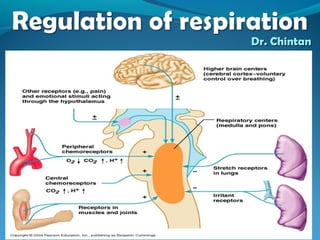
Two Mechanisms Controlling Respiration: Neural and Chemical
- 2. Two Mechanisms which control respirationTwo Mechanisms which control respiration 1) Neural Mechanism 2) Chemical Mechanism
- 3. Neural control of respiration 1) Voluntary control of respiration 2) Automatic control of respiration 3) Reflex control of respiration
- 4. Voluntary control of respiration Respiration is under automatic or involuntary control basically. But to some extent it can be controlled voluntary as most of the respiratory muscles are voluntary muscles. Respiration can be modified both in rate and depth at will for a specific period only. Voluntary hyperventilation or hypoventilation, breath holding, forceful inspiration or expiration efforts etc, are examples of this.
- 5. Centre for voluntary control isCentre for voluntary control is motor cortexmotor cortex Centre is in motor cortex which sends impulses via corticospinal tract to the respiratory muscles For inspiration, Phrenic nerve motor neurons in C3,4,5 and external intercostal muscles motor neurons in ventral horn cells of T1,2 stimulate the resp muscles Corticobulbar tract which modifies activity of medullary neurons
- 6. Ondine’s curseOndine’s curse In conditions like Bulbar Poliomyelitis, Tumors of brain stem etc automatic control is lost and voluntary control is present. This is because impulses arising from brain stem control automatic respiration. This is known as Ondine’s curse. Death is due to exhaustion.
- 8. Automatic control of respirationAutomatic control of respiration The center is located in brainstem in pons and medulla bilaterally. It is divided into three major collections of neurons: (1) a dorsal respiratory group, located in the dorsal portion of the medulla, which mainly causes inspiration; (2) a ventral respiratory group, located in the ventrolateral part of the medulla, which mainly causes expiration; (3) the pneumotaxic center, located dorsally in the superior portion of the pons, which mainly controls rate and depth of breathing.
- 9. 4) Apneustic center in lower pons. It is thought to have an excitatory effect on Inspiratory neurons .
- 11. Experimental studies done on cat toExperimental studies done on cat to show the centersshow the centers 1) Section A – made above Pons- normal respiration- eupnoea. 2) Section B - made below medulla- stops respiration – apnoea. 3) Section C - in pons between Pneumotaxic center and Apneustic center - Apneustic breathing, 4) Section D - below Apneustic but above medulla- more or less respiration continues rhythmically showing evidence of reciprocal innervation between inspiratory and expiratory neurons.
- 12. DRG- in NTS - controls inspiration and rhythmDRG- in NTS - controls inspiration and rhythm The dorsal respiratory group of neurons extends most of the length of the medulla. Most of its neurons are located within the nucleus of the tractus solitarius, although additional neurons in the adjacent reticular substance of the medulla also play important roles in respiratory control. The NTS is the sensory termination of both the vagal and the glossopharyngeal nerves, which transmit sensory signals into the respiratory center from (1) peripheral chemoreceptors, (2) baroreceptors, and (3) several types of receptors in the lungs.
- 13. Rhythmical inspiratory discharges from DRGRhythmical inspiratory discharges from DRG The basic rhythm of respiration is generated mainly in the dorsal respiratory group of neurons. Even when all the peripheral nerves entering the medulla have been sectioned and the brain stem transected both above and below the medulla, this group of neurons still emits repetitive bursts of inspiratory neuronal action potentials.
- 14. Inspiratory Ramp SignalInspiratory Ramp Signal The nervous signal that is transmitted to the inspiratory muscles, mainly the diaphragm, is not an instantaneous burst of action potentials. Instead, in normal respiration, it begins weakly and increases steadily in a ramp manner for about 2 seconds. Then it ceases abruptly for approximately the next 3 seconds, which turns off the excitation of the diaphragm and allows elastic recoil of the lungs and the chest wall to cause expiration.
