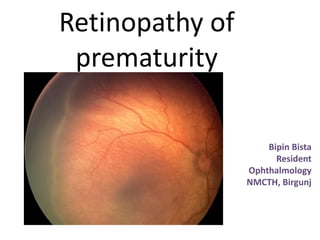
Retinopathy of prematurity
- 2. Definition : • Retinopathy of prematurity (ROP) is a proliferative retinopathy affecting premature infants of very low birth weight, who have often been exposed to high ambient oxygen concentrations.
- 3. Schematic diagram for vessels development
- 4. History • Identified by Terry in 1942 , where he first told regarding retrolental fibroplasia. • Later Owens and Owens found out that hyaloid system are normal at the time of birth and retrolental fibroplasia developed post-natally. • Term coined by Heath in 1951. • In late 60s and 70s, ABG analysis came into use, this evolved the paediatrician to titrate the incubator oxygen.
- 5. Role of Oxygen • In 1950s, confirmation were brought regarding oxygen being the major cause. • Later on, on different experimental findings : ― factors associated with very low birth weight (Lucey and dangman). ―Cyanotic heart disease and ROP (Kalina et al and Johns et al) • Supplemental Therapeutic Oxygen for Prethreshold ROP (STOP-ROP) trial.
- 6. Mechanism of Oxygen’s effect in immature retina Primary Stage : Retinal vasoconstriction and vascular occlusion • Vascular caliber decreases by 50% but may rebound to its original dimensions. • May be sustained vasoconstriction if there’s elevated arterial oxygen pressure. • Local vascular obliteration is completed by 2-3 days of sustained hyperoxic environment.
- 7. Secondary stage :Retinal neovascularization • Marked endothelial proliferation from residual vascular complexes, immediately adjacent to ablated retinal capillaries during hyperoxia. • New vessels are formed & erupt from Internal Limiting Membrane. • Newly formed angioblastic mass called as popcorn formation, mature into neovascular formation which are filled with pericytes. • Remodelling : regress from areas of higher oxygen and grows towards area of lower oxygen.
- 10. Pathogenesis • Mesenchyme, blood vessel precursor, grows from optic disc through nerve fiber of retina. On posterior edge of advancing mesenchyme, a “chicken wire” meshwork of capillaries develops to produce mature arteries and veins. (Ashton) • Similarly Vascular endothelial growth factor (VEGF)key factor for vessels growth was stated as Factor X. (Michaelson) • According to Foos, he divided into Vanguard and Rearguard. Vanguard –anterior compartment containing spindle cells (progenitors)- Garner for nourishment. Rearguard contains primitive endothelial cells which aggregates into cords for neovascularization.
- 12. Flynn and co-workers 1. Injury occurs where it has differentiated from mesenchyme to form primitive capillary meshwork. 2. After injury, mature vessels merge and survive via few vascular channels and forms mesenchymal AV shunts that replaces destroyed capillary bed. 3. Shunt (AP-AV) consists of a nest of primitive mesenchymal & maturing endothelial cells ,fed by mature arteries and veins.
- 13. Flynn also stated :- • Retina will remain in dormant period after injury for days to months • Fate of the eye is decided as the tissue thickens and changes its colour. Grey white > pink > salmon > red. • In Progressive disease, primitive cells proliferate. • Normally, these cells divide and differentiate to form normal capillary endothelium.
- 14. International Classification • The International Classification of ROP (ICROP) that was published in 1984 standardized the terminology used to describe ROP .In 2005, a second committee for the classification of ROP revised the original ICROP.
- 16. Staging of ROP • 5 stages : 1. Demarcation line 2. Ridge 3. Ridge with extraretinal fibrovascular proliferation 4. Subtotal Retinal Detachment (RD) ―4a : Extrafoveal RD ―4b : Partial RD with fovea 5. Total RD
- 17. Stage 1 : Demarcation Line • Line separating Ant. & Post. Retina • Usually white & flat , lies within plane of retina • Due to abnormal branching or arcading of vessels.
- 18. Stage 2 : Ridge • Grown demarcation line • Has height & width & occupies volume • Extends centripetally within the globe • Small tufts of new vessels (“popcorn “ lesion) seen posterior but not attached to ridge.
- 19. Stage 3:Ridge with extraretinal fibrovascular proliferation • Localised continuous with posterior & inferior aspect, causing ragged appearance of ridge as proliferation increases. • Presence of increased retinal vessels coursing from retinal surface ,not only constitute RD but also signify Vitreous Traction.
- 20. Stage 4a : Subtotal Retinal Detachment (Extrafoveal) • concave, tractional type • Occurs in periphery without central macula • Located at proliferative areas. • May extend 360 degrees without including macula • Prognosis : good if anterior.
