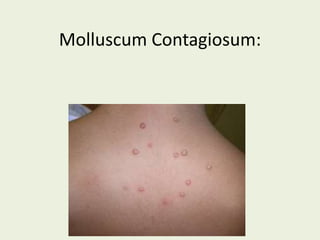
Molluscum contagiosum Made Extremely Simple
- 2. Introduction: • Molluscum contagiosum virus is classified within the poxvirus family in a specific genus, the Molluscipox • Molluscum contagiosum virus causes a benign viral infection characterized by single or multiple, rounded, dome-shaped, pink, waxy papules that are 2-5 mm in diameter. The papules are umbilicated and contain a caseous plug.
- 3. Epidemiology: Incidence and prevalence • Occurs commonly in childhood. • Estimated prevalence of 5–11% • Viral DNA can be detected on the normal skin of people with molluscum and from objects in their environment • Infection follows contact with infected persons or contaminated objects. • In young adults sexual transmission causes lesions that are more common in the genital area. • It is not known if epidermal injury is important for establishment of infection.
- 4. Age: • The disease is rare under the age of 1 year, due to maternally transmitted immunity and a long incubation period. • Vertical transmission responsible for lesions detected in the first few days or weeks of life. • Peak incidence: is between 2 and 5 years
- 5. Pathophysiology: Predisposing factors • Sexual abuse in children if accompanied by other suspicious features of abuse. • Atopic eczema • Topical steroids and topical calcineurin inhibitors have been suspected as contributing factors in eczema and other patients. • Unusually widespread lesions in patients with immune compromise, such as: – HIV disease – Haematological malignancy – Sarcoidosis – Idiopathic CD4 lymphocytopaenia – Hyper‐IgE syndrome – DOCK8 deficiency – Those receiving immunosuppressive therapy • Cell‐mediated immunity is significant in controlling and eliminating the infection.
- 6. Causative organisms: • Molluscum contagiosum virus is classified within the poxvirus family in a specific genus, the Molluscipox • It cannot be grown in tissue culture or eggs. • Following types exist: – MCV‐1: commonest type (76-95% of the cases) – MCV‐2: seen in adults and HIV patients – MCV‐3 – MCV‐4 Rarer subtypes
- 7. Pathology: • The virus enters the basal epidermis causing an increase in cell division extending into the suprabasal layer. • The cellular proliferation produces lobulated epidermal growths which compress the papillae until they appear as fibrous septa between the lobules, which are pear shaped with the apex upwards. • Basal layer remains intact. • Cells at the core of the lesion show the greatest distortion and are ultimately destroyed, and appear as large hyaline bodies (Molluscum bodies/ Henderson-Patterson Bodies) containing cytoplasmic masses of virus material. • Inflammatory changes in the dermis are absent or slight. • Lesions of long duration: may exhibit chronic granulomatous infiltrate due to the discharge into the dermis of the contents of a papule . • In spontaneous regression: the lesions are surrounded by an infiltrate of interferon‐producing plasmacytoid dendritic cells.
- 8. Lobular Epidermal growths Molluscum Bodies Compressed dermis Basement Membrane Intact Histopathology of Molluscum Contagiosum:
- 10. Clinical features: • Incubation period: 14 days to 6 months. • The individual lesion is a shiny, pearly white, hemispherical, umbilicated papule which may show a central pore • Size ranges from 1mm enlarging to 5-10mm in 6-12 weeks. • Rarely a lesion may become considerably larger if solitary. • Agminate form/ Giant Molluscum: are plaques composed of many small lesions. • After trauma, or spontaneously after several months, inflammatory changes result in suppuration, crusting and eventual destruction of the lesion.
- 12. Clinical variants: Distribution of the lesions depends on: the mode of infection, the type of clothing worn, and the climate. • In temperate regions: lesions commonly seen on the neck or on the trunk, particularly around the axillae. • In the tropics: lesions are more common on the limbs. • In teenagers and young adults: lesions in the ano‐genital area are most common due to sexual transmission. • In otherwise healthy subjects: facial lesions are seen, particularly on the eyelids, scalp, and any part of the body. • Soles may display an atypical form. • In immunosuppressed patients following patterns are seen: – Widespread and refractory mollusca on the face are seen in HIV disease – Oral lesions on the lips, tongue or buccal mucous membranes – Giant or widespread molluscum contagiosum lesions. • Molluscum can occur in scars and in tattoos • Follicular molluscum contagiosum has been reported, producing atypical, less protuberant pale papules .