- 15. Ramp signal advantageousRamp signal advantageous The inspiratory signal begins again for another cycle; this cycle repeats again and again, with expiration occurring in between - ramp signal. It causes a steady increase in the volume of the lungs during inspiration, rather than inspiratory gasps.
- 16. Two qualities of inspiratory rampTwo qualities of inspiratory ramp controlled as followscontrolled as follows 1. Control of the rate of increase of the ramp signal, so that during heavy respiration, the ramp increases rapidly and therefore fills the lungs rapidly. 2. Control of the limiting point at which the ramp suddenly stops. This is the usual method for controlling the rate of respiration; the earlier the ramp ceases → the shorter the duration of inspiration → shortens the duration of expiration → the frequency of respiration is increased
- 17. Newer conceptNewer concept Rhythmic respiration is initiated by a small group of synaptically coupled pacemaker cells in the pre-Botzinger complex on either side of the medulla between the nucleus ambiguous and the lateral reticular nucleus. These neurons discharge rhythmically, and they produce rhythmic discharges in phrenic motor neurons that are abolished by sections between the pre-Botzinger complex and these motor neurons. They also contact the hypoglossal nuclei, and the tongue is involved in the regulation of airway resistance.
- 18. Pre Botzinger areaPre Botzinger area Rhythmic discharge (tracing below) of neurons in the pre-Botzinger complex (pre- BOTC) in a brain slice from a neonatal rat. IO, inferior olive; LRN, lateral reticular nucleus; NA, nucleus ambiguous; XII, nucleus of 12th cranial nerve; 5SP, spinal nucleus of trigeminal nerve
- 20. VRG- functions in both inspiration andVRG- functions in both inspiration and expirationexpiration Located in each side of the medulla, about 5 millimeters anterior and lateral to the dorsal respiratory group of neurons, is the ventral respiratory group of neurons, found in the nucleus ambiguous rostrally and the nucleus retroambiguous caudally.
- 21. VRG differs functionally from DRG as followsVRG differs functionally from DRG as follows 1) The neurons of the ventral respiratory group remain almost totally inactive during normal quiet respiration. normal quiet breathing is caused only by repetitive inspiratory signals from the dorsal respiratory group transmitted mainly to the diaphragm, and expiration results from elastic recoil of the lungs and thoracic cage.
- 22. 2) When the respiratory drive for increased pulmonary ventilation becomes greater than normal, respiratory signals spill over into the ventral respiratory neurons from the basic oscillating mechanism of the dorsal respiratory area. As a consequence, the ventral respiratory area contributes extra respiratory drive
- 23. 3) Electrical stimulation of a few of the neurons in the ventral group causes inspiration, whereas stimulation of others causes expiration. These neurons contribute to both inspiration and expiration. They are especially important in providing the powerful expiratory signals to the abdominal muscles during very heavy expiration.
- 24. Newer conceptNewer concept Both DRG and VRG are interconnected and equally important for rhythmic respiration along with several other neurons in the vicinity. There is reciprocal innervation between I and E neurons.
- 26. Pneumotaxic centerPneumotaxic center It Limits the Duration of Inspiration and Increases the Respiratory Rate. It is located dorsally in the nucleus Para brachialis of the upper pons, transmits signals to the inspiratory area. The primary effect of this center is to control the “switch-off” point of the inspiratory ramp, thus controlling the duration of the filling phase of the lung cycle.
- 27. Limits duration of inspirationLimits duration of inspiration When the pneumotaxic signal is strong, inspiration might last for as little as 0.5 second, thus filling the lungs only slightly; when the Pneumotaxic signal is weak, inspiration might continue for 5 or more seconds, thus filling the lungs with a great excess of air.
- 28. Limitation of inspiration affects rate ofLimitation of inspiration affects rate of respirationrespiration A secondary effect of increasing the rate of breathing, because limitation of inspiration also shortens expiration and the entire period of each respiration. A strong pneumotaxic signal can increase the rate of breathing to 30 to 40 breaths per minute, Whereas a weak pneumotaxic signal may reduce the rate to only 3 to 5 breaths per minute.
- 29. Pneumotaxic center alsoPneumotaxic center also inhibits the Apneustic centerinhibits the Apneustic center Thus it prevents Apneusis which is a type of arrested breathing.
