Cancer of oral cavity- Easy explanation for Nurses-
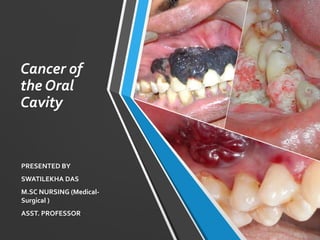
- 1. Cancer of the Oral Cavity PRESENTED BY SWATILEKHA DAS M.SC NURSING (Medical- Surgical ) ASST. PROFESSOR
- 2. Cancer of the Oral Cavity and Pharynx Cancer of the oral cavity and pharynx can occur in any part of the mouth (lips, lateral tongue, floor of mouth most common) or throat and is highly curable if discovered early.
- 3. Risk factors Cigarette, cigar, and pipe smoking use of smokeless tobacco excessive use of alcohol Oral cancers are often associated with the combined use of alcohol and tobacco. Other factors include gender (male), age (older than 50 years) African American descent Malignancies of the oral cavity are usually squamous cell cancers.
- 4. Clinical Manifestations • Few or no symptoms; most commonly a painless sore or mass that will not heal. • Typical lesion is a painful indurated ulcer with raised edges. • As the cancer progresses, patient may complain of tender-ness; difficulty in chewing, swallowing, or speaking; coughing of blood-tinged sputum; or enlarged cervical lymph nodes.
- 5. Assessment and Diagnostic Methods Oral examination, assessment of cervical lymph nodes, and biopsies of suspicious lesions (not healed within 2 weeks)
- 6. Medical Management • Management varies with the nature of the lesion, preference of the physician, and patient choice. Resectional surgery radiation therapy, chemotherapy, or a combination may be effective. • Lip cancer: Small lesions are excised liberally; larger lesions may be treated by radiation therapy.
- 7. • Tongue cancer:Treated aggressively, recurrence rate is high. Radiation and surgery (total resection or hemiglossectomy) are performed. • Radical neck dissection for metastases of oral cancer to lymphatic channel in the neck region with reconstructive surgery.
- 8. Nursing Management Preoperative • Assess the patient’s nutritional status preoperatively; a dietary consultation may be necessary. • Implement enteral (through the GI tract) or parenteral (IV) feedings as needed to maintain adequate nutrition. • If a radial graft is to be performed, perform an Allen test on the donor arm must to ensure that the ulnar artery is patent and can provide blood flow to the hand after removal of the radial artery. • Assess the patient’s ability to communicate in writing as ver-bal communication may be impaired by radical surgery for oral cancer (provide a pen and paper after surgery to patients who can use them to communicate). • Obtain a communication board with commonly used words or pictures (give after surgery to patients who cannot write so that they may point to needed items). • Consult a speech therapist.
- 9. Postoperative • Assess for a patent airway. • Perform suctioning if the patient is unable to manage oral secretions; if grafting was part of the surgery, suctioning must be performed with care to prevent damage to the graft. • Assess the graft for viability; assess color (white may indicate arterial occlusion, and blue mottling may indicate venous congestion), although it can be difficult to assess the graft by looking into the mouth. • A Doppler ultrasound device may be used to locate the radial pulse at the graft site and to assess graft perfusion.