- 21. Stage 4b : Partial Retinal detachment with foveal involvement. • Involves fovea • Prognosis : poor
- 22. Stage 5 : Total Retinal Detachment • Usually funnel shaped as seen in USG. • Involves both anterior and posterior part. • Concave configuration and extends upto optic disc.
- 23. Plus Disease • More florid form of ROP • Increased dilatation & tortuosity of retinal vessels • Iris vascular engorgement. • Pupillary rigidity • Vitreous haze • + : key sign of worst prognosis.
- 24. Preplus disease/(‘rush’) disease • Uncommon but if untreated reaches to stage 5 within few days • Posterior location • Prominence of plus disease • Ill-defined nature of retinopathy.
- 25. Other factors 1. Appearance of retrolenticular space 2. Peripheral trough : presence of peripheral red reflex in combination with apparent narrow funnel shows avascular peripheral retina. ( stage 5) 3. Anterior segment abnormalities ( stage 4 or 5).
- 26. Prethreshold and threshold disease • Prethreshold ROP, Type 1. › Zone I, any stage with plus disease; › zone I, stage 3 without plus disease; › zone II, stage 2 or 3 with plus disease. • Prethreshold ROP, Type 2. › Zone I, stage 1 or 2 without plus disease; › zone II, stage 3 without plus disease. • Threshold ROP. › Zone I or II, stage 3 (five contiguous or eight total clock hours with plus disease).
- 27. Involution of ROP • Typically at 38-39 weeks post-conceptual or post-menstrual • Downgrading of staging &/or growth of retinal vessels into more peripheral zone • Present in 70-80 % .
- 28. Cicatricial Disease • About 20% of infants with active ROP may develop this complication. • More general and more advanced or more posterior the proliferation , worse the sequelae. • Temporal vitreoretinal fibrosis and straightening of vascular arcades with ‘dragging’ of macula and disc .
- 29. Cicatricial disease (continue) • Progress to retrolental fibrovascular tissue lead to falciform retinal fold formation and to retinal detachment, sometimes total and called as retrolental fibroplasia. • Secondary glaucoma (angle closure) : major challenge.
- 30. Differential Diagnosis Stage 1 to 3 • Familial exudative vitreoretinopathy (FEVR) (chief consideration) • Coats disease • Eales disease • retinoschisis Stage 4 & 5 • Retinoblastoma • Persistent fetal vasculature • Congenital cataract • Incontinentia pigmenti -XD • FEVR -AD • Norrie’s disease -XR
- 31. Risk Factors • Cyanosis • Apnea • Mechanical ventilation • Intraventricular Hemorrhage • Seizures • Transfusions • Septicaemia • In utero hypoxia • Anemia • Patent ductus arteriosus • Vitamin E Deficiency • High Myopic
- 32. Screening Guidelines • every infant ≤306/7 weeks’ GA regardless of birth weight, as well as any infant with a birth weight ≤1250 g were screened. • In 2014, an updated (2009 to 2014) literature search was conducted.
- 33. Screening Guidelines • 1st examination should be considered 4-6 weeks from birth i.e., 31 to 33 weeks post- conception. • Prior to 4 weeks are not considered necessary.
- 37. Techniques of eye examination • Effective dilatation ( cyclopentolate 0.2% and phenylephrine 1%) twice 1 to 5 minutes apart. • Lid speculum : Cook,Alfanso,Sauer & Schaefer spatula • Restrain • N-P cultural swab • Scleral depression
- 38. Prophylaxis & Therapy 1. Vitamin E : Recognized antioxidant of choice . shouldn’t exceed 3 mg/dl. (hittner et al and kretzer et al).
- 39. Role of Light • On various researches and trials, no effective results have been found. • Neither the American Academy of Ophthalmology nor the American Academy of Pediatrics have made any recommendations about restricting ambient light from the eyes of premature infants.
- 40. Management • Laser > cryotherapy : easier and few post-op sequalae. • Diode laser (810 nm) is better than argon laser (488- 532 nm ). • Photocoagulation burns are distributed 0.5-1 burn width apart . • 600-1000 laser spots. • Power : 0.15 watts • Pulse duration : 0.3-0.4 seconds.
- 41. Management (continue) • Chest & CVS examination • Swaddled in blanket with mydriatics & anaesthesia. • In case of GA, perform laser in both the eyes.
- 42. Intravitreal anti- VEGF agents • More precedence in zone I • Look after systemic complications and long term effects. • The Bevacizumab Eliminates the Angiogenic Threat of Retinopathy of Prematurity (BEAT-ROP) Study
- 43. Lens-sparing vitrectomy • Can be performed for stage 4a , where success rate is 90 % .