- 31. Apneustic centerApneustic center It is located in in lower part of Pons. It stimulates the inspiratory center and increases the inspiration. It gets feedback from vagal afferents and also from other respiratory centers . Pneumotaxic center inhibits it. It works in association with Pneumotaxic center to control depth of inspiration.
- 32. Its function is demonstrated by sectioning of vagus nerve to medulla and by blocking the connection from Pneumotaxic center by transecting PONS in mid region. This causes loss of inhibitory control over Apneustic center which sends signals to DRG and prevents switch off of ramp signals so lungs become completely filled with air and only occasional expiratory gasps occur.
- 33. Thus if vagus is intact regular rhythm of respiration continues. If vagus is cut arrest of respiration occurs called Apneusis.
- 35. Reflex control of respirationReflex control of respiration 1) By receptors inside respiratory system a) Hering Breuer Reflexes due to stretch receptors in muscular wall of bronchi and bronchioles, b) pulmonary irritant receptors, c) J receptors 2) By receptors outside respiratory system A) Those which stimulate respiration - proprioceptors, nociceptors, thermoceptors, emotional stimuli from hypothalamus and limbic system. B)Those which inhibit respiration- Baroreceptors and visceroreceptors
- 36. Hering Breuer ReflexesHering Breuer Reflexes Located in the muscular portions of the walls of the bronchi and bronchioles throughout the lungs are stretch receptors transmit signals through the vagi into the dorsal respiratory group of neurons when the lungs become overstretched.
- 37. These signals act in same way as signalsThese signals act in same way as signals from Pneumotaxic centerfrom Pneumotaxic center when the lungs become overly inflated, the stretch receptors activate an appropriate feedback response that “switches off” the inspiratory ramp and thus stops further inspiration. This is called the Hering - Breuer inflation reflex. This reflex also increases the rate of respiration, as is true for signals from the pneumotaxic center
- 38. Importance of H-B inflation reflexImportance of H-B inflation reflex 1) This reflex operates only when Tidal volume exceeds 1.5 liters as in exercise and not in normal ventilation and so prevents over inflation of lungs and is thus protective 2) This effect is not seen in man if vagi are cut and also so in transplanted lungs which are denervated.
- 39. Hering Breuer Deflation reflexHering Breuer Deflation reflex It is seen when there is extreme deflation of lungs as seen in collapse of lungs, pneumothorax, hydrothorax, etc. The receptors are stimulated by change in shape of small airways in collapsed area so also called as compression receptors. So forceful deflation of lungs causes stimulation of receptors → stimulation of inspiration via vagus
- 40. Effect of irritant receptors in theEffect of irritant receptors in the airwaysairways The epithelium of the trachea, bronchi and bronchioles is supplied with sensory nerve endings called pulmonary irritant receptors and are rapidly adapting and innervated by myelinated vagal nerve fibers. They are stimulated by many incidents like lung hyperinflation, exogenous subs like SO2, smoke and endogenous subs like histamine, PGs. These cause hyperpnoea, coughing and sneezing, bronchial constriction and mucus secretion in diseases as asthma and emphysema.
- 41. Function of ‘J receptors’Function of ‘J receptors’ A few sensory nerve endings have been described in the alveolar walls in juxtaposition to the pulmonary capillaries—hence the name “J receptors.” they are non myelinated nerve endings (C fibers). They are stimulated especially when the pulmonary capillaries become engorged with blood or when pulmonary edema occurs as in congestive heart failure. Although the functional role of the J receptors is not clear, their excitation may give the person a feeling of dyspnea
- 42. J receptors cause the pulmonaryJ receptors cause the pulmonary chemo reflexchemo reflex Apnea followed by Hyperventilation, bradycardia, hypotension, bronchoconstriction, and mucus secretion and skeletal muscle weakness (Seen in Bhopal gas tragedy). This is similar to Coronary Chemo reflex or Bezold Jarisch Reflex
- 43. Receptors outside respiratory systemReceptors outside respiratory system which stimulate respirationwhich stimulate respiration 1) Proprioceptors – Present in muscles, tendons, joints etc when stimulated reflexly stimulates Inspiratory neurons. This helps to increase ventilation at the start of exercise even before changes in Pco2, Po2 and H ions concentration occur.
