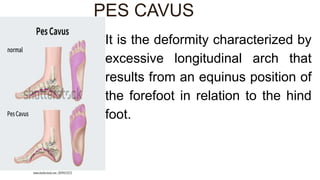
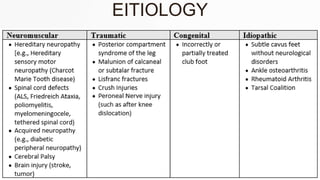
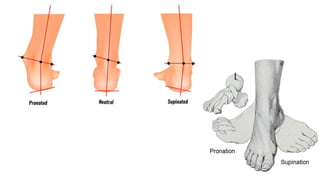
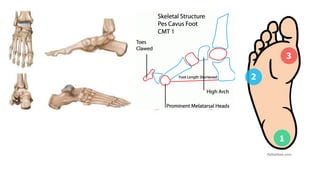
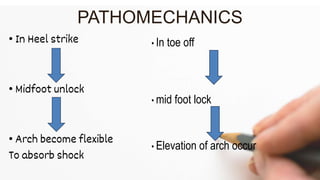
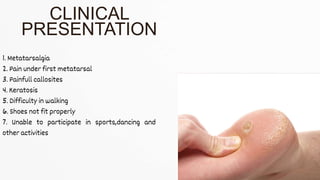
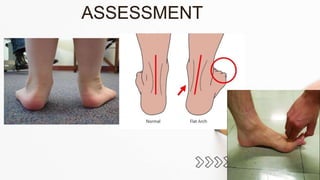
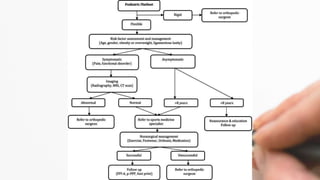
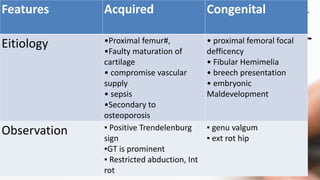
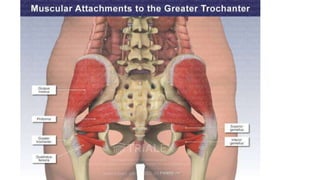
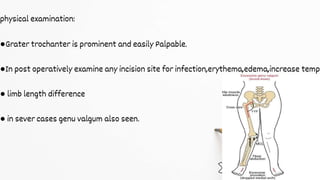
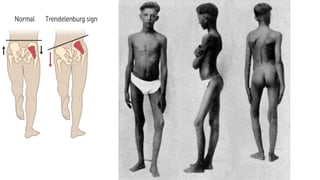
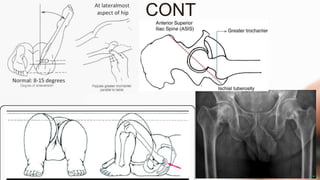
The document details the physiotherapy management of various foot deformities, including pes cavus and pes planus, as well as coxa vara. Key points include the definition, etiology, clinical presentations, assessment methods, and rehabilitation strategies for each condition. The document emphasizes the need for tailored therapeutic approaches to improve mobility, alleviate pain, and correct deformities.