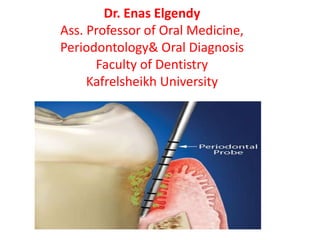
Periodontal pocket
- 1. Dr. Enas Elgendy Ass. Professor of Oral Medicine, Periodontology& Oral Diagnosis Faculty of Dentistry Kafrelsheikh University
- 2. Periodontal pocket • Periodontal pocket is pathologically deepened gingival sulcus due to apical migration of junction epithelium on the root surface with subsequent separation and hyperplasia of the gingiva resulting from inflammation • It is consider one of the important clinical features of periodontal disease.
- 3. Measurement Periodontal Pocket The probing pocket depth is the distance from the gingival margin to the bottom of the pocket (end of the probe).
- 4. Clinical attachment level/loss It is the distance from the CEJ to the end of the probe (bottom of the pocket). It is more constant measurement.
- 5. The measurement of the pocket depth is mainly influenced by the following factors:- a) The thickness of the probe. b) Malposition of the probe due to anatomic features such as the contour of the tooth surface. c) The pressure applied on the instrument during probing (Constant force probe).
- 6. Deeping of the pocket • The apical migration of the epithelial attachment during pocket formation is hindered mainly by the principal gingival fibers, which lies apical to the junctional epithelium. • The inflammatory process with in the gingival connective tissue might result in destruction of C.T fibers, and stimulate the epithelium to proliferate apically, destroying the subjacent collagen fibers.
- 7. Deeping of the pocket • The proliferating epithelium have some lysing effect on the collagen fibers or cause degeneration of gingival fibers by pressure atrophy. • It suggested the migration of epithelial rete pegs apically, which extend between the principal fibers causing its detachment N.B.: In all the above explanations, the inflammatory process initiates the reactions.
- 8. Stage I: The initial lesion :2- 4 days Stage II: The early lesion.: 4- 7 days Stage III: The established lesion.: 14-21 days Stage IV: The advanced lesion: 21 days
- 9. 9 Stages of Periodontal Disease
- 10. Classification of Pockets Gingival pocket (pseudo pocket) The sulcus is deepened because gingival enlargement without destruction of the underlying periodontal tissue (without apical migration of J.E). Periodontal pocket (true pocket) It is due to apical proliferation of junctional epithelium and destruction of the underlying supporting structures.
- 11. Classification of Periodontal Pockets Periodontal pockets are classified according to the relation of the base of the pocket to the alveolar crest into: Suprabony (supracrestal or supraalveolar) The bottom of the pocket is coronal to the underlying alveolar bone. Intrabony (infra bony pocket, subcrestal, or intraalveolar) The bottom of the pocket is apical to the underlying alveolar bone.
- 12. Different types of periodontal pockets. A, Gingival pocket, There is no destruction of the supporting periodontal tissue. B, Suprabony pocket, the base of the pocket is coronal to the level of underlying bone. Bone loss is horizontal. C, Intrabony pocket, the base of the pocket is apical to the level of adjacent bone. Bone loss is vertical.
- 13. Distinguishing features of the Suprabony pocket and the Infrabony pocket Suprabony pocket Infrabony pocket 1- The base of the pocket Coronal to the crest of the alveolar bone Apical to the crest of the alveolar bone 2- Pattern of bone destruction Horizontal Vertical 3-PL fibers Transeptal fibers are arranged horizontally in the space between the base of the pocket and the alveolar bone. Transeptal fibers are arranged obliquely from cementum beneath the base of the pocket over the crest to the cementum of the adjacent tooth
- 15. Classification of Periodontal Pockets Periodontal pockets are classified according to the number of tooth surfaces involved into: Simple pocket: involves one tooth surface Compound pocket: involves more than one tooth surface but the base and orifice of the pocket are located on the same tooth surface. Complex pocket: spiral pocket that involves more than one tooth surface where the base and the orifice are not located on the same surface.
- 16. Classification of pockets according to involved tooth surface. A, Simple pocket. B, Compound pocket. C, complex pocket (spiral pocket). A CB
- 17. Classification of Periodontal Pockets Intrabony pocket can be classified according to The number of the remaining osseous walls 1- One osseous wall infraboney pocket 2- Tow osseous wall infraboney pocket 3- Three osseous wall infraboney pocket 4- Combined osseous defect: in which the number of the osseous walls in the apically differ from that in occlusally. combination of one, two or three wall defect The depth and width of the defect: 1. Narrow deep, 2. Wide deep, 3. Narrow shallow 4. Deep shallow pocket.