- 44. 2) Nociceptors - Pain receptors 3) Emotional stimuli – all stimulate respiratory system via hypothalamus and limbic system. 4) Chemoreceptors – stimulated by acidosis and hypoxia. Hypotension and shock produce hyperventilation due to stimulation of chemoreceptors.
- 45. 5) Thermoreceptors – present in hypothalamus are stimulated when there is increase in body temperature as in fever, exercise they send impulses to respiratory center and produce increase in rate of respiration.
- 46. Those which inhibit respirationThose which inhibit respiration 1) Baroreceptors – inhibit reflexly. Adrenaline apnea is an eg of this. 2) Visceroreceptors – visceral reflexes like vomiting, swallowing, etc reflexly inhibit respiration, Eg is Deglutition apnea
- 48. Other factors affecting respirationOther factors affecting respiration 1) Sleep- Respiration is less rigorously controlled during sleep than in the waking state, and brief periods of apnea occur in normal sleeping adults. Sleep Apnea Syndrome It is a type of obstructive sleep apnea. It occurs at any age. Cause is failure of Genioglossus muscle to contract during inspiration which causes the tongue to fall backward to obstruct the airways. This muscle normally keeps the tongue forward.
- 49. S/S are morning headache, fatigue, hypoxemic, Hypercapneic condition Prevention by avoiding sedatives or respiratory depressants prior to sleep, breathing in prone and avoiding sleeping on back, Positive pressurePositive pressure controlled O2 inhalationcontrolled O2 inhalation.
- 50. Sudden Infant DeathSudden Infant Death SyndromeSyndrome A type of central sleep apnea due to failure of respiratory centers to produce neural impulses so causing total stoppage of respiration.
- 51. Effect of brain edemaEffect of brain edema The activity of the respiratory center may be depressed or even inactivated by acute brain edema resulting from brain concussion. the head might be struck against some solid object, after which the damaged brain tissues swell, compressing the cerebral arteries against the cranial vault and thus partially blocking cerebral blood supply.
- 52. TreatmentTreatment Respiratory depression resulting from brain edema can be relieved temporarily by intravenous injection of hypertonic solutions such as highly concentrated mannitol solution. These solutions osmotically remove some of the fluids of the brain, thus relieving intracranial pressure and sometimes re-establishing respiration within a few minutes
- 53. Effect of Anesthesia- respiratoryEffect of Anesthesia- respiratory depressiondepression The most prevalent cause of respiratory depression and respiratory arrest is over dosage with anesthetics or narcotics. For instance, sodium pentobarbital depresses the respiratory center considerably more than many other anesthetics, such as halothane.
- 54. At one time, morphine was used as an anesthetic, but this drug is now used only as an adjunct to anesthetics because it greatly depresses the respiratory center while having less ability to anesthetize the cerebral cortex
- 56. Chemical regulation of respirationChemical regulation of respiration The ultimate goal of respiration is to maintain proper concentrations of oxygen, carbon dioxide, and hydrogen ions in the tissues. Respiratory activity is highly responsive to changes in each of these. Excess carbon dioxide or excess hydrogen ions in the blood mainly act directly on the respiratory center itself, causing greatly increased strength of both the inspiratory and the expiratory motor signals to the respiratory muscles.