- 13. Molluscum Contagiosum In AIDS Patients:
- 15. Differential diagnosis: • Solitary molluscum may resemble: – Pyogenic granuloma, – Keratoacanthoma – Squamous cell carcinoma • Multiple small lesions may resemble – Plane warts. • In HIV disease, molluscum contagiosum may resemble cutaneous cryptococcosis .
- 16. Complications and co‐morbidities: • In at least 10% of cases, particularly in atopic subjects, a patchy eczema, often very irritable, develops around one or more of the lesions a month or more after their onset. • Erythema annulare centrifugum • Erythema multiforme. • Chronic conjunctivitis and superficial punctate keratitis may complicate lesions on or near the eyelids. These complications resolve spontaneously after removal of the lesion.
- 17. Disease course and prognosis: • Most cases are self‐limiting within 6–9 months. • Some may persist for 3 or 4 years. • Inflammatory responses around lesions indicate that immunological resolution is likely to occur within a few months. • Depressed scars or anetoderma‐like lesions can remain when mollusca clear.
- 18. Investigations: • Clinical diagnosis: when multiple lesions at different stages of evolution are present and the typical umbilicated papule is evident. • The diagnosis can be confirmed by direct microscopy or electron microscopy of the papule contents, by histopathology or by molecular analysis.
- 19. Management: • In many instances, therapy is not necessary as natural resolution can occur. • The risk of dissemination can be minimized by reducing scratching. • Associated dry skin or eczema should be treated with emollients and a weak topical steroid. • Transmitting the infection to other individuals may be reduced by: – Avoidance of shared towels, – Avoiding contact sports and – Abstaining from using communal baths. • Treatment is indicated when: – Spontaneous clearance is slow, – Lesions are symptomatic, or – Associated eczema is troublesome • The choice of treatment depend on: – Age of the patient, – Number of the lesion and – Position of the lesions. • Aim of the treatment: – Is to destroy the infected epidermal cells, – Stimulate an immunological response – Act directly against the virus.
- 21. First line: • Topical agents: used to produce mild to moderate inflammation and therefore stimulate the development of an immune response against the virus: (a) Caustics: – Cantharidin, – Trichloroacetic acid – Diluted liquefied phenol (b) Irritants: – Topical salicylic acid – Tretinoin – Adapalene – Nitric oxide cream – 5–10% potassium hydroxide solution – Benzoyl peroxide cream – Lemon myrtle oil – Tea tree oil • Damage to the lesions by squeezing the contents or insertion of a pointed cocktail stick may stimulate inflammation and clearance. • Immunologicals: with the aim of enhancing the immune response include: – topical diphencyprone – Imiquimod cream – Intralesional or systemic interferon – Systemic cimetidine – Intralesional immunotherapy Are strong irritants which can cause pain, blistering and scarring but with careful application and appropriate dilution can increase lesion clearance Lead to an irritant reaction but if the strength of preparation and the frequency of application is adjusted, resolution occurs.
- 22. Second line: • Cryotherapy: – Effective and commonly used in older children and adults – Needs to be repeated at 3–4 weekly intervals. • Carbon dioxide or Pulsed dye lasers: – useful but can cause scars • Photodynamic therapy • Curretage: – Can cause scarring. – Clearance rate reduced if there are many lesions – Children will usually need prior application of topical anaesthetic cream with strict observance of the maximum safe dose.
- 23. Third line: • Cidofovir: – This antiviral agent has been shown to effectively resolve molluscum lesions – Used either intravenously or topically as a 1–3% cream or ointment. – Should be considered for treating extensive lesions in, for example, immuno‐incompetent patients where standard treatment regimens have been unsuccessful. • Intravenous paclitaxel: – For severe disease in immunocompromised.
- 25. Future Topics: Bacterial exanthems. Also check previously discussed topics: • Human Papilloma virus and anogenital warts • Epidermodysplasia Verruciformis • Viral Exanthems: – Mealses – Rubella – Infectious mononucleous – Roseola Infantum – Erythema Infectiousum – Cytomegalovirus.