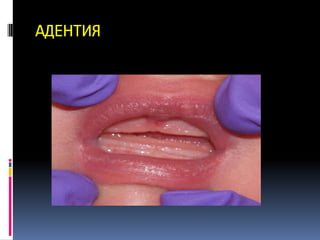
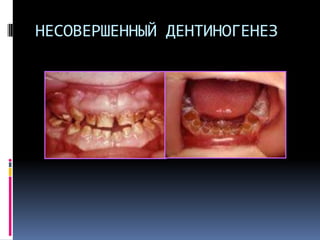
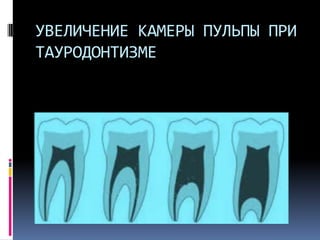
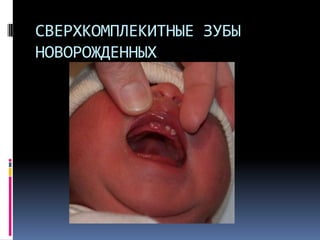
Документ описывает различные аномалии развития зубов, включая адентия, сверхкомплектные зубы, мезиодентия и патологии формы зубов. Приводятся классификации и причины возникновения данных аномалий, такие как наследственные синдромы и изменения в челюстно-лицевой области. Также рассматриваются проблемы, связанные с диагностикой и лечением данных состояний.