- 57. Oxygen acts via peripheralOxygen acts via peripheral ChemoreceptorsChemoreceptors Oxygen, in contrast, does not have a significant direct effect on the respiratory center of the brain in controlling respiration. Instead, it acts almost entirely on peripheral chemoreceptors located in the carotid and aortic bodies, these in turn transmit appropriate nervous signals to the respiratory center for control of respiration
- 59. CO2 and H ions act directly on centralCO2 and H ions act directly on central chemoreceptorschemoreceptors Chemo sensitive area (CSA) is located bilaterally, lying only 0.2 millimeter beneath the ventral surface of the medulla. This area is highly sensitive to changes in either blood Pco2 or hydrogen ion concentration, and it in turn excites the other portions of the respiratory center
- 60. Excitation of CSA sensor neurons byExcitation of CSA sensor neurons by HH ions is the primary stimulusions is the primary stimulus Hydrogen ions do not easily cross the blood- brain barrier. changes in hydrogen ion concentration in the blood have considerably less effect in stimulating the chemo sensitive neurons than do changes in blood carbon dioxide, carbon dioxide stimulate these neurons secondarily by changing the hydrogen ion concentration. CO2 has more potent effect than H ions
- 61. Chemo sensitive areaChemo sensitive area
- 63. Decreased stimulatory effect of CO2Decreased stimulatory effect of CO2 after first 1 to 2 daysafter first 1 to 2 days Excitation of the respiratory center by carbon dioxide is great for the first few hours after the blood carbon dioxide first increases, but then it gradually declines over the next 1 to 2 days, decreasing to about one fifth the initial effect. It results from renal readjustment of the hydrogen ion concentration in the circulating blood back toward normal after the carbon dioxide first increases the hydrogen concentration. The kidneys achieve this by increasing the blood bicarbonate, which binds with the hydrogen ions in the blood and cerebrospinal fluid to reduce their concentrations
- 64. Diffusion of Bicarbonate ions- combineDiffusion of Bicarbonate ions- combine with H ions & decreasewith H ions & decrease 2) Over a period of hours, the bicarbonate ions also slowly diffuse through the blood - brain and blood – CSF barriers and combine directly with the hydrogen ions adjacent to the respiratory neurons as well, thus reducing the hydrogen ions back to near normal.
- 65. A change in blood carbon dioxide concentration therefore has a potent acute effect on controlling respiratory drive but only a weak chronic effect after a few days’ adaptation
- 66. Unimportance of oxygen for control ofUnimportance of oxygen for control of respiratory centrerespiratory centre Changes in oxygen concentration have virtually no direct effect on the respiratory center itself to alter respiratory drive although oxygen changes do have an indirect effect, acting through the peripheral chemoreceptors
- 67. Hb as a good bufferHb as a good buffer The hemoglobin oxygen buffer system delivers almost normal amounts of oxygen to the tissues even, when the pulmonary Po2 changes from a value as low as 60 mm Hg up to a value as high as 600 mm Hg.
- 68. Chemoreceptors - O2Chemoreceptors - O2 The carotid bodies are located bilaterally in the bifurcations of the common carotid arteries. Their afferent nerve fibers pass through Herring's nerves to the glossopharyngeal nerves and then to the dorsal respiratory area of the medulla. The aortic bodies are located along the arch of the aorta; their afferent nerve fibers pass through the vagi, also to the dorsal medullary respiratory area.
- 70. Stimulation of chemoreceptors byStimulation of chemoreceptors by decreased arterial Po2decreased arterial Po2 Shows the effect of different levels of arterial Po2 on the rate of nerve impulse transmission from a carotid body. the impulse rate is particularly sensitive to changes in arterial Po2 in the range of 60 down to 30 mm Hg, a range in which hemoglobin saturation with oxygen decreases rapidly
- 71. Effect of CO2 and H ion concentrationEffect of CO2 and H ion concentration on chemoreceptorson chemoreceptors Indirect effect- An increase in either carbon dioxide concentration or hydrogen ion concentration also excites the peripheral chemoreceptors and, in this way, indirectly increases respiratory activity. However, the direct effects of both these factors in the respiratory center itself via CSA are much more powerful than peripheral ones.
- 72. One difference between peripheral andOne difference between peripheral and central effects of CO2 & H ionscentral effects of CO2 & H ions The stimulation by way of the peripheral chemoreceptors occurs as much as five times as rapidly as central stimulation. So that the peripheral chemoreceptors might be especially important in increasing the rapidity of response to carbon dioxide at the onset of exercise. Thus direct effect via CSA is very powerful than indirect via peripheral chemoreceptors. But indirect effect is very rapid than direct effect.
- 73. Basic mechanism of stimulation of chemoreceptorsBasic mechanism of stimulation of chemoreceptors by o2 deficiency – NT Dopamineby o2 deficiency – NT Dopamine
- 74. Mechanism of release of NTsMechanism of release of NTs Type I glomus cells have O2-sensitive K+ channels, whose conductance is reduced in proportion to the degree of hypoxia to which they are exposed. This reduces the K+ efflux, depolarizing the cell and causing Ca2+ influx, primarily via L-type Ca2+ channels. The Ca2+ influx triggers action potentials and transmitter release, with consequent excitation of the afferent nerve endings
- 75. Low Po2 stimulates ventilation whenLow Po2 stimulates ventilation when co2& H ions constantco2& H ions constant Only the ventilatory drive due to the effect of low oxygen on the chemoreceptors is active. There is almost no effect on ventilation as long as the arterial Po2 remains greater than 100 mm Hg. But at pressures lower than 100 mm Hg, ventilation approximately doubles when the arterial Po2 falls to 60 mm Hg
- 76. AcclimatizationAcclimatization Chronic Breathing of Low Oxygen Stimulates Respiration Even More—The Phenomenon of “Acclimatization” Mountain climbers have found that when they ascend a mountain slowly, over a period of days rather than a period of hours, they breathe much more deeply and therefore can withstand far lower atmospheric oxygen concentrations than when they ascend rapidly.
- 77. Reason for acclimatizationReason for acclimatization Within 2 to 3 days, the respiratory center in the brain stem loses about four fifths of its sensitivity to changes in Pco2 and hydrogen ions. Therefore, the excess ventilatory blow-off of carbon dioxide that normally would inhibit an increase in respiration fails to occur, and low oxygen can drive the respiratory system to a much higher level of alveolar
- 78. Instead of the 70 per cent increase in ventilation that might occur after acute exposure to low oxygen, the alveolar ventilation often increases 400 to 500 per cent after 2 to 3 days of low oxygen; this helps greatly in supplying additional oxygen to the mountain climber
- 79. Effect of exercise on respirationEffect of exercise on respiration regulationregulation In exercise there is rise of co2 formation and more of o2 consumption. Neurogenic stimulation by higher centers and proprioceptors is first most important mechanism to increase ventilation on initiation of exercise even before chemical stimulation develops.
- 80. If nervous signals are too weak or too strong then chemical factors play an important role in respiratory adjustment in exercise. 1) At the beginning of exercise anticipatory stimulation of respiration occurs thus increasing alveolar ventilation so that it decreases arterial Pco2.
- 81. 2) After 30 to 40 seconds the amount of co2 released by exercising muscles into blood matches approximately with increase rate of alveolar ventilation and arterial Pco2 returns to normal. Neurogenic factor in exercise shifts the ventilation to higher levels to match the rate of co2 formation and o2 utilization thus keeping Po2 and Pco2 toward normal level.
- 82. Factors causing Increased ventilationFactors causing Increased ventilation in exercisein exercise 1) Higher centers – motor cortex, hypothalamus, which cause rise of ventilation even before exercise, stimulate VMC increasing BP. 2) Sympathetic stimulation can further stimulate. 3) Increase body temperature 4) Sensory proprioceptors
- 83. 5) Low P02, high Pco2 and H ions via peripheral chemoreceptors. 6) Increase in plasma K during exercise stimulates peripheral chemoreceptors. 7) Lactic acid liberated in exercise increases co2 which stimulates respiration. 8) Better match of ventilation –
- 84. Effect of acid base changesEffect of acid base changes Acidosis – H ions conc- stimulation↑ ↑ Alkalosis- H ions conc- stimulation↓ ↓ In metabolic acidosis as seen in diabetes, renal failure, severe muscular exercise, starvation etc more H ions and less HCO3 in blood which stimulate respiration (Kussumaul breathing) which reduces co2 which leads to compensatory fall in blood H ion conc.
- 85. In metabolic alkalosis as in vomiting with loss of HCL due to pyloric or high intestinal obstruction there is less H ions and more HCO3 so ventilation is depressed and arterial PCO2 increases which brings H ions towards normal.
- 86. Respiratory acidosis- Here ventilation is depressed due to causes like emphysema, depression of respiratory center, morphine or COPD. Here hypoventilation causes rise of co2 which stimulates central and peripheral chemoreceptors and increases alveolar ventilation and correction of respiratory acidosis.
- 87. Respiratory alkalosis - as seen in voluntary hyperventilation, chronic lack of o2 at high altitudes, anxiety, hysteria salicylate over dosage etc.
- 88. Breath holdingBreath holding Respiration can be voluntarily inhibited for some time, but eventually the voluntary control is overridden. The point at which breathing can no longer be voluntarily inhibited is called the breaking point. Breaking is due to the rise in arterial PCO2 and the fall in PO2. Individuals can hold their breath longer after removal of the carotid bodies. Breathing 100% oxygen before breath holding raises alveolar PO2 initially, so that the breaking point is delayed. The same is true of hyperventilating room air, because CO2 is blown off and arterial PCO2 is lower at the start.
- 89. Reflex or mechanical factors appear to influence the breaking point Subjects who breathe a gas mixture low in CO2 and high in O2 can hold their breath for an additional 20 seconds or more. Psychological factors also play a role, and subjects can hold their breath longer when they are told their performance is very good
- 90. Hormonal effects on respirationHormonal effects on respiration Ventilation is increased during the luteal phase of the menstrual cycle and during pregnancy Experiments with animals indicate that this is due to activation of estrogen - dependent progesterone receptors in the hypothalamus. However, the physiologic significance of this increased ventilation is unknown.
- 91. Periodic breathingPeriodic breathing An abnormality of respiration called periodic breathing occurs in a number of disease conditions. The person breathes deeply for a short interval and then breathes slightly or not at all for an additional interval, with the cycle repeating over and over. One type of periodic breathing, Chyne-Stokes breathing, is characterized by slowly waxing and waning respiration occurring about every 40 to 60 seconds.
- 92. Chyne- Stokes breathingChyne- Stokes breathing Apnea followed by hyperventilationApnea followed by hyperventilation
- 93. MechanismMechanism Hyperventilation causes - Po2 and wash out of co2↑ – which causes depression of respiration and so apnoea --- which now increases Pco2 and reduces Po2 --- which now stimulates ventilation again.
- 94. The basic cause of Cheyne-Stokes breathing occurs in everyone. However, under normal conditions, this mechanism is highly “damped.” That is, the fluids of the blood and the respiratory center control areas have large amounts of dissolved and chemically bound carbon dioxide and oxygen. Therefore, normally, the lungs cannot build up enough extra carbon dioxide or depress the oxygen sufficiently in a few seconds to cause the next cycle of the periodic breathing
- 95. CausesCauses Physiological Voluntary hyperventilation Healthy infants and adults during sleep High altitude hypoxia Pathological Uremia Cardiac failure(LVF) Brain damage
- 96. In cardiac failure (LVF)- Slow blood flow- so delayed gas transport from lungs to brain. In LVF - Pulmonary congestion so hampering gas exchange – hypoxia — stimulates resp center --- increase vent – washout of co2 and more o2 – due to sluggish blood flow blood with low co2 takes more time to reach brain resp centers so — apnea.
- 97. The brain damage often turns off the respiratory drive entirely for a few seconds; then an extra intense increase in blood carbon dioxide turns it back on with great force. Cheyne-Stokes breathing of this type is frequently a preface to death from brain malfunction.
- 98. Biot’s breathingBiot’s breathing Respiration characterized by alternate Eupnoea and Apnea. 3-4 cycles of normal breathing followed by abrupt apnea and again abrupt onset of normal respiration. Seen in meningitis, severe brain damage and diseases affecting medulla.
- 99. Kussumaul’s breathingKussumaul’s breathing Seen in metabolic acidosis Rapid and deep breathing without uneasiness. Acidosis – H ions conc- stimulation↑ ↑ Alkalosis- H ions conc- stimulation↓ ↓ metabolic acidosis seen in diabetes, renal failure, severe muscular exercise, starvation etc more H ions and less HCO3 in blood which stimulate respiration (Kussumaul's breathing) which reduces co2 which leads to compensatory fall in blood H ion conc.
- 100. Thanq…Thanq…