- 44. Early treatment of ROP (ETROP) Trial 2003 Type 1 ROP • ZONE II : plus disease with stage 2 or 3. • ZONE I :Plus disease with stage 1, 2 or 3. • Stage 3 without Plus disease. • Treatment : Peripheral laser ablation. • Plus disease: involve at least 2 quadrants of fundus with floridity. Type 2 ROP • Zone II : Stage 3 without plus disease. • Zone I : Stage 1 or 2 without plus disease. • Treatment : Wait and watch for progression.
- 45. Other recent studies • IGF-1 pathway & dietary supplementation with omega-3 polyunsaturated fatty acids (PUFAs). • Recombinant Erythropoeitin (Epo)
- 46. Associated conditions & late sequalae • Myopia with astigmatism • Anisometropia • Strabismus • Amblyopia • Cataract • Glaucoma • Macular pigment epitheliopathy • VR scarring • TRD • Anomalous foveal changes.
- 47. TELE-ROP • Digital photographic retinal images that are captured and sent for remote interpretation is a developing approach to ROP screening Evaluating Acute-phase ROP (e-ROP) study
- 48. References 1. Retina , 4th edition , Stephen J. Ryan 2. Kanski’s clinical ophthalmology , 8th edition, Brad bowling. 3. Jefferies, A. L., & Canadian Paediatric Society, Fetus and Newborn Committee. (2016). Retinopathy of prematurity: An update on screening and management. Paediatrics & Child Health, 21(2), 101–104.
- 49. THANK YOU
Editor's Notes
- 15 million preterm birth, India, china, Nigeria, rate of pre-term birth – 5 to 18% .Updated analysis -Sustainable dev. Goals 2016
- 4 mnths grow from disc, reach ora serrata 8 mnths & ora temporally after birth,
- Still no trials for determining the best level for targeted saturation.
- Temporal retina is susceptible to ROP. Oxygen exerts an important effect on the remodeling of the original primitive capillary network that develops in the retina
- Showed vasoconstriction followed by vascular occlusion.
- New vessels are formed from these cells..
- Neovsculrstn posterior to ciliary closure-long arrow,short-lens cpsule. 2) neovsculristn in surface of disc.
- FA of young kitten with o2 induced nv. Midtrnst phase & late phase of angiogram.
- Specimen from 29 week old infnt. Thickened VNGURD---vasodilatation RERGUARD..
- Similarly, role of Nitric oxide (Brooks and ass.) and decreased production of VEGF (Alon et al) , overall results in vasoattenuation. Mesenchyml shunt are found suggestive of pathognomic of ROP.
- , where retinal findings are stable. --ie, endothelial proliferation and erupt through ILM growing anteriorly .---else leads to Tractional RD.
- Inner zone : radius is twice the distance from disc to macul.2Peripheral of Zone I and encircles tangential to ora serrata.--Remaining temporal crest anterior to Zone II. Farthest and last zone to localize. As per 30 degree sector involvement.
- These extra-retinal vascularization can be : placoid, polypoid or pedunculated.Placoid being the most common. Significant synchysis and condensation of vitreous over the ridge due to depolymerisation of hyaluronic acid and collapse of collagen framework.
- pupil difficult to dilate because of adhesions to the anterior lens capsule and persistence of the pupillary membrane with retention of its vascular network.
- Posterior synechiae, iris atrophy, ectropion uveae are common formations…
- As defined by Cryo-ROP 1986-2003…
- In 2010, the Canadian Paediatric Society suggested by the Royal College of Paediatrics and Child Health, and the Royal College of Ophthalmologists-found that the risk for severe ROP was greatest in infants ≤28 weeks’ GA or weighing <1000 g at birth.
- ROP takes longest to develop in very immature infants
- Fierson WM, American Academy of Pediatrics, Section on Ophthalmology. American Academy of Ophthalmology. American Association for Pediatric Ophthalmology and Strabismus. American Association of Certified Orthoptists Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2013;131(1):189–95.
- Leads to maturation of spindle cells which decreases gap junction between adjacent cells , decreases cytoplasmic volume of RER and thus cessation of synthesis of angiogenic factors
- peripheral ablation of the avascular retina for type 1 prethreshold ROP. monitored closely for regression of plus disease, neovascularization and ridge elevation. Lens sparing vitrectomy-ridge elevation (particularly six clock-hours or more), persistent plus disease or vitreous haze
- regulating VEGF signaling through VEGF receptors can restore physiologic homeostasis and permit ordered developmental intraretinal angiogenesis thereby reducing hypoxic peripheral avascular retina, which drives disordered angiogenesis.later recurrence, myopia, longer f/u
- essential for vascular growth through regulation of VEGF signalling…promoter of red blood cell formation, used to treat anemia in some premature infants
- Late-onset retinal detachment and cataracts also require aggressive management. Individuals with ROP must be followed for eye disease throughout their lives.