- 18. A, Three wall defect B, Two wall defect C, One wall defect
- 19. Combined defect – combination of one, two or three wall defect
- 20. Periodontal pocket According to the relation of the base of the pocket to the alveolar crest into Suprabony Intrabony According to the number of tooth surfaces involved into Simple Compound Complex The number of the remaining osseous walls The depth and width of the defect 1. Narrow deep, 2. Wide deep, 3. Narrow shallow 4. Deep shallow pocket 1- One osseous wall 2- Tow osseous wall 3- Three osseous wall 4- Combined osseous defect
- 23. The furcation is the area located between individual roots. The progress of inflammatory periodontal diseases may ultimately results in attachment loss sufficient enough to affect the bifurcation or tri-furcation of multi- rooted teeth.
- 24. Classification of furcation Involvement: 1- Glickman (1958): Horizontal Classification 2- Hamp et al. (1975): Horizontal Classification 3- Tarnow and Fletcher (1984): Vertical Classification
- 25. Glickman (1958): Horizontal classification: Grade I: It incipient involvement into furcation with suprabony pockets and no interradicular bone loss. Grade II: involvement of the interradicular bone without through-and-through probability. Grade III: Through-and through loss of interradicular bone. Grade IV: Through-and through loss of interradicular bone, with total exposure of furcation owing to gingival recession.
- 26. 2- Hamp et al. (1975): Horizontal Classification : Grade I (initial): Loss of interradicular bone less than or equal to one-third. Grade II (partial): Loss of interradicular bone greater than one-third but not through and through. Grade III (total): through-and through loss of interradicular bone.
- 27. 3- Tarnow and Fletcher (1984): Vertical Classification: Grade A: Vertical loss of 1 to 3mm Grade B: Vertical loss of 4 to 6mm Grade C: Vertical loss of 7+ mm.
- 28. Grade I Grade IIIGrade II
- 30. Abscess of the Periodontium The periodontal abscess is a localized purulent inflammation of the periodontal tissues.
- 31. Periodontal abscess It has been classified into three diagnostic groups: Gingival abscess Periodontal abscess Pericoronal abscess
- 32. Etiology of periodontal abscess 1. Periodontal abscesses often arise as acute exacerbation of a preexisting pocket. 2. Improper scaling that may force bacteria or dislodge calculus fragment into the tissue. 3. Occlusion of the orifice of deep periodontal pocket: Inadequate scaling which will allow calculus to remain in the deepest pocket area, while the resolution of the inflammation at pocket area will occlude the normal drainage and then cause the abscess formation. 4. After receiving systemic antibiotic therapy. 5. Poorly controlled diabetes mellitus has been considered a predisposing factor for periodontal abscess formation. 6. Perforation of the tooth wall by an endodontic instrument. 7. Tooth fracture and foreign body impaction.
- 33. Etiology of periodontal abscess The existence of tortuous pockets (with cul-de- sac) which eventually become isolated, may favor the formation of abscess.
- 34. periodontal abscess resulting from partial healing of a periodontal pocket over residual calculus.
- 35. Clinical features I-Acute periodontal abscess versus Chronic Abscess: Abscesses are classified as acute or chronic. • The acute abscess is often an exacerbation of a chronic inflammatory periodontal lesion. Influencing factors include increased number and virulence of bacteria present, combined with lowered tissue resistance and lack of spontaneous drainage. The drainage may have been prevent by deep, tortuous pocket morphology, debris, or closely adapted pocket epithelium blocking the pocket orifice. • The chronic abscess forms after the spreading infection has been controlled by spontaneous drainage, host response, or therapy. Once homeostasis between the host and infection has been reached, the patient may have few or no symptoms.
- 36. Acute abscess Chronic abscess Painful, red, edematous, smooth, ovoid swelling of the gingival tissues. No pain or dull pain Exudate may be expressed with gentle pressure. Localized inflammation and a fistulous tract often associated with deep pocket. The tooth may be percussion sensitive and feel elevated in the socket . Slight tooth elevation Fever and regional lymphadenopathy are occasional findings. Usually without systemic involvement Compares the signs and symptoms of the acute and chronic abscess.
- 37. II- Periodontal versus Pulpal Abscess Periodontal abscess Pulpal abscess Associated with pre-existing periodontal pocket. Offending tooth may have large restoration or deep caries. May have no periodontal pocket. Tests show vital pulp Tests show non-vital pulp Swelling usually includes gingival tissue, with occasional fistula. Swelling often localized to apex, with a fistulous tract. Pain usually dull and localized. Pain often severe and difficult to localize. Sensitivity to horizontal percussion Sensitivity to vertical percussion. Radiographs show periodontal angular bone loss and furcation radiolucency. Radiographic changes along the lateral wall of the root Radiographic changes at the apical region.
- 39. Diagnosis of periodontal abscess Diagnosis of a periodontal abscess requires correlation of the history and clinical and radiograghic findings. It is based on: • Symptoms revealed by the patient, • The signs found during the oral examination. • A periodontal abscess is usually associated with pre-existing periodontitis. • Drainage of the pus may occur during periodontal probing or without provocation. • Careful medical and dental history and radiographic examination.
