Sperm cryopreservation is the process of freezing sperm to preserve fertility. It involves adding cryoprotective agents to minimize freezing damage before slowly cooling sperm to -196°C in liquid nitrogen storage. Factors like semen quality, freezing technique, and thawing process can impact sperm survival. While some studies found cryopreservation may damage DNA, properly performed it selectively affects defective sperm and clinical pregnancy rates are similar to fresh sperm. Optimization involves semen preparation, controlled freezing and thawing rates, and cryoprotectant use. Further research is still needed on impacts to DNA and reproductive outcomes.

















![Cryopreservation and Reproductive
Outcome
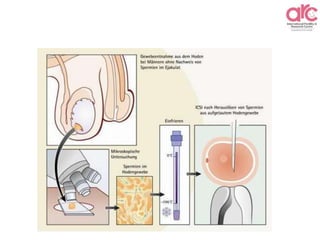
Testicular Spermatozoa:
• No statistically significant differences in all parameters examined (fertilization rate,
cleavage rate, embryo quality, implantation rate, clinical pregnancy rate, and ongoing
pregnancy rate) between ICSI cycles with fresh or cryopreserved testicular spermatozoa.
• Only, De Croo and colleagues stated that fertilization, implantation, and live-birth rates per
embryo transfer are significantly lower after ICSI.
Epididymal Spermatozoa:
• Tournaye and colleagues reported that the clinical pregnancy rate in ICSI cycles was
comparable between fresh and frozen-thawed epididymal spermatozoa.
• Sukcharoen and colleagues came to the same conclusion; also Cayan and colleagues [64]
supported the same opinion.](https://image.slidesharecdn.com/dr-170412050006/85/Spermcryoperservation-by-Dr-Chandan-19-320.jpg)


![References
[1] Marlea Di Santo, Nicoletta Tarozzi, Marco Nadalini, and Andrea Borini. Human Sperm
Cryopreservation: Update on Techniques, Effect on DNA Integrity, and Implications for ART.
Advances in Urology. Volume 2012 (2012), Article ID 854837, 12 pages.
[2] 2014 Andrology and Embryology Review Course Manual of the American Board of
Bioanalysis (ABB).
[3] World Health Organisation: Department of Reproductive Health and Research WHO
laboratory manual for the examination and processing of human semen. 5th edition. 2010.
[4] Gardner DK, Weissman A, Howles CM, Shoham Z. Textbook of Assisted Reproductive
Techniques. 3rd ed. Vol. 1. In: Agarwal A, Erenpreiss J, Sharma R. Sperm chromatin assessment.
United Kingdom: Informa healthcare, 2009:67-84.](https://image.slidesharecdn.com/dr-170412050006/85/Spermcryoperservation-by-Dr-Chandan-22-320.jpg)
