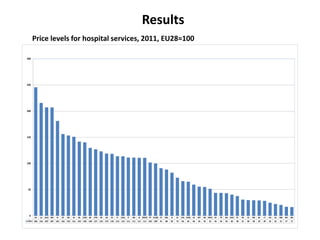
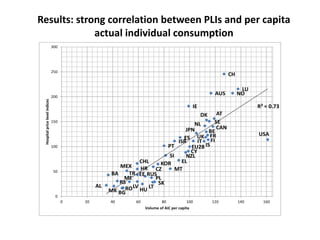
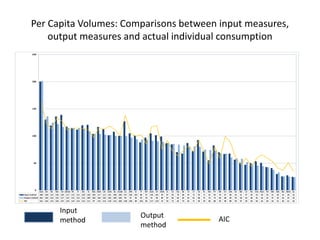
This document presents a new methodology for comparing hospital and health prices and volumes across countries using spatial price indices (PPPs). It finds price levels for hospital services are highest in Switzerland, Luxembourg, Australia, and Scandinavian countries, and lowest in Central and Eastern European countries. Total health expenditure volumes are more equal across countries when calculated using health-specific PPPs compared to GDP PPPs. However, more work is still needed on quality adjustments and accounting for non-standard medical conditions.