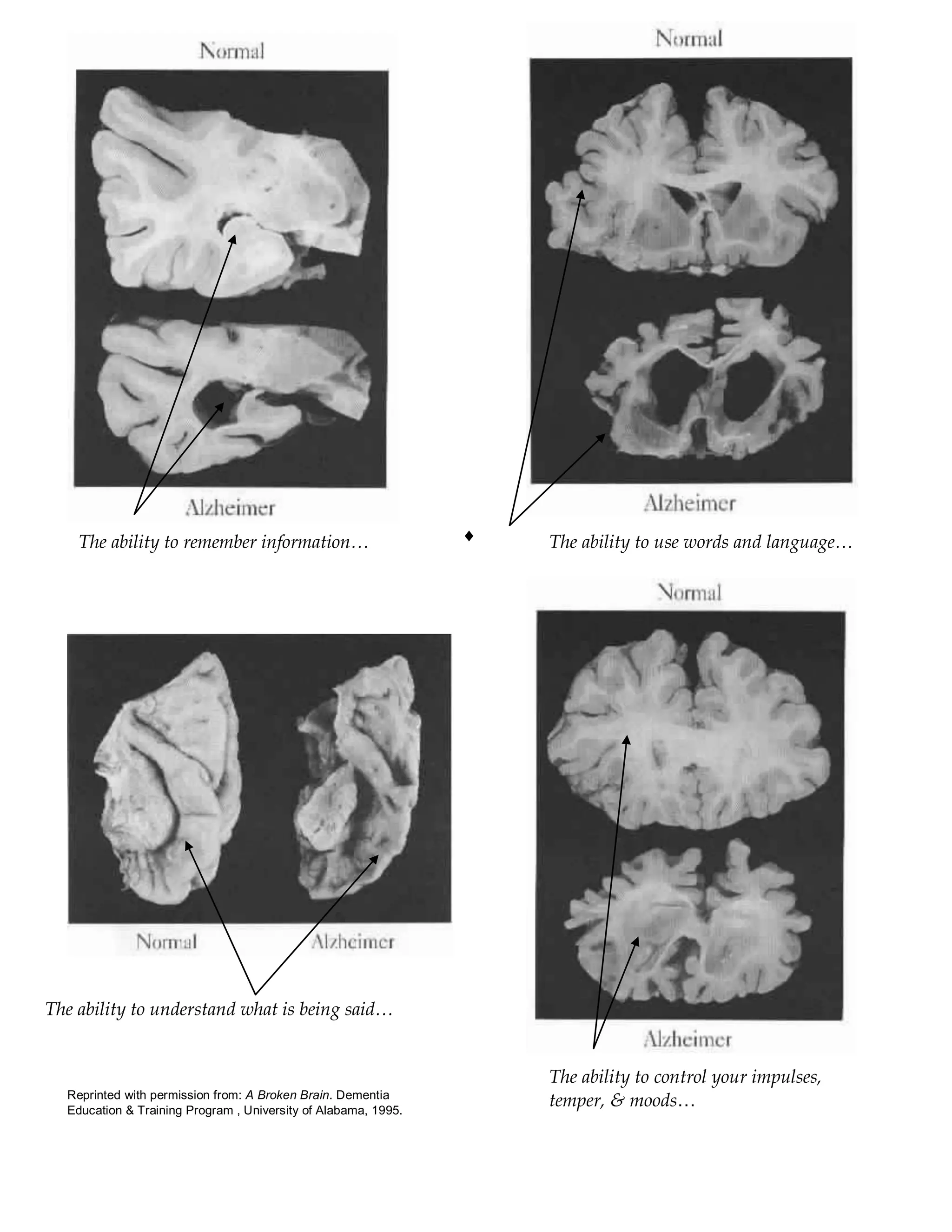
This document explains dementia as a serious disease that impairs cognitive functions and impacts daily living, detailing various types such as Alzheimer's, vascular dementia, and lewy body dementia. It outlines common symptoms, drug treatments, and emphasizes the importance of supportive interactions with individuals affected by dementia, highlighting approaches for effective communication and care. The document also provides strategies to meet the physical and emotional needs of those with dementia while fostering a positive environment for their care.