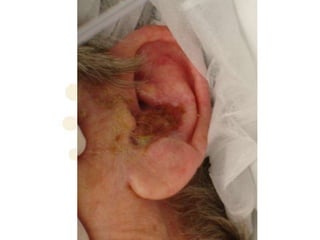
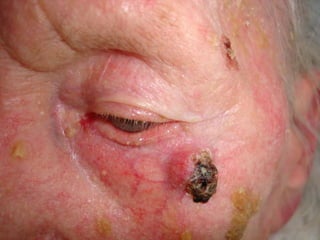
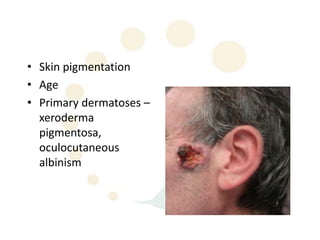
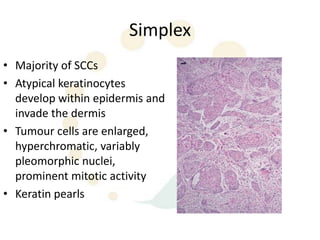
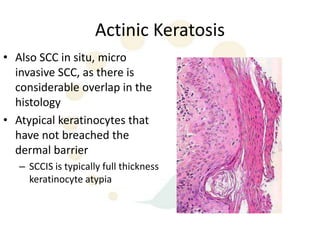
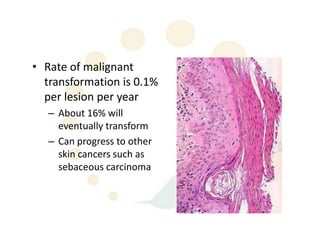
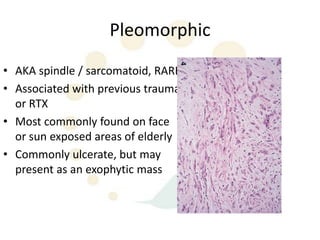
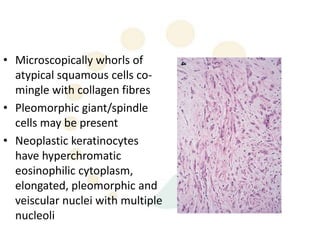
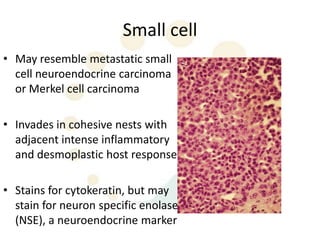
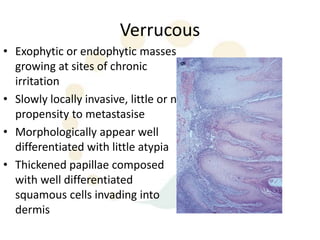
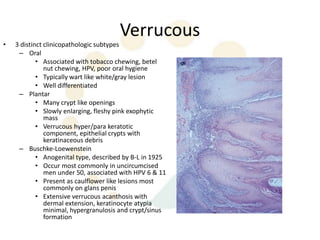
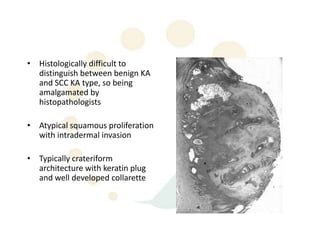
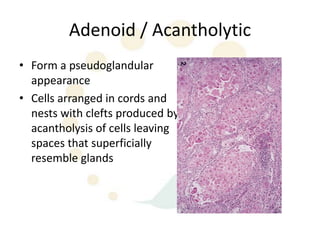
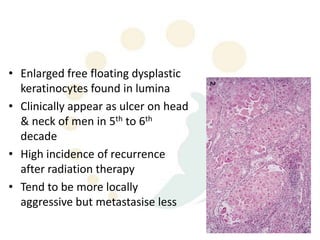
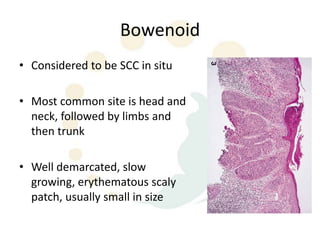
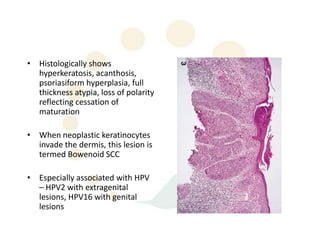
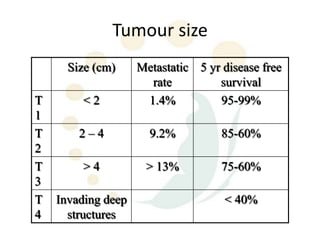
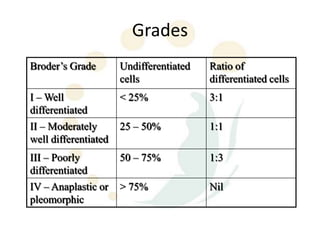
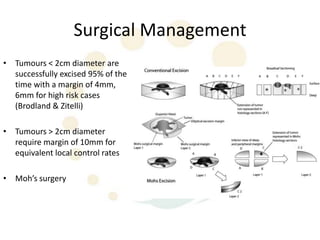
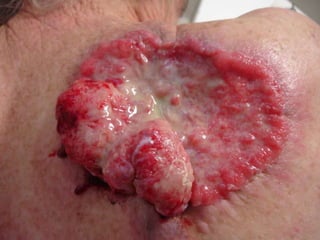
Squamous cell carcinoma (SCC) is the second most common skin cancer. It has a propensity to metastasize, making it responsible for most skin cancer deaths. Risk factors include UV exposure, age, immunosuppression, and primary dermatoses. Histological subtypes include pleomorphic, adenoid, small cell, verrucous, and keratoacanthoma. Tumor size greater than 2 cm and depth greater than 6 mm increase metastatic risk. Treatment involves surgical excision with adequate margins or other modalities like radiation for high risk cases.