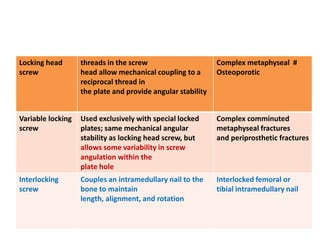
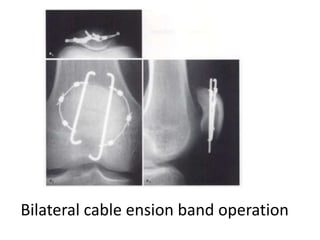
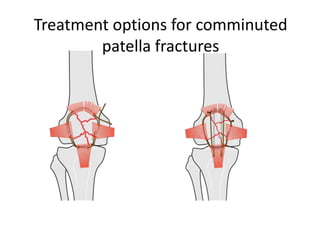
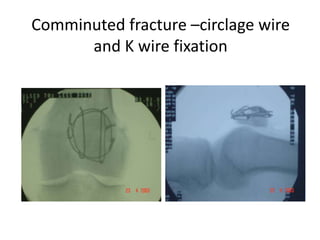
This document discusses the principles of internal fracture fixation according to the AO foundation. It covers the historical background of internal fixation techniques dating back to the late 19th century pioneers. The key principles of internal fixation are outlined as anatomical reduction, stable fixation, preservation of blood supply, and early mobilization. Various internal fixation devices, techniques, and their functions are described in detail including plates, screws, intramedullary nails. Factors such as fracture pattern, bone quality, and soft tissue injury that influence the choice of implants are also discussed.





















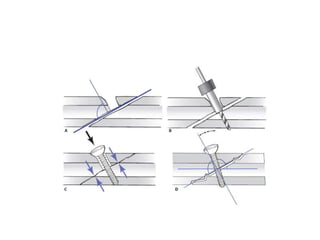
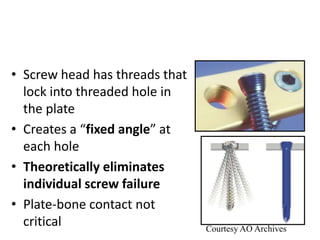
![• Area of typical application (cortex, cancellous
bone, bicortical,or monocortical)
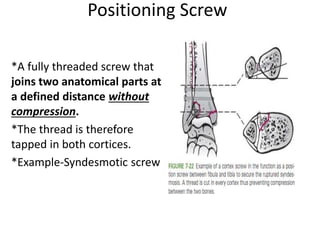
• Function (lag screw, locking head screw [LHS],
position screw, etc.)](https://image.slidesharecdn.com/principlesofinternalfixation-180130203819/85/Principles-of-internal-fixation-27-320.jpg)