- 40. Radiographic examination • It may reveal some degree of bone loss ranging from widening of periodontal space to a dramatic radiographic bone loss. • Radiograph alone can not be relied on for the diagnosis of periodontal abscess since (give reasons): 1- In early stages of the lesion no radiographic changes can be detected. 2- Abscess on the facial and lingual surface are obscured by the radio-opacity of the roots
- 41. Treatment approaches The periodontal abscess is the third most prevalent emergency infection after periapical abscess and pericoronitis. Treatment of the periodontal abscess includes two phases: • Resolving the acute lesion • Followed by the management of the resulting chronic condition.
- 42. Treatment approaches I-Acute Abscess • The acute abscess is treated to alleviate symptoms, control the spread of infection, and establish drainage. Before treatment, the patient’s medical history, dental history, and systemic condition are reviewed and evaluated (such as rise temperature fever, lymphadenopathy) to assist in the diagnosis and to determine the need for systemic antibiotics.
- 43. Treatment approaches Drainage through Periodontal Pocket: The peripheral area around the abscess is anesthetized with sufficient topical and local anesthetic to ensure comfort. The pocket wall is gently retracted with a periodontal probe or curette in an attempt to initiate drainage through the pocket entrance. Gentle digital pressure and irrigation may be used to express exudates and clear the pocket.
- 46. Treatment approaches Drainage through External Incision: • The abscess is dried and isolated with gauze sponges. Topical anesthetic is applied, followed by local anesthetic injected peripheral to the lesion. A vertical incision through the most fluctuant center of the abscess is made with a #15 surgical blade. • Pus is expressed and the wound edges approximated under light digital pressure with a moist gauze pad.
- 47. Drainage through External Incision:
- 48. Indications for antibiotic therapy in the patients with acute abscess 1. In abscesses presenting with severe swelling and inflammation, cellulitius (non-localized, spreading infection) aggressive mechanical instrumentation should be delayed in favor of antibiotic therapy so as to avoid damage to healthy contiguous periodontal tissues. 2. The lesions are large, deep, inaccessible and drainage cannot be established. 3. Fever 4. Regional lymphadenopathy 5. Immunocompromised patient
- 49. Antibiotic options for periodontal infection • Amoxicillin, 500 mg 3 times a day for 3 days (1 g loading dose) • Penicillin allergy: 1- Clindamycin 300 mg 4 times a day for 3 days (600 mg loading dose) 2- Azithromycin 500 mg four times a day for 3 days (1.0-g loading dose)
- 50. Instruction after drainage • Area then painted with antiseptic. Patients without systemic complications are instructed to rinse with a solution of 1 tsp. salt in a glass of warm water and periodic application of chlorhexidine gluconate either by rinsing or locally with a cotton-tipped applicator. • Analgesics may be prescribed for comfort. • Patient is followed up until swelling and symptoms have disappeared and then the lesion is ready for the usual treatment of chronic periodontitis.
- 51. Treatment approaches Chronic Abscess • As with a periodontal pocket, the chronic abscess is usually treated with scaling and root planing or surgical therapy. Surgical treatment is suggested when deep vertical or furcation defects are encountered that are beyond the therapeutic capabilities of nonsurgical instrumentation. As with the acute abscess antibiotic therapy may be indicated.
- 52. Fistula is observed in attached gingiva of maxillary right canine. Elevated flap shows the cause to be a root fracture.
- 54. Gingival Abscess Treatment of the gingival abscess is aimed at reversal of the acute phase and, when applicable, immediate removal of the cause. To ensure procedural comfort, topical or local anesthesia by infiltration is administered. The fluctuant area is incised with a #15 scalpel blade, and exudate may be expressed by gentle digital pressure. Any foreign material (e.g., dental floss, impression material) is removed. The area is irrigated with warm water and covered with moist gauze under light pressure. Once bleeding has stopped, the patient is dismissed with instructions to rinse with warm salt water every 2 hours for the remainder of the day. After 24 hours the area is reassessed, and if resolution is sufficient, scaling not previously completed is undertaken. If the residual lesion is large or poorly accessible, surgical access may be required.
- 55. Pericoronal Abscess As with the other abscesses of the periodontium, the treatment of the pericoronal abscess is aimed at management of the acute phase, followed by resolution of the chronic condition. The acute pericoronal abscess is properly anesthetized for comfort, and drainage is established by gently lifting the soft tissue operculum with a periodontal probe or curette. If the underlying debris is easily accessible, it may be removed, followed by gentle irrigation with sterile saline. If there is regional swelling, lymphadenopathy, or systemic signs, systemic antibiotics may be prescribed. The patient is dismissed with instructions to rinse with warm salt water every 2 hours, and the area is reassessed after 24 hours. If discomfort was one of the original complaints, appropriate analgesics should be employed.
- 56. Once the acute phase has been controlled, the partially erupted tooth may be definitively treated with either surgical excision of the overlying tissue or removal of the offending tooth